Abstract
Purpose
To evaluate the short-term efficacy of astigmatism correction and rotational stability of AcrySof Toric Intraocular lens (IOL) implants.
Method
We analyzed 27 eyes of 23 patients who underwent microcoaxial cataract surgery (MCCS) and AcrySof Toric IOL implantation between March 2008 and July 2008. We evaluated visual acuity, keratometry, and refraction. Slit-lamp retro-illumination photographs were obtained in all patients on 1 day, 1 month and 3 months postoperatively. The change of postoperative IOL axis alignment and the presence of anterior capsular shrinkage were analyzed.
Result
The mean unaided visual acuity (LogMAR) improved from 1.02±0.38 to 0.10±0.12. Although postoperative manual keratometric value was not different from the preoperative value, post-operative astigmatism decreased from a mean value of 1.66±0.42D to 0.61±0.38D at 3 months postoperatively. The mean difference between achieved and intended lens axis was 1.63±2.83 degrees at the first post-operative day, and 1.91±2.92 degrees on the first postoperative month, with all cases within 10 degrees. There were two cases of IOL rotation between one day and one month postoperative follow-up, and severe anterior capsule contractions were found in them.
Conclusions
AcrySof Toric IOL is effective for correction of astigmatism and it has good post-operative rotational stability. Because most of misalignments were found at the postoperative day 1, the precise implantation of IOL, according to the intended axis, can be important during operation and immediately after the operation.
References
2. Colin J, Cochener B, Le Floch G. Excimer laser treatment of myopic astigmatism: a comparison of three ablation programs. Ophthalmology. 1998; 105:1182–8.
3. Dausch D, Klein R, Landesz M, Schroder E. Photorefractive keratectomy to correct astigmatism. J Cataract Refract Surg. 1994; 20:S252–7.
4. Salchow DJ, Zirm ME, Stieldorf C, Parisi A. Laser in situ keratomileusis for myopia and myopic astigmatism. J Cataract Refract Surg. 1998; 24:175–82.

5. Knorz MC, Wiesinger B, Liermann A, et al. Laser in situ keratomileusis for moderate and high myopia and myopic astigmatism. Ophthalmology. 1998; 105:932–40.

6. Lee KM, Kim EC, Kim MS. Excimer laser refractive surgery to correct anisometropia due to residual astigmatism after cataract surgery. J Korean Ophthalmol Soc. 2008; 49:1589–96.

7. Niles C, Culp B, Teal P. Excimer laser photorefractive keratectomy using an erodible mask to treat myopic astigmatism. J Cataract Refract Surg. 1996; 22:436–40.

8. Shimizu K, Misawa A, Suzuki Y. Toric intraocular lenses: correcting astigmatism while controlling axis shift. J Cataract Refract Surg. 1994; 20:523–6.

9. Werblin TP. Do three-piece PMMA IOLs rotate after implantation in the capsular bag? J Refract Surg. 1995; 11:468–71.

10. Grills JP, Martin RG, Sanders DR. Sutureless Cataract Surgery: An Evolution Toward Minimally Invasive Technique. Thorofare, NJ: Slack Inc;1992. p. 183–97.
11. Gills JP, Martin RG, Thornton SP, Sanders DR. Surgical Treatment of Astigmatism. Thorofare, NJ: Slack Inc;1994. p. 159–64.
12. Mendicute J, Irigoyen C, Aramberri J, et al. Foldable toric intraocular lens for astigmatism correction in cataract patients. J Cataract Refract Surg. 2008; 34:601–7.

13. Cravy TB. Calculation of the change in corneal astigmatism following cataract extraction. Ophthalmic Surg. 1979; 10:38–49.
16. Weinand F, Jung A, Stein A, et al. Rotational stability of a single-piece hydrophobic acrylic intraocular lens: new method for high-precision rotation control. J Cataract Refract Surg. 2007; 33:800–3.

17. Sun X-Y, Vicary D, Montgomery P, et al. Toric intraocular lenses for correcting astigmatism in 130 eyes. Ophthalmology. 2000; 107:1776–82.

