Abstract
Anisakiasis usually occurs in the stomach and can easily be diagnosed by digestive tract endoscopy as opposed to enteric anisakiasis which is very rare and difficult to be diagnosed definitively. The most important and useful tool in diagnosing enteric anisakiasis is obtaining an accurate patient history of having eaten raw fish before the onset of symptoms. We report a case of small bowel obstruction caused by acute invasive enteric anisakiasis. A 60-year-old woman visited the emergency room suffering from sudden abdominal pain. She had eaten raw fish 1 day before the onset of symptom. Radiologic studies showed small bowel obstruction. However, no definitive cause could be found. An emergency laparotomy revealed edematous and dilated proximal jejunum and a focal stenosis of the distal jejunum. Segmental resection of the jejunum was performed, and histopathological examination revealed enteric anisakiasis. The patient was discharged on the 7th day after surgery following an uneventful course of recovery.
Go to : 
REFERENCES
1. van Thiel P, Kuipers FC, Roskam RT. A nematode parasitic to herring, causing acute abdominal syndromes in man. Trop Geogr Med. 1960; 12:97–113.
2. Caramello P, Vitali A, Canta F, et al. Intestinal localization of anisakiasis manifested as acute abdomen. Clin Microbiol Infect. 2003; 9:734–737.

4. Ishikura H, Kikuchi K, Nagasawa K, et al. Anisakidae and anisakidosis. Prog Clin Parasitol. 1993; 3:43–102.

5. Pellegrini M, Occhini R, Tordini G, Vindigni C, Russo S, Marzocca G. Acute abdomen due to small bowel anisakiasis. Dig Liver Dis. 2005; 37:65–67.

6. Kim LS, Lee YH, Kim S, Park HR, Cho SY. A case of anisakiasis causing intestinal obstruction. Korean J Parasitol. 1991; 29:93–96.

7. Choi SJ, Lee JC, Kim MJ, Hur GY, Shin SY, Park HS. The clinical characteristics of anisakis allergy in Korea. Korean J Intern Med. 2009; 24:160–163.

8. Matsuo S, Azuma T, Susumu S, Yamaguchi S, Obata S, Hayashi T. Small bowel anisakiosis: a report of two cases. World J Gastroenterol. 2006; 12:4106–4108.

9. Watanabe T, Ohta S, Iwamoto S, et al. Small bowel anisakiasis with self-limiting clinical course. Intern Med. 2008; 47:2191–2192.

10. Ishida M, Harada A, Egawa S, Watabe S, Ebina N, Unno M. Three successive cases of enteric anisakiasis. Dig Surg. 2007; 24:228–231.

11. Perteguer MJ, Chivato T, Montoro A, Cué llar C, Mateos JM, Laguna R. Specific and total IgE in patients with recurrent, acute urticaria caused by Anisakis simplex. Ann Trop Med Parasitol. 2000; 94:259–268.

