Abstract
Purpose
Forty patients who maintained a clear cornea for at least 20 years after receiving penetrating keratoplasty (PKP) were evaluated to determine favorable prognostic factors of PKP.
Methods
Among 78 patients who underwent PKP before 1986, 40 patients continue to maintain clear corneas in 2008. Demographic features of the recipients and the donors, along with underlying diseases causing blindness, the trephine size of the donor and recipient corneas, suturing methods, preoperative and postoperative visual acuity, and cause of death of the donors were evaluated retrospectively. The criteria of clear cornea maintenance was based on patient medical records.
Results
Among those patients maintaining clear corneas 20 years after PKP, females outnumbered male patients by 25 patients more. Patients who underwent the operation in their twenties had the highest success rates. The most common condition necessitating PKP was keratoconus, followed by traumatic corneal opacity and herpes keratitis in descending order of frequency. Female donors exceeded male donors in number. Most donors were aged 60 years or older, and the most common cause of donor death was accident. The most frequently used trephine size was 7.0 mm for the recipient and 7.5 mm for the donor, and continuous suture was used more often than interrupted suture. Patients who preserved clear corneas for at least 20 years after PKP displayed a preoperative visual acuity of counting fingers at 30 cm, which improved to 0.11 after the operation.
References
1. Paton RT. Keratoplasty. New York: The Blakiston Division McGraw-Hill Book Co., Inc.;1955. p. 4–35.
2. Uhm SL, Chung SK, Rhee SW, Myung YW. Clinical Analysis of Keratoplasty over a 23 Year-Time Span. J Korean Ophthalmol Soc. 1991; 32:421–9.
3. Ha D, Kim CK, Lee SE. . Penetration keratoplasty results in 275 cases. J Korean Ophthalmol Soc. 2001; 42:20–9.
4. Lee SJ, Cho EY, Kim MS. Clinical Outcomes 10 Years after Penetrating Keratoplasty. J Korean Ophthalmol Soc. 2006; 47:1043–8.
5. Krachmer JH, Alldredge OC. Subepithelial infiltrates: a probable sign of corneal transplant rejection, Arch Ophthalmol. 1978; 96:2234–7.
6. Alldredge OC, Krachmer JH. Clinical types of corneal transplant rejection: their manifestations, frequency, preoperative correlates and treatment, Arch Ophthalmol. 1981; 99:599–604.
7. Irvine AR, Kaufman HE. Intraocular pressure following penetrating keratoplasty, Am J Ophthalmol. 1969; 68:835–44.
8. Goldberg DB, Schanzlin DJ, Brown SI. Insidence of increased intraocular pressure after keratoplasty, Am J Ophthalmol. 1981; 92:372–7.
9. Charlin R, Polack FM. The effect of elevated intraocular pressure on the endothelium of corneal grafts. Cornea. 1982; 1:241–9.

10. Olivares Jiménez JL, Guerrero Jurado JC, Bermudez Rodriguez FJ, Serrano Laborda D. Keratoconus: age of onset and natural history. Optom Vis Sci. 1997; 74:147–51.
11. Kennedy RH, Bourne WM, Dyer JA. A 48-year clinical and epidemiologic study of keratoconus, Am J Ophthalmol 1986; 101. 267–73.
12. Kim JH. Advances in Keratoplasty. Off J Res Med Sci Korea. 1975; 7:91–107.
13. Beauchamp GR. Pediatric keratoplasty: problems in management, J Pediatr Ophthalmol Strabismus. 1979; 16:388–94.
14. Stulting RD, Sumers KD, Cavanagh HD. . Penetrating keratoplasty in children. Ophthalmology. 1984; 91:1222–30.

15. Panda A, Mohan M, Venkateswarlu K, Gupta AK. Keratoplasty in children. Ann Ophthalmol. 1988; 20:183–7.
16. Dana MR, Moyes AL, Gomes JA. . The indications for and outcome in pediatric keratoplasty: a multicenter study, Ophthalmology. 1995; 102:1129–38.
17. Kim MK, Lee JH. Long-term outcome of graft rejection after penetrating keratoplasty. J Korean Ophthalmol Soc. 1997; 38:1553–60.
