Abstract
The ectopic ovary is a rarely reported gynecologic entity. A variety of synonymous terms have been used to describe this condition, such as supernumerary ovary, accessory ovary, and ovarian implant syndrome. The etiology of ectopic ovary is poorly understood. The ectopic ovaries may occur in two ways. First, in the embryonic theories, they are believed to result from abnormal separation of a small portion of the developing and migrating ovarian primordium. Second, the accessory ovary can occur from acquired conditions such as inflammation and operations. In this report, we describe a case of the ectopic ovary with a mature cystic teratoma autoamputated into the cul-de-sac and subsequently diagnosed by laparoscopy.
Figures and Tables
Fig. 1
Transvaginal ultrasonogram. In Douglas pouch, a welldefined 5×4 cm sized cystic mass was noted. The cyst showed a smooth, regular outline with inhomogeneous internal echoes.
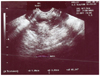
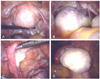
Fig. 2
T2 weighted magnetic resonance imaging (A) and fat suppression magnetic resonance imaging (B) in the transverse view of the pelvis showing left ectopic ovary (arrow) and normal right ovary (arrow head).

References
1. Kusaka M, Mikuni M. Ectopic ovary: a case of autoamputated ovary with mature cystic teratoma into the cul-de-sac. J Obstet Gynaecol Res. 2007. 33:368–370.
2. Lachman MF, Berman MM. The ectopic ovary. A case report and review of the literature. Arch Pathol Lab Med. 1991. 115:233–235.
3. Kuga T, Esato K, Takeda K, Sase M, Hoshii Y. A supernumerary ovary of the omentum with cystic change: report of two cases and review of the literature. Pathol Int. 1999. 49:566–570.
4. Ushakov FB, Meirow D, Prus D, Libson E, BenShushan A, Rojansky N. Parasitic ovarian dermoid tumor of the omentum-A review of the literature and report of two new cases. Eur J Obstet Gynecol Reprod Biol. 1998. 81:77–82.
5. Wharton LR. Two cases of supernumerary ovary and one of accessory ovary, with an analysis of previously reported cases. Am J Obstet Gynecol. 1959. 78:1101–1119.
6. Lim MC, Park SJ, Kim SW, Lee BY, Lim JW, Lee JH, et al. Two dermoid cysts developing in an accessory ovary and an eutopic ovary. J Korean Med Sci. 2004. 19:474–476.
7. Levy B, DeFranco J, Parra R, Holtz P. Intrarenal supernumerary ovary. J Urol. 1997. 157:2240–2241.
8. Moon W, Kim Y, Rhim H, Koh B, Cho O. Coexistent cystic teratoma of the omentum and ovary: report of two cases. Abdom Imaging. 1997. 22:516–518.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download