Abstract
Neuroendocrine tumors of the extrahepatic biliary tree are extremely rare malignancies accounting for 0.2–2.0% of all gastrointestinal carcinoid tumors. Neuroendocrine tumors obstructing the biliary tree are extremely difficult to diagnose preoperatively and nearly impossible to differentiate from cholangiocarcinoma. Statistically, the most common anatomic location in the biliary tree is the common bile duct, followed by the perihilar region. Herein, we present a case of a small cell neuroendocrine carcinoma of the hilum in a 79-year-old man following laparotomy. To our knowledge, this is the first case of small cell type neuroendocrine carcinoma of hilar bile duct reported in Korea.
References
1. Klimstra DS, Modlin IR, Adsay NV, et al. Pathology reporting of neuroendocrine tumors: application of the Delphic consensus process to the development of a minimum pathology data set. Am J Surg Pathol. 2010; 34:300–313.

2. Ganetsky A, Bhatt V. Gastroenteropancreatic neuroendocrine tumors: update on therapeutics. Ann Pharmacother. 2012; 46:851–862.

3. Cho MY, Kim JM, Sohn JH, et al. The Gastrointestinal Pathology Study Group of Korean Society of Pathologists. Current trends of the incidence and pathological diagnosis of gastroenteropancreatic neuroendocrine tumors (GEP-NETs) in Korea 2000–2009: multicenter study. Cancer Res Treat. 2012; 44:157–165.

4. Yao JC, Hassan M, Phan A, et al. One hundred years after “carcinoid”: epidemiology of and prognostic factors for neuroendocrine tumors in 35,825 cases in the United States. J Clin Oncol. 2008; 26:3063–3072.

5. Chamberlain RS, Blumgart LH. Carcinoid tumors of the extrahepatic bile duct. A rare cause of malignant biliary obstruction. Cancer. 1999; 86:1959–1965.
6. Judge DM, Dickman PS, Trapukdi S. Nonfunctioning argyrophilic tumor (APUDoma) of the hepatic duct: simplified methods of detecting biogenic amines in tissue. Am J Clin Pathol. 1976; 66:40–45.

7. Brown WM 3rd, Henderson JM, Kennedy JC. Carcinoid tumor of the bile duct. A case report and literature review. Am Surg. 1990; 56:343–346.
8. Gembala RB, Arsuaga JE, Friedman AC, et al. Carcinoid of the intrahepatic ducts. Abdom Imaging. 1993; 18:242–244.

9. Sankary HN, Foster P, Frye E, Williams JW. Carcinoid tumors of the extrahepatic bile duct: an unusual cause of bile duct obstruction. Liver Transpl Surg. 1995; 1:122–123.

10. Ferrone CR, Tang LH, D'Angelica M, et al. Extrahepatic bile duct carcinoid tumors: malignant biliary obstruction with a good prognosis. J Am Coll Surg. 2007; 205:357–361.

11. Schmitt TM, Bonatti H, Hagspiel KD, Iezzoni J, Northup P, Pruett TL. Carcinoid of the bile duct bifurcation. J Am Coll Surg. 2008; 206:399.

12. Park SY, Lee SH, Kim JY, et al. A case of large cell neuroendocrine cell carcinoma in the hilar bile duct. Korean J Med. 2011; 80(Suppl 2):S137–S141.
13. Kim J, Lee WJ, Lee SH, et al. Clinical features of 20 patients with curatively resected biliary neuroendocrine tumours. Dig Liver Dis. 2011; 43:965–970.

14. Lee SS, Lee JL, Ryu MH, et al. Extrapulmonary small cell carcinoma: single center experience with 61 patients. Acta Oncol. 2007; 46:846–851.
15. Kim SH, Park YN, Yoon DS, Lee SJ, Yu JS, Noh TW. Composite neuroendocrine and adenocarcinoma of the common bile duct associated with Clonorchis sinensis: a case report. Hepatogastroenterology. 2000; 47:942–944.
16. Kim JH, Lee SH, Park J, et al. Extrapulmonary small-cell carcinoma: a single-institution experience. Jpn J Clin Oncol. 2004; 34:250–254.

