Abstract
Purpose
To investigate the diurnal variation of subjective visual symptoms of diabetic patients and to evaluate its correlation with visual acuity, blood pressure, blood glucose and OCT-measured macular thickness.
Methods
Fifty-five diabetic patients (56 eyes) who were hospitalized for the operation of the fellow eye were enrolled in the study. They underwent optical coherence tomography (OCT) measurements of macular thickness with retinal mapping protocol of OTI/SLO OCT at 5PM, 8PM on operation day, and at 7AM, 10AM on following day. Visual acuity (log MAR), refraction, intraocular pressure, blood glucose and blood pressure were also measured at each time. We surveyed the patients' symptomatic visual variation and its pattern if there is any change over a day.
Results
Thirteen patients (25%) had reported changes in their subjective visual symptom over a day according to their blood glucose level. Among twenty-four cases with changes in their subjective visual acuity throughout the exam, only ten showed their real visual acuity change in accordance with their symptoms.
References
1. Klein R, Klein BE, Moss SE, Cruickshanks KJ. The Wisconsin Epidemiologic Study of Diabetic Retinopathy: XVII. The 14-year incidence and progression of diabetic retinopathy and associated risk factors in type 1 diabetes. Ophthalmology. 1998; 105:1801–15.

2. Klein R, Sternberg P Jr, Fitzke F, Finkelstein D.Cyclic macular edema. Am J Ophthalmol. 1982; 94:664–9.
3. Frank RN, Schulz L, Abe K, lezzi R. Temporal variation in diabetic macular edema measured by optical coherence tomography. Ophthalmology. 2004; 111:211–7.

4. Wiemer NG, Eekhoff EM, Simsek S, et al. The effect of acute hyperglycemia on retinal thickness and ocular refraction in healthy subjects. Graefes Arch Clin Exp Ophthalmol. 2008; 246:703–8.

5. Diabetic Retinopathy Clinical Research Network. Danis RP, Glassman AR. Diurnal variation in retinal thickening measurement by optical coherence tomography in center-involved diabetic macular edema. Arch Ophthalmol. 2006; 124:1701–7.

6. Polito A, Del Borrello M, Polini G, et al. Diurnal variation in clinically significant diabetic macular edema measured by the Stratus OCT. Retina. 2006; 26:14–20.

7. Polito A, Polini G, Chiodini RG, et al. Effect of posture on the diurnal variation in clinically significant diabetic macular edema. Invest Ophthalmol Vis Sci. 2007; 48:3318–23.

8. Larsen M, Wang M, Sander B. Overnight thickness variation in diabetic macular edema. Invest Ophthalmol Vis Sci. 2005; 46:2313–6.

9. Okamoto F, Sone H, Nonoyama T, Hommura S. Refractive changes in diabetic patients during intensive glycaemic control. Br J Ophthalmol. 2000; 84:1097–102.

