Abstract
Purpose
Laparoscopic pyeloplasty was developed as a minimally invasive alternative to an open procedure for the treatment of ureteropelvic junction (UPJ) obstruction. We present our experience with the first 30 consecutive cases of laparoscopic pyeloplasty performed at our institution.
Materials and Methods
We studied 30 patients with ureteropelvic junction obstructions who underwent laparoscopic pyeloplasty between March 2004 and March 2009. Of the 30 patients, 5 patients underwent robot-assisted laparoscopic pyeloplasty (RALP) since April 2008. Patients were divided into 4 groups according to operative procedure: group 1, early laparoscopic pyeloplasty-dismembered (E/LP-D, n=9); group 2, late la-paroscopic pyeloplasty-dismembered (L/LP-D, n=9); group 3, laparoscopic pyeloplasty-Fenger’s method (LP-F, n=7); and group 4, RALP (n=5).
Results
The mean age of the patients was 34.0±12.8 years (range, 17-61 years). A crossing vessel was present in 37.9% of cases. Mean follow-up was 30±14 months (range, 11-62 months). Mean operative time was 267.3±78.7 minutes (range, 154-460 minutes), and the average length of the postoperative hospital stay was 4.6±1.6 days (range, 3-10 days). There were no intraoperative complications or transfusion. The success rate was 73.3%. The success rates of E/LP-D, L/LP-D, LP-F, and RALP were 6/9 (66.7%), 7/9 (77.8%), 5/7 (71.4%), and 4/5 (80%), respectively, without significant difference (p>0.05). Operation time and length of hospital stay were shorter in the L/LP-D group than in the E/LP-D group.
Go to : 
REFERENCES
2.Schuessler WW., Grune MT., Tecuanhuey LV., Preminger GM. Laparoscopic dismembered pyeloplasty. J Urol. 1993. 150:1795–9.

3.Klingler HC., Remzi M., Janetschek G., Kratzik C., Marberger MJ. Comparison of open versus laparoscopic pyeloplasty techniques in treatment of uretero-pelvic junction obstruction. Eur Urol. 2003. 44:340–5.

4.Smith JA Jr. Robotically assisted laparoscopic prostatectomy: an assessment of its contemporary role in the surgical management of localized prostate cancer. Am J Surg. 2004. 188(4A Suppl):63S–7.

5.Fernbach SK., Maizels M., Conway JJ. Ultrasound grading of hydronephrosis: introduction to the system used by the Society for Fetal Urology. Pediatr Radiol. 1993. 23:478–80.

7.O'Reilly PH., Brooman PJ., Mak S., Jones M., Pickup C., Atkinson C, et al. The long-term results of Anderson-Hynes pyeloplasty. BJU Int. 2001. 87:287–9.
8.Anderson JC., Hynes W. Retrocaval ureter; a case diagnosed pre-operatively and treated successfully by a plastic operation. Br J Urol. 1949. 21:209–14.
9.Tan BJ., Smith AD. Ureteropelvic junction obstruction repair: when, how, what? Curr Opin Urol. 2004. 14:55–9.

10.Tawfiek ER., Liu JB., Bagley DH. Ureteroscopic treatment of ureteropelvic junction obstruction. J Urol. 1998. 160:1643–6.

11.Shalhav AL., Giusti G., Elbahnasy AM., Hoenig DM., McDougall EM., Smith DS, et al. Adult endopyelotomy: impact of etiology and antegrade versus retrograde approach on outcome. J Urol. 1998. 160:685–9.

12.Adeyoju AB., Hrouda D., Gill IS. Laparoscopic pyeloplasty: the first decade. BJU Int. 2004. 94:264–7.

13.Han DY., Park KS., Seo IY., Rim JS. A comparison of minimally invasive surgical techniques for ureteropelvic junction obstructions: endopyelotomy, acucise endopyelotomy, and laparoscopic pyeloplasty. Korean J Urol. 2008. 49:592–7.

14.Dimarco DS., Gettman MT., McGee SM., Chow GK., Leroy AJ., Slezak J, et al. Long-term success of antegrade endopyelotomy compared with pyeloplasty at a single institution. J Endourol. 2006. 20:707–12.
15.Janetschek G., Peschel R., Frauscher F. Laparoscopic pyelo- plasty. Urol Clin North Am. 2000. 27:695–704.
16.Jarrett TW., Chan DY., Charambura TC., Fugita O., Kavoussi LR. Laparoscopic pyeloplasty: the first 100 cases. J Urol. 2002. 167:1253–6.

18.Sundaram CP., Grubb RL 3rd., Rehman J., Yan Y., Chen C., Landman J, et al. Laparoscopic pyeloplasty for secondary ureteropelvic junction obstruction. J Urol. 2003. 169:2037–40.

19.Hwangbo K., Seo SI., Kim JC., Hwang TK. Retroperitoneo-scopic pyeloplasty. Korean J Urol. 2003. 44:624–7.
20.Kim BS., Woo SH., Han HY., Lee SB. Initial experience of laparoscopic pyeloplasty: retrograde stenting using flexible cystoscopes. Korean J Urol. 2006. 47:1302–8.

21.Iwamura M., Soh S., Irie A., Kadowaki K., Matsusita Y., Fujioka T, et al. Laparoscopic pyeloplasty for ureteropelvic junction obstruction: outcome of initial 12 procedures. Int J Urol. 2004. 11:449–55.

