Abstract
Purpose
To evaluate the usefulness of imaging diagnosis in patients with atypical oculomotor abnormalities and paralytic strabismus.
Methods
The magnetic resonance imaging (MRI) or computed tomography (CT) of 3 patients with atypical Y pattern vertical incomitance and medial rectus (MR) paresis after MR impingement reduction and A pattern vertical incomitance were analyzed. High-resolution, surface coil MRI was used to obtain sets of contiguous, 2-mm thick quasi-coronal images in 9-cardinal gaze directions. Digital image analysis was used to evaluate the results.
Results
MRI revealed lateral displacement of the superior rectus (SR) and inferior displacement of the lateral rectus (LR) during upper temporal gaze and inferior displacement of the LR during lateral gaze in patients with Y pattern vertical incomitance. In patients with MR paresis, the maximal surface area of MR cross section is in the image plane 10 mm posterior from the orbital center at primary gaze. The maximal surface area of MR cross section is in the image plane 22 mm posterior from the orbital center during medial gaze. Quasi-coronal images show that contraction tends to cause the plane of maximum cross-section to move posteriorly. Surgical treatment was avoided and observational treatment maintained. There is incyclotorsion of both extraocular muscles in patients with A pattern vertical incomitance and upslanted palpebral fissure.
Go to : 
References
1. Koornneef L. New insights in the human orbital connective tissue: results of a new anatomical approach. Arch Ophthalmol. 1977; 95:1269–73.
2. Demer JL, Miller JM, Poukens V, et al. Evidence for fibromu-scular pulleys of the recti extraocular muscles. Invest Ophthalmol Vis Sci. 1995; 36:1125–36.
3. Porter JD, Poukens V, Baker RS, Demer JL. Structure-function correlations in the human medial rectus extraocular muscle pulleys. Invest Ophthalmol Vis Sci. 1996; 37:468–72.
4. Kono R, Clark RA, Demer JL. Active pulleys: Magnetic resonance imaging of rectus muscle paths in tertiary gazes. Invest Ophthalmol Vis Sci. 2002; 43:2179–88.
5. Miller JM, Robins D. Extraocular muscle side-slip and orbital geometry in monkeys. Vision Res. 1987; 27:381–92.

6. Demer JL. Pivotal role of orbital connective tissues in binocular alignment and strabismus. Invest Ophthalmol Vis Sci. 2004; 45:729–38.
7. Heo H, Park SW, Park YG. The study of normal intraorbital positions of the rectus muscles. J Korean Ophthalmol Soc. 2005; 46:1675–83.
8. Clark RA, Miller JM, Demer JD. Location and stability of rectus muscle pulleys: muscle paths as a function of gaze. Invest Ophthalmol Vis Sci. 1997; 38:227–40.
9. Miller JM. Functional anatomy of normal human rectus muscle. Vision Res. 1989; 29:223–40.
10. Clark RA, Miller JM, Demer JL. Three-dimensional location of human rectus pulleys by path inflections in secondary gaze positions. Invest Ophthalmol Vis Sci. 2000; 41:3787–97.
12. Demer JL, Oh SY, Poukens V. Evidence for active control of rectus extraocular muscle pulleys. Invest Ophthalmol Vis Sci. 2000; 41:1280–90.
13. Demer JL. The orbital pulley system: A revolution in concepts of orbital anatomy. Ann N Y Acad Sci. 2002; 956:17–32.

14. Clark RA, Miller JM, Rosenbaum AL, Demer JL. Heterotopic muscle pulleys or oblique muscle dysfunction. J AAPOS. 1998; 2:17–25.

15. Clark RA, Demer JL. Rectus extraocular muscle pulley displacement after surgical transposition and posterior fixation for treatment of paralytic strabismus. Am J Ophthalmol. 2002; 133:119–28.
16. Oh SY, Clark RA, Velez F, Rosenbaum AL. Incomitant strabismus associated with instability of rectus pulleys. Invest Ophthalmol Vis Sci. 2002; 43:2169–78.
17. Clark RA, Ariyasu R, Demer JL. Medial rectus pulley posterior fixation is as effective as scleral posterior fixation for acquired esotropia with a high AC/A ratio. Am J Ophthalmol. 2004; 137:1026–33.

