Abstract
Klebsiella pneumonia e liver abscess has a tendency to spread to distant sites early in the course of disease and to involve multiple organs synchronously. A 59-year-old male was admitted because of liver abscess accompanied by fever and abdominal pain. The patient underwent percutaneous catheter drainage and received intravenous antibiotics. Symptom relief was achieved after the treatment as well as marked reduction in the size of the abscess. Despite proper treatment of the liver abscess, however, patient developed multiple metastatic infections in a non-concurrent manner: left and right endophthalmitis, psoas abscess, and infectious spondylitis at 5, 23, 30 and 65 days after initial manifestations of liver abscess, respectively. Each infectious episode followed one another after resolution of the former one. For each episode of metastatic infections, the patient promptly underwent treatment with systemic and local antibiotics, interventional abscess drainage, and surgical treatments as needed. The patient fully recovered without sequelae after the use of intravenous antibiotics for an extended period of time. Herein, we report a case of K. pneumoniae liver abscess complicated with delayed-onset multiple metastatic infections.
References
1. Singh S, Chaudhary P, Saxena N, Khandelwal S, Poddar DD, Biswal UC. Treatment of liver abscess: prospective randomized comparison of catheter drainage and needle aspiration. Ann Gastroenterol. 2013; 26:332–339.
2. Chung DR, Lee SS, Lee HR, et al. Korean Study Group for Liver Abscess. Emerging invasive liver abscess caused by K1 serotype Klebsiella pneumoniae in Korea. J Infect. 2007; 54:578–583.

3. Siu LK, Yeh KM, Lin JC, Fung CP, Chang FY. Klebsiella pneumoniae liver abscess: a new invasive syndrome. Lancet Infect Dis. 2012; 12:881–887.

4. Yoon JH, Kim YJ, Jun YH, et al. Liver abscess due to Klebsiella pneumoniae: risk factors for metastatic infection. Scand J Infect Dis. 2014; 46:21–26.

5. Shin SU, Park CM, Lee Y, Kim EC, Kim SJ, Goo JM. Clinical and radiological features of invasive Klebsiella pneumoniae liver abscess syndrome. Acta Radiol. 2013; 54:557–563.

6. Lee JY, Nah BK, Kim JH, et al. Septic metastatic lesions associated with klebsiella pneumoniae liver abscess. Infect Chemother. 2006; 38:95–100.
7. Rahimian J, Wilson T, Oram V, Holzman RS. Pyogenic liver abscess: recent trends in etiology and mortality. Clin Infect Dis. 2004; 39:1654–1659.

8. Lee SS, Chen YS, Tsai HC, et al. Predictors of septic metastatic infection and mortality among patients with Klebsiella pneumoniae liver abscess. Clin Infect Dis. 2008; 47:642–650.
9. Braiteh F, Golden MP. Cryptogenic invasive Klebsiella pneumoniae liver abscess syndrome. Int J Infect Dis. 2007; 11:16–22.

