Abstract
Methods
The present study included 3,662 subjects who were diagnosed with a cataract by ophthalmic examination out of 11,058 subjects in the fourth Korea National Health and Nutrition Examination Survey (KNHANES IV). Among the 3,662 participants, 944 were aware that they already had a cataract. The sociodemographic disparities in cataract awareness were identified using multivariate analysis.
Results
The mean age of the study population was 65.6 years (standard deviation, 0.2). The awareness calculated based on total weighted population was 24.6% in people over 19 years of age (95% confidence interval, 22.5–26.6%). In multivariate logistic analysis, subjects with higher income, living in a rural area, having a spouse, and binge alcohol use were less likely to be aware of their cataract. In multivariate linear regression analysis after adjusting for confounding factors, there were statistically significant differences of mean in age and monthly house income. Deajeon (11%), and Gwangju (16%) were the lower ranked regions for cataract awareness in Korea.
Conclusions
The cataract awareness in Korea was lower than in other developed countries. Public education and strategies to improve cataract awareness in susceptible people are necessary. More effort is needed to improve cataract awareness based on the Korean society's acceptance of ophthalmologists as in other countries.
Go to : 
References
1. Mitchell P, Cumming RG, Attebo K, Panchapakesan J. Prevalence of cataract in Australia: the Blue Mountains eye study. Ophthalmology. 1997; 104:581–8.
2. Leske MC, Connell AM, Wu SY, et al. Prevalence of lens opacities in the Barbados Eye Study. Arch Ophthalmol. 1997; 115:105–11.

3. Klein BE, Klein R, Linton KL. Prevalence of age-related lens abdominal in a population. The Beaver Dam Eye Study. Ophthalmology. 1992; 99:546–52.
4. Thylefors B, Négrel AD, Pararajasegaram R, Dadzie KY. Global data on blindness. Bull World Health Organ. 1995; 73:115–21.
5. Yoon KC, Mun GH, Kim SD, et al. Prevalence of eye diseases in South Korea: data from the Korea National Health and Nutrition Examination Survey 2008–2009. Korean J Ophthalmol. 2011; 25:421–33.

6. Dandona R, Dandona L, John RK, et al. Awareness of eye diseases in an urban population in southern India. Bull World Health Organ. 2001; 79:96–102.
7. Lau JT, Lee V, Fan D, et al. Knowledge about cataract, glaucoma, and age related macular degeneration in the Hong Kong Chinese population. Br J Ophthalmol. 2002; 86:1080–4.

8. Garraway WM, Whisnant JP. The changing pattern of hypertension and the declining incidence of stroke. JAMA. 1987; 258:214–7.

9. Worden JK, Solomon LJ, Flynn BS, et al. A community-wide abdominal in breast self-examination training and maintenance. Prev Med. 1990; 19:254–69.
10. Mckay J, Miller G. Prevention and treatment of alcohol and other drug use: engaging indigenous people in the northern territory. Drug Alcohol Rev. 2009; 28:A43–4.
11. Zhou JB, Guan HJ, Qu J, et al. A study on the awareness of cataract disease and treatment options in patients who need surgery in a abdominal area of Eastern China. Eur J Ophthalmol. 2008; 18:544–50.
12. Livingston PM, McCarty CA, Taylor HR. Knowledge, attitudes, and self care practices associated with age related eye disease in Australia. Br J Ophthalmol. 1998; 82:780–5.

13. Noertjojo K, Maberley D, Bassett K, Courtright P. Awareness of eye diseases and risk factors: identifying needs for health education and promotion in Canada. Can J Ophthalmol. 2006; 41:617–23.

14. Chew YK, Reddy SC, Karina R. Awareness and knowledge of common eye diseases among the academic staff (non-medical fac-ulties) of University of Malaya. Med J Malaysia. 2004; 59:305–11.
15. Attebo K, Mitchell P, Cumming R, Smith W. Knowledge and be-liefs about common eye diseases. Aust N Z J Ophthalmol. 1997; 25:283–7.

16. Javitt JC. Preventing blindness in Americans: the need for eye health education. Surv Ophthalmol. 1995; 40:41–4.
17. Livingston PM, Lee SE, De Paola C, et al. Knowledge of abdominal, and its relationship to self-care practices, in a population sample. Aust N Z J Ophthalmol. 1995; 23:37–41.
18. Cigarette smoking among adults–United States, 1992, and changes in the difinition of current cigarette smoking. MMWR Morb Mortal Wkly Rep. 1994; 43:342–6.
19. Edelman D, Christian A, Mosca L. Association of acculturation status with beliefs, barriers, and perceptions related to abdominal disease prevention among racial and ethnic minorities. J Transcult Nurs. 2009; 20:278–85.
20. Hwang SY, Kweon YR, Kim AL. Perceptions of barriers to abdominal risk factors and decision to seek treatment among mid-dle-aged men with acute myocardial infarction. J Korean Acad Adult Nurs. 2010; 22:537–51.
21. Crosson JC, Heisler M, Subramanian U, et al. Physicians' perceptions of barriers to cardiovascular disease risk factor control among patients with diabetes: results from the translating research into action for diabetes (TRIAD) study. J Am Board Fam Med. 2010; 23:171–8.