18. Schönherr U, Martus P, Händel A, Naumann GO. Transplant reaction after keratoplasty for keratoconus. Frequency and risk factors. Ophthalmology. 1996; 93:227–31.
19. Buxton JN, Westphalen JA. Indications and contraindications. Brightbill FS, editor. Corneal Surgery. 2nd. St. Louis: Mosby;1993. v. 1. chap. 32.
20. Jang HS, Song SW, Kim BY. Prognosis and survival rate of penetrating keratoplasty in corneal dystrophy and corneal degeneration. J Korean Ophthalmol Soc. 2002; 43:941–7.
21. Myoung YW, Song SW, Park CK. A clinical study of risk factors of graft rejection for penetrating keratoplasty. J Korean Ophthalmol Soc. 1996; 37:1095–104.
22. Küchle M, Cursiefen C, Nguyen NX. . Risk factors for corneal allograft rejection: intermediate results of a prospective normal-risk keratoplasty study. Graefes Arch Clin Exp Ophthalmol. 2002; 240:580–4.

23. Reinhard T, Sundmacher R, Heering P. Systemic cyclosporine A in high-risk keratoplasties. Graefes Arch Clin Exp Ophthalmol. 1996; 234:S115–21.
24. Hill JC. Systemic cyclosporin in high-risk keratoplasty: Short versus long-term therapy. Ophthalmology. 1994; 101:128–33.
