Abstract
Purpose
To compare macular thickness and visual acuity before and after panretinal photocoagulation in patients with severe diabetic retinopathy without diabetic macular edema.
Methods
Macular thickness and visual acuity (LogMAR) of 40 eyes were compared before and after panretinal photocoagulation, for severe diabetic retinopathy. Macular thickness was measured by optical coherence tomography(OCT). In addition, changes in macular thickness and visual acuity were compared with the patient's level of HbA1c, blood pressure, and diabetic nephropathy.
Results
Mean visual acuity before and 1.47±0.80 months after panretinal photocoagulation were 0.28±0.23 and 0.33±0.27, respectively, which was not a significant decrease (p=0.131). However mean central macular thickness (216.98±34.09 μ m to 255.22±73.40 μ m), and mean peripheral macular thickness (269.26±34.59 μ m to 291.96±46.49 μ m) did increase significantly after panretinal photocoagulation (p=0.001). The decrease of mean visual acuity and increase of mean macular thickness were greater in patients with high blood glucose, high blood pressure and diabetic nephropathy.
Conclusions
In eyes with severe diabetic retinopathy treated with panretinal photocoagulation, mean visual acuity did not decrease significantly, but mean central and peripheral macular thickness significantly increased after treatment. We posit that visual prognosis after panretinal photocoagulation in eyes with severe diabetic retinopathy without macular edema is influenced by the control of blood glucose and blood pressure and the presence of diabetic nephropathy.
Go to : 
References
1. The Diabetic Retinopathy Study Group. Photocoagulation treatment of proliferative diabetic retinopathy: Clinical application of DRS findings. DRS report No. 8. Opthalmology. 1981; 88:583–600.
2. Early Treatment Diabetic Retinopathy Study Group. Photocoagulation for diabetic macular edema. ETDRS report No. 1. Arch Ophthalmol. 1985; 103:1796–806.
3. Early Treatment Diabetic Retinopathy Study Research Group. Early photocoagulation for diabetic retinopathy. Early Treatment Diabetic Retinopathy Study Report No 9. Ophthalmology. 1991; 98:766–85.
4. Diabetic Retinopathy Study Research Group. DRS Report No. 3: four risk factors for severe visual loss in diabetic retinopathy. Arch Ophthalmol. 1979; 97:654–5.
5. McDonald HR, Schatz H. Macular edema following panretinal photocoagulation. Retina. 1985; 5:5–10.

6. Gardner TW, Eller AW, Friberg TR. Reduction of severe macular edema in eyes withpoor vision after panretinal photocoagulation for proliferative diabetic retinopathy. Graefes Arch Clin Exp Ophthalmol. 1991; 229:323–8.
7. Aroca PR, Salvat M, Fernández J, Méndez I. Risk factors for diffuse and focal macular edema. J Diabetes Complications. 2004; 18:211–5.

8. Yun CJ, Seon HB, Jong WK. Comparison of effects of IVTA and photocoagulation, depending on types of diabetic macular edema. J Korean Ophthalmol Soc. 2007; 45:655–63.
9. Panozzo G, Parolini B, Gusson E, et al. Diabetic macular edema: an OCT-based classification. Semin Ophthalmol. 2004; 19:13–20.

10. Shimura M, Yasuda K, Nakazawa T, et al. Quantifying alterations of macular thickness before and after panretinal photocoagulation in patients with severe diabetic retinopathy and good vision. Ophthalmology. 2003; 110:2386–94.

11. The Diabetic Retinopathy Study Research Group. DRS Report No.14: Indications for photocoagulation treatment of diabetic retinopathy. Int Ophthalmol Clin. 1979; 274:239–52.
12. McDonald HR, Schatz H. Visual loss following panretinal photocoagulation for proliferative diabetic retinopathy. Ophthalmology. 1985; 92:388–93.

13. Frank RN. Visual field and electroretinography following extensive photocoagulation. Arch Ophthalmol. 1975; 93:591–8.
14. Theodossiadis GP, Boudouri A, Georgopoulous G, Koutsandrea C. Central visual field changes after photocoagulation in proliferative diabetic retinopathy. Ophthalmologica. 1990; 201:71–8.
