Abstract
Purpose
To compare macular thickness measurements obtained from time domain optical coherence tomography (TD-OCT) and 2 spectral domain (SD) OCTs and to evaluate their repeatability and agreement in normal subjects and diabetic macular edema patients.
Methods
Fifty-four healthy, normal subjects and 26 diabetic macular edema patients were participated in this study. In a randomly selected eye from each subject, two serial macular measurements were obtained from TD-OCT (Stratus OCT) and SD-OCTs (Cirrus HD-OCT, Spectralis HRA+OCT) by an experienced technician in random order. Nine areas of macular thickness map and repeatabilities obtained by the 3 OCTs were compared.
Results
In relative repeatability, SD-OCT showed better results overall compared to TD-OCT. Macular thickness was greatest in the Spectralis HRA+OCT in both normal subjects and diabetic macular edema patients, followed by Cirrus HD-OCT and Stratus OCT. In normal subjects, regardless of the type of comparison between the machines there was a statistically significant difference in all 9 areas.
Conclusions
While the TD-OCT and the 2 SD-OCTs are reliable for macular thickness measurement, SD-OCT has better measurement repeatability compared with TD-OCT. Because macular measurements obtained from the 3 OCT systems cannot be interchanged, an effort should be made to standardize the measurement of each system.
References
1. Drexler W, Fujimoto JG. State-of-the-art retinal optical coherence tomography. Prog Retin Eye Res. 2008; 27:45–88.

2. van Velthoven ME, Faber DJ, Verbraak FD, et al. Recent developments in optical coherence tomography for imaging the retina. Prog Retin Eye Res. 2007; 26:57–77.

3. Gupta V, Gupta P, Singh R, et al. Spectral-Domain Cirrus High-Definition Optical Coherence Tomography Is Better than Time-Domain Stratus Optical Coherence Tomography for Evaluation of Macular Pathologic Features in Uveitis. Am J Ophthalmol. 2008; 145:1018–22.

4. Leung CK, Chan WM, Yung WH, et al. Comparison of macular and peripapillary measurements for the detection of glaucoma: an optical coherence tomography study. Ophthalmology. 2005; 112:391–400.
5. Kanadani FN, Hood DC, Grippo TM, et al. Structural and functional assessment of the macular region in patients with glaucoma. Br J Ophthalmol. 2006; 90:1393–7.

6. Chen TC, Cense B, Pierce MC, et al. Spectral Domain Optical Coherence Tomotraphy: Ultra-high Speed, Ultra-high Resolution Ophthalmic Imaging. Arch Ophthalmol. 2005; 123:1715–20.
7. Yi K, Chen TC, de Boer JF. Spectral domain optical coherence tomography. Techniques in Ophthalmology. 2006; 4:170–4.

8. Age-Related Eye Disease Study Group. The Age-Related Eye Disease Study Sevberity Scale for Age Related Macular Degeneration: Areds Report No. 17. Arch Ophthalmol. 2005; 123:1484–98.
9. Bland JM, Altman DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet. 1986; 1:307–10.

10. Bland JM, Altman DG. Comparing methods of measurement: why plotting difference against standard method is misleading. Lancet. 1995; 346:1085–7.

11. Leung CK, Cheung CY, Weinreb RN, et al. Comparison of Macular Thickness Measurements between Time Domain and Spectral Domain Optical Coherence Tomography. Invest Ophthalmol Vis Sci. 2008; 49:4893–7.

12. Kakinoki M, Sawada O, Sawada T, et al. Comparison of macular thickness between Cirrus HD-OCT and Stratus OCT. Ophthalmic Surg Lasers Imaging. 2009; 40:135–40.

13. Forooghian F, Cukras C, Meyerle CB, et al. Evaluation of Time Domain and Spectral Domain Optical Coherence Tomography in the Measurement of Diabetic Macular Edema. Invest Ophthalmol Vis Sci. 2008; 49:4290–6.

14. Massin P, Vicaut E, Haouchine B, et al. Reproducibility of retinal mapping using optical coherence tomography. Arch Ophthalmol. 2001; 119:1135–42.

15. Polito A, Del Borrello M, Isola M, et al. Repeatability and reproducibility of fast macular thickness mapping with stratus optical coherence tomography. Arch Ophthalmol. 2005; 123:1330–7.