25. Biosjoly HM, Bernard PM, Dubé I. . Effect of factors unrelated to tissue matching on corneal transplant endothelial rejection. Am J Ophthalmol. 1989; 107:647–54.
26. Sanfilippo F, Macqueen JM, Vaughn WK, Foulks GN. Reduced graft rejection with good HLA-A and B matching in high risk corneal transplantions. N Engl J Med. 1986; 315:29–35.
27. Seo JS, Jeong SK, Yang KJ, Park YG. Clinical evaluation of the graft rejection after penetrating keratoplasty. J Korean Ophthalmol Soc. 1997; 38:1121–7.
28. Krachmer JH, Mannis MJ, Holland EJ. Therapeutic keratoplasty: Cornea, 2nd ed. Vol. 2. St. Louis: Mosby,. 2000; 1695–707.
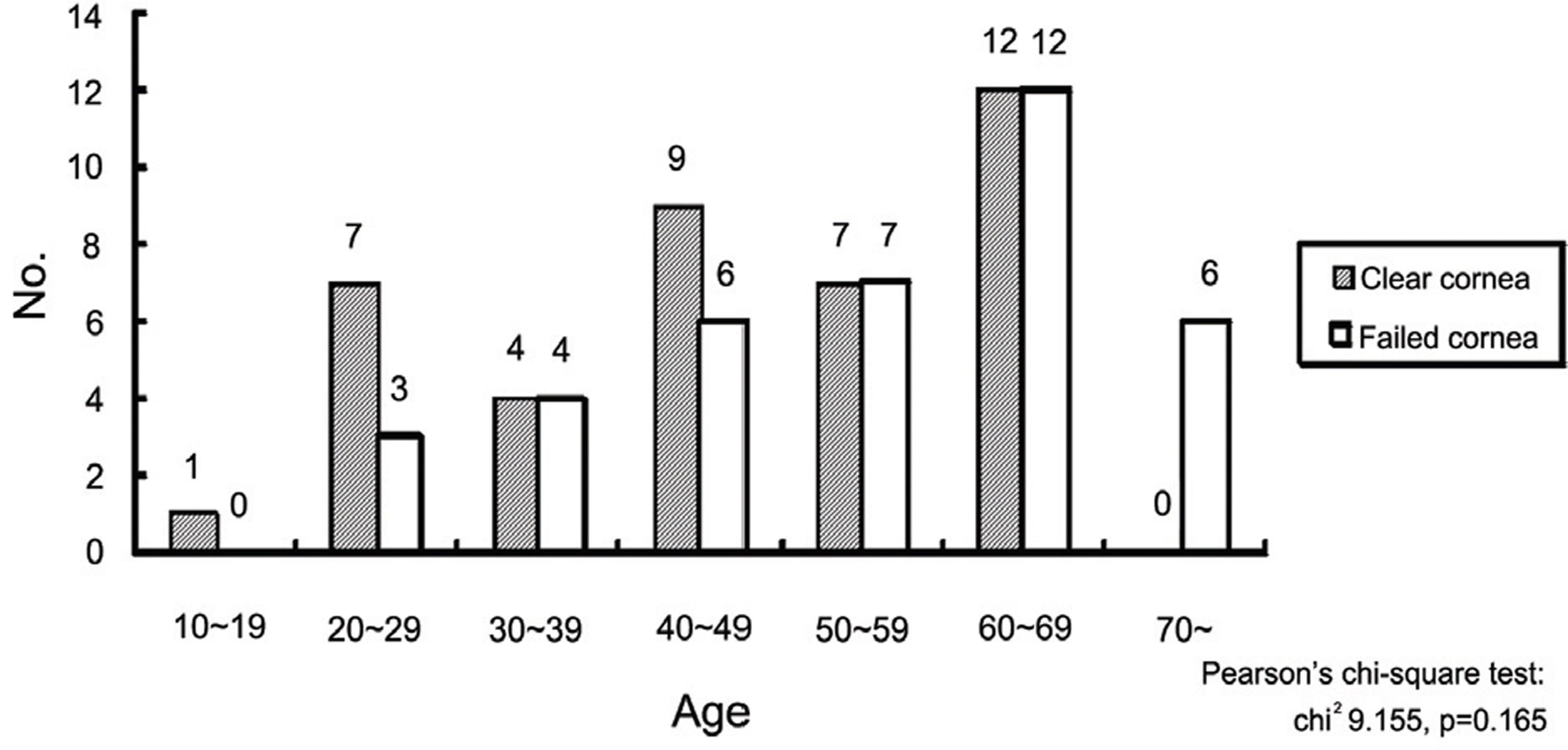
Figure 1.
