Abstract
Case Summary
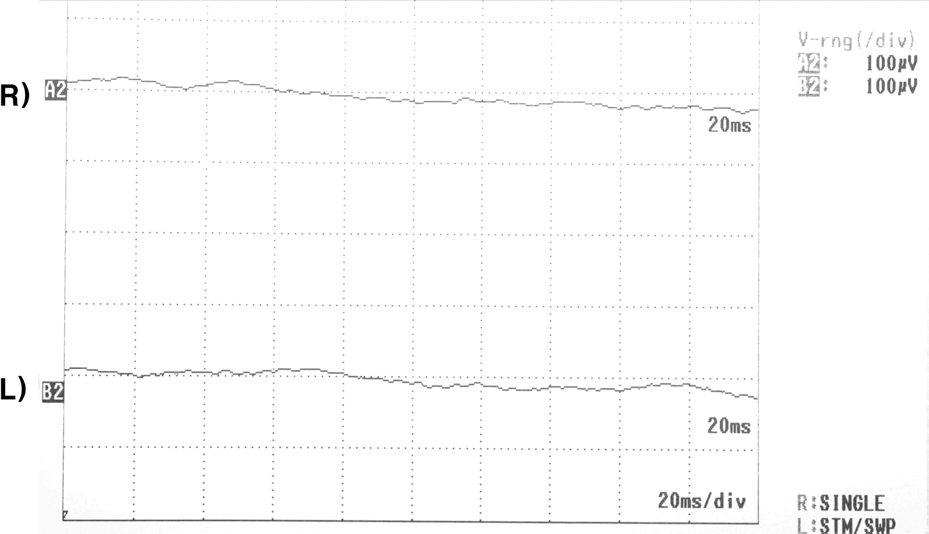
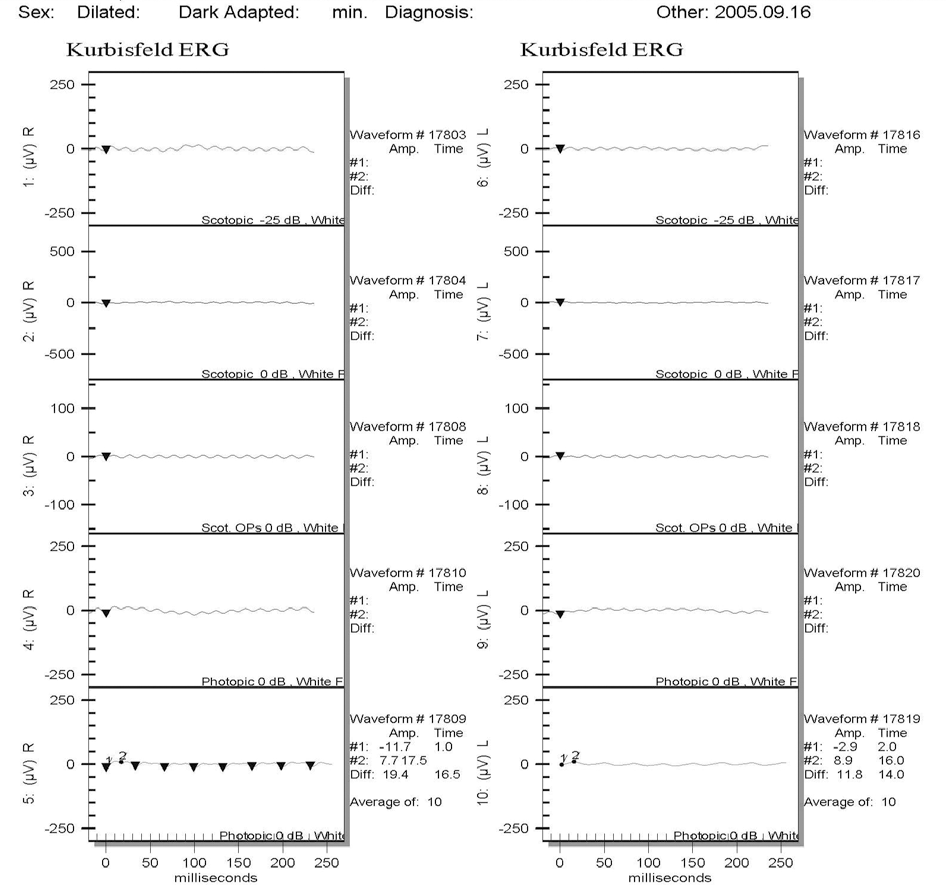
A 7-month-old boy was referred for poor eye contact and esodeviation since birth. He could not fixate with his eyes or follow objects. Nystagmus in both eyes and moderate angle esotropia were present. Slit lamp examination and fundus examination showed no significant findings. Visual evoked potential and electroretinogram were extinguished in both eyes. The patient showed abnormal respiratory patterns, developmental delay, and hypotonia. Brain MRI showed aplasia of the cerebellar vermis, and he was diagnosed with Joubert syndrome. At 2 years of age, he was moderately able to fixate with his eyes and to crudely follow objects. Nystagmus and esotropia had diminished, but the visual evoked potential and electroretinogram still showed no response in both eyes.
Go to : 
References
1. Joubert M, Eisenring JJ, Robb JP, Andermann F. Familial agenesis of the cerebellar vermis: A syndrome of episodic hyperpnea, abnormal eye movements, ataxia, and retardation. Neurology. 1969; 19:813–25.