18. Demer JL, Miller JM. Clinical strabismus management, principles and surgical techniques. 1st ed.Philadelphia: WB Saunders;1999. p. 84–98.
Go to : 
 | Figure 1.(A) Preoperative 9-cardinal photograph shows 40PD of Y-pattern exotropia. (B) Postoperative 9-cardinal photograph shows no improvement of Y-pattern exotropia (postoperative 3 months). (C) Postoperative 9-cardinal photograph shows improvement of Y-pattern vertical incomitance (second postoperative 3 months). |
 | Figure 2.(A) Preoperative 9-cardinal photograph shows medial rectus motility limitation of the right eye. (B) Postoperative 9-cardinal photograph shows orthotropia in primary position and no motility restriction (postoperative 4 months). |
 | Figure 3.(A) Preoperative 9-cardinal photograph shows 25PD of A-pattern exotropia and 25PD of left hypertropia. (B) Orbital MRI image shows incyclotorsion of both extraocular muscles and mucocele involved both the frontal and ethmoid sinuses. |
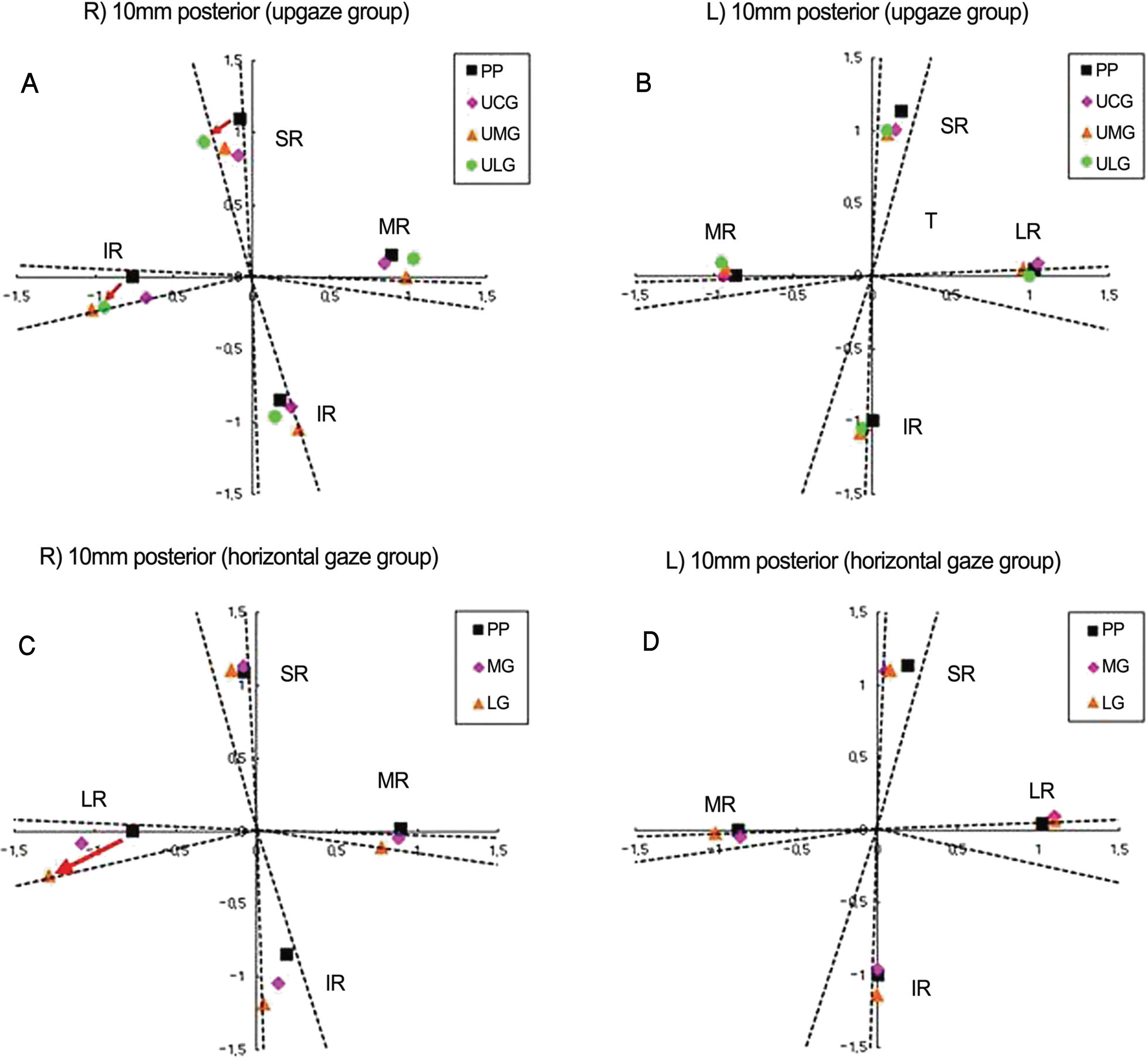 | Figure 4.(A, B) Diagram of 4 rectus muscles position in upper lateral gaze, upgaze, upper medial gaze and primary position. (C, D) Diagram of 4 rectus muscles position in lateral, medial gaze and primary position. (A) Note the lateral displacement of SR (red arrow) and inferior displacement of LR (red arrow) in upper lateral gaze (right eye). (B) Note the minimal rectus muscles shift during upgaze (left eye). (C) Note the inferior displacement of LR (red arrow) in lateral gaze (right eye). (D) Note the minimal rectus muscle pulleys shift during horizontal gaze (left eye). PP=primary position; UCG=upper central gaze; UMG=upper medial gaze; ULG=upper lateral gaze; MG= medial gaze; LG=lateral gaze. |
 | Figure 5.Quasi-coronal images of right orbit in primary position and medial gaze in a patient, who underwent medial rectus impingement reduction surgery (postoperative 2 months). (A) 10 mm posterior to the orbital center at primary gaze. (B) 10 mm posterior to the orbital center at medial gaze. (C) 22 mm posterior from the orbital center at primary gaze. (D) 22 mm posterior from the orbital center in medial gaze. At primary position the maximal surface area or medial rectus (MR) cross section is in image plane 10 mm posterior from the orbital center. In medial gaze the maximal surface area of MR cross section is in image plane 22 mm from the orbital center. Quasi-coronal images show that contraction tends to cause the planes of maximum cross-section to move posteriorly. |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download