22. Mann KV, Putnam RW. Barriers to prevention: physician perceptions of ideal versus actual practices in reducing cardiovascular risk. Can Fam Physician. 1990; 36:665–70.
Go to : 
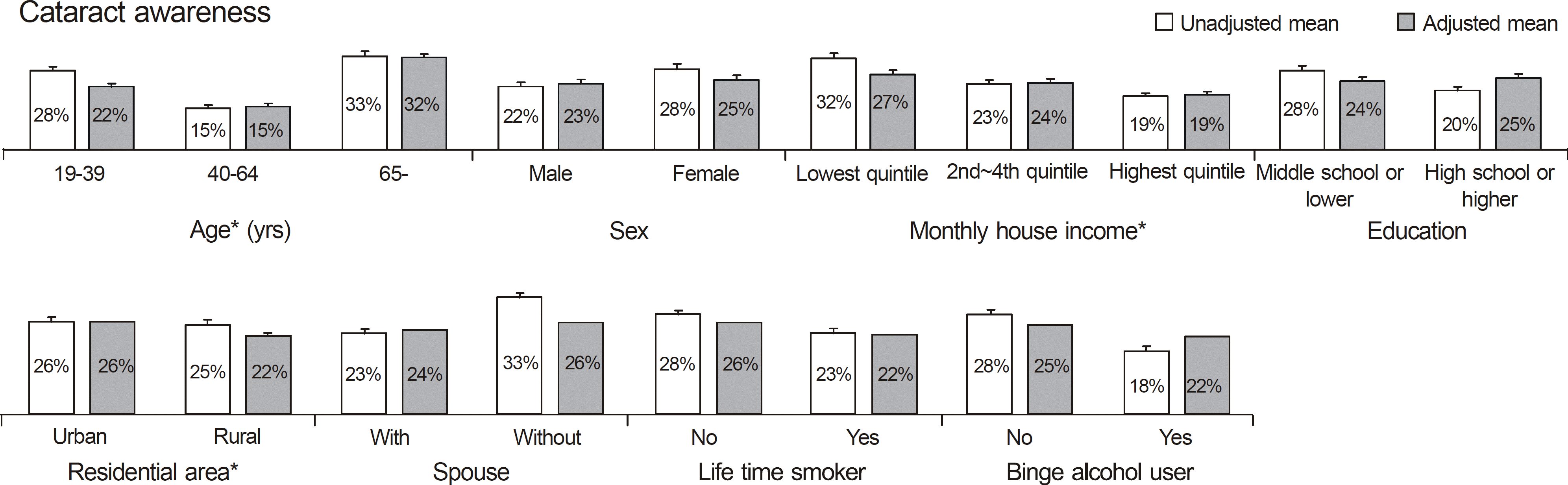 | Figure 1.Unadjusted and adjusted mean of cataract awareness for adjusting confounding factors including age, sex, income, education, residential area, lifetime smoker, and binge alcohol user. When we consider one variable as an independent variable, we adjust other confounding factors except that variable. For example, to calculate adjusted mean of cataract awareness between age groups, we adjusted all confounding factors but age. * p < 0.05 in multivariate linear regression. |
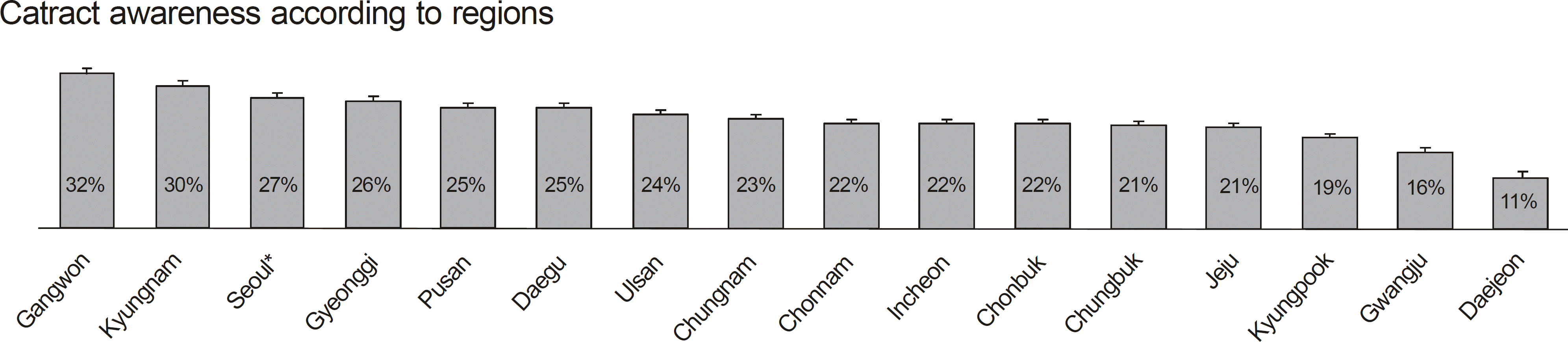 | Figure 2.Unadjusted mean of cataract awareness according to regions. * The capital city of South Korea. |
Table 1.
Characteristic of study population (n = 3,662)
Table 2.
Factors associated with cataract awareness (n = 3,662)




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download