Abstract
Background/Aims
The prevalence of Helicobacter pylori (H. pylori) infection has been reported to be lower in individuals with inflammatory bowel disease (IBD) in some Western countries. We investigated H. pylori infection in Korean patients with IBD and any possible associations of H. pylori infection with drug therapy for IBD and the phenotype of Crohn's disease (CD).
Methods
We studied 316 unselected patients with IBD, including 169 ulcerative colitis (UC) patients and 147 with CD, and the control group consisted of 316 age- and gen-der-matched healthy people who received a comprehensive medical examination for a regular checkup purpose. Infection rates of H. pylori as detected by the urea breath test were compared between the IBD patients and the controls.
Results
A statistically significant difference in H. pylori infection rate was noticed between the IBD patients (25.3%) and the controls (52.5%; p<0.001), and between UC (32.0%) and CD patients (17.7%; p=0.04). Among the IBD patients, the age group of <60 and individuals with a history of taking metronidazole (13.0%; p=0.038) or ciprofloxacin (6.7%; p=0.001) were found to have a meaningfully lower infection rate, but those who did not take antibiotics still showed H. pylori infection rate significantly lower than the controls (CD 22.0% vs. UC 33.8% vs. Control 52.5%, p<0.001). With an exception of age, phenotypic characteristics showed no significant relations with H. pylori infection rate in CD patients.
Conclusions
Korean patients with IBD, particularly CD, were found to have a significantly lower H. pylori infection rate than the controls. This association was more evident in those <60 years old, which suggested that H. pylori infection might be deemed to lower possible risks of IBD in younger adults.
REFERENCES
1. El-Omar E, Penman I, Cruikshank G, Dover S, Banerjee S, Williams C. Low prevalence of Helicobacter pylori in inflammatory bowel disease: association with sulfasalazine. Gut. 1994; 35:1385–1388.
2. Halme L, Kä rkkä inen P, Rautelin H, Kosunen T, Sipponen P. High frequency of Helicobacter pylori negative gastritis in patients with Crohn's disease. Gut. 1996; 38:379–383.
3. Halme L, Rautelin H, Leidenius M, Kosunen TU. Inverse correlation between Helicobacter pylori infection and inflammatory bowel disease. J Clin Pathol. 1996; 49:65–67.
4. De Reuck M, Brad M, Otero J, Cozzoli A, Denis P, De Koster E. H. pylori prevalence in IBD patients: role of IBD treatment. Gut. 1996; 39(suppl 2):A89–90.
5. Parente F, Molteni P, Bollani S, Maconi G, Vago L, Duga PG. Prevalence of Helicobacter pylori infection and related upper gastrointestinal lesions in patients with inflammatory bowel disease. A cross-sectional study with matching. Scand J Gastroenterol. 1997; 32:1140–1146.
6. Masato M, Toshiyuki M, Sadamune H, et al. Prevalence of Helicobacter pylori infection and correlation between severity of upper gastrointestinal lesions and H. pylori infection in Japanese patients with Crohn's disease. J Gastroenterol. 2001; 36:740–747.
7. Sousa LS, Santos AM, Macedo TC, et al. Prevalence of H. pylori infection in inflammatory bowel disease: a controlled study. Gut. 1996; 39(suppl 2):A94–95.
8. Loftus EV Jr. Clinical epidemiology of inflammatory bowel disease: incidence, prevalence, and environmental influences. Gastroenterology. 2004; 126:1504–1517.

9. Patrizia D, Stefano B, Anna RD, et al. Familial clustering of Helicobacter pylori infection: population based study. BMJ. 1999; 319:537–541.
10. Guillermo I, Perez-Perez , Dietrich R, Hermann B. Epidemiology of Helicobacter pylori infection. Helicobacter. 2004; 9(suppl 1):1–6.
11. Marion R, Leslie D, Marian V, Anna H, Billy B, Brendan D. Age-specific incidence of Helicobacter pylori. Gastroenterology. 2006; 130:65–72.
12. Kim JH, Kim HY, Kim NY, et al. Seroprevalence of Helicobacter pylori infection in asymptomatic people in Korea. Korean J Intern Med. 2000; 59:388–397.
13. Yang SK, Hong WS, Min YI, et al. Incidence and prevalence of ulcerative colitis in the Songpa-Kangdong District, Seoul, Korea, 1986-1997. J Gastroenterol Hepatol. 2000; 15:1037–1042.

14. Song IS, Chang DK, Kim CY. Current status of Crohn's disease in Korea. Korean J Intern Med. 1998; 55:158–168.

15. Andreas P, Clemens D, Georg O, et al. Influence of Helicobacter pylori infection on the phenotype of Crohn's disease. Am J Gastroenterol. 1999; 94:3239–3244.
16. László P, László S, Zsuzsa O, Pá l M, Zsolt T. Lower prevalence of Helicobacter pylori infection in patients with inflammatory bowel disease but not with chronic obstructive pulmonary disease-antibiotic use in the history does not play a significant role. Helicobacter. 2004; 9:278–283.
17. Gasche C, Scholmerich J, Brynskov J, et al. A simple classification of Crohn's disease: report of the Working Party for the World Congresses of Gastroenterology, Vienna 1998. Inflamm Bowel Dis. 2000; 6:8–15.

