Abstract
Purpose
To report a case of high dose steroid-responsive Purtscher's retinopathy which was developed after operation for diaphragmatic laceration sustained in motorcycle accident.
Case summary
A 68-year-old man came to our hospital with complaining of decreased visual acuity in the right eye after diaphragmatic laceration operation. Best corrected visual acuity was 0.1 in the right eye. Anterior segment was nonspecific. However, afferent pupillary defect was observed. Superficial intraretinal hemorrhage, numerous cotton-wool spots, peripapillary hemorrhage, and macular edema were detected on fundus examination. Fluorescein angiography revealed capillary nonperfusion and fluorescein filling defect due to retinal hemorrhage in arteriovenous phase and fluorescein leakage from the macula and capillary nonperfusion area in the late venous phase. Accordingly, Purtscher's retinopathy was diagnosed and the patient was observed without specific treatment. After 2 weeks of observation, symptoms and fundus findings were not changed. High-dose steroid therapy was begun with injection of one gram of methylprednisone for three days, switched to oral prednisolone, and then slowly tapered in period of 3 weeks. 7 days after the treatment, visual acuity was improved to 0.2 in the right eye but afferent pupillary defect was still observed. Cotton-wool spots slightly decreased, peripapillary hemorrhage was absorbed but macular edema was remained. 14 days after the treatment, visual acuity greatly improved to 0.63 and afferent pupillary defect was not observed. Cotton-wool spots and macular edema were decreased but fluoroscein leakage from capillary nonperfusion area was remained.
Go to : 
References
2. Jacob HS, Craddock PR, Hammerschmidt DE, Moldow CF. Complement induced granulocyte aggregation. An unsuspected mechanism if disease. N Engl J Med. 1980; 302:789–94.
3. Behrens-Baumann W, Scheurer G, Schroer H. Pathogenesis of Purtscher's retinopathy. An experimental study. Graefes Arch Clin Exp Ophthalmol. 1992; 230:286–91.
4. Lai JC, Johnson MW, Martonyi CL, et al. Complement-induced retinal arteriolar occlusions in the cat. Retina. 1997; 17:239–46.

6. Scheurer G, Praetorius G, Damerau B, et al. Vascular occlusion of the retina: an experimental model. I. Leukocyte aggregates. Graefes Arch Clin Exp Ophthalmol. 1992; 230:275–80.
7. Hammerschmidt DE, White JG, Craddock PR, Jacob HS. Corticosteroids inhibit Complement-induced granulocyte aggregation. A possible mechanism for their efficacy in shock states. J Clin Invest. 1979; 63:798–803.

8. Wang AG, Yen MY, Liu JH. Pathogenesis and neuroprotective treatment in Purtscher's retinopathy. Jpn J Ophthalmol. 1998; 42:318–22.

9. Atabay C, Kansu T, Nurlu G. Late visual recovery after intra-venous methylprednisolone treatment of Purtscher's retinopathy. Ann Ophthalmol. 1993; 25:330–3.
10. Kiryu J, Ogura Y. Hyperbaric oxygen treatment for macular edema in retinal vein occlusion: relation to severity of retinal leakage. Ophthalmologica. 1996; 210:168–70.

11. Bojić L, Ivanisević M, Gosovicć G. Hyperbaric oxygen therapy in two patients with non-arteritic anterior optic neuropathy who did not respond to prednisone. Undersea Hyperb Med. 2002; 29:86–92.
12. Weinberger AW, Siekmann UP, Wolf S, et al. Treatment of acute central retinal artery occlusion (CRAO) by hyperbaric oxygenation therapy (HBO). Pilot study with 21 patients. Klin Monatsbl Augenheilkd. 2002; 219:728–34.
13. Frayser R, Hickam JB. Effect of vasodilator drugs on the retinal blood flow in man. Arch Ophthalmol. 1965; 73:640–2.

14. Lemagne JM, Michiels X, Van Causenbroeck S, Sonyers B. Purtscher-like retinopathy after retrobulbar anesthesia. Ophthalmology. 1990; 97:859–61.

