Abstract
Purpose
To compare the abilities of optical coherence tomography (Stratus OCT) and scanning laser polarimetry with variable corneal compensation (GDx VCC) in detecting localized retinal nerve fiber layer (RNFL) defects of red‐ free photography
Methods
Thirty six normal subject and 50 patients with localized RNFL defects were included in this study. Only one eye per subject was considered. The peripapillary RNFL was divided into 12 clock-hour sectors and localized RNFL defects were evaluated in these 12 sectors. To compare the diagnostic performance of Stratus OCT and GDx VCC based on the findings of red-free photography, we calculated the sensitivity, specificity, and area under the receiver operating characteristic curve (AUC) of each analyzer using a criterion of 1≥ clock hours abnormal at the <5% level.
Results
The sensitivity (78.6%), specificity (94.4%), and AUC (0.872) of Stratus OCT were not significantly different from those of GDx VCC (83.3%, 94.4%, and 0.882, respectively) (McNemar test, p=0.75, 1.00, and 0.82, respectively). However, the sensitivity (64.0%) of Stratus OCT for superior RNFL defect was significantly lower than that (84.8%) for inferior defect (Fisher’s exact test, p=0.02).
References
1. Quigley HA, Addicks EM, Green WR, Maumenee AE. Optic nerve damage in human glaucoma. II. The site of injury and susceptibility to damage. Arch Ophthalmol. 1981; 99:635–49.
3. Schuman JS, Hee MR, Puliafito CA. . Quantification of nerve fiber layer thickness in normal and glaucomatous eyes using optical coherence tomography. Arch Ophthalmol. 1995; 113:586–96.

4. Weinreb RN, Shakiba S, Zangwill L. Scanning laser polarimetry to measure the nerve fiber of normal and glaucomatous eyes. Am J Ophthalmol. 1995; 119:627–36.
5. Zhou Q, Weinreb RN. Individualized compensation of anterior segment birefringence during scanning laser polarimetry. Invest Ophthalmol Vis Sci. 2002; 43:2221–8.
6. Schuman JS, Pedut-Kloizman T, Hertzmark E. . Reproducibility of nerve fiber layer thickness measurements using optical coherence tomography. Ophthalmology. 1996; 103:1889–98.

7. Weinreb RN, Shakiba S, Zangwill L. Scanning laser polarimetry to measure the nerve fiber of normal and glaucomatous eyes. Am J Ophthalmol. 1995; 119:627–36.
8. Guedes V, Schuman JS, Hertzmark E. . Optical coherence tomography measurement of macular and nerve fiber layer thickness in normal and glaucomatous human eyes. Ophthalmology. 2003; 110:177–89.

9. Medeiros FA, Zangwill LM, Bowd C. . Fourier analysis of scanning laser polarimetry measurements with variable corneal compensation in glaucoma. Invest Ophthalmol Vis Sci. 2003; 44:2606–12.

10. Medeiros FA, Zangwill LM, Bowd C, Weinreb RN. Comparison of the GDx VCC scanning laser polarimeter, HRT II confocal scanning laser ophthalmoscope, and stratus OCT optical coherence tomograph for the detection of glaucoma. Arch Ophthalmol. 2004; 122:827–37.
11. Leung CK, Chan WM, Chong KK. . Comparative study of retinal nerve fiber layer measurement by StratusOCT and GDx VCC, I: correlation analysis in glaucoma. Invest Ophthalmol Vis Sci. 2005; 46:3214–20.

12. Brusini P, Salvetat ML, Zeppieri M. . Comparison between GDx VCC scanning laser polarimetry and Stratus OCT optical coherence tomography in the diagnosis of chronic glaucoma. Acta Ophthalmol Scand. 2006; 84:650–5.

13. Kanamori A, Nagai-Kusuhara A, Escaño MF. . Comparison of confocal scanning laser ophthalmoscopy, scanning laser polarimetry and optical coherence tomography to discriminate ocular hypertension and glaucoma at an early stage. Graefes Arch Clin Exp Ophthalmol. 2006; 244:58–68.

14. Quigley HA, Addicks EM, Green WR. Optic nerve damage in human glaucoma. III. Quantitative correlation of nerve fiber loss and visual field defect in glaucoma, ischemic neuropathy, papilledema, and toxic neuropathy. Arch Ophthalmol. 1982; 100:135–46.
15. Sommer A, Katz J, Quigley HA. . Clinically detectable nerve fiber atrophy precedes the onset of glaucomatous field loss. Arch Ophthalmol. 1991; 109:77–83.

16. Mok KH, Lee VW. Disc‐ to‐ macula distance to disc- diameter ratio for optic disc size estimation. J Glaucoma. 2002; 11:392–5.
17. Newcombe RG. Improved confidence intervals for the difference between binomial proportions based on paired data. Stat Med. 1998; 17:2635–50.

18. Odberg T, Riise D. Early diagnosis of glaucoma. The value of successive stereophotography of the optic disc. Acta Ophthalmol. 1985; 63:257–63.
19. Quigley HA, Brown AE, Morrison JD, Drance SM. The size and shape of the optic disc in normal human eyes. Arch Ophthalmol. 1990; 108:51–7.