15. Tae GS, Mun YS, Jin HS. Short term clinical courses after panretinal photocoagulation treatment in diabetic retinopathy patients. J Korean Ophthalmol Soc. 2003; 44:1996–2003.
16. Choi KS, Chung JK, Lim SH. Laser photocoagulation combined with intravitreal triamcinolone acetonide injection in proliferative diabetic retinopathy with macular edema. Korean J Ophthalmol. 2007; 21:11–7.

17. Zein WM, Noureddin BN, Jurdi FA, et al. Panretinal photocoagulation and intravitreal triamcinolone acetonide for the management of proliferative diabetic retinopathy with macular edema. Retina. 2006; 26:137–42.

Go to : 
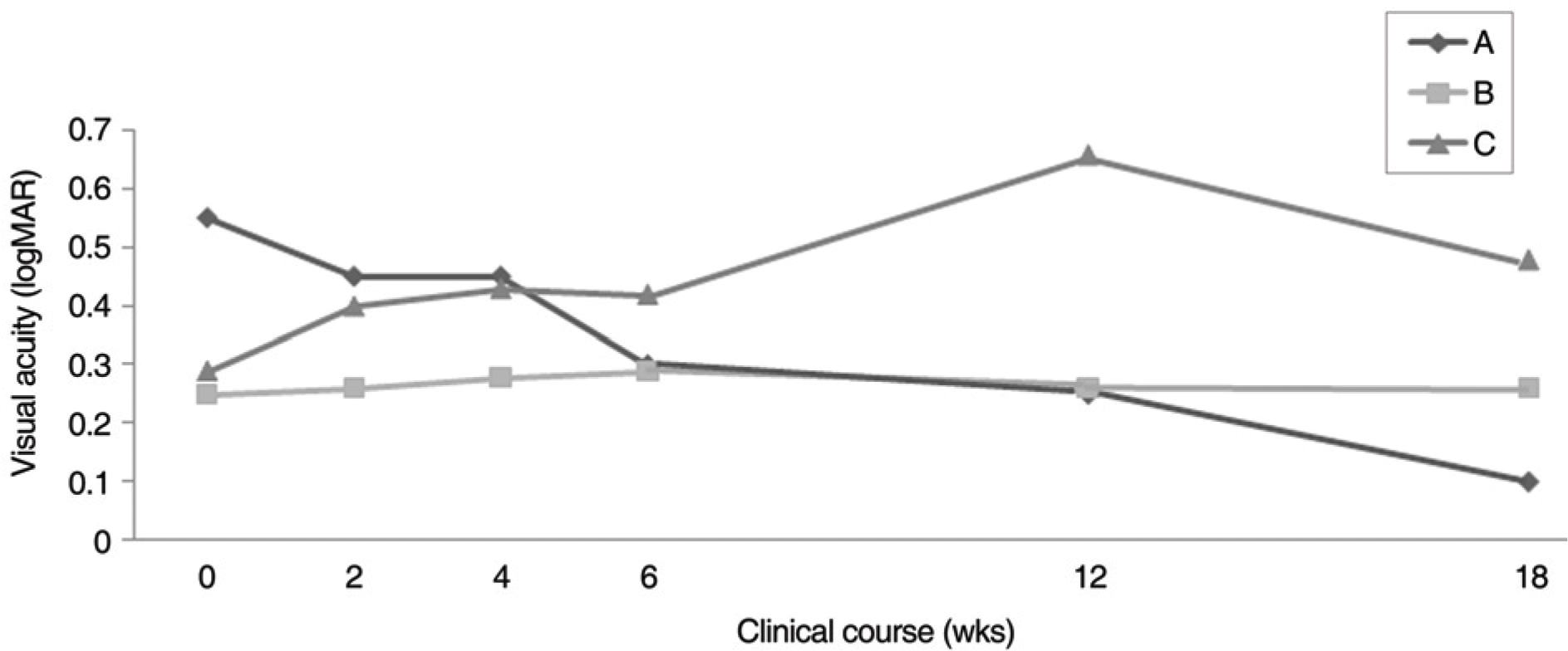 | Figure 1.Alteration of visual acuity. Two eyes (A) showed increase of visual acuity. Most eyes (29 eyes, B) maintained their visual acuity during the experimental period, and 9 eyes (C) showed decrease of visual acuity in this clinical course of 18 weeks. |
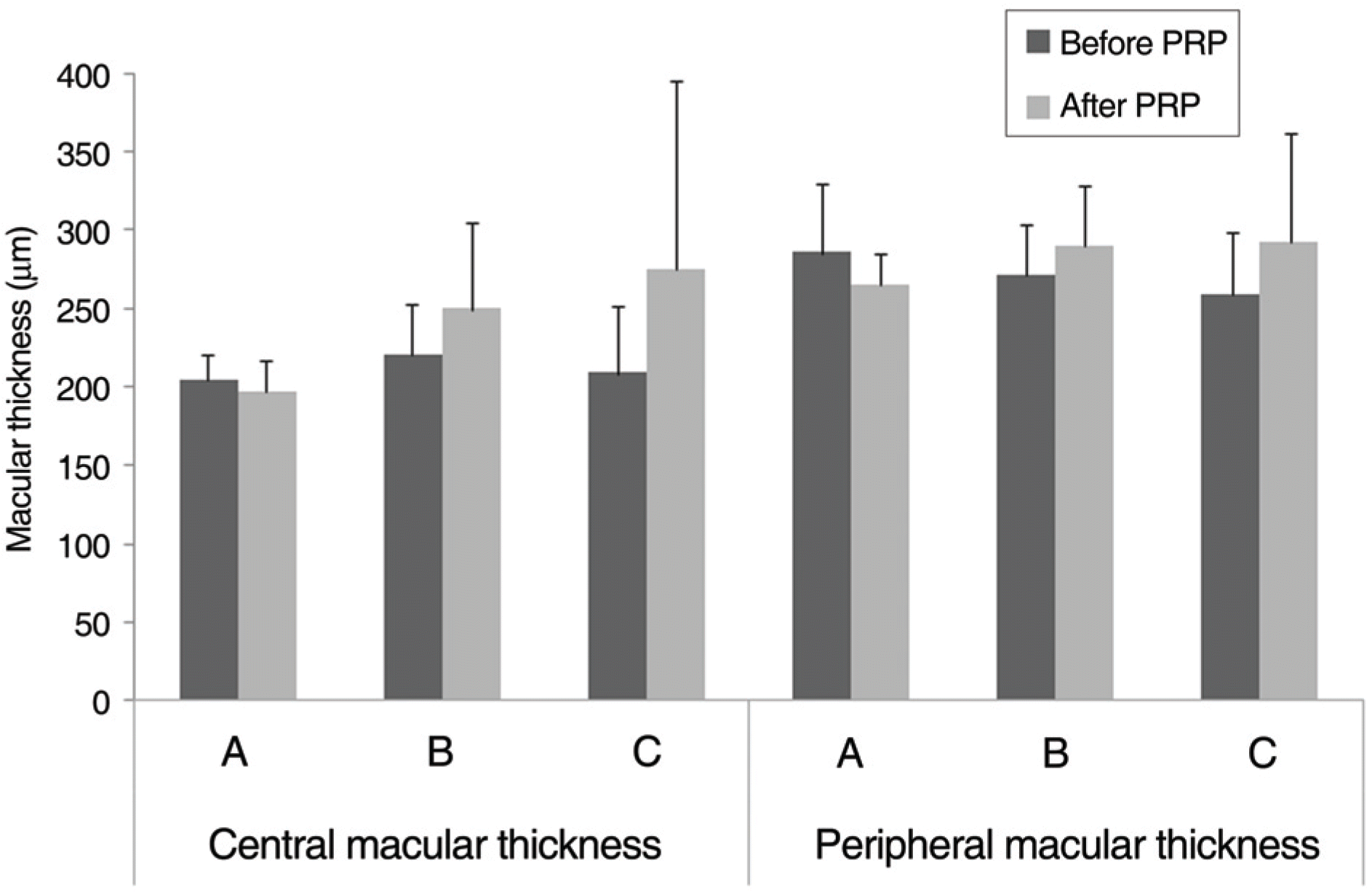 | Figure 2.Alterations of macular thickness before and 1.47 months after the last panretinal photocoagulation (PRP). Macular thickness