12. Park SH, Suh JM, Shim KS, Baeg NJ, Kim BS, Moon IS. A case report of intestinal anisakiasis. Korean J Gastrointest Endosc. 1990; 10:373–375.
13. Lee CM, Choi JY, Kim JH. Intestinal obstruction caused by anisakiasis. J Korean Surg Soc. 2008; 74:154–156.
Go to : 
 | Fig. 2.Abdominopelvic CT showed dilated small bowel loops filled with fluid and target shaped wall thickening of the jejunum (arrow) with luminal narrowing. |
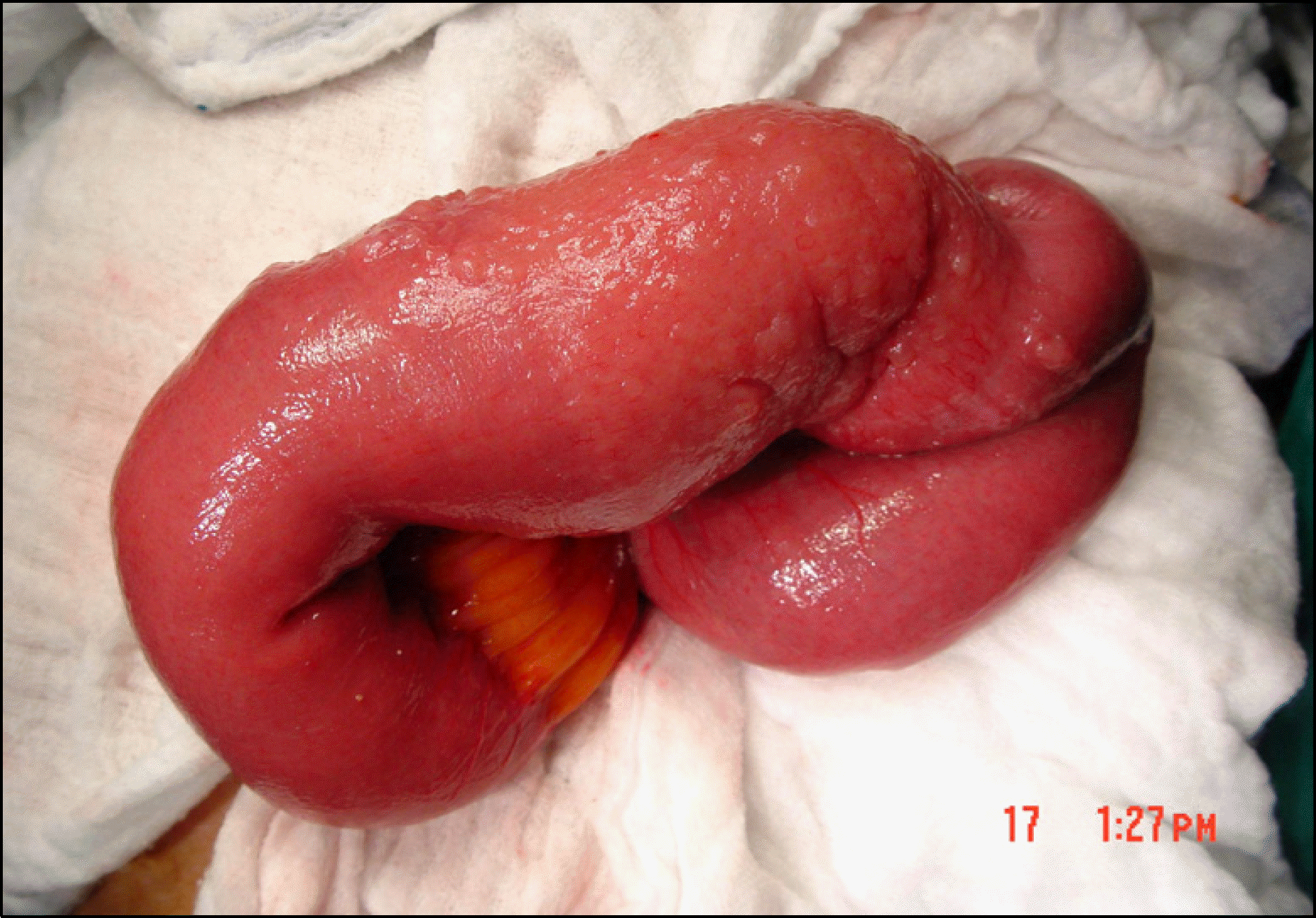 | Fig. 3.Operative finding showed focal stenosis of the distal jejunum and inflammatory change around the stenotic lesion. |
 | Fig. 4.Histopathologic findings showed the severe infiltration of inflammation and edema in all layers of the intestinal wall with a submucosal eosinophilic granuloma around larvae (arrows), which were findings of anisakiasis (A) (H&E ×40), and magnification view of square showed eosinophilic granuloma around anisakiasis larva (B) (H&E ×200). |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download