Abstract
Purpose
To evaluate the change in anterior chamber depth and refraction after AT-45 implantation Methods: Twenty-two eyes from 22 patients were enrolled in this prospective study. After phacoemulsification, AT-45 (11 eyes) and SA60AT (11 eyes) were implanted. Clinical data included anterior chamber depth and refractive error at 1 week, 1 month, 2 months and 6 months postoperatively. The correlation between anterior chamber depth change and spherical equivalent change was also evaluated.
Results
In the AT-45 implanted group, the mean anterior chamber depth was 4.56±0.59 mm at 1 week postoperative, 4.70±0.69 mm at 1 month postoperative, 4.78±0.71 mm at 2 months postoperative and 4.76± 0.69 mm at 6 months postoperative. The mean spherical equivalent was −0.53±0.48D, −0.37±0.42D, −0.27± 0.47D, and −0.33±0.44D respectively. When analyzed using the Mann-Whitney U test, p-values of anterior chamber depth differences between the 2 groups were P=0.52 at 1 week to 1 month, P=0.32 at 1 month to 2 months, P=0.89 at 2 months to 6 months, and P=0.02 at 1 week to 6 months, showing a deeper anterior chamber in the AT-45 implanted group. P-values (Mann-Whitney U test) of spherical equivalent differences between the 2 groups were P=0.33, P=0.56, P=0.94, and P=0.19, respectively, showing more hyperopic change in the AT-45 implanted group. The correlation between anterior chamber depth change and spherical equivalent change in the AT-45 implanted group at 1 week to 6 months was not statistically significant (Spearman correlation analysis, P=0.223).
Go to : 
References
1. Im YW, Lee KH, Park SC. The differences of the near visual acuity between multifocal IOL and monofocal IOL. J Korean Ophthalmol Soc. 1994; 35:1027–32.
2. Hayashi K, Hayashi H, Nakao F, Hayashi F. Aging changes in apparent accommodation in eyes with a monofocal intraocular lens. Am J Ophthalmol. 2003; 135:432–6.

3. Kuchle M, Langenbucher A, Gusek-Schneider GC, et al. First results of implantation of a new, potentially accommodative posterior chamber intraocular lens. Klin Monatsbl Augenheilkd. 2001; 218:603–8.
4. Kuchle M, Seitz B, Langenbucher A, et al. Comparison of 6-month results of implantation of the 1CU accommodative intraocular lens with conventional intraocular lenses. Ophthalmology. 2004; 111:318–24.

5. Hara T, Hara T, Yasuda A, Yamada Y. Accommodative intraocular lens with spring action-part 1: design and placement in an excised animal eye. Ophthalmic Surg. 1990; 21:128–33.
6. Hara T, Hara T, Yasuda A, et al. Accommodative intraocular lens with spring action-part 2: fixation in the living rabbit. Ophthalmic Surg. 1992; 23:632–5.

7. McLeod SD, Portney V, Ting A. A dual optic accommodating foldable intraocular lens. Br J Ophthalmol. 2003; 87:1083–5.

8. Cumming JS, Slade SG, Chayet A. Clinical evaluation of the model AT-45 silicone accommodating intraocular lens. Ophthalmology. 2001; 108:2005–10.
9. Coleman PJ. On the hydraulic suspension theory of accommodation. Trans Am Ophthalmol Soc. 1986; 84:846–68.
10. Strenk SA, Semmlow JL, Strenk LM, et al. Age-related changes in human ciliary muscle and lens: a magnetic resonance imaging study. Invest Ophthalmol Vis Sci. 1999; 40:1162–9.
11. Cumming JS, Ritter JA. The measurement of vitreous cavity length and its comparison pre- and postoperatively. Eur J Implant Refract Surg. 1994; 6:261–72.

12. Kim JH, Park JS, Chung TY, Chung ES. Clinical evaluation of AT-45 implantation. J Korean Ophthalmol Soc. 2007; 48:368–75.
13. Nejima R, Miyai T, Kataoka Y, et al. Prospective intrapatient comparison of 6.0-millimeter optic single-piece and 3-piece hydrophobic acrylic foldable intraocular lenses. Ophthalmology. 2006; 113:585–90.

14. Cazal J, Lavin-Dapena C, Marin J, Verges C. Accommodative intraocular lens tilting. Am J Ophthalmol. 2005; 140:341–4.