Age distribution of the patients. (Recipient); In the clear cornea group, 20s were most common, while in the failed cornea group, 60s were most common.
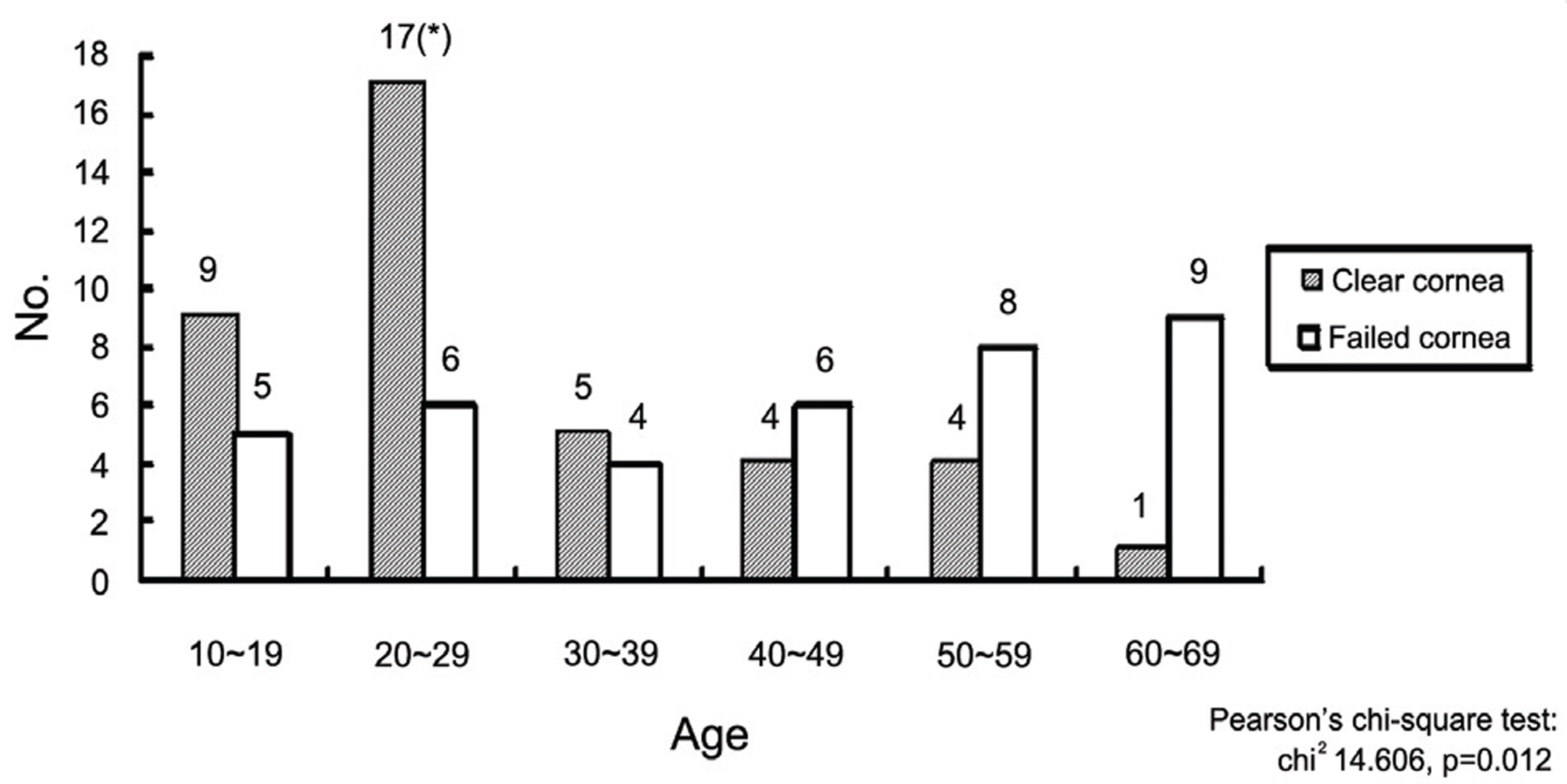
Figure 2.
Sex distribution of the patients. (Recipient); Females were more common in the clear cornea group, while males were more common in the failed cornea group.
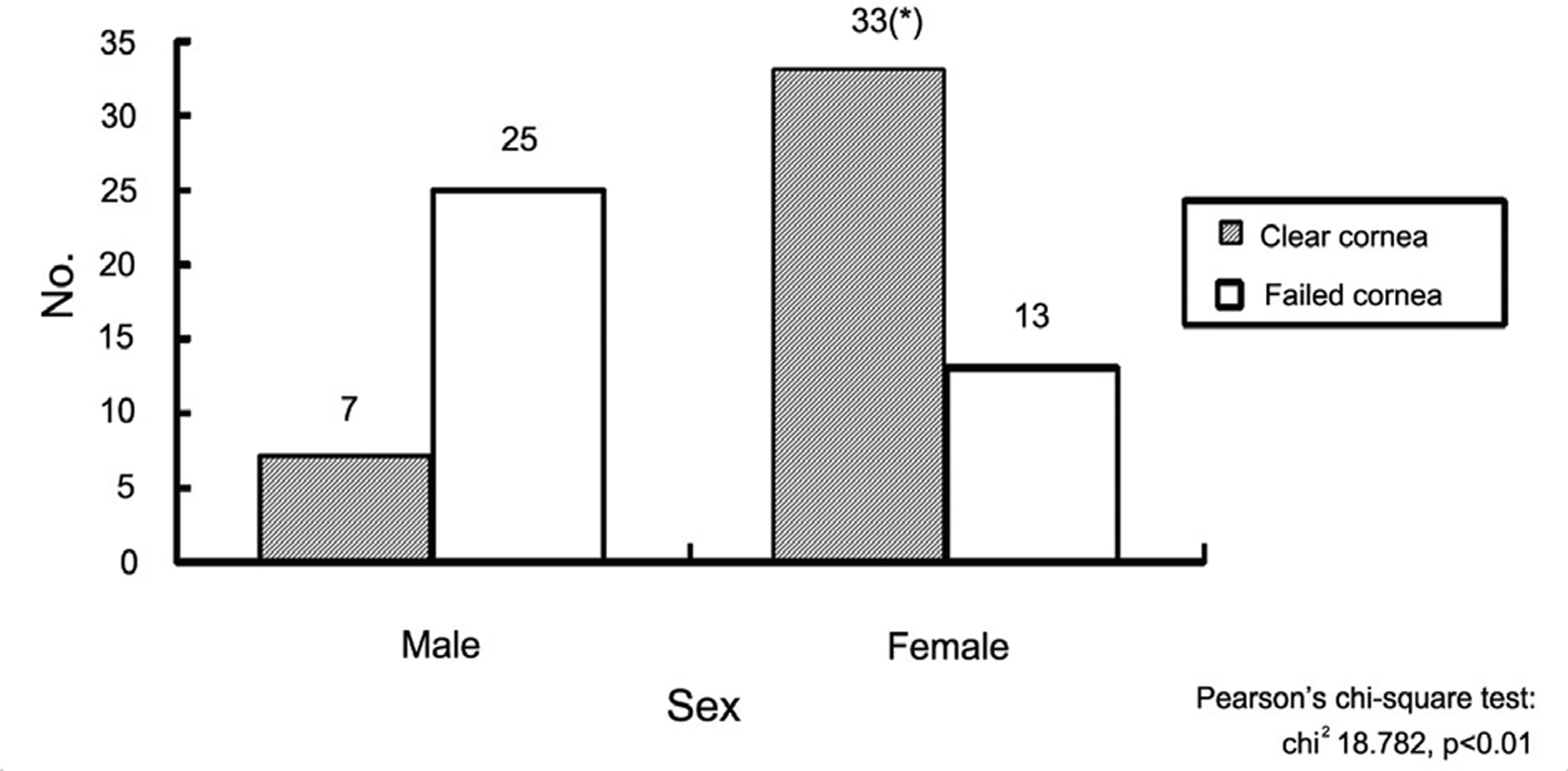
Figure 5.
Trephine size of donor’s cornea; The most common used donor’s trephine size was 7.5 mm in both groups.
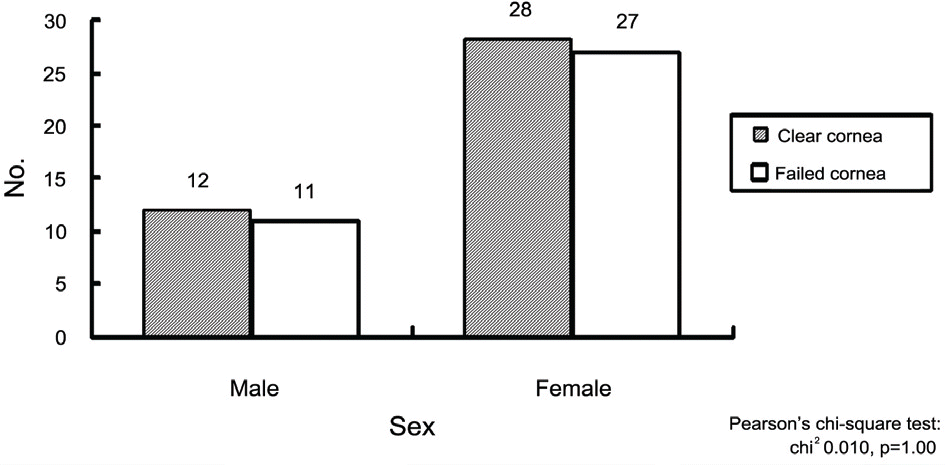
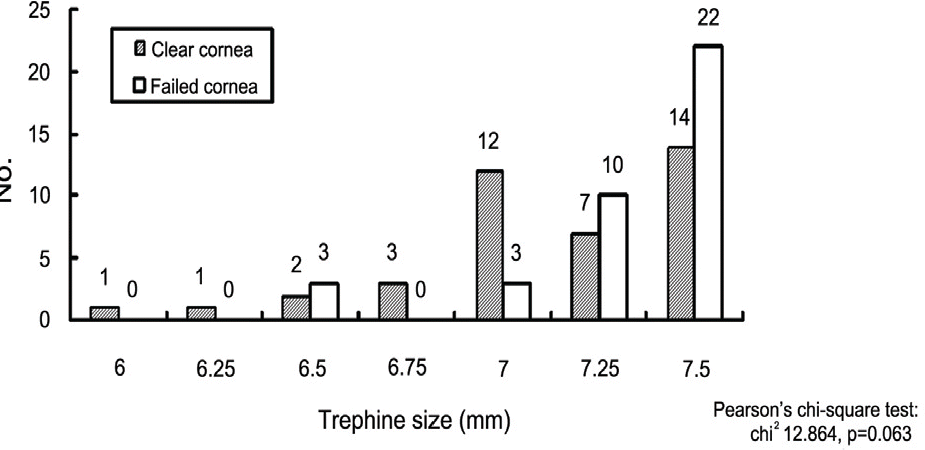
Figure 6.