15. Purtscher O. Angiopathia retinae traumatica: Lymphorrhagien des Augengrunds. Gradfes Arch Klin Exp Ophthalmol. 1912; 82:347–71.
16. Lew HM, Rho SH, Kim DI, Lee SJ. A Case of Purtscher's Retinopathy. J Korean Ophthalmol Soc. 1983; 24:293–5.
17. Rah SH, Whang SK. A Case of Purtscher's Retinopathy. J Korean Ophthalmol Soc. 1991; 32:200–3.
18. Bae JG, Park JS. Purtscher's Retinopathy due to safety belts. J Korean Ophthalmol Soc. 2003; 44:231–4.
19. Mark W. Balles. Traumatic retinopathy. Albert DM, Jakobiec FA, editors. Principle and Practice of Ophthalmlogy. 2nd ed.Philadelphia: WB Saunders;2001. 3:chap. 165.
20. Jacob HS, Craddock PR, Hammerschmidt DE, et al. Complement-induced granulocyte aggregation: an unsuspected mechanism of disease. N Engl J Med. 1980; 302:789–94.
21. Tachfouti S, Karmane A, El Moussaif H, Boutimzine N. Purtscher's retinopathy with a favorable outcome after corticosteroid. Bull Soc Belge Ophtalmol. 2005; 298:45–50.
Go to : 
