Abstract
Background/Aims
Adenoma detection rate (ADR) is widely used as an index of colonoscopy quality management. Although advanced adenomas can be found less frequently than non-advanced adenomas, advanced adenomas have a higher clinical significance during screening for colorectal cancer. The aim of this study was to investigate the correlation between advanced and non-advanced ADR among colonoscopists.
Methods
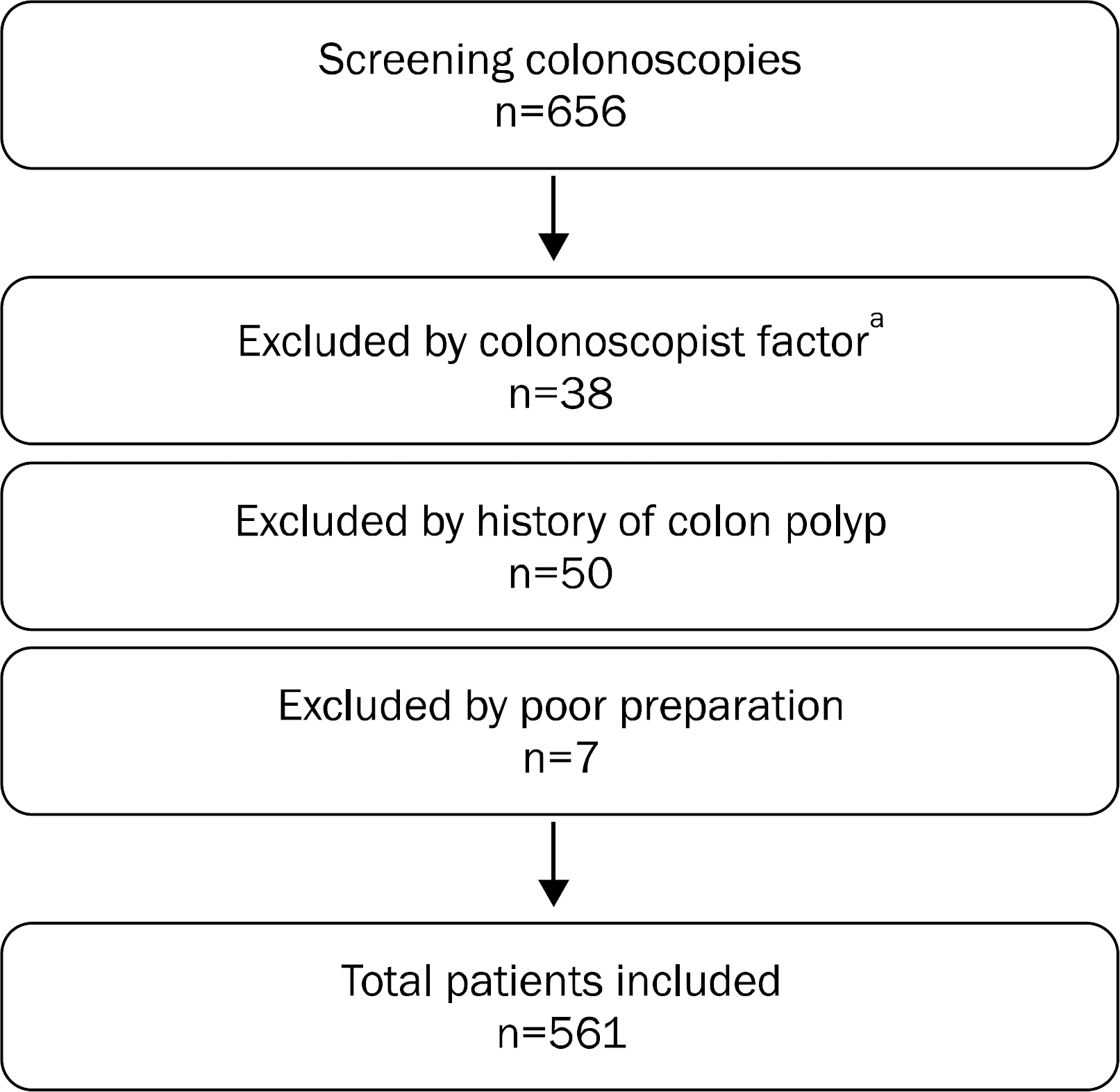
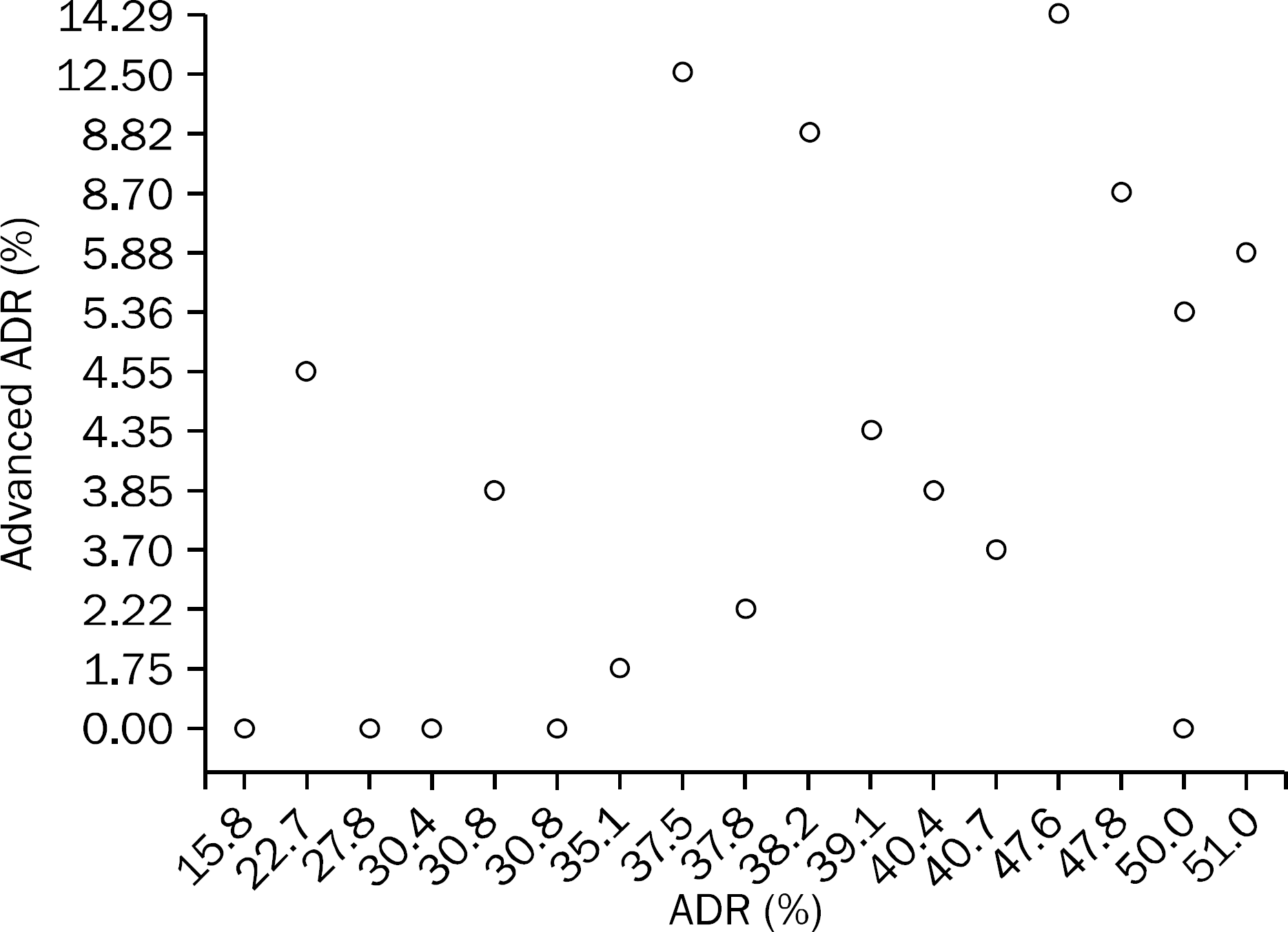
This study is an observational study of a cohort of patients undergoing screening colonoscopy between 2009 and 2010. We collected the data on patients' characteristics and colonoscopic findings. The detection rates of adenoma and advanced adenoma were calculated. Logistic regression was used to determine the effects of variables on advanced adenoma detection, and spearman's rank-order correlation was used to evaluate the relationship between advanced ADR and ADR. Results: A total of 561 patients underwent screening colonoscopy by 18 experienced colonoscopists. Most colonoscopists had adequate (>20%) ADRs. Logistic regression showed that increased patient age (OR 1.07 per 1 year increase, 95% CI 1.009–1.133, p=0.023) and male gender (OR 1.860, 95% CI 0.764–4.529, p=0.171) were associated with advanced ADR. When colonoscopists were divided into two groups on the basis of advanced ADR of 5%, ADR was also significantly higher in the group having higher level of advanced ADR. However, there was no correlation between advanced ADR and ADR among colonoscopists as an individual.
References
1. Ministry of Health & Welfare, National Cancer Center. Cancer facts & figures 2014. Seoul: Ministry of Health & Welfare; Goyang: National Cancer Center;2014.
2. Lee SH, Park DI, Sung JM, et al. Usefulness of polyp detection rate as a quality indicator in colonoscopy. Intest Res. 2011; 9:105–111.