16. Gurses-Ozden R, Teng C, Vessani R, et al. Macular and retinal nerve fiber layer thickness measurement reproducibility using optical coherence tomography (OCT-3). J Glaucoma. 2004; 13:238–44.
Figure 1.
AREDS grid at right used for reporting retinal thickness (F=fovea; S1=superior inner;, N1=nasal inner; I1=inferior inner; T1=temporal inner; S2=superior outer; N2=nasal outer; I2: inferior outer; T2=temporal outer).
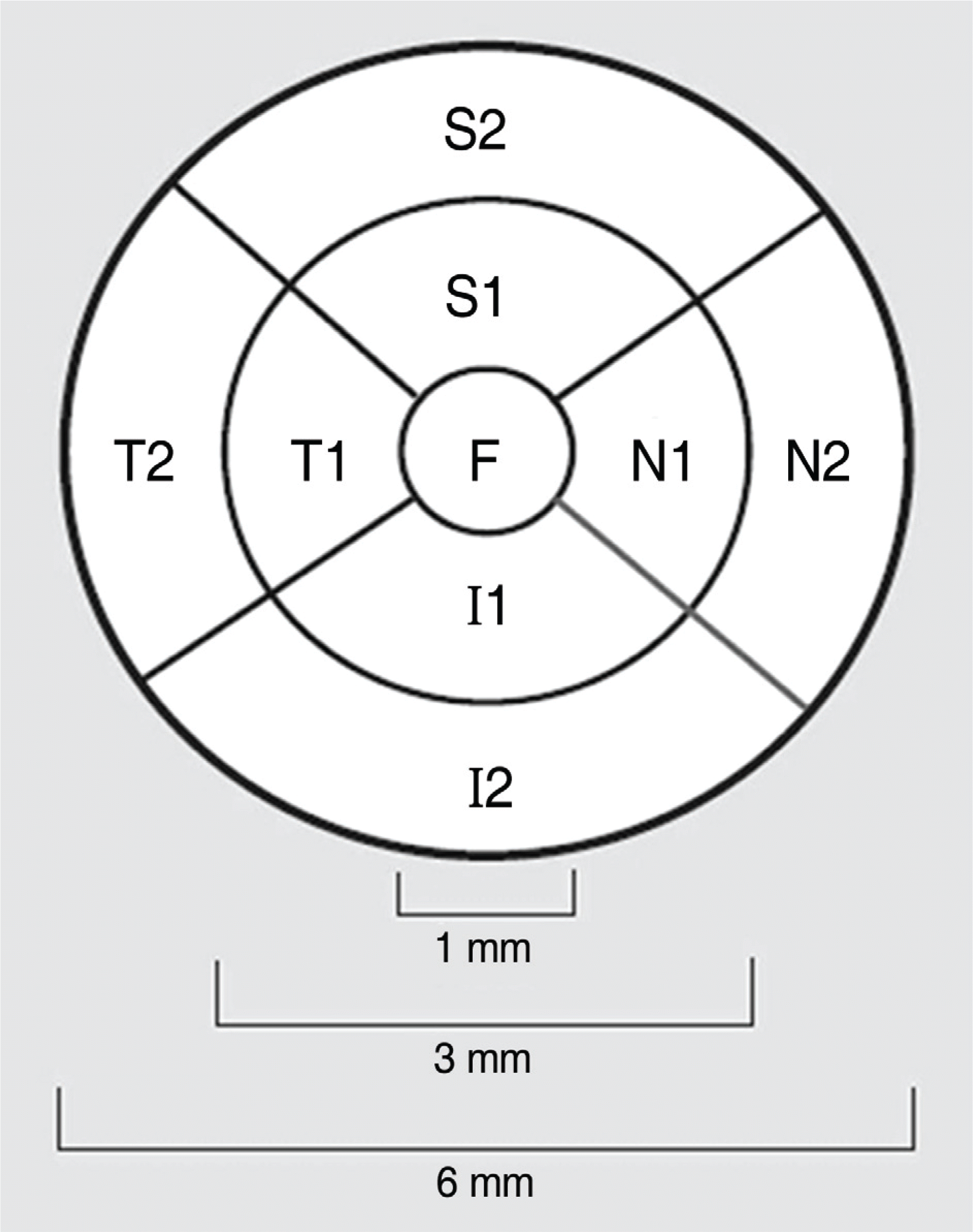