Trephine size of recipient's cornea; The most common used recipients’ trephine size was 7.0 mm in both groups.
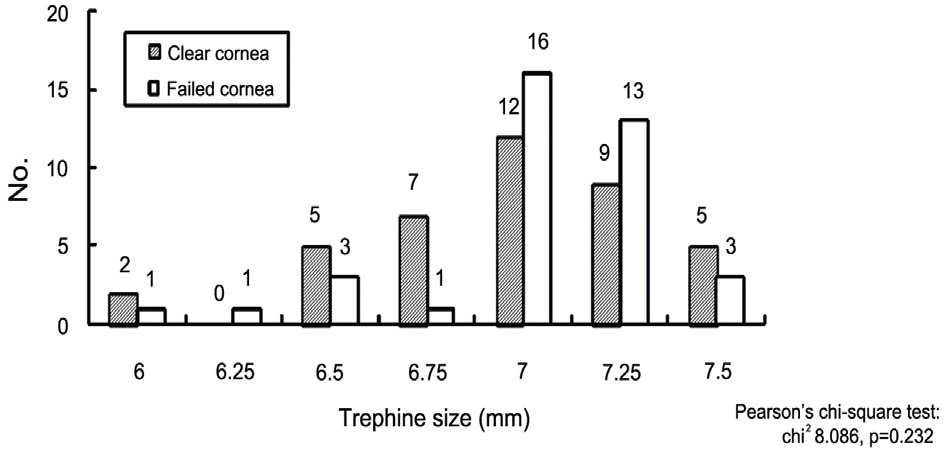
Figure 11.
Change of visual acuity after the PPKP; In the clear cornea group, 26 patients improved the visual acuity while, 14 patients had no change in visual acuity after PPKP. In the failed group, 20 patients improved, while 6 patients had no change and even 12 patients had a decrease in visual acuity after PPKP.
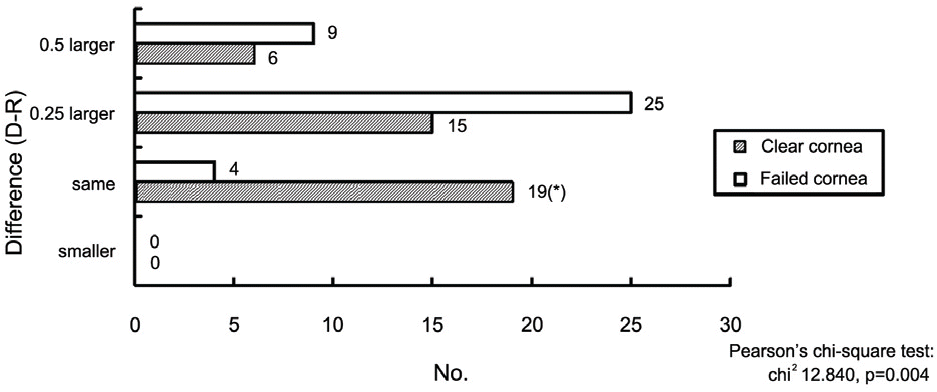
Figure 12.
Duration of clear cornea in the failure group; In the failed group, most of the patients had the problems that affect the corneal transparency within 1 year after PPKP.