18. Kim MH, Kim MK, Choi BY, Shin YJ. Educational dis-parities in the metabolic syndrome in a rapidly changing soci-ety-the case of South Korea. Int J Epidemiol. 2005; 34:1266–1273.

19. Nishise Y, Fukao A, Takahashi T. Risk factors for Helicobacter pylori infection among a rural population in Japan: relation to living environment and medical history. J Epidemiol. 2003; 13:266–273.
20. Mendall M, Goggin PM, Molineaux N, et al. Childhood living conditions and Helicobacter pylori seropositivity in adult life. Lancet. 1992; 339:896–897.
21. Mitchell JD, Mitchell HM, Tobias V. Acute Helicobacter pylori in an infant, associated with gastric ulceration and sero-logical evidence of intra- familial transmission. Am J Gastroenterol. 1992; 87:382–386.
22. Gent AE, Hellier MD, Grace RH, Swarbrick ET, Coggon D. Inflammatory bowel disease and domestic hygiene in infancy. Lancet. 1994; 343:766–767.

23. Montgomery SM, Pounder RE, Wakefield AJ. Infant mortality and the incidence of inflammatory bowel disease. Lancet. 1997; 349:472–473.

24. Duggan AE, Usmani I, Neal KR, Logan RF. Appendicecto-my, childhood hygiene, Helicobacter pylori status, and risk of inflammatory bowel disease: a case control study. Gut. 1998; 43:494–498.
25. Gent AE, Hellier MD, Grace RH, et al. Inflammatory bowel disease and domestic hygiene in infancy. Lancet. 1994; 343:766–767.