15. Cumming JS, Colvard DM, Dell SJ, et al. Clinical evaluation of the Crystalens AT-45 accommodating intraocular lens: results of the U.S. Food and Drug Administration clinical trial. J Cataract Refract Surg. 2006; 32:812–25.
16. Alio JL, Tavolato M, De la Hoz F, et al. Near vision restoration with refractive lens exchange and pseudoaccommodating and multifocal refractive and diffractive intraocular lenses: comparative clinical study. J Cataract Refract Surg. 2004; 30:2494–503.
17. Marchini G, Pedrotti E, Sartori P, Tosi R. Ultrasound biomicroscopic changes during accommodation in eyes with accommodating intraocular lenses: pilot study and hypothesis for the mechanism of accommodation. J Cataract Refract Surg. 2004; 30:2476–82.
18. Lee DY, Ahn CS. Statistical study of the ocular dimensions on refractive error. J Korean Ophthalmol Soc. 1994; 35:1137–46.
19. Kim CS, Kim MY, Kim HS, Lee YC. Change of corneal astigmatism with aging in Koreans with normal visual acuity. J Korean Ophthalmol Soc. 2002; 43:1956–62.
20. Foster PJ, Baasanhu J, Alsbirk PH, et al. Central corneal thickness and intraocular pressure in a Mongolian population. Ophthalmology. 1998; 105:969–73.

21. La Rosa FA, Gross RL, Orengo-Nania S. Central corneal thickness of Caucasians and African Americans in glaucomatous and nonglaucomatous populations. Arch Ophthalmol. 2001; 119:23–7.
22. Yo C, Ariyasu RG. Racial differences in central corneal thickness and refraction among refractive surgery candidates. J Refract Surg. 2005; 21:194–7.

23. Clemmesen V, Olurin O. Lens thickness in western Nigeria. A comparative ultrasonic study in Negros and Danes. Acta Ophthalmol. 1985; 63:274–6.
24. Wojciechowski R, Congdon N, Anninger W, Teo Broman A. Age, gender, biometry, refractive error, and the anterior chamber angle among Alaskan Eskimos. Ophthalmology. 2003; 110:365–75.