Figure 1.
Central subfield thickness, blood glucose, visual acuity, and blood pressure throughout the day from 7 AM to 8 PM.
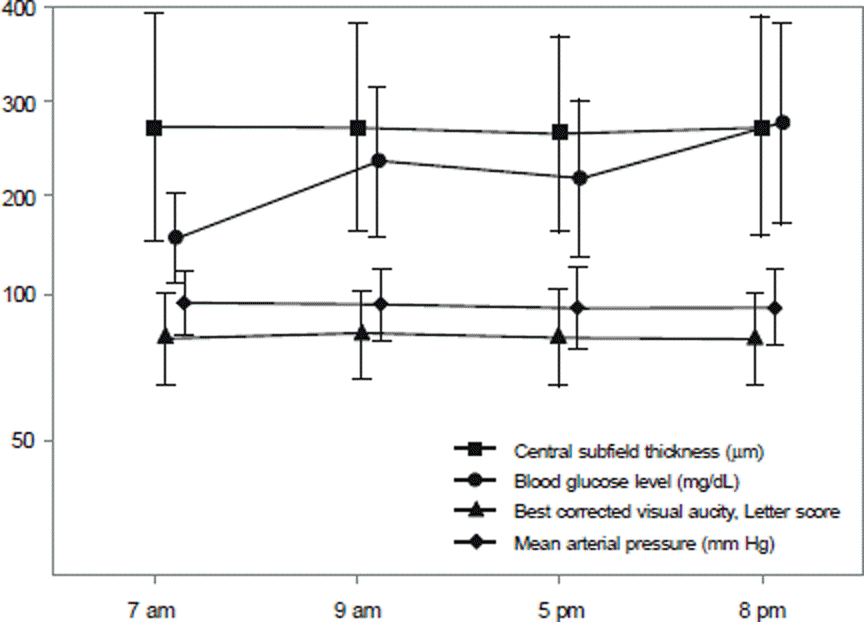
Figure 2.
Correlation between blood pressure change and best corrected visual acuity, letter score change. There was no correlation between two factors (correlation coefficient = −0.081, p = 0.295, Pearson correlation test).
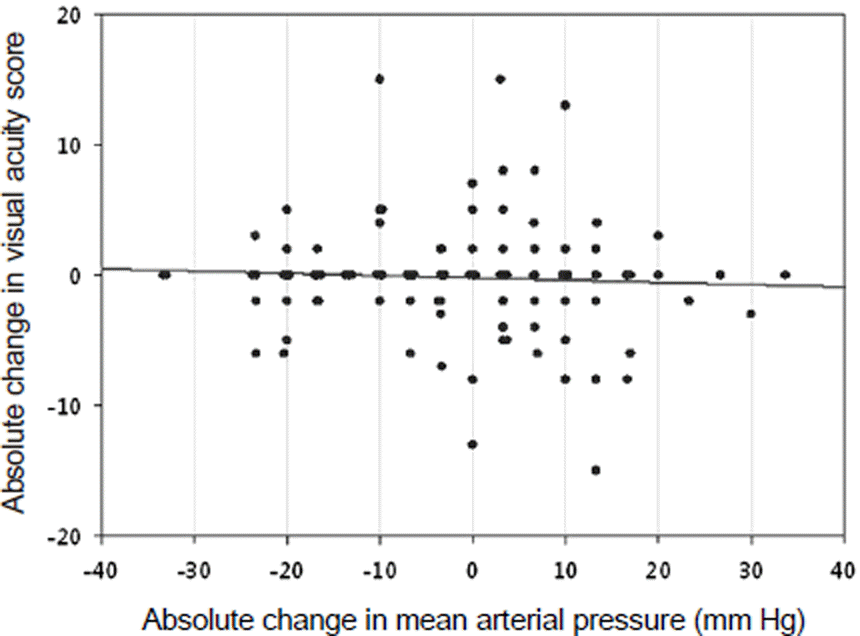
Figure 3.
Correlation between blood pressure change and retinal thickness change. There was no correlation between two factors (correlation coefficient = 0.098, p = 0.204, Pearson correlation test).
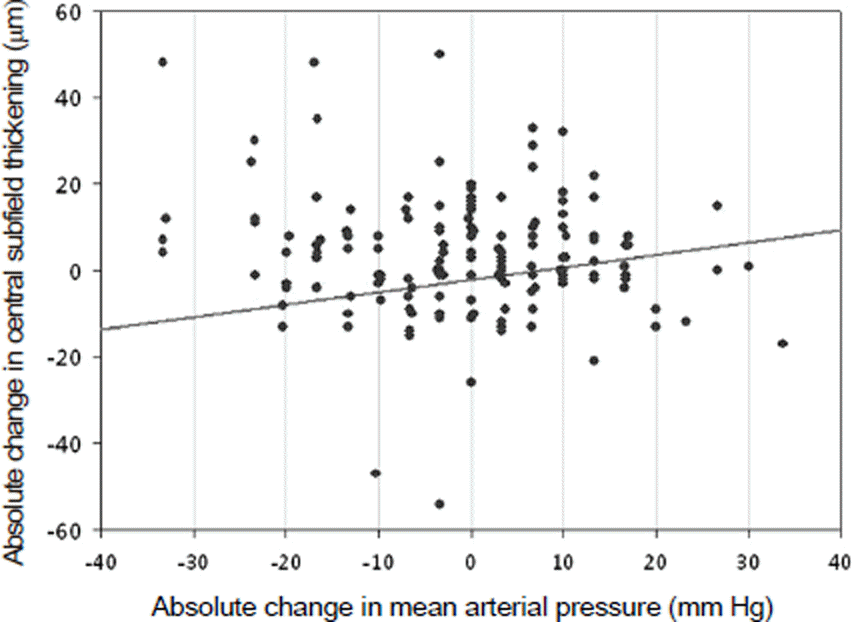
Figure 4.
Correlation between retinal thickness and best-corrected visual acuity, letter score. They showed significant relationship between two factors. (A = all group, B = macula edema group, C = macula edema-free group).
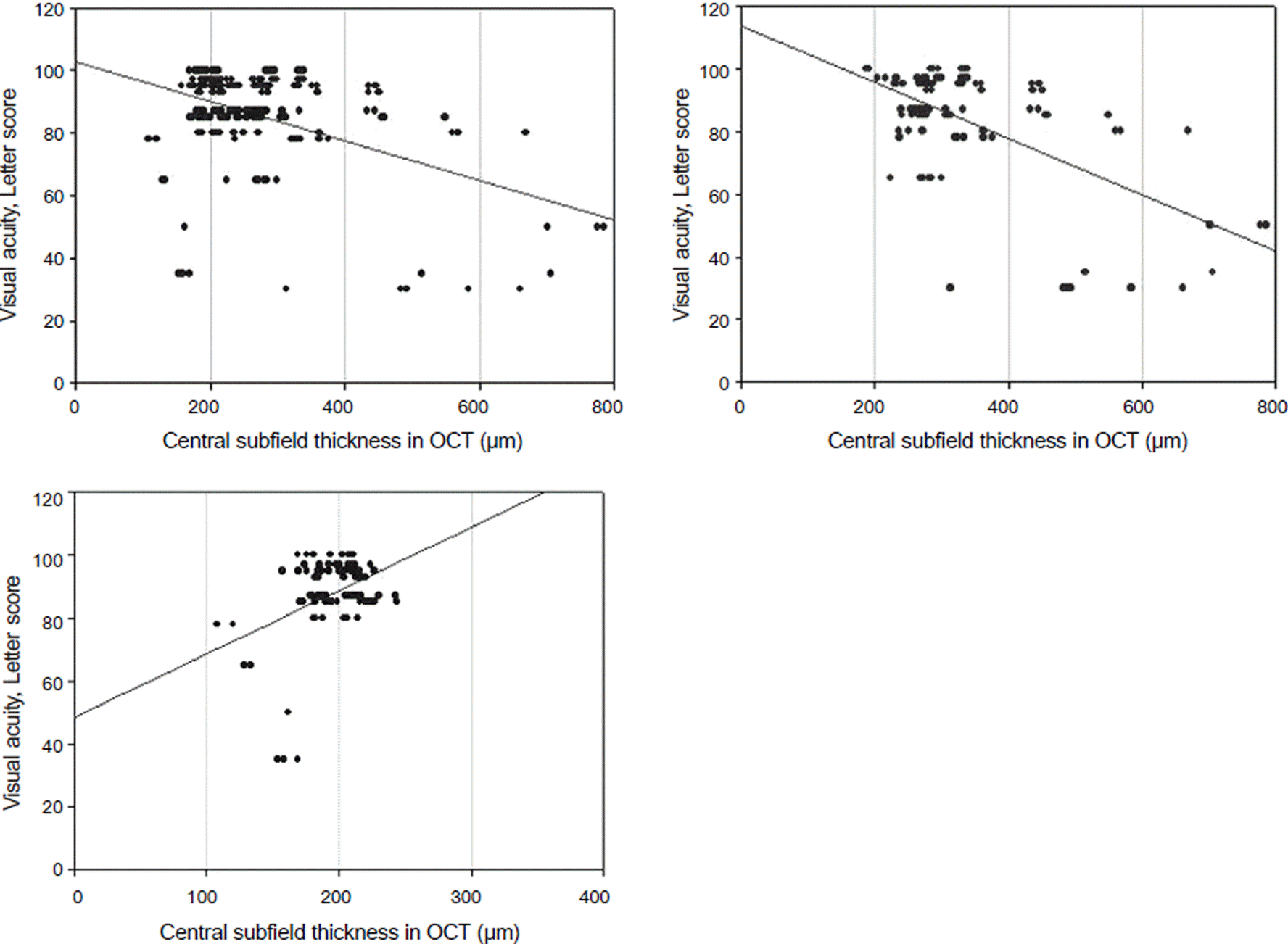
Table 1.
Characteristics of patients
Table 2.
Characteristics of eye in 7AM
Table 3.
Diurnal variations of central subfield thickness (CST). CST changes from supper fasting or pp2 state to morning fasting or pp2 state
| Fasting state | PP2 | ||||
|---|---|---|---|---|---|
| ME +* | No. of eye | CST change (μm) | No. of eye | CST change (μm) | |
| Decrease | 14 | -84.93 ± 92.46 | 14 | 19.86 ± 33.56 | |