17. Park HW, Seo SH, Jang BK, et al. A case of primary small cell carcinoma in the common bile duct. Korean J Gastroenterol. 2004; 43:260–263.
18. Jeon WJ, Chae HB, Park SM, Youn SJ, Choi JW, Kim SH. A case of primary small cell carcinoma arising from the common bile duct. Korean J Gastroenterol. 2006; 48:438–442.
19. Cho SB, Park SY, Joo YE. Small cell carcinoma of extrahepatic bile duct presenting with hemobilia. Korean J Gastroenterol. 2009; 54:186–190.
Fig. 1.
(A, B) Contrast-enhanced CT image shows a diffusely infiltrating soft-tissue mass at the hilum (arrows) that extends along the gallbladder neck and cystic duct.
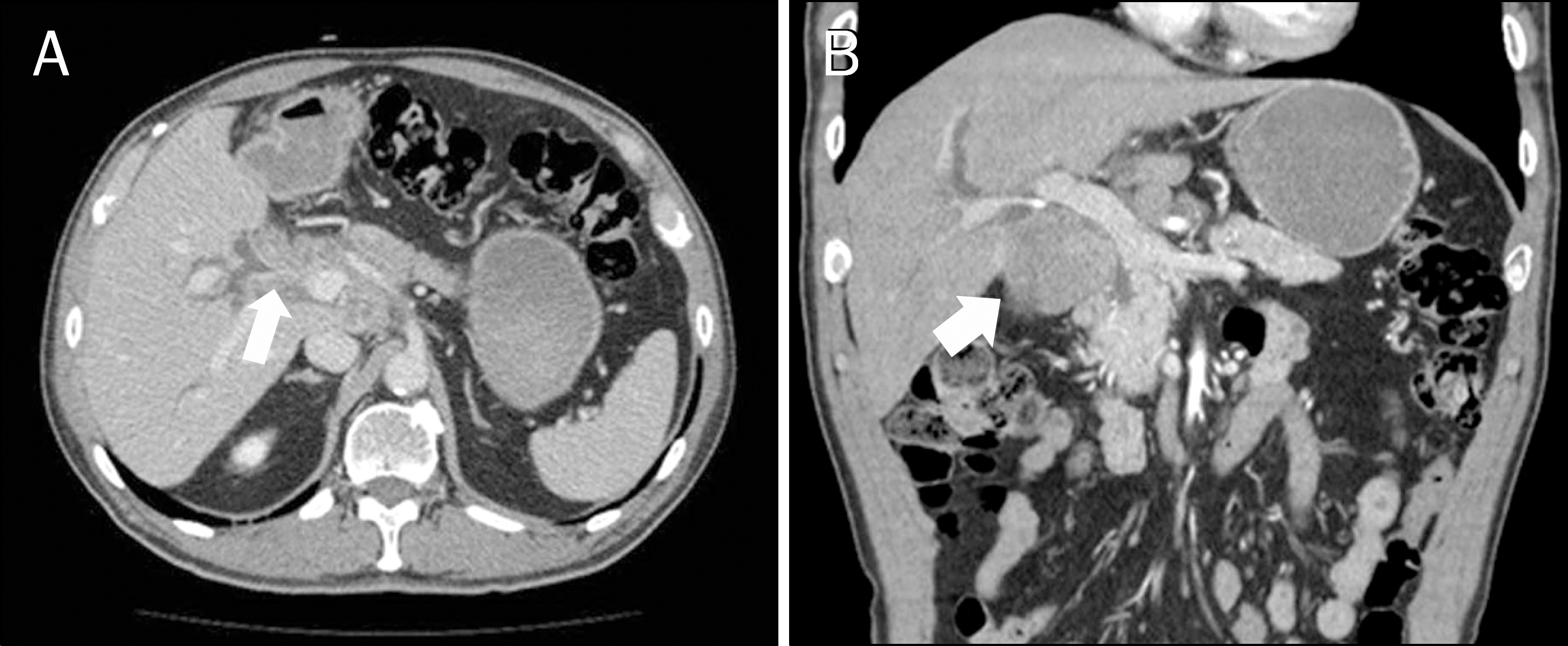
Fig. 2.
Magnetic resonance cholangiopancreatography demonstrates low signal intensity mass involving the hepatic duct confluence (arrow). Both the right and left hepatic ducts are dilated.
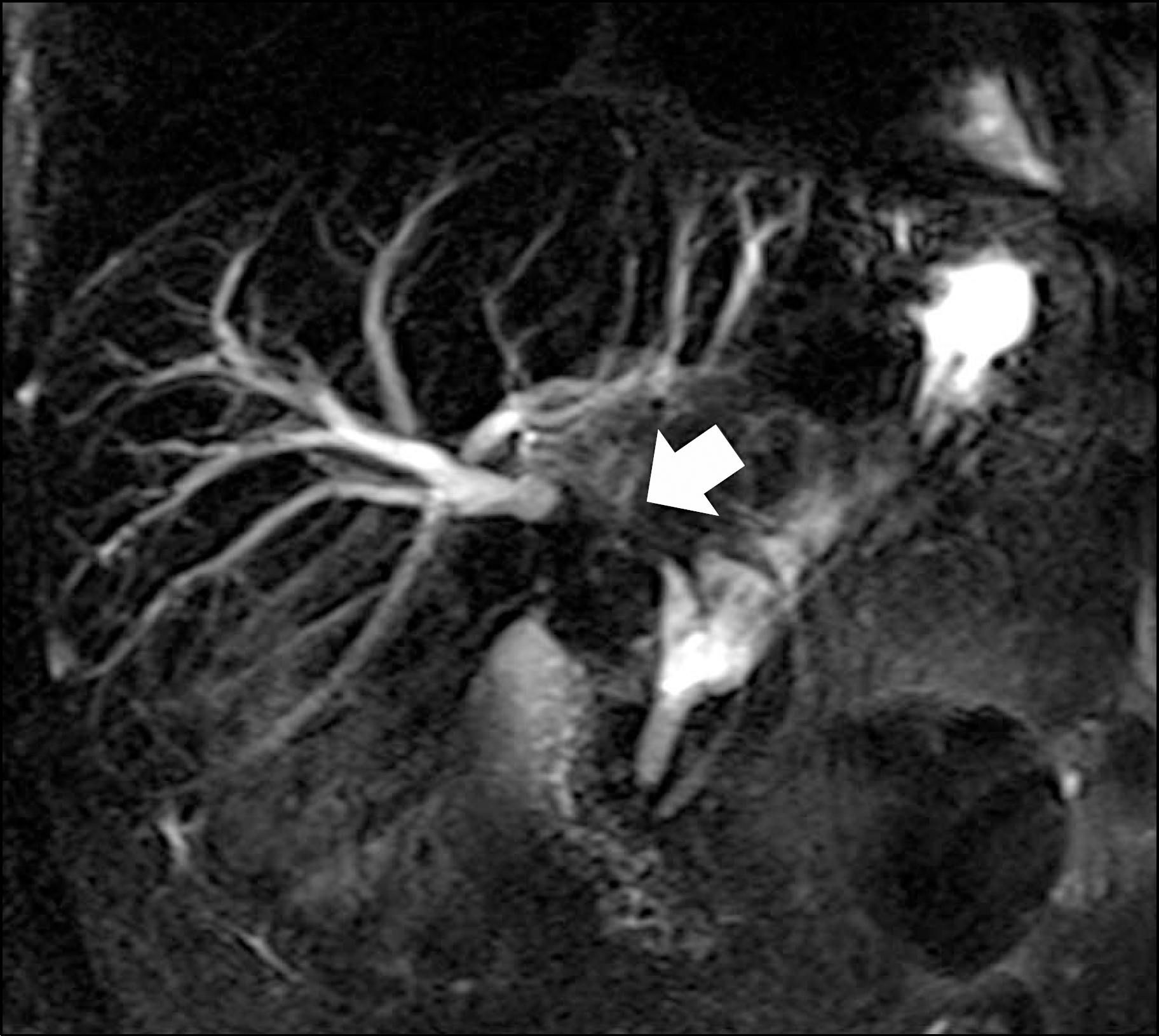
Fig. 4.
Histopathological findings. (A) The tumor cells are composed predominantly of small