Figure 2.
Comparison of macular thickness among the three OCTs in nine areas (A=normal; B=diabetic macular edema) (F=fovea; S1=superior inner; N1= nasal inner; I1=inferior inner; T1=temporal inner; S2=superior outer; N2=nasal outer; I2=inferior outer; T2=temporal outer).
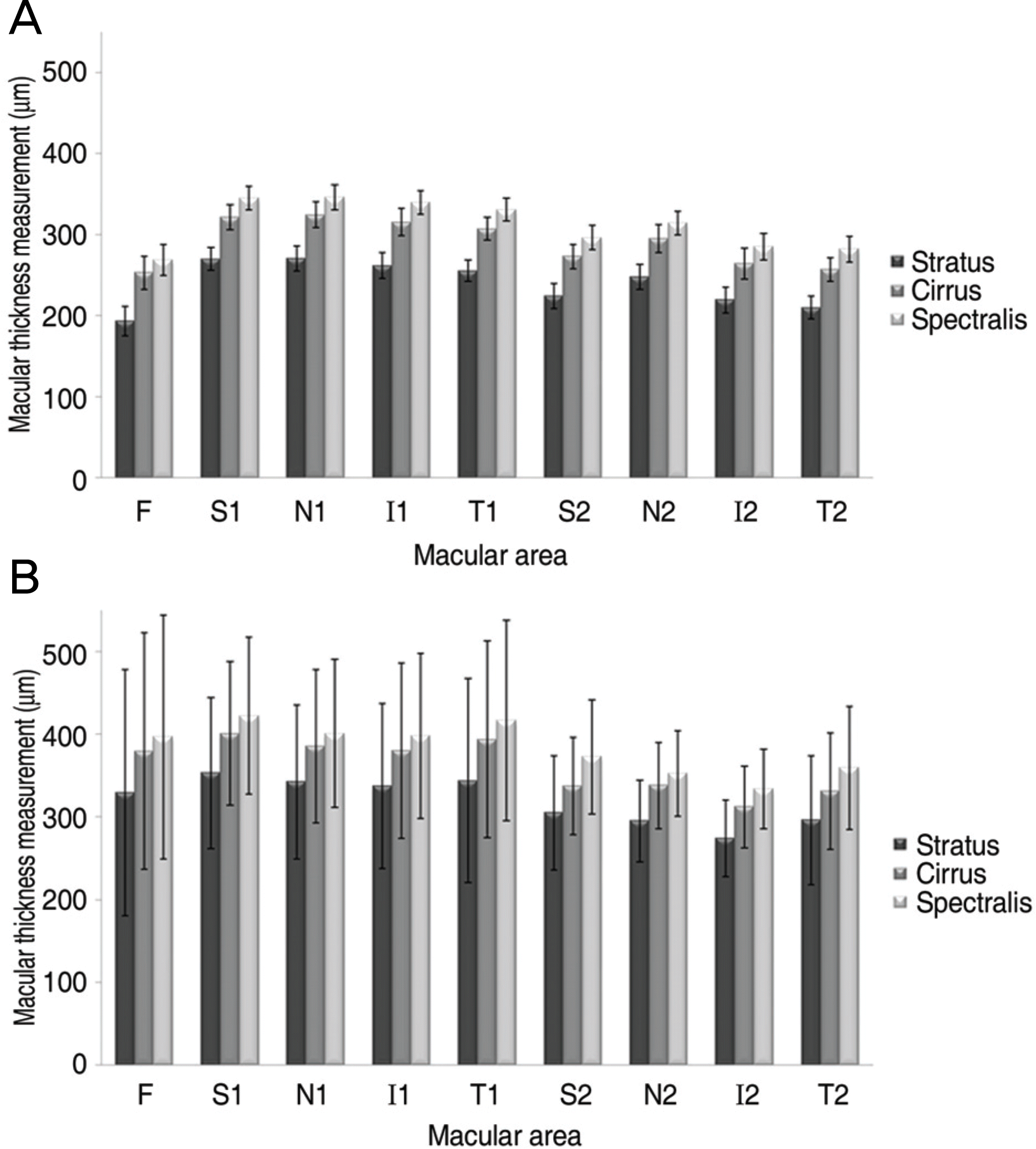
Figure 3.
Comparison of the three OCT's relative repeatability (%) (A=normal; B=diabetic macular edema) (F=fovea; S1=superior