20. Seong GJ, Chung GW, Oh ST. Topographic measurements of the optic nerve head with confocal scanning laser tomography in normal Koreans. J Korean Ophthalmol Soc. 1997; 38:1834–41.
21. Park SJ, Park KH, Yu YS. . Early detection of glaucoma with retinal nerve fiber layer photograph. J Korean Ophthalmol Soc. 1998; 39:180–6.
22. Niessen AG, van den Berg TJ, Langerhorst CT, Bossuyt PM. Grading of retinal nerve fiber layer with a photographic reference set. Am J Ophthalmol. 1995; 120:577–86.

23. Quigley HA, Reacher M, Katz J. . Quantitative grading of nerve fiber layer photographs. Ophthalmology. 1993; 100:1800–7.

24. Budenz DL, Michael A, Chang RT. . Sensitivity and specificity of the StratusOCT for perimetric glaucoma. Ophthalmology. 2005; 112:3–9.

25. Jeoung JW, Park KH, Kim TW. . Diagnostic ability of optical coherence tomography with a normative database to detect localized retinal nerve fiber layer defects. Ophthalmology. 2005; 112:2157–63.

26. Varma R, Skaf M, Barron E. Retinal nerve fiber layer thickness in normal human eyes. Ophthalmology. 1996; 103:2114–9.

27. Poinoosawmy D, Fontana L, Wu JX. . Variation of nerve fiber layer thickness measurements with age and ethnicity by scanning laser polarimetry. Br J Ophthalmol. 1997; 81:350–4.
Figure 1.
Method to identify a localized retinal nerve fiber layer (RNFL) defect by the Stratus OCT optical coherence tomography and GDx VCC scanning laser polarimetry with variable corneal compensation. (A) Red-free RNFL photograph of right eye of a 69 year-old male patient. The peripapillary RNFL was divided into 12 clock-hour sectors like a sector average analysis of Stratus OCT. There is a wedge-shaped RNFL defect at the inferotemporal region (white arrows). (B) Sector average analysis of Stratus OCT of the same eye. There are all 12 sectors and 2 abnormal sectors at 6 and 7 clock-hour (red arrows), which are correlated with the finding of red-free photograph. (C) Deviation map analysis of GDx VCC of the same eye. The peripapillary RNFL was artificially divided into 12 sectors like the sector average analysis of Stratus OCT. There are a few color-coded squares abnormal at p<0.05 (white arrows), which are correlated with the finding of red-free photograph.