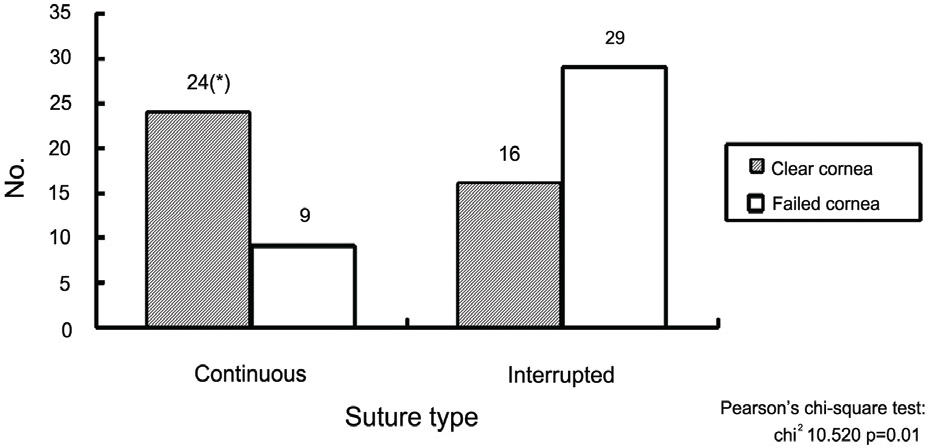
Figure 7.
Difference in trephine size between donor and recipient; In the clear cornea group, 19 patients had no difference between donor and recipient’s trephine size. While in failed group. 25 patients had 0.25 mm larger donor’s trephine than recipient’s.
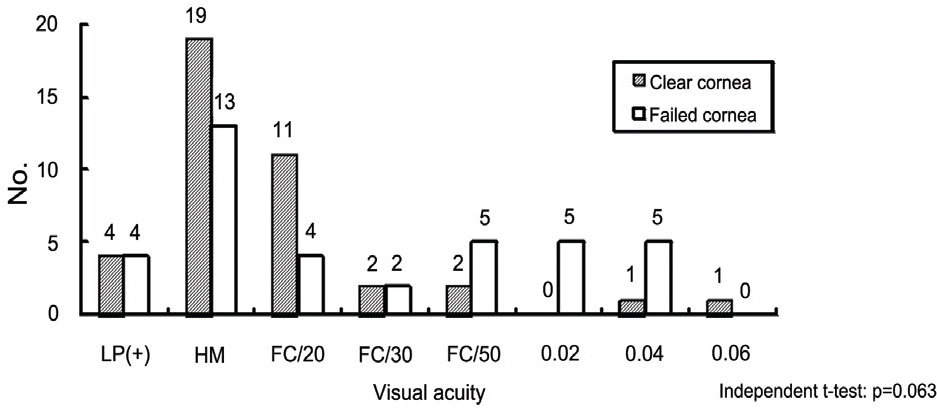
Figure 9.
Preoperative visual acuity of the donor; Most common preoperative visual acuity is hand motion in both groups. The average visual acuity in the clear cornea group was FC/30 cm, while in the failed group was 0.010±0.013.
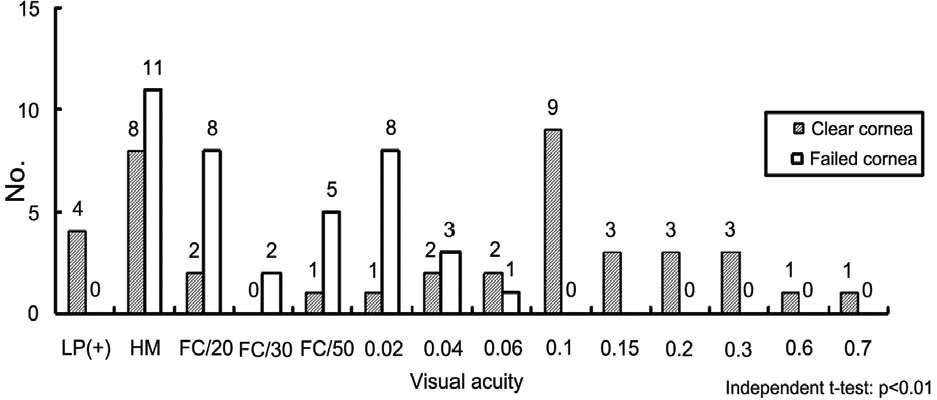
Figure 8.
Suture type; In the clear cornea group, a continuous suture was more commonly used, while, in the failed group, interrupted suture was used often.