18. Till JS, Yoder PR Jr, Wilcox TK, Spielman JL. Toric intraocular lens implantation: 100 consecutive cases. J Cataract Refract Surg. 2002; 28:295–301.

19. Zuberbuhler B, Signer T, Gale R, Haefliger E. Rotational stability of the AcrySof SA60TT toric intraocular lenses: A cohort study. BMC Ophthalmology. 2008; 8:1471–2415.

20. Bauer NJC, Vries NE, Webers CA, et al. Astigmatism management in cataract surgery with the AcySof toric intraocular lens. J Cataract Refract Surg. 2008; 34:1483–8.
Figure 1.
Time course of uncorrected visual acuity (UCVA) and best corrected visual acuity (BCVA). Both post-operative UCVA and BCVA were significantly improved when compared with pre-operative values (p-value<0.001).
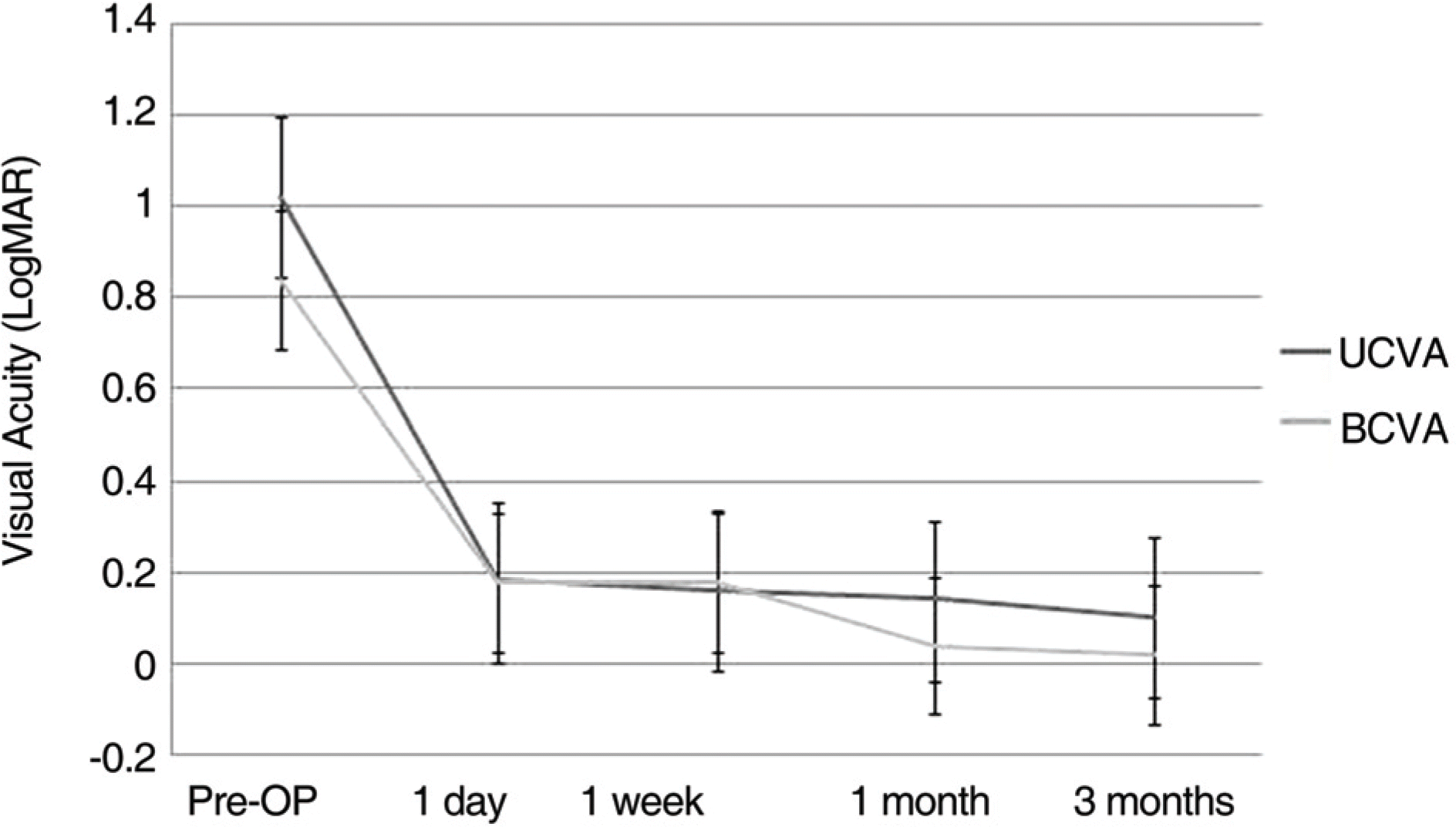
Figure 2.
Bar chart of magnitude of the refractive cylinders (corneal plane). Before cataract surgery, the refractive cylinder was 1.66±0.42D and considering