| Change -† | 1 | 2 | 0 | ||
| Increase | 15 | 26.63 ± 12.71 | 14 | -14.79 ± 21.3 | |
| Total | 30 | -27.35 ± 69.33 | 30 | 4.58 ± 31.59 | |
| ME -‡ | Decrease | 12 | -7.0 ± 6.98 | 15 | -6.87 ± 6.09 |
| Change - | 1 | 1 | |||
| Increase | 13 | 8.85 ± 7.66 | 10 | 6.6 ± 4.35 | |
| Total | 26 | 1.19 ± 10.6 | 26 | -1.42 ± 8.44 | |
Table 4.
Differences between two groups divided by whether ordinary subjective visual symptom changes or not
| Ordinary symptom change (−) | Ordinary symptom change (+) | p-value | |
|---|---|---|---|
| Number of case | 43 | 13 | |
| Subjective visual symptom change, No. (%) | 17 (40%) | 7 (54%) | 0.361 |
| Currently medically treated for hypertension, No. (%) | 31 (72%) | 7 (54%) | 0.541 |
| Currently treated with subcutaneous insulin, No. (%) | 10 (23%) | 3 (23%) | 0.424 |
| Vitrectomized eye, No. (%) | 4 (9%) | 5 (40%) | 0.012* |
| Abnormal BUN/Cr, No. (%) | 16 (37%) | 4 (31%) | 0.671 |
| Presence of ME, No. (%) | 22 (51%) | 8 (62%) | 0.511 |
| Pseudophakia, No. (%) | 19 (44%) | 4 (31%) | 0.085 |
| BUN/Cr (mg/dL) | 16.3 ± 5.3 | 17.4 ± 5.8 | 0.554 |
| BCVA, letter score | 86.7 ± 15.1 | 82.2 ± 18.0 | 0.165 |
| Maximum change in blood glucose (mg/dL) | 144.3 ± 86.3 | 163.2 ± 74.8 | 0.388 |
| CST (μm) | 266.6 ± 105.6 | 285.5 ± 135.8 | 0.575 |
| Maximal CST change, μm (%) | 19.0 ± 16.6 | 54.6 ± 92.5 | 0.593 |