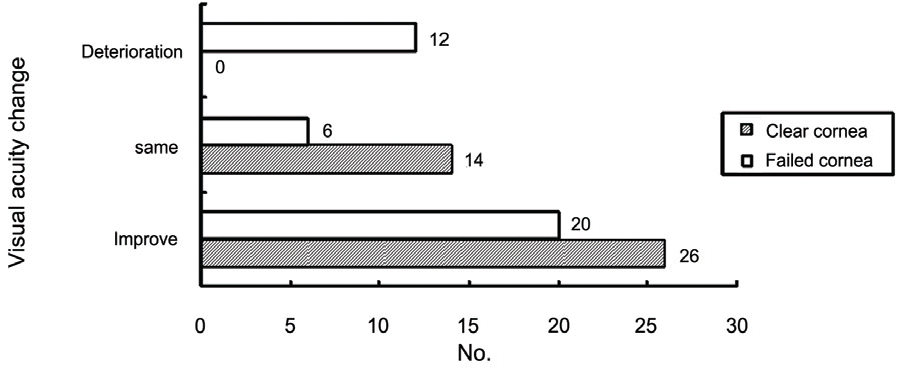
Figure 10.
Postoperative visual acuity of the donor; The average visual acuity in the clear cornea group was 0.11±0.15, while in the failed group was 0.011±0.014.
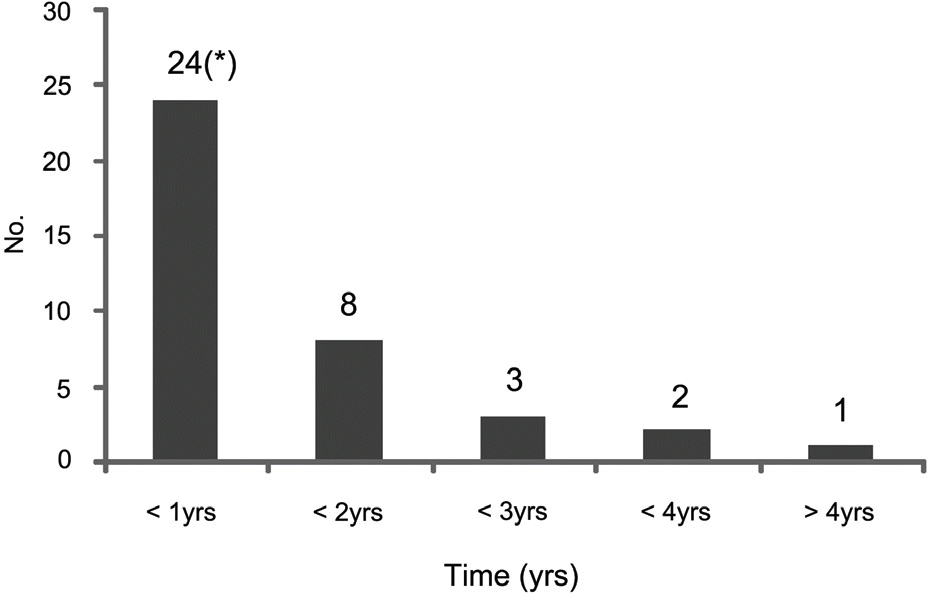
Table 1.
Demography of the study
∗ Statistically significant; Independent t-test was used to evaluate the difference between 2 groups in age of recipient and donor, preoperative visual acuity and postoperative visual acuity, while Pearson’s chi-square test was used in trephine size comparision of donor and recipient between 2 groups; P<0.05 for the difference between the 2 groups.
Table 2.
Preoperative diagnosis of recipients
| Diagnosis | Clear cornea | Failed cornea | p-value |
|---|---|---|---|
| Keratoconus | 10 | 2 | 0.021∗ |
| Trauma | 9 | 9 | 1.00 |
| Recurrent herpes keratits | 7 | 7 | 1.00 |
| Bullous keratopathy | 6 | 5 | 0.763 |
| Corneal dystrophy | 4 | 5 | 0.739 |
| Corneal ulcer | 2 | 4 | 0.414 |
| Graft failure | 2 | 6 | 0.157 |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download