to medium-sized round or oval cells with hyperchromatic nuclei, inconspicuous nucleoli, and scanty cytoplasm (H&E, ×400). (B) Tumor cells are stained positive for synaptophysin immunohistochemistry, which indicates the presence of a neuroendocrine tumor (×200).
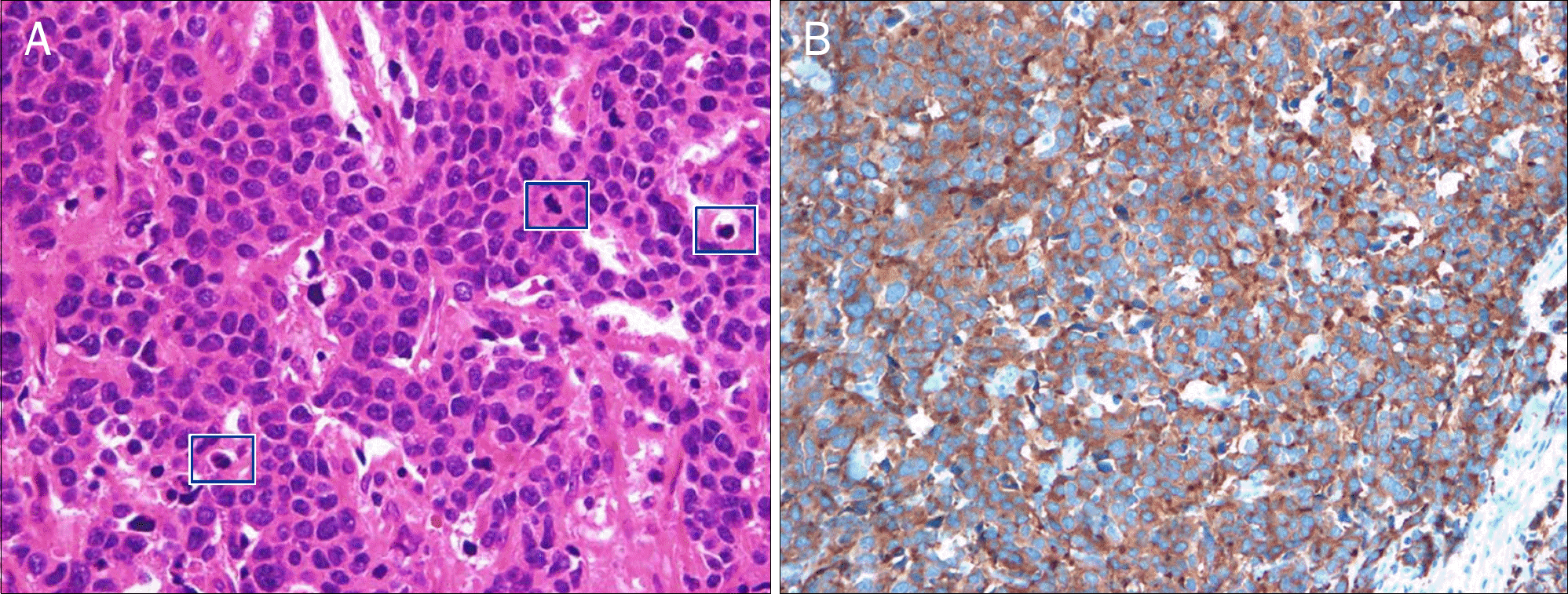
Table 1.
Data on Hilar Neuroendocrine Tumors
Table 2.
Reported Cases of Small Cell Neuroendocrine Tumors of Bile Duct in Korea




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download