| (7.8 ± 6.4) | (16.6 ± 20.7) | (0.415) | |
| Maximal mean arterial pressure change (mm Hg) | 18.3 ± 8.9 | 14.2 ± 11.9 | 0.077 |
Table 5.
Differences between two groups divided by whether subjective visual acuity changes or not throughout the examination
| Subjective visual symptom change (-) | Subjective visual symptom change (+) | p-value | |
|---|---|---|---|
| Number of case | 32 | 24 | |
| Ordinary visual symptom change, No. (%) | 6 (19) | 7 (30) | 0.361 |
| Currently treated for hypertension, No. (%) | 15 (47) | 11 (46) | 0.938 |
| Currently treated with subcutaneous insulin, No. (%) | 8 (25) | 10 (42) | 0.186 |
| Vitrectomized eye, No. (%) | 5 (16) | 4 (17) | 0.916 |
| Abnormal BUN/Cr, No. (%) | 10 (31%) | 10 (42%) | 0.421 |
| Presence of ME, No. (%) | 16 (50%) | 14 (59%) | 0.536 |
| Pseudophakia, No. (%) | 17 (53%) | 6 (25%) | <0.001 |
| BUN/Cr (mg/dL) | 16.8 ± 5.5 | 16.4 ± 5.4 | 0.896 |
| BCVA, letter score | 86.7 ± 15.5 | 84.3 ± 16.3 | 0.113 |
| Maximum change in blood glucose (mg/dL) | 152.0 ± 84.0 | 144.4 ± 84.1 | 0.667 |
| CST (μm) | 266.9 ± 127.9 | 276.3 ± 90.6 | 0.325 |
| Maximal CST change, μm (%) | 34.5 ± 62.4 | 17.7 ± 19.7 | 0.182 |
| (11.4 ± 12.6) | (7.7 ± 10.5) | (0.042*) | |
| Maximal mean arterial pressure change (mm Hg) | 19.6 ± 10.1 | 14.5 ± 8.6 | 0.048* |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download