inner; N1=nasal inner; I1= inferior inner; T1=temporal inner; S2=superior outer; N2=nasal outer; I2=inferior outer; T2=temporal outer).
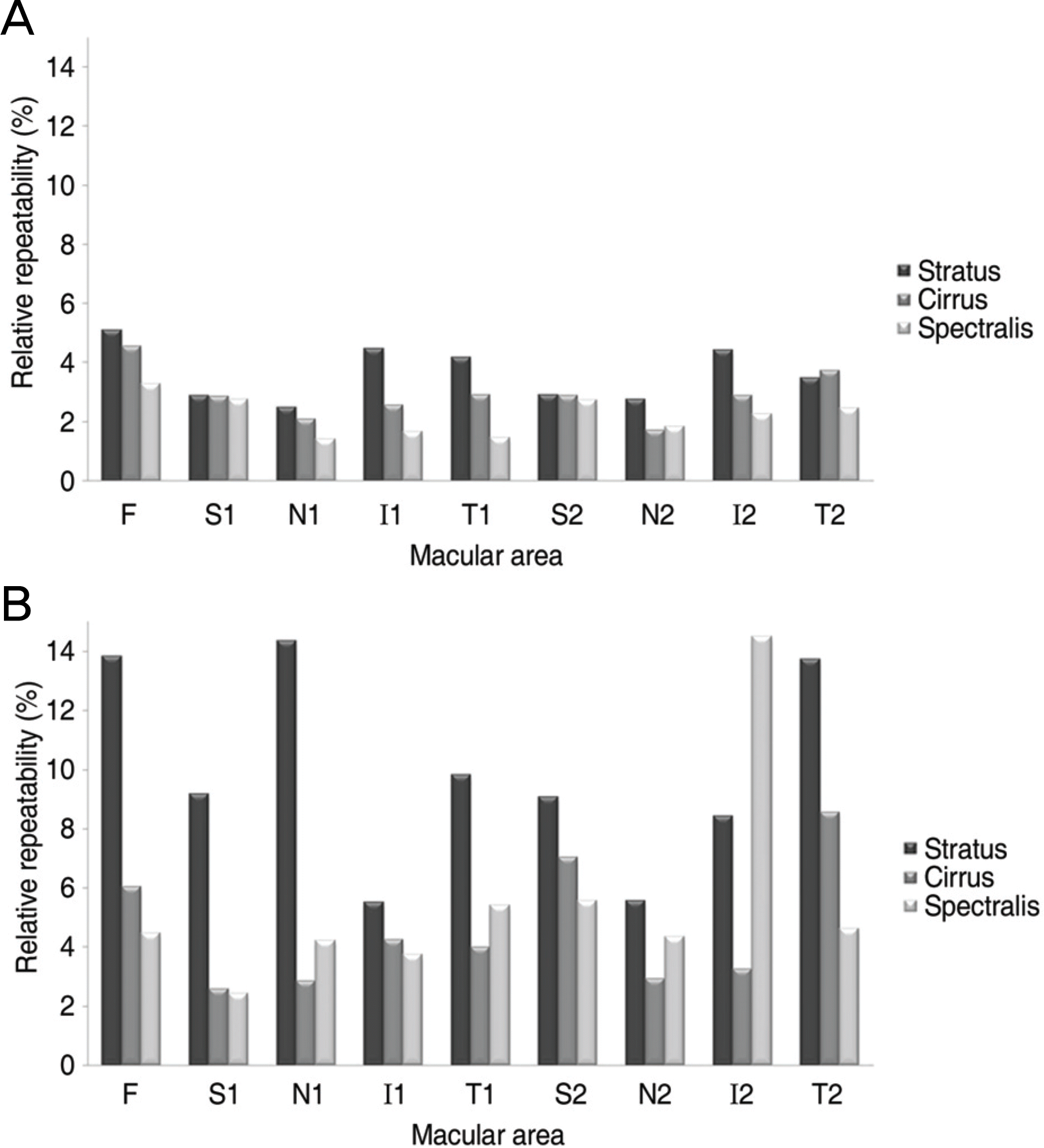
Figure 4.
Bland-Altman plots of the three OCTs. The mean difference is represented by the blue solid line and the 95% confidence limits, by the dotted lines (A=normal; B=diabetic macular edema).
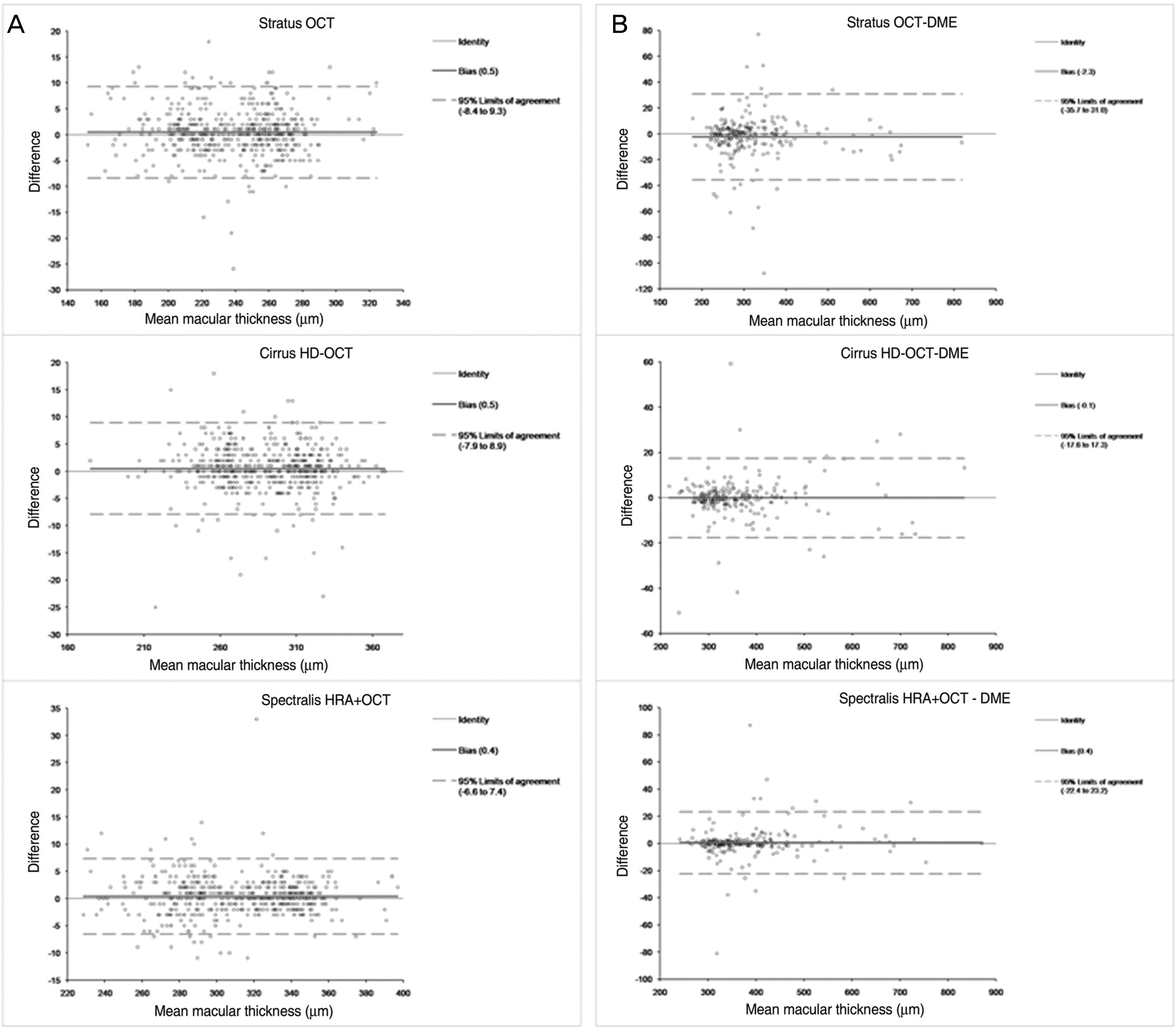
Figure 5.