3. Maria BL, Boltshauser E, Palmer SC, Tran T. Clinical features and revised diagnostic criteria in Joubert syndrome. J Child Neurol. 1999; 14:583–91.
4. Leber T. Uber Retinitis pigmentosa und angeborene amaurose. Albrecht Von Graefes Arch Ophthalmol. 1869; 15:1–25.
5. Tomita H, Ohno K, Tamai A. Joubert syndrome associated with Leber’s congenital amarosis. Brain Dev (domestic edition). 1979; 11:459–65.
6. King MD, Dudgeon J, Stephenson JB. Joubert’s syndrome with retinal dysplasia: Neonatal tachypnea as the clue to a genetic brain-eye malformation. Arch Dis Child. 1984; 59:709–18.
7. Ivarsson S, Bjerre I, Brun A. . Joubert syndrome associated with Leber amaurosis and multicystic kidneys. Am J Med Genet. 1993; 45:542–7.

8. Cho EH, Kim YS, Jin YH. Joubert syndrome presented with ocular motor apraxia. J Korean Ophthalmol Soc. 1995; 36:210–5.
9. Kwon GR, Kim MS, Chang HR. Congenital ocular motor apraxia without head thrust (A case of Joubert syndrome). J Korean Ophthalmol Soc. 1996; 37:1236–40.
10. Bordarier C, Aicardia J. Dandy-Walker syndrome and agenesis of the cerebellar vermis: Diagnostic problems and genetic counseling. Dev Med Chlid Neurol. 1990; 32:285–94.
11. Castori M, Valente EM, Donati MA. . NPHP1 gene deletion is a rare cause of Joubert syndrome related disorders. J Med Genet. 2005; 42:9.

12. Moore AT, Taloy DS. A syndrome of congenital retinal dystrophy and saccade palsy-a subset of Leber's amaurosis. Br J Ophthalmol. 1984; 68:421–31.

13. Noble KG, Carr RE. Leber’s congenital amaurosis. A retrospective study of 33 cases and a histopathological study on one case. Arch Ophthalmol. 1978; 96:818–21.
14. Galvin JA, Fishman GA, Stone EM, Koenekoop RK. Clinical phenotypes in carriers of Leber congenital amaurosis mutations. Ophthalmology. 2005; 112:349–56.

15. Ferland RJ, Eyaid W, Collura RV. . Abnormal cerebellar development and axonal decussation due to mutations in AHI1 in Joubert syndrome. Nat Genet. 2004; 36:1008–13.

16. Parisi MA, Bennett CL, Eckert ML. . NPHP1 gene deletion associated with juvenile nephronophthisis is present in a subset of individuals with Joubert syndrome. Am J Hum Genet. 2004; 75:82–91.
Go to : 
 | Figure 3.The classic ”molar tooth sign” of Joubert syndrome is shown in the T1-weighted transverse MRI image. Note the thickened superior cerebellar peduncles (indicated by the white arrows) that do not decussate, so the isthmus is reduced, causing the interpeduncular fossa (black arrow) to be enlarged. |




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download