References
1. van Geenen EJ, van der Peet DL, Bhagirath P, Mulder CJ, Bruno MJ. Etiology and diagnosis of acute biliary pancreatitis. Nat Rev Gastroenterol Hepatol. 2010; 7:495–502.

2. Forsmark CE, Baillie J. AGA Institute Clinical Practice and Economics Committee; AGA Institute Governing Board. AGA Institute technical review on acute pancreatitis. Gastroenterology. 2007; 132:2022–2044.

3. Uhm MS, Kim YS, Suh SC, et al. Acute pancreatitis induced by traditional acupuncture therapy. Eur J Gastroenterol Hepatol. 2005; 17:675–677.

4. Puri R, Vilmann P. Endoscopic ultrasound scanning in gallstone disease. Scand J Gastroenterol. 2006; 41:1369–1381.

Go to : 
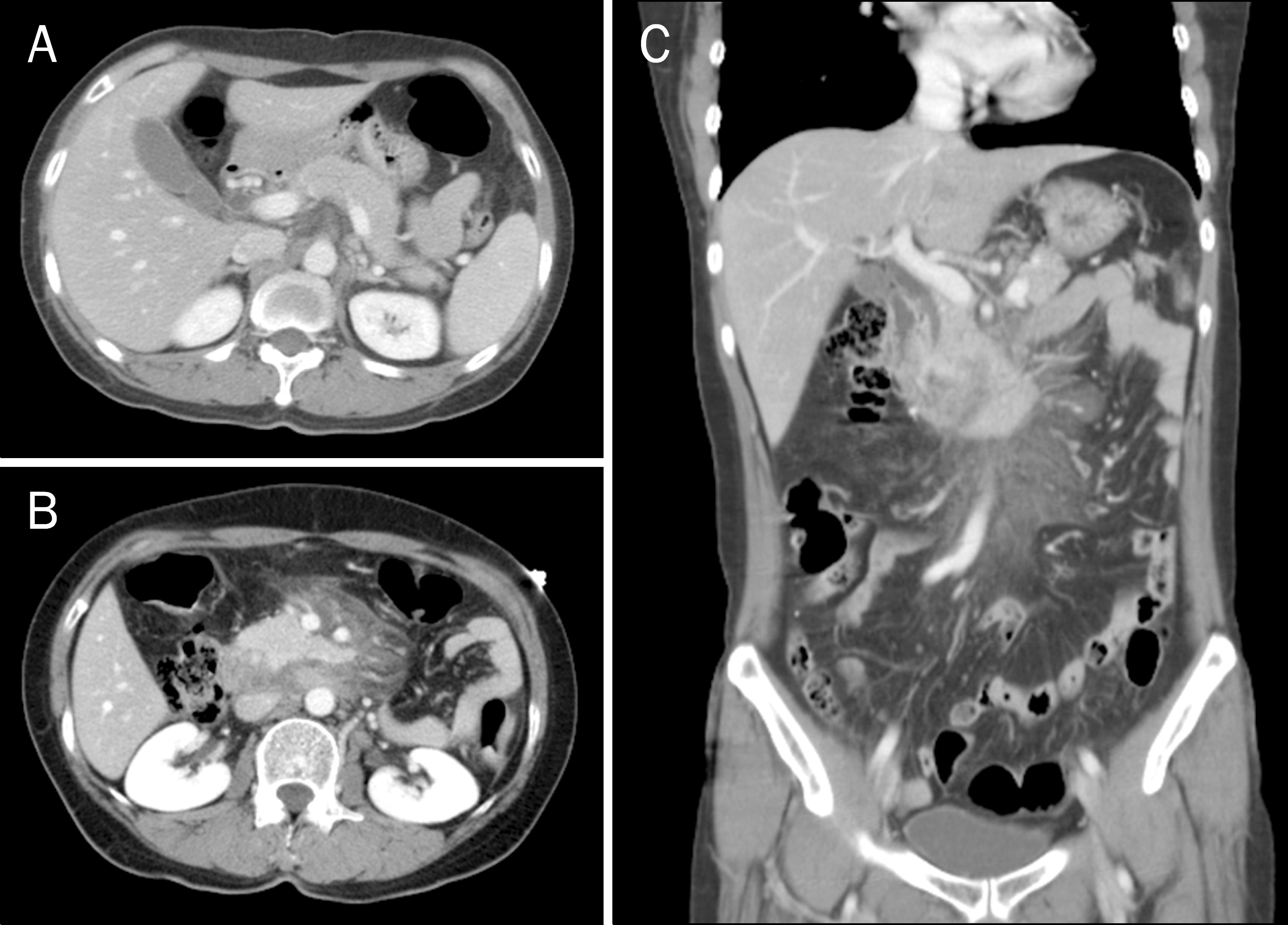 | Fig. 1.Initial abdominal CT scan. (A) Entrapped free air between stomach and pancreas is seen on axial scan, along with (B) edematous change of duodenal wall and swelling of pancreatic head with peripancreatic inflammation. (C) Mildly dilated common bile duct without stone and localized mesenteric infiltrations and haziness can also be observed. |
 | Fig. 2.Abdominal CT scan taken 12 days after admission. (A) Pancreatic head swelling is more aggravated, but (B) duodenal wall edema and mesenteric infiltrations have improved. |




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download