3. Rex DK, Cutler CS, Lemmel GT, et al. Colonoscopic miss rates of adenomas determined by back-to-back colonoscopies. Gastroenterology. 1997; 112:24–28.

4. Pickhardt PJ, Nugent PA, Mysliwiec PA, Choi JR, Schindler WR. Location of adenomas missed by optical colonoscopy. Ann Intern Med. 2004; 141:352–359.

5. Greenspan M, Rajan KB, Baig A, Beck T, Mobarhan S, Melson J. Advanced adenoma detection rate is independent of non-advanced adenoma detection rate. Am J Gastroenterol. 2013; 108:1286–1292.

6. Moon CM. Quality indicators of colonoscopy: old and news. Korean Soc Gastrointest Endosc. 2013; 49:134–136.
7. Kaminski MF, Regula J, Kraszewska E, et al. Quality indicators for colonoscopy and the risk of interval cancer. N Engl J Med. 2010; 362:1795–1803.

8. Ferlitsch M, Reinhart K, Pramhas S, et al. Sex-specific prevalence of adenomas, advanced adenomas, and colorectal cancer in individuals undergoing screening colonoscopy. JAMA. 2011; 306:1352–1358.

9. Choe JW, Chang HS, Yang SK, et al. Screening colonoscopy in asymptomatic average-risk Koreans: analysis in relation to age and sex. J Gastroenterol Hepatol. 2007; 22:1003–1008.

10. Park HW, Byeon JS, Yang SK, et al. Colorectal neoplasm in asymptomatic average-risk Koreans: the KASID prospective multicenter colonoscopy survey. Gut Liver. 2009; 3:35–40.

11. Regula J, Rupinski M, Kraszewska E, et al. Colonoscopy in colorectal-cancer screening for detection of advanced neoplasia. N Engl J Med. 2006; 355:1863–1872.

12. Barclay RL, Vicari JJ, Doughty AS, Johanson JF, Greenlaw RL. Colonoscopic withdrawal times and adenoma detection during screening colonoscopy. N Engl J Med. 2006; 355:2533–2541.

13. Pox CP, Altenhofen L, Brenner H, Theilmeier A, Von Stillfried D, Schmiegel W. Efficacy of a nationwide screening colonoscopy program for colorectal cancer. Gastroenterology. 2012; 142:1460–1467.e2.

14. Nagorn A, Katic V, Zivkovic V, Stanojevic G. Advanced colorectal adenoma. Arch Oncol. 2004; 12(Suppl 1):59–60.
15. Imperiale T, Glowinski EA, Lin-Cooper C, Ransohoff DF. Tailoring colorectal cancer screening by considering risk of advanced proximal neoplasia. Am J Med. 2012; 125:1181–1187.

Table 1.
Demographic Characteristics of the Participants Who Underwent Screening Colonoscopy
| Age group (yr) | Male | Female | Total |
|---|---|---|---|
| 41–50 | 62 | 35 | 97 (17.3) |
| 51–60 | 198 | 135 | 333 (59.3) |
| 61–70 | 64 | 49 | 113 (20.1) |
| >71 | 5 | 13 | 18 (3.2) |
| Total | 329 (58.6) | 232 (41.4) | 561 |
Table 2.
Adenoma and Advanced Adenoma Detection Rates of the Individual Colonoscopist
Table 3.
Comparison of Adenoma Detection Rates of Colonoscopists on the Basis of Advanced Adenoma Detection Rate
| Advanced ADR Mean | ADR (%) | p-value a | OR (95% CI) |
|---|---|---|---|
| ≤3% | 41.98 | 0.078 | 1.377 (0.964–1.966) |
| >3% | 33.16 | ||
| ≤4% | 43.49 | 0.064 | 1.381 (0.981–1.944) |
| >4% | 34.93 | ||
| ≤5% | 46.77 | 0.009 | 1.613 (1.125–2.313) |
| >5% | 34.72 | ||
| ≤6% | 42.55 | 0.674 | 1.113 (0.675–1.837) |
| >6% | 38.33 | ||
| ≤10% | 43.24 | 0.91 | 0.942 (0.338–2.631) |
| >10% | 38.74 |
Table 4.
Logistic Regression Analysis of Advanced Adenomas with Increasing Patient Age, Male Gender, and Withdrawal Time
| Patients, n (%) | p-value a | OR (95% CI) | |
|---|---|---|---|
| Age group (yr) | |||
| 41–50 | 97 (17.3) | − | 1 |
| 51–60 | 333 (59.3) | 0.1 | 5.486 (0.723–41.62) |
| 61–70 | 113 (20.1) | 0.408 | 2.618 (0.268–25.59) |
| >71 | 18 (3.2) | 0.013 | 19.2 (1.87–196.8) |
| Withdrawal time (min) Sex | <0.001 | 1.191 (1.094–1.296) | |
| Female | 232 (41.4) | 1 | |
| Male | 329 (58.6) | 0.171 | 1.860 (0.764–4.529) |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download