the SIA (surgically-induced astigmatism), we could predict the post-operative refractive cylinder as 1.82±0.78D using non-toric IOL. However, in this study, the post-operative refractive cylinder was 0.61±0.38D using the toric IOL. Decrement of the cylinder was statistically significant (p-value<0.001).
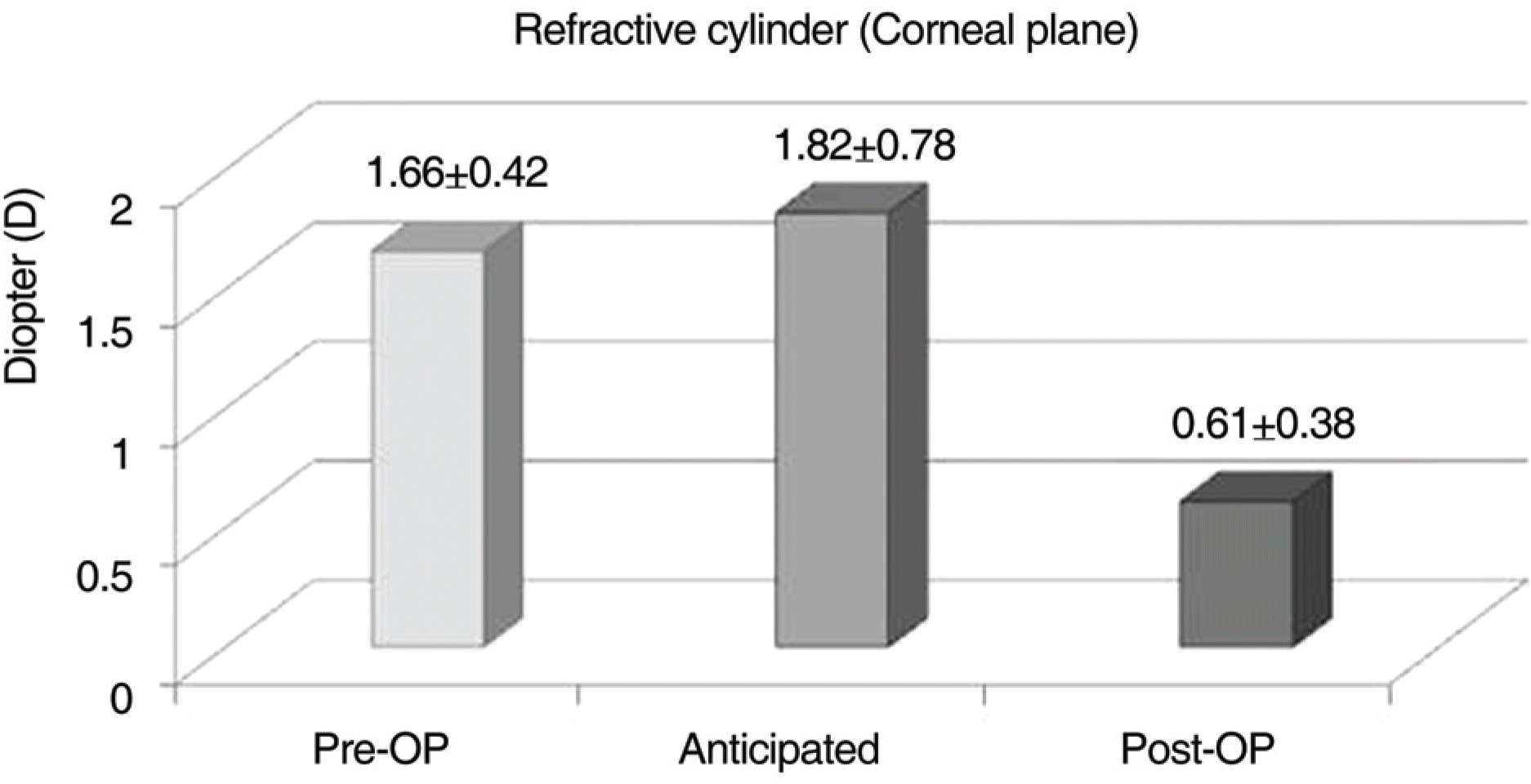
Figure 3.
Two sets of anterior segment photographs representing two cases of IOL rotation at one day and one month postoperative follow-up (Arrow: reference marks on the optic surface, red line: axis). (A, B)=Case I; (C, D)=Case II; (A, C)=In both cases, IOL was placed precisely into the intended axis (90 degrees) on the first post-operative day observation; (B, D)=At post-operative one month, IOL was rotated counterclockwise by 5 degrees and 7 degrees in Case I and II, respectively. In both cases, anterior capsules showed fibrotic change and capsule contraction.