Figure 2.
Ven diagrams showing the number of eyes discriminated into having a localized retinal nerve fiber layer (RNFL) defect by Stratus OCT or GDx VCC among the eyes with a superior RNFL defect (A), among the eyes with an inferior RNFL defect (B), and among the eyes with a RNFL defect in either superior or inferior RNFL region (C).
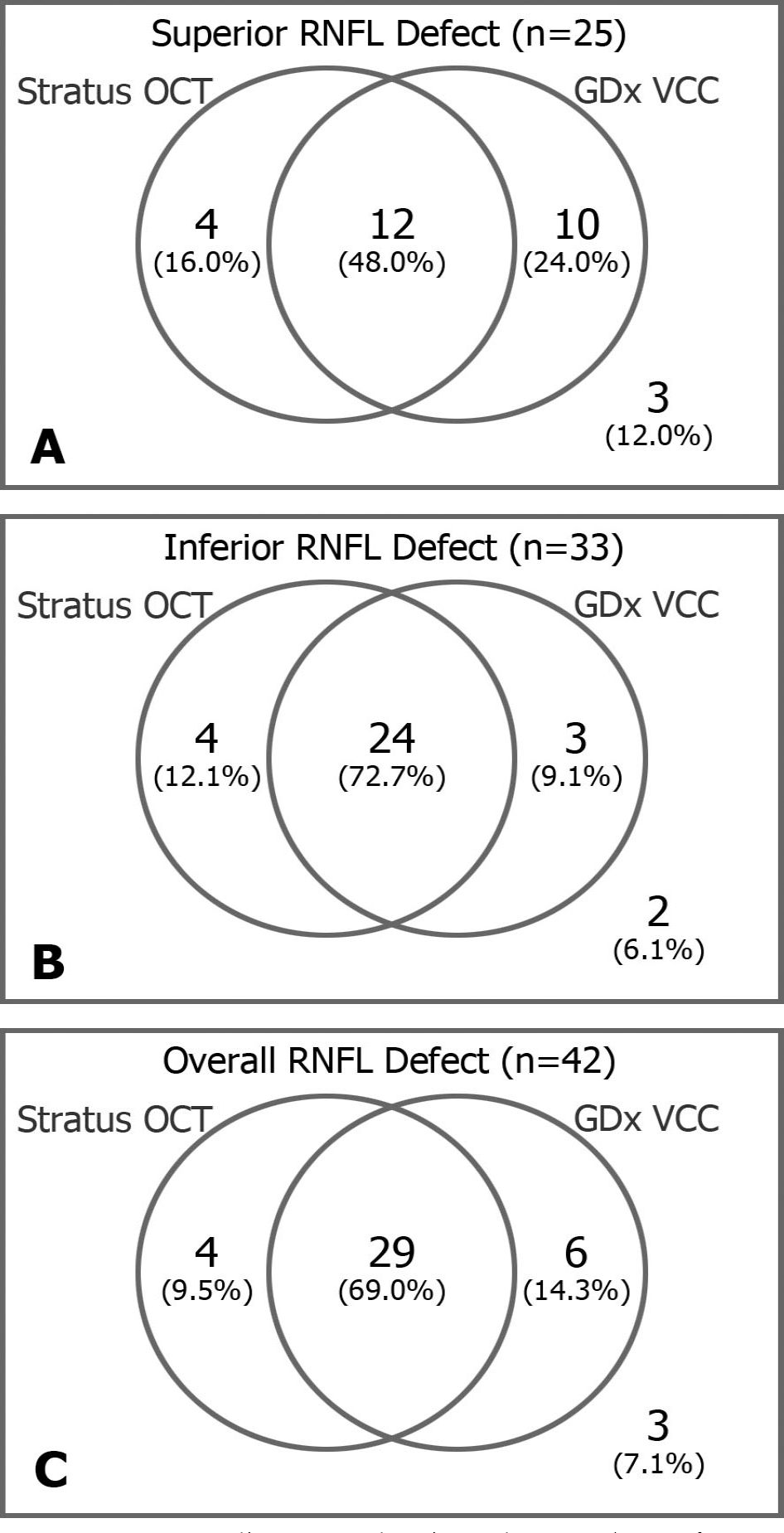
Table 1.
Demographics and clinical characteristics of study group
| RNFL defect group (n=50) | Healthy control group (n=36) | P-value | |
|---|---|---|---|
| Age, year (mean±SD) | 54.54±12.75 | 52.53±14.90 | 0.50* |
| Sex, no (men:women) | 26:24 | 14:22 | 0.33† |
| BCVA (mean±SD) | 0.83±0.14 | 0.89±0.11 | 0.09* |
| SE, diopter (mean±SD) | ‐1.98±2.91 | ‐1.36±2.44 | 0.41* |
| IOP, mmHg (mean±SD) | 17.57±3.92 | 13.99±2.98 | <0.01* |
| Vertical C/D ratio (mean±SD) | 0.67±0.19 | 0.43±0.13 | <0.01* |
| DM:DD ratio | 2.52±0.27 | 2.57±0.24 | 0.45* |
| MD, dB (mean±SD) | ‐3.93±3.57 | ‐0.66±1.12 | <0.01* |
| PSD, dB (mean±SD) | 6.29±4.41 | 1.29±0.31 | <0.01* |
Table 2.
Quantitatively measured peripapillary retinal nerve fiber layer thickness of study group
| RNFL defect group (n=50) | Healthy control group (n=36) | P-value* | |
|---|---|---|---|
| Superior RNFL thickness | |||
| Stratus OCT | 107.28±17.72 | 134.25±12.74 | <0.01 |
| GDx VCC | 59.82±9.79 | 70.64±8.06 | <0.01 |
| Inferior RNFL thickness | |||
| Stratus OCT | 99.58±24.36 | 135.11±16.04 | <0.01 |
| GDx VCC | 53.91±10.22 | 66.73±8.09 | <0.01 |
| Average RNFL thickness | |||
| Stratus OCT | 85.16±15.54 | 108.12±9.94 | <0.01 |
| GDx VCC | 49.09±8.49 | 57.34±5.82 | <0.01 |
Table 3.
Diagnostic performance of Stratus OCT and GDx VCC for localized retinal nerve fiber layer defect
| Stratus OCT | GDx VCC | P-value | |
|---|---|---|---|
| Superior RNFL Defect (n=25) | |||
| Sensitivity (95% CI) | 64.0% (44.5‐79.8%) | 72.0% (52.4‐85.7%) | 0.75* |
| Specificity (95% CI) | 96.7% (88.8‐99.1%) | 100.0% (94.1‐100.0%) | 0.50* |
| AUC (95% CI) | 0.804 (0.704‐0.881) | 0.860 (0.768‐0.925) | 0.45† |
| Inferior RNFL Defect (n=33) | |||
| Sensitivity (95% CI) | 84.8% (69.1‐93.3%) | 81.8% (65.6‐91.4%) | 1.00* |
| Specificity (95% CI) | 96.2% (87.2‐99.0%) | 94.3% (84.6‐98.1%) | 1.00* |
| AUC (95% CI) | 0.905 (0.823‐0.958) | 0.881 (0.793‐0.941) | 0.64† |
| Overall RNFL Defect (n=42) | |||
| Sensitivity (95% CI) | 78.6% (64.1‐88.3%) | 83.3% (69.4‐91.7%) | 0.75* |
| Specificity (95% CI) | 94.4% (81.9‐98.5%) | 94.4% (81.9‐98.5%) | 1.00* |
| AUC (95% CI) | 0.872 (0.783‐0.934) | 0.882 (0.795‐0.942) | 0.84† |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download