 | Figure 1.At the first visit. (A) A Color photograph of the right eye shows hemorrhages with numerous cotton wool spots in the peripapillary region, superficial intraretinal hemorrhage and macular edema. (B) On fluorescein angiography, capillary nonperfusion and fluorescein filling defects due to numerous cotton-wool spots and retinal hemorrhages were detected in the arteriovenous phase. (C) Fluorescein leakage from macular edema and capillary nonperfusion area was detected in the late venous phase. |
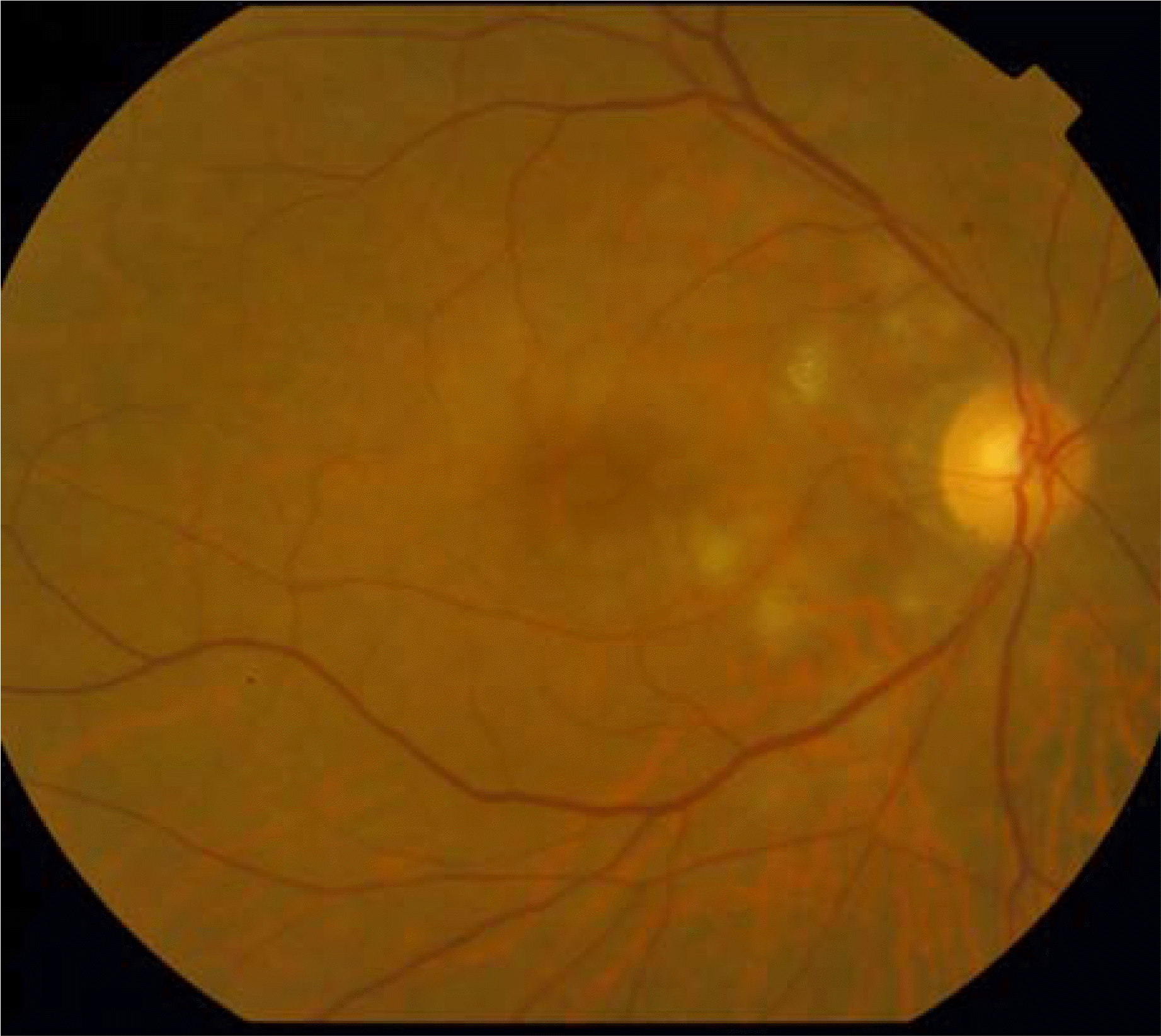 | Figure 2.Seven days after high dose steroid therapy. Fundus photogragh showed that numerous cotton-wool spots, superficial intraretinal hemorrhage, and macular edema were all slightly decreased but still remained and peripapillary hemorrhage was absorbed. |
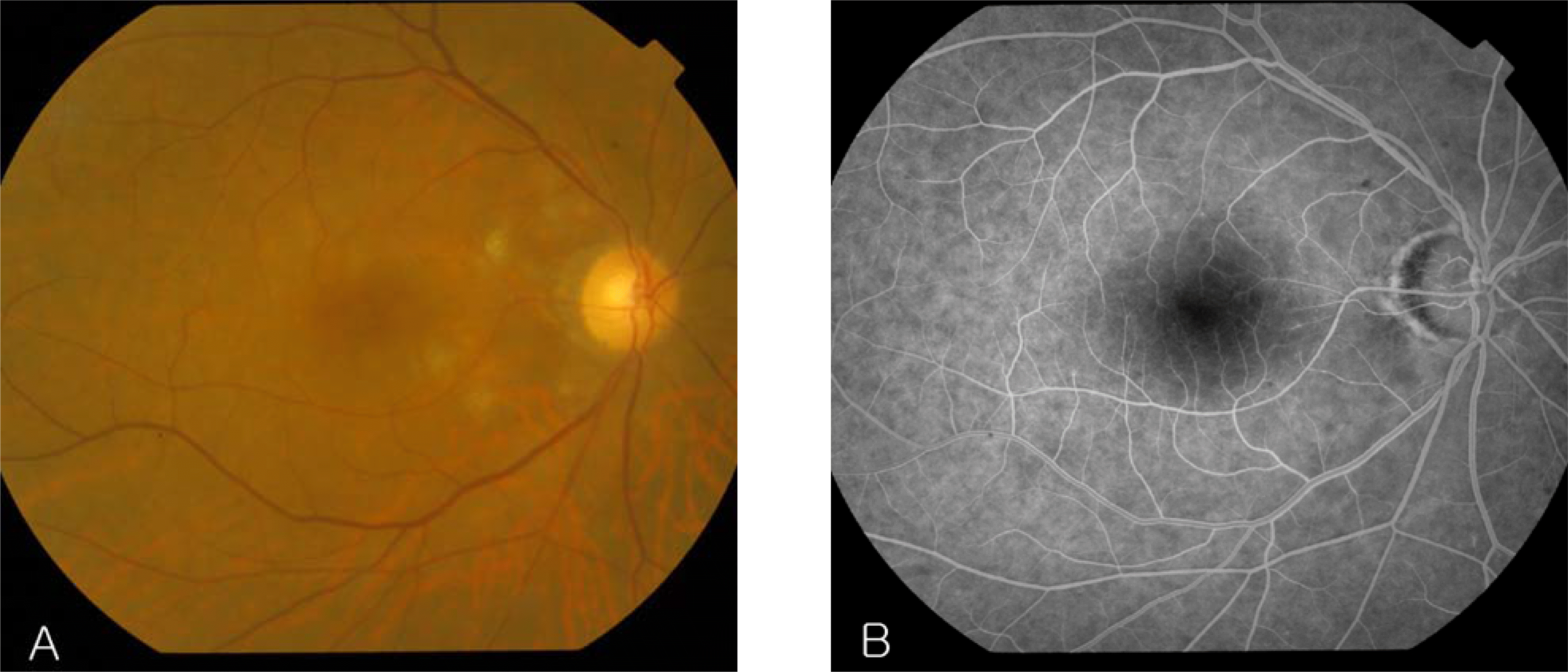 | Figure 3.Fourteen days after high dose steroid therapy. (A) In fundoscopic findings, peripapillary numerous cotton-wool spots were remarkably decreased and only small amount of retinal hemorrhage was still observed. (B) Fluorescein angiography revealed decreased capillary nonperfusion area in the arteriovenous phase. |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download