26. Bach JF. The effect of infections and susceptibility to autoimmune and allergic diseases. N Engl J Med. 2002; 347:911–920.
27. Christelle B, John H, Alexandra B, Dino V, Stuart B. Are Helicobacter species and Enterotoxigenic Bacteroides fragilis involved in inflammatory bowel disease. Dig Dis Sci. 2004; 49:1425–1432.
30. Tursi A. Onset of Crohn's disease after Helicobacter pylori eradication. Inflamm Bowel Dis. 2006; 12:1008–1009.
31. Jovanovic IR, Miloslavljevic TN, Jankovic GP, et al. Clinical onset of the Crohn's disease after eradication therapy of Helicobacter pylori infection. Does Helicobacter pylori inter-act with natural history of inflammatory bowel diseases? Med Sci Monit. 2001; 7:137–141.
Fig. 1.
The prevalence of Helicobacter pylori infection in the IBD patients and controls. IBD, inflammatory bowel disease; UC, ulcerative colitis; CD, Crohn's disease.
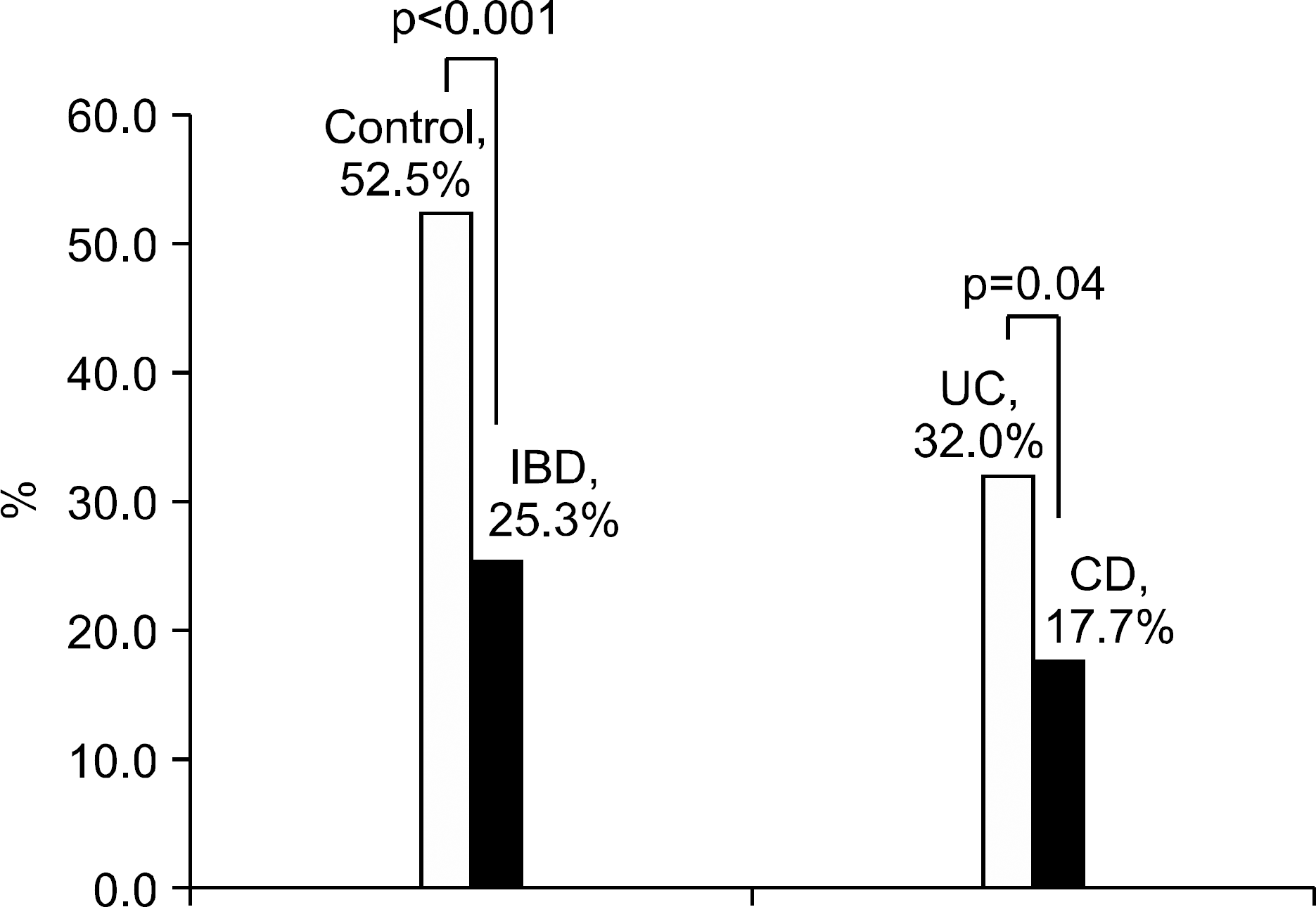
Table 1.
Clinical Characteristics of the IBD Patients and Controls
| CD | UC | Control | p | |
|---|---|---|---|---|
| Number | 147 | 169 | 316 | |
| Mean age (years)∗ | 33.5±14.5 | 44.7±14.0 | 40.7±14.2 | <0.001 |
| Male/Female | 99/48 | 107/62 | 206/110 | N.S. |
| Education (years) n | (%) | <0.001 | ||
| ≤9 | 46 | 57 | 73 | |
| (31.3%) | (33.7%) | (23.1%) | ||
| >9 | 101 | 112 | 243 | |
| (68.7%) | (66.3%) | (76.9%) | ||
| Prevalence of | 17.7 | 32.0 | 52.5 | <0.001 |
| Hp+ (%) |
Table 2.
Prevalence of Helicobacter pylori Infection in the IBD Patients and Controls by Age
| Number | Prevalence of Hp infection (%) | ||||
|---|---|---|---|---|---|
| Control (n=316) | IBD (n=316) | CD (n=147) | UC (n=169) | ||
| <30 | 167 | 31/72 (43.1%) | 14/95 (14.7%)∗ | 8/70 (11.4%)∗ | 6/25 (24.0%) |
| 30-44 | 247 | 77/135 (57%) | 26/112 (23.2%)∗ | 6/45 (13.3%)∗ | 20/67 (29.9%)∗ |
| 45-59 | 143 | 40/74 (54.1%) | 21/69 (30.4%)∗ | 8/22 (36.4%) | 13/47 (27.7%)∗ |
| ≥60 | 75 | 13/35 (51.4%) | 19/40 (47.5%) | 4/10 (40.0%) | 15/30 (50%) |
Table 3.
Prevalence of H. pylori Infection in the IBD Patients according to Drug History
Table 4.
Preva Phenotype alence of H. pylori In nfection a according to IBD
| Subgroup | Number | Prevalence of Hp infection (%) | |
|---|---|---|---|
| Crohn's disease | |||
| Age∗ | |||
| A1, <40 years | 114 | 14.7% | |
| A2, ≥40 years | 33 | 33.3% | |
| Location | |||
| L1, terminal ileum | 27 | 28.0% | |
| L2, colon | 39 | 25.0% | |
| L3, ileocolon | 74 | 14.9% | |
| L4, upper GI | 7 | 0% | |
| Behavior | |||
| B1, non-stricturing | 95 | 20.0% | |
| non-penetrating | |||
| B2, stricturing | 33 | 16.7% | |
| B3, penetrating | 19 | 17.6% | |
| Ulcerative colitis | |||
| Proctitis | 65 | 29.4% | |
| Left colitis | 53 | 31.7% | |
| Pancolitis | 51 | 35.0% | |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download