10. Sheu SJ, Kung YH, Wu TT, Chang FP, Horng YH. Risk factors for endogenous endophthalmitis secondary to klebsiella pneumoniae liver abscess:20-year experience in Southern Taiwan. Retina. 2011; 31:2026–2031.
11. Wang JH, Liu YC, Lee SS, et al. Primary liver abscess due to Klebsiella pneumoniae in Taiwan. Clin Infect Dis. 1998; 26:1434–1438.
Fig. 1.
(A) Initial abdominal CT scan shows multiple liver abscesses with the largest one in segment 7 (arrow). (B) Fluoroscopy image shows properly placed percutaneous catheter within the liver abscess.
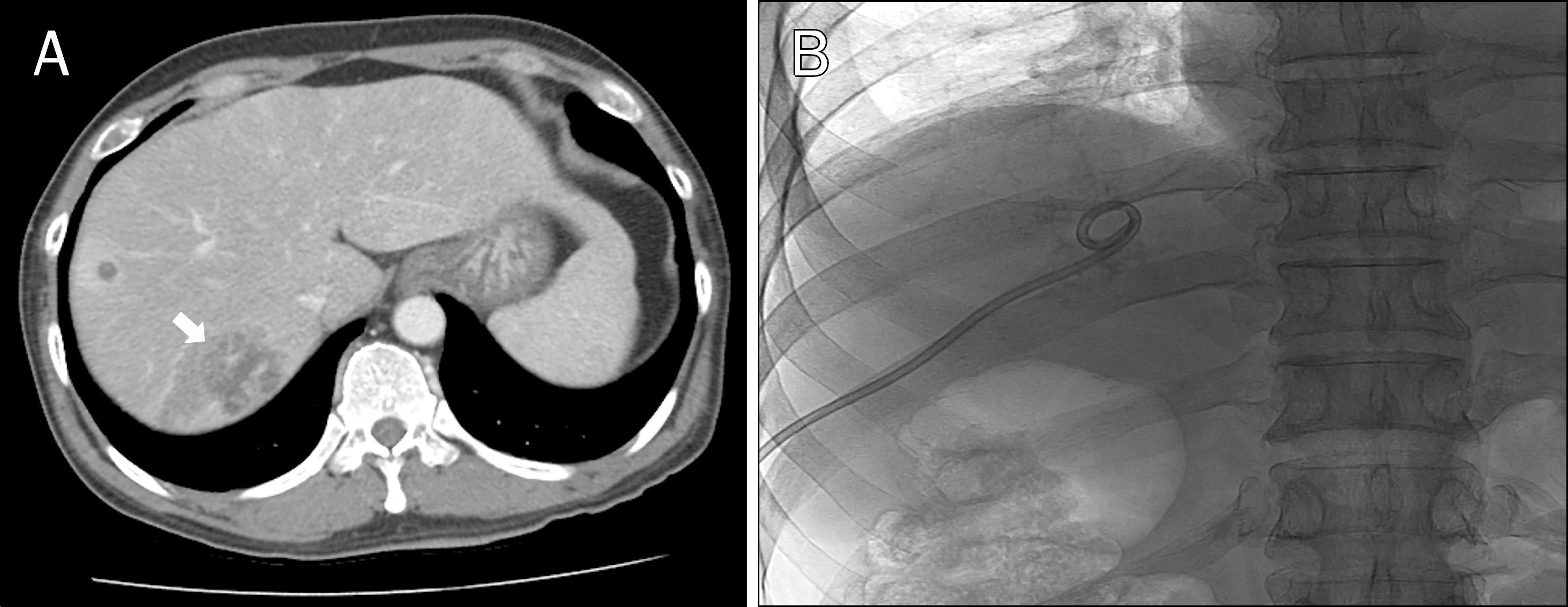
Fig. 2.
(A) Initial abdominal CT scan shows no abscess formation in both psoas muscles. (B) Abdominal CT scan taken after 30 days reveals abscess formation in left psoas muscle (arrow).
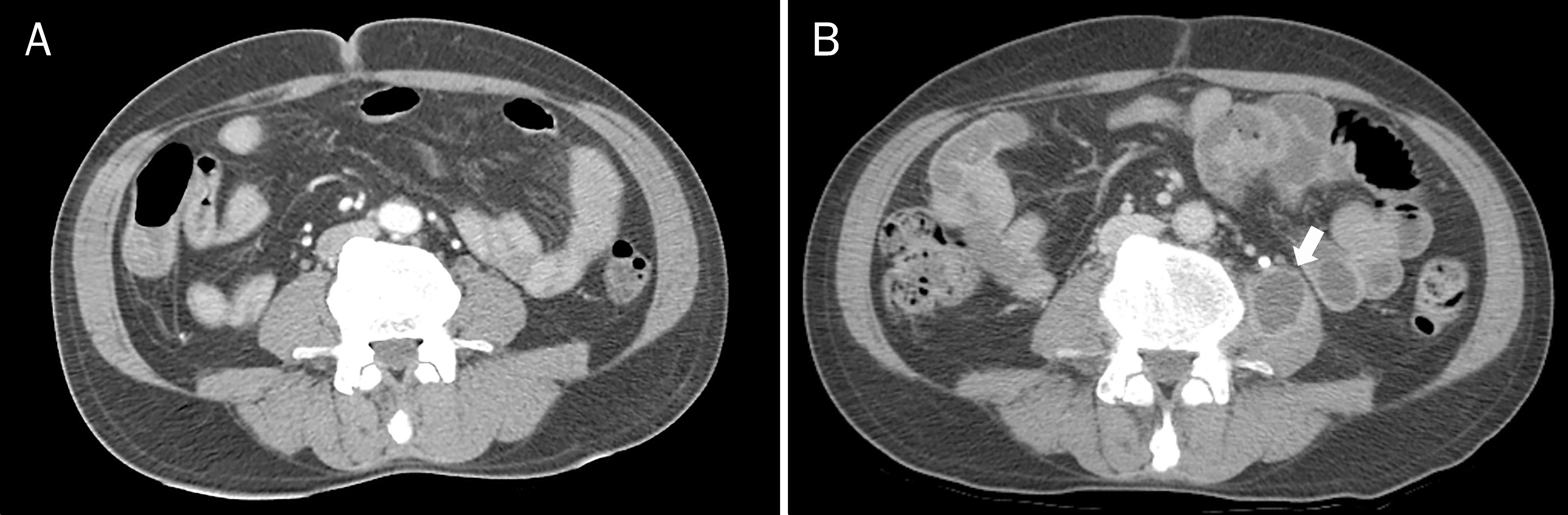
Fig. 3.
(A) Follow-up CT scan taken after 60 days shows irregular bone destruction and paravertebral enhancing soft tissue lesion (arrow) at L3 upper endplate. (B) Sagittal T1-weighted scan shows disc space narrowing and paravertebral inflammatory mass formation at L2–3 level (arrow).