of 2 eyes (A), which showed increase of visual acuity, decreased after PRP. Macular thickness of 29 eyes (B), which maintained their visual acuity during the experimental period, increased after PRP. Macular thickness of 9 eyes (C), which showed decrease of visual acuity, increased more than that of B after PRP. |
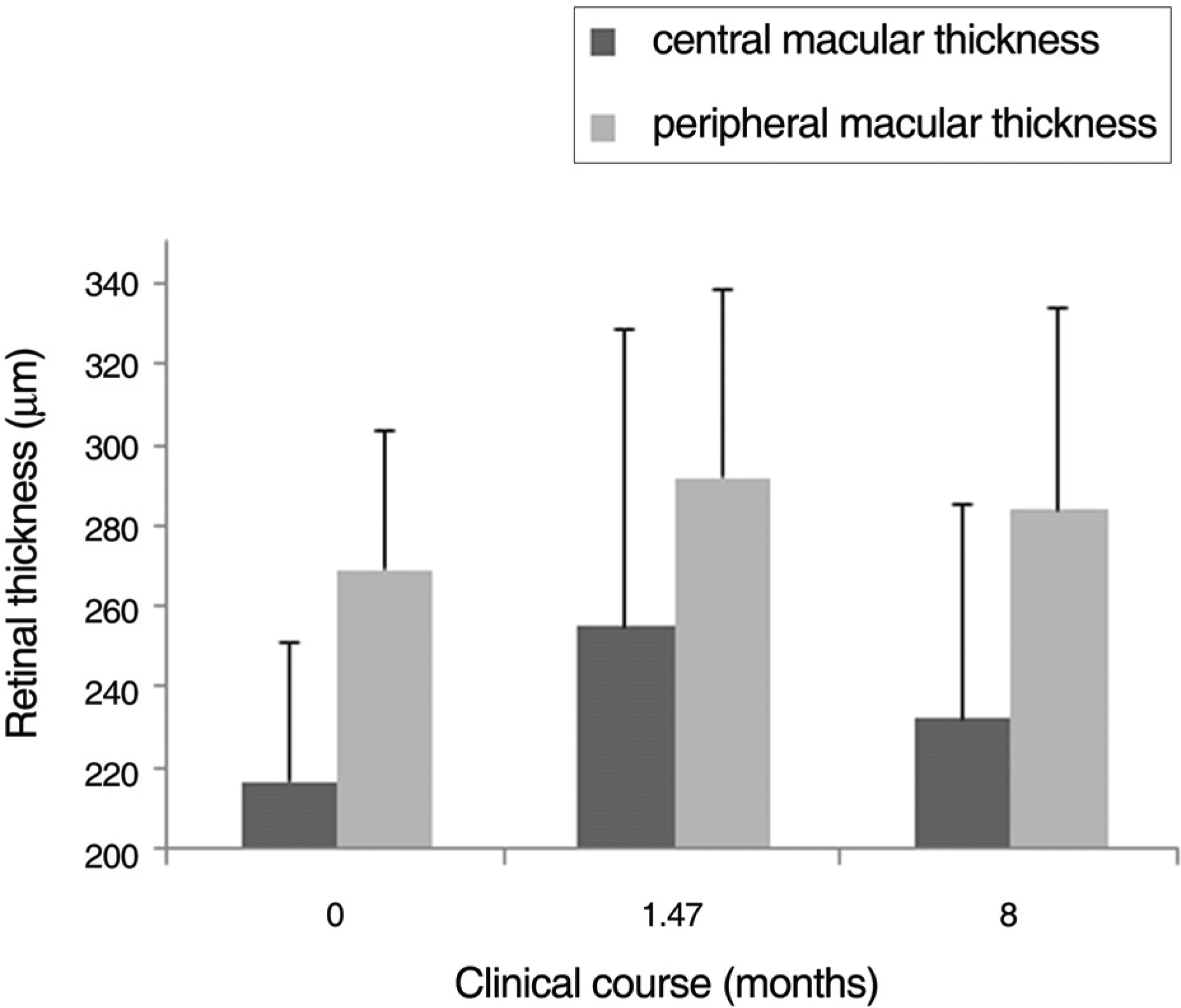 | Figure 3.Alterations of macular thickness before and after panretinal photocoagulation (PRP). Central and peripheral macular thickness increased 1.47 and 8 months after PRP. |
Table 1.