Illustration of how time domain and spectral domain OCT samples the retina differently (Right= SD-OCT; Left=TD-OCT).
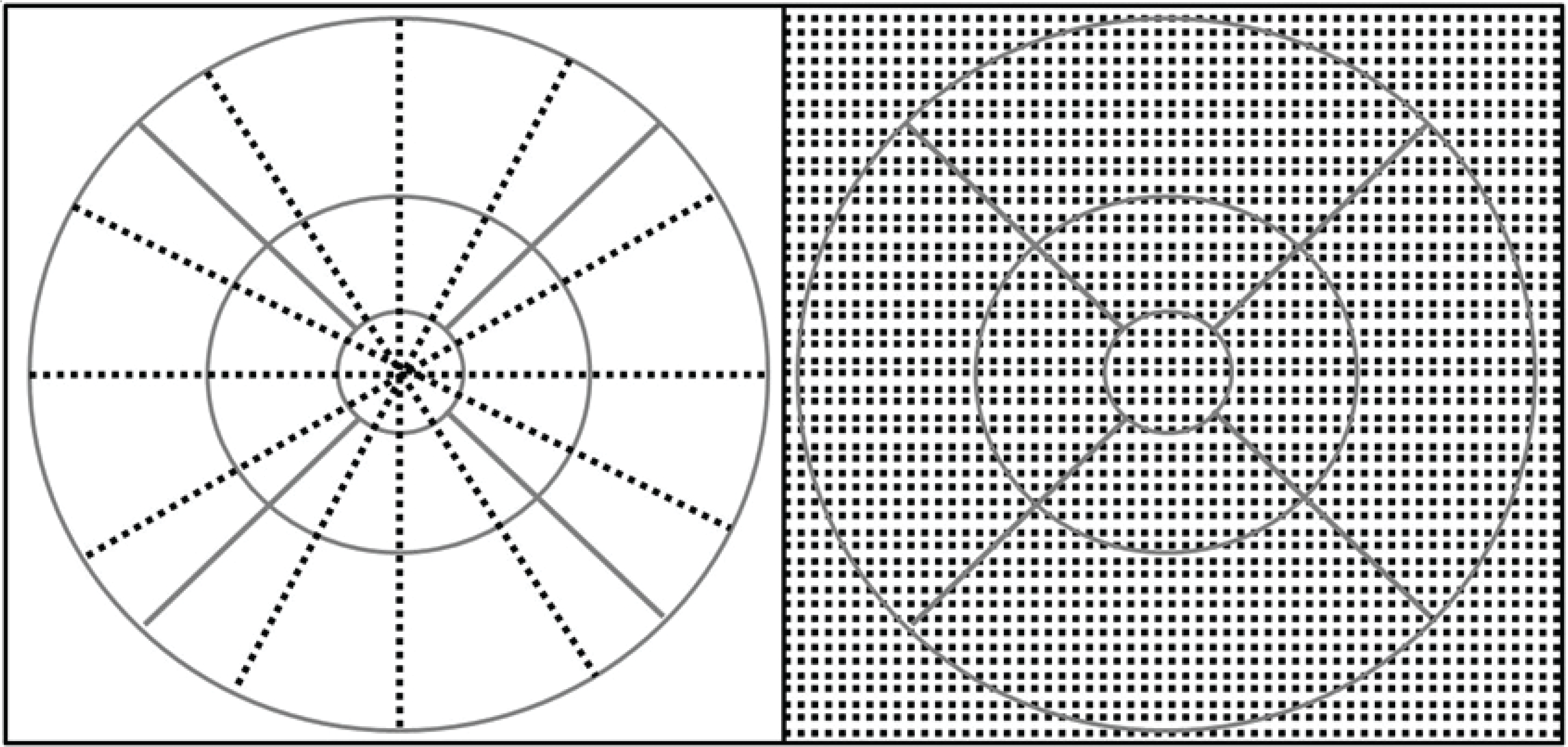
Figure 6.
Tomographies of the macula taken by the three OCTs with reference lines. All three anterior lines are similar to the ILM, but each posterior line is situated differently.

Table 1.!
Mean values and reliabilities of macular thickness parameter in Stratus OCT
Table 2.!
Mean values and reliabilities of macular thickness parameter in Cirrus HD-OCT
Table 3.!
Mean values and reliabilities of macular thickness parameter in Spectralis HRA+OCT
Table 4.
Mean and standard deviation of each OCT's macular thickness measurement difference. In the comparison of each OCT's macular thickness, all 9 areas showed a significant difference of p<0.001 (* paired t-test. all of them (9 areas))




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download