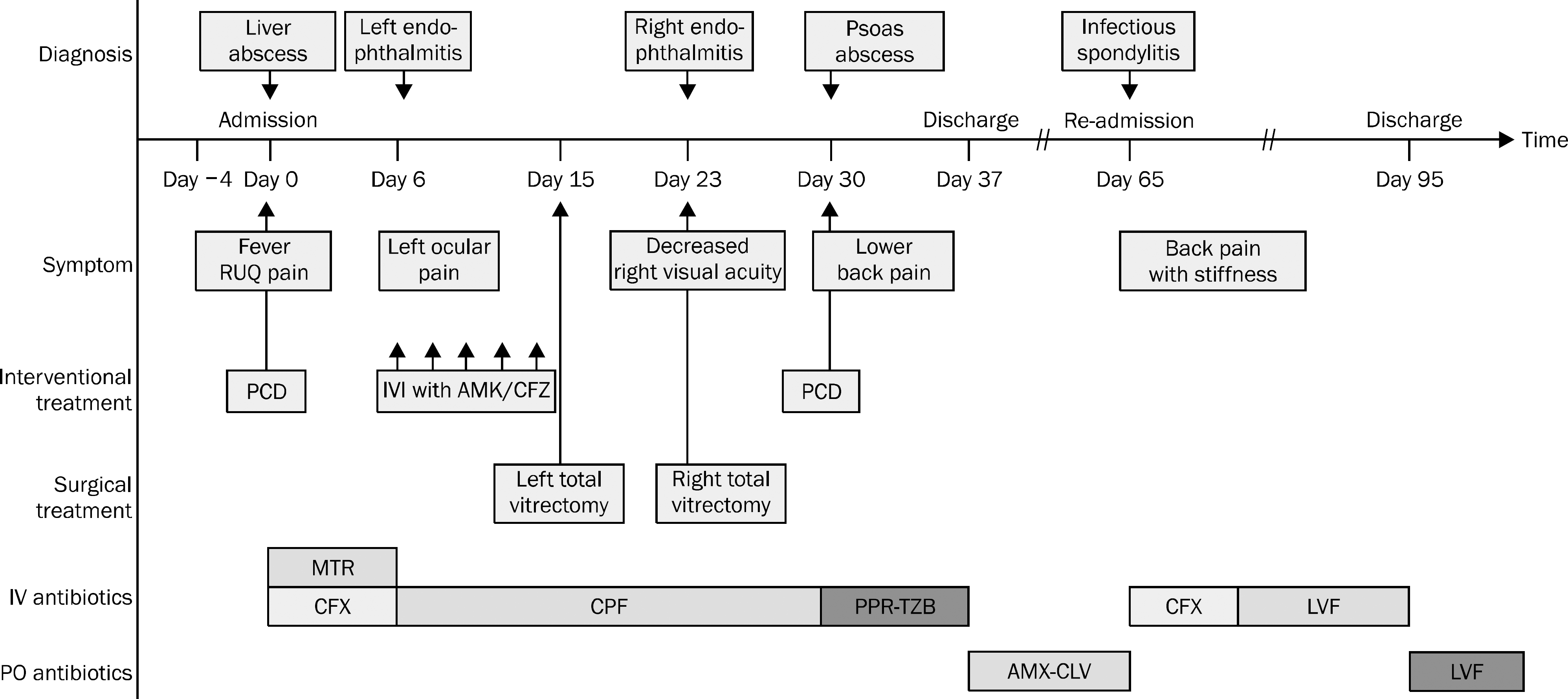
Fig. 4.
Clinical course of the patient. RUQ, right upper quadrant; PCD, percutaneous catheter drainage; IVI, intravitreal injection; AMK, amikacin; CFZ, ceftazidime; MTR, metronidazole; CFX, ceftriaxone; CPF, ciprofloxacin; PPR-TZB, piperacillin-tazobactam; AMX-CLV, amoxicillin- clavulanate; LVF, levofloxacin; IV, intravenous; PO, per oral.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download