25. Stachs O, Schneider H, Stave J, Guthoff R. Potentially accommodating intraocular lenses-an in vitro and in vivo study using three-dimensional high-frequency ultrasound. J Refract Surg. 2005; 21:37–45.
Go to : 
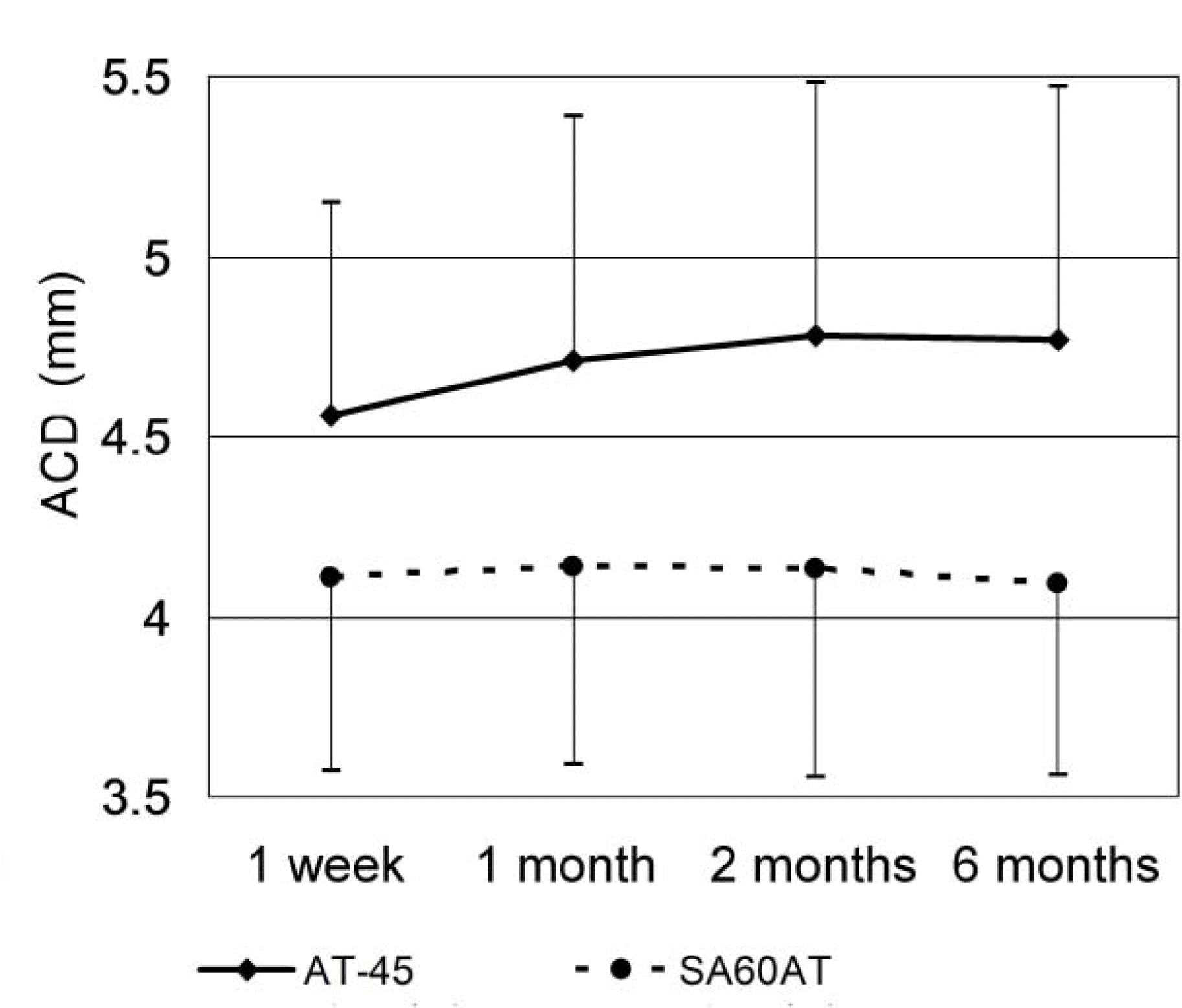 | Figure 1.Changes in mean anterior chamber depth (ACD) after AT-45 (n=11) and SA60AT (n=11) implantation, according to the follow-up period. |
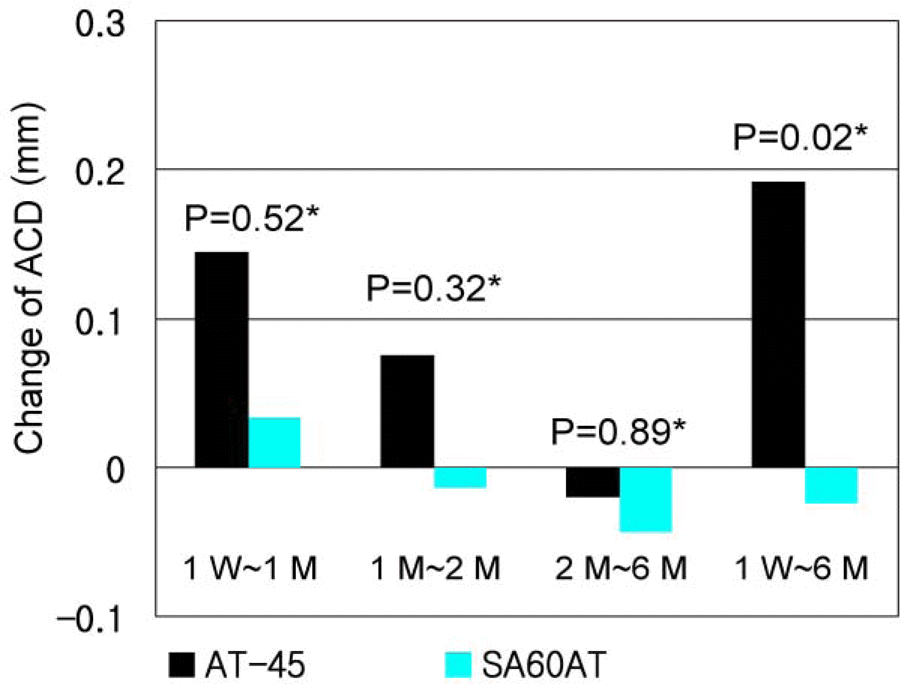 | Figure 2.Mean anterior chamber depth (ACD) difference in AT-45 group (n=11) and SA60AT group (n=11), according to the follow-up period. Positive value represents deepening of the anterior chamber, whereas negative value represents shallowing of the anterior chamber (* : Mann-Whitney U test, W: week, M: month). |
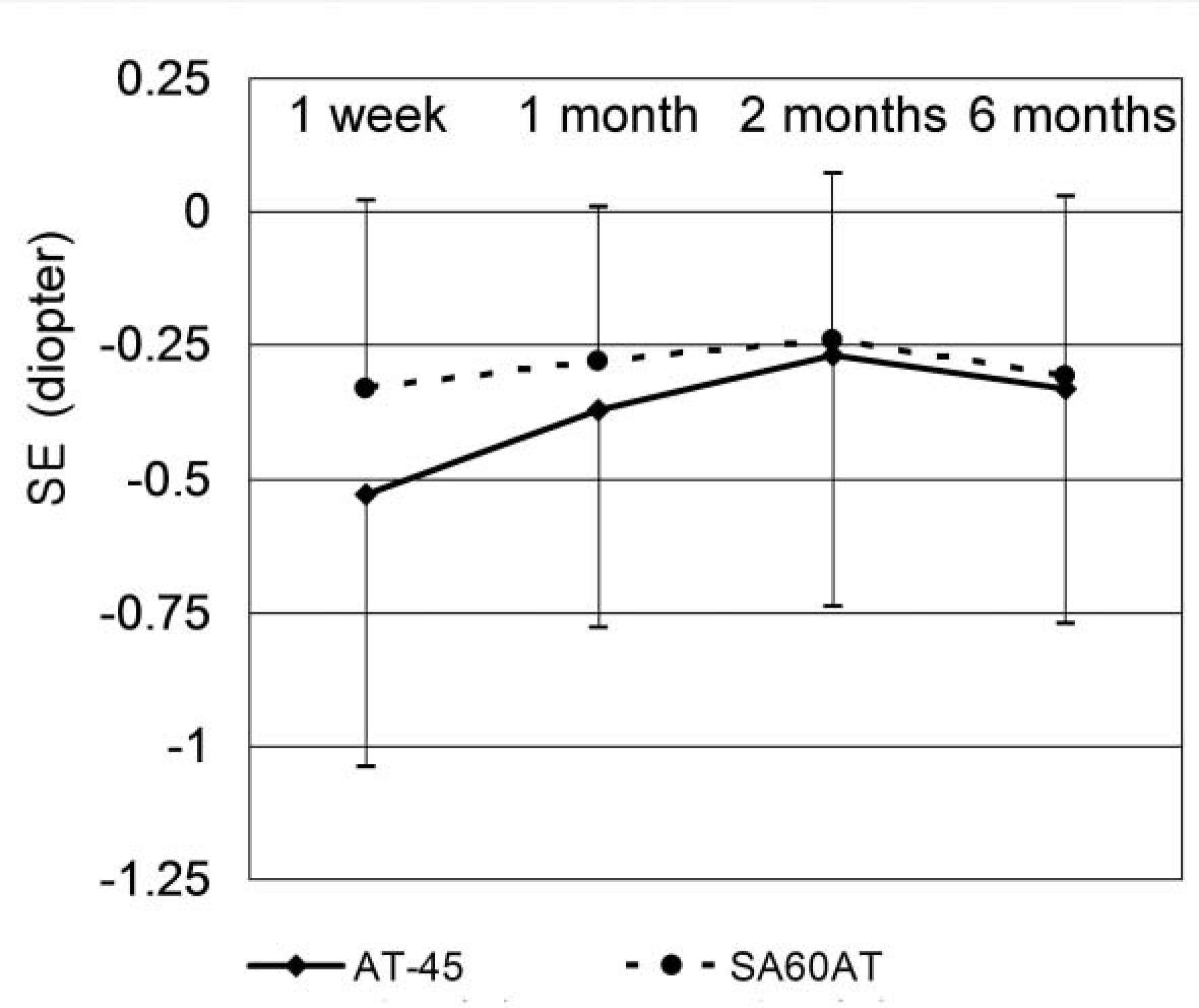 | Figure 3.Mean spherical equivalent (SE) change after AT-45 (n=11) and SA60AT (n=11) implantation, according to the follow-up period. |