Figure 4.
The degree and direction of IOL rotation. Two eyes had against-the-rule astigmatism (ATR), and 8 eyes had with-the-rule astigmatism (WTR). Plus and minus refers to clockwise and counterclockwise direction, respectively. Clockwise rotation was present in 3 eyes, while the remainders had counterclockwise rotation.
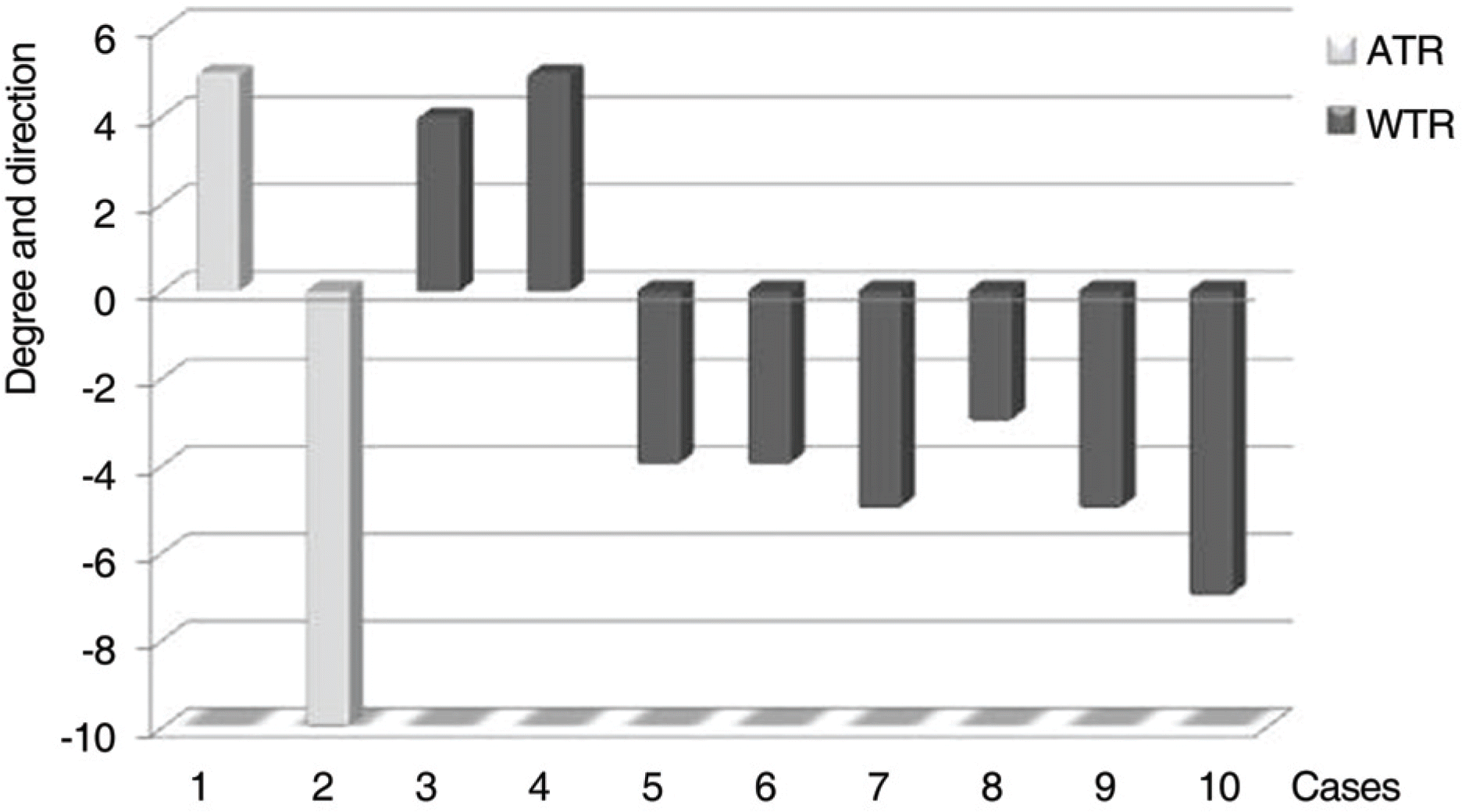
Table 1.
Patients demographics and pre-operative data
| | All eyes | SN60T3 | SN60T4 | SN60T5 |
|---|---|---|---|---|
| Eyes (N) | 27 | 8 | 14 | 5 |
| Patients (N) | 23 | 7 | 12 | 4 |
| Age (Year) | 63.6±12.3 | 67.88±8,51 | 64.21±13.62 | 55.00±10.98 |
| Age (Year) | (39∼82) | (53∼81) | (46∼82) | (39∼70) |
| Follow-up (Months) | 2.85±0.53 | 2.50±0.93 | 3.00±0.00 | 3.00±0.00 |
| OD/OS | 12/15 | 5/3 | 7/7 | 1/3 |
| Male/Female | 12/15 | 4/4 | 7/7 | 1/3 |
| BCVA (LogMAR) | 0.55±0.35 | 0.38±0.33 | 0.51±0.23 | 0.84±0.52 |
| | (0.10∼1.40) | (0.10∼1.0) | (0.22∼0.90) | (0.30∼1.40) |
| Spherical equivalent (D*) | 1.62±3.99 | 0.08±2.49 | −2.15±4.49 | −1.95±3.83 |
| | (−14.25∼-2.24) | (−2.88∼3.25) | (−14.25∼+3.00) | (−4.88∼2.38) |