Characteristics of patients before panretina photocoagulation
| Number of eyes | 40 |
| Gender | |
| Male (eyes) | 27 |
| Female (eyes) | 13 |
| Age (years) | 54.15±8.25 (45∼72) |
| Type of DMR* | |
| NPDR† | 19 |
| PDR‡ | 21 |
| Duration of DMR (years) | 11.93±6.70 (1∼30) |
| Visual acuity (LogMAR) | 0.28±0.23 |
| Macular thickness | |
| Central (μm) | 216.98±34.09 |
| Peripheral (μm) | 269.26±34.59 |
Table 2.
Comparison of the visual acuity (VA) by glucose control, described by LogMAR scale
| HbA1c (mg/dL) | No. of eyes | VA before PRP* | VA after PRP* | p-value |
|---|---|---|---|---|
| ≤ 7.0 | 8 | 0.26±0.32 | 0.27±0.34 | 0.901 |
| > 7.0 | 16 | 0.24±0.22 | 0.28±0.27 | 0.475 |
Table 3.
Comparison of the macular thickness (MT) by glucose control
| | HbA1c (mg/dL) | No. of eyes | MT (μm) before PRP* | MT (μm) after PRP* | p-value |
|---|---|---|---|---|---|
| Central | ≤ 7.0 | 8 | 219.38±30.45 | 238.25±35.63 | 0.019 |
| > 7.0 | 16 | 210.13±27.30 | 228.31±29.46 | 0.039 | |
| Peripheral | ≤ 7.0 | 8 | 264.27±27.10 | 273.96±31.24 | 0.144 |
| > 7.0 | 16 | 269.17±32.70 | 285.11±28.00 | 0.003 |
Table 4.
Comparison of the macular thickness (MT) by hypertension
| | Hypertension | No. of eyes | MT (μm) before PRP* | MT (μm) after PRP* | p-value |
|---|---|---|---|---|---|
| Central | Well controlled | 11 | 213.00±36.25 | 222.82±29.78 | 0.198 |
| Poorly controlled | 16 | 216.50±27.07 | 257.81±86.74 | 0.101 | |
| Peripheral | Well controlled | 11 | 265.13±39.86 | 272.85±34.91 | 0.206 |
| Poorly controlled | 16 | 266.74±19.44 | 293.99±44.60 | 0.030 |
Table 5.
Comparison of the visual acuity (VA) by nephropathy, described by LogMAR scale
| | No. of eyes | VA before PRP* | VA after PRP* | p-value |
|---|---|---|---|---|
| No nephropathy | 25 | 0.33±0.19 | 0.36±0.22 | 0.627 |
| Nephropathy | 15 | 0.19±0.28 | 0.29±0.34 | 0.044 |
Table 6.
Compairson of the macular thickness (MT) by nephropathy
| | Hypertension | No. of eyes | MT (μm) before PRP* | MT (μm) after PRP* | p-value |
|---|---|---|---|---|---|
| Central | No nephropathy | 25 | 216.16±33.97 | 252.48±62.86 | 0.001 |
| Nephropathy | 15 | 218.33±35.45 | 259.80±90.55 | 0.127 | |
| Peripheral | No nephropathy | 25 | 272.65±36.33 | 291.64±44.67 | 0.003 |
| Nephropathy | 15 | 263.61±31.86 | 292.49±50.99 | 0.033 |
Table 7.
Comparison of the macular thickness (MT) by PRP spots
| | No. of PRP* spot | No. of eyes | MT (μm) before PRP* | MT (μm) after PRP* | p-value |
|---|---|---|---|---|---|
| Central | 1600≤ | 21 | 213.26±29.58 | 238.32±43.62 | 0.001 |
| 1600> | 19 | 220.33±38.13 | 270.52±90.97 | 0.023 | |
| Peripheral | 1600≤ | 21 | 267.02±37.50 | 280.55±33.52 | 0.011 |
| 1600> | 19 | 271.28±32.52 | 302.28±54.48 | 0.005 |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download