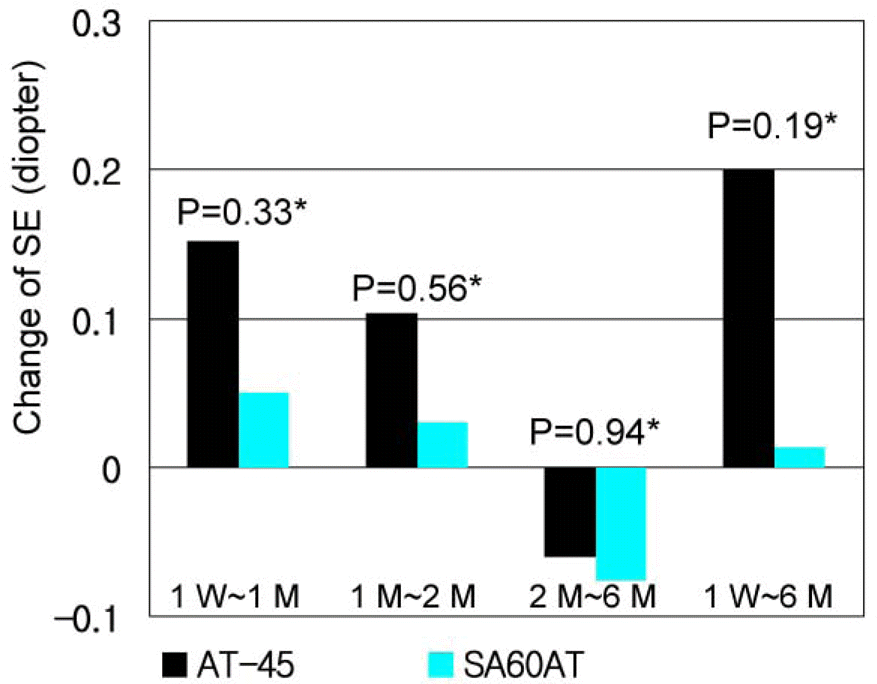 | Figure 4.Mean spherical equivalent (SE) difference in AT-45 group (n=11) and SA60AT group (n=11), according to the follow-up period. Positive value represents hyperopic change, whereas negative value represents myopic change in spherical equivalent (* : Mann-Whitney U test, W: week, M: month). |
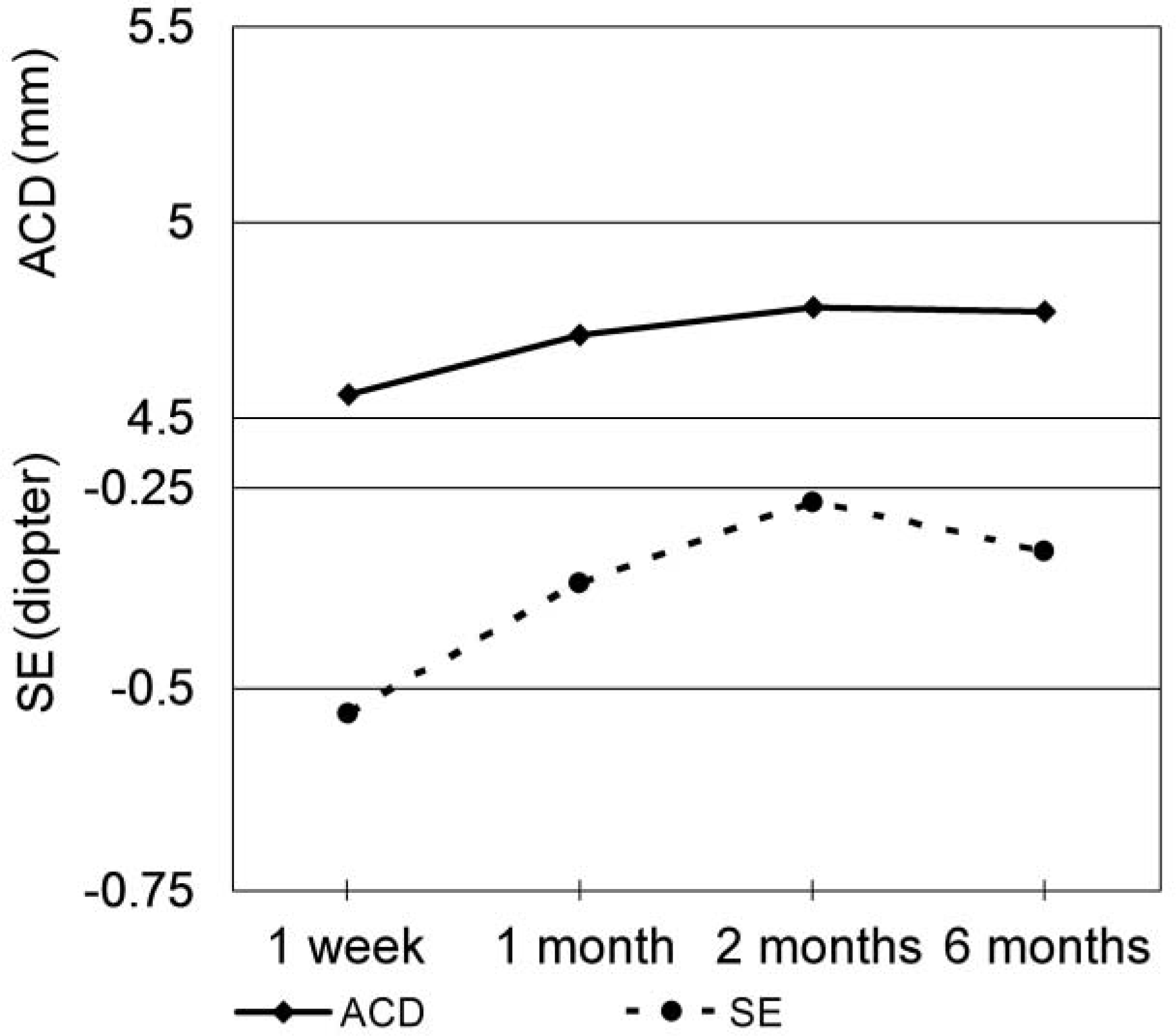 | Figure 5.Anterior chamber depth (ACD) and spherical equivalent (SE) change in AT-45 implanted group. Correlation between ACD change and SE change between 1 week and 6 months was not statistically significant (Spearman correlation analysis, P=0.223). |
Table 1.
Patients’ demographics
| AT-45 group | SA60AT group | P-value | |
|---|---|---|---|
| Male / female (number of eyes) | 7 / 4 | 6 / 5 | 1.000† |
| Age (years) | 54.55± 14.58* | 61.45±6.54* | 0.133‡ |
| Axial length (mm) | 23.67±0.43* | 23.26±0.82* | 0.088‡ |
| Implanted IOL (diopter) | 21.18± 1.87* | 20.7 5± 1.95* | 0.468‡ |
| Predicted postoperative refraction (diopter) | -0.62±0.08* | -0.60±0.18* | 0.478‡ |
Table 2.