| Spherical IOL power (D*) | 19.68±2.44 | 21.40±0.96 | 19.05±1.77 | 19.90±4.19 |
| Refractive cylinder (D*) (corneal plane) | 1.66±0.42 | 1.80±0.51 | 1.63±0.37 | 1.60±0.54 |
| | (0.89∼2.24) | (0.89∼2.07) | (−2.21∼-0.89) | (1.09∼2.24) |
| Manual keratometric cylinder (D*) | 1.84±0.66 | 1.50±0.27 | 1.66±0.32 | 2.75±0.92 |
| | (1.00∼4.25) | (1.00∼1.75) | (1.25∼2.25) | (1.75∼4.25) |
| Toric IOL cylinder | 1.49±0.36 | 1.03 | 1.55 | 2.06 |
| power (D*) (corneal plane) | (1.03∼2.06) | | | |
Table 2.
Absolute misalignment and direction of the AcrySof toric intraocular lenses rotation according to time course
| | Postoperative 1 day* | Postoperative 1 mon† | Postoperative 3 mon† |
|---|---|---|---|
| Eyes (n) | 27 | 25 | 24 |
| No rotation | 19 | 23 | 24 |
| Misalignment | 8 | 2 | 0 |
| Absolute misalignment (degrees) | | | |
| Mean± SD | 4.78±2.11 | 6.00±1.41 | |
| Range | (3.00∼10.00) | (5.00∼7.00) | |
| Direction of rotation (n) | | | |
| Clockwise | 3 | 0 | |
| Counterclockwise | 5 | 2 | |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download