Mean anterior chamber depth (ACD) and spherical equivalent (SE) difference in AT-45 group (n=11) and SA60AT group (n=11), according to the follow-up (F/U) period. Positive value represents deepening of the anterior chamber, whereas negative value represents shallowing of the anterior chamber in ACD change. Positive value represents hyperopic change, whereas negative value represents myopic change in SE in SE change
| F/U period | AT-45 | SA60AT | P-value | |
|---|---|---|---|---|
|
Mean±SD (mm) |
||||
| ACD | 1W∼1M | 0.14±0.25 | 0.03±0.18 | 0.52* |
| 1M∼2M | 0.07±0.20 | -0.01±0.15 | 0.32* | |
| 2M∼6M | -0.02±0.24 | -0.04±0.18 | 0.89* | |
| 1W∼6M | 0.19±0.28 | -0.02±0.25 | 0.02* | |
|
Mean±SD (diopter) |
||||
| SE | 1W∼1M | 0.15±0.37 | 0.05±0.20 | 0.33* |
| 1M∼2M | 0.10±0.30 | 0.03±0.25 | 0.56* | |
| 2M∼6M | -0.06±0.32 | -0.08±0.18 | 0.94* | |
| 1W∼6M | 0.20±0.50 | 0.01±0.31 | 0.19* | |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download