22.Sarle R., Tewari A., Shrivastava A., Peabody J., Menon M. Surgical robotics and laparoscopic training drills. J Endourol. 2004. 18:63–6.

23.Partin AW., Adams JB., Moore RG., Kavoussi LR. Complete robot-assisted laparoscopic urologic surgery: a preliminary report. J Am Coll Surg. 1995. 181:552–7.
24.Gettman MT., Neururer R., Bartsch G., Peschel R. Anderson-Hynes dismembered pyeloplasty performed using the da Vinci robotic system. Urology. 2002. 60:509–13.

25.Mitre AI., Brito AH., Srougi M. Laparoscopic dismembered pyeloplasty in 47 cases. Clinics. 2008. 63:631–6.

26.Inagaki T., Rha KH., Ong AM., Kavoussi LR., Jarrett TW. Laparoscopic pyeloplasty: current status. BJU Int. 2005. 95(Suppl 2):102–5.

27.Seo IY., Park SC., Oh SJ. Laparoscopic pyeloplasty with transperitoneal approach for ureteropelvic obstruction. Korean J Urol. 2005. 46:370–4.
28.Mufarrij PW., Shah OD., Berger AD., Stifelman MD. Robotic reconstruction of the upper urinary tract. J Urol. 2007. 178:2002–5.

Go to : 
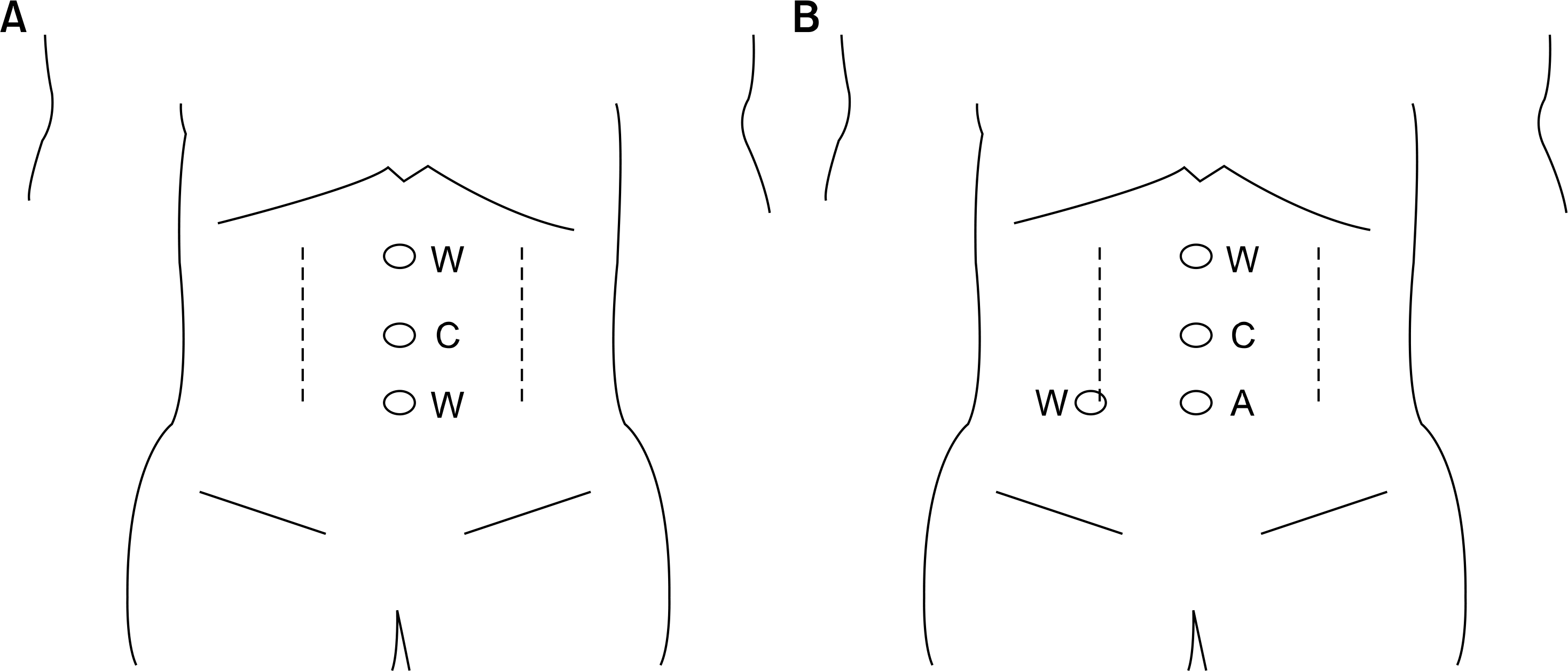 | Fig. 1.Port placement in laparoscopic pyeloplasty. (A) Laparoscopic pyeloplasty: 5 mm left working port (W) & 12 mm right working port (W) midway between the umbilicus and the xiphoid process, at least 5 cm below the umbilicus in the midline, and 12 mm camera port (C) at the umbilicus. (B) Robot-assisted laparoscopic pyeloplasty: two 8 mm working ports (W) midway between the umbilicus and the xiphoid process, pararectally below the level of the umbilicus; a 12 mm camera port (C) at the umbilicus; and a 12 mm assistant port (A) at least 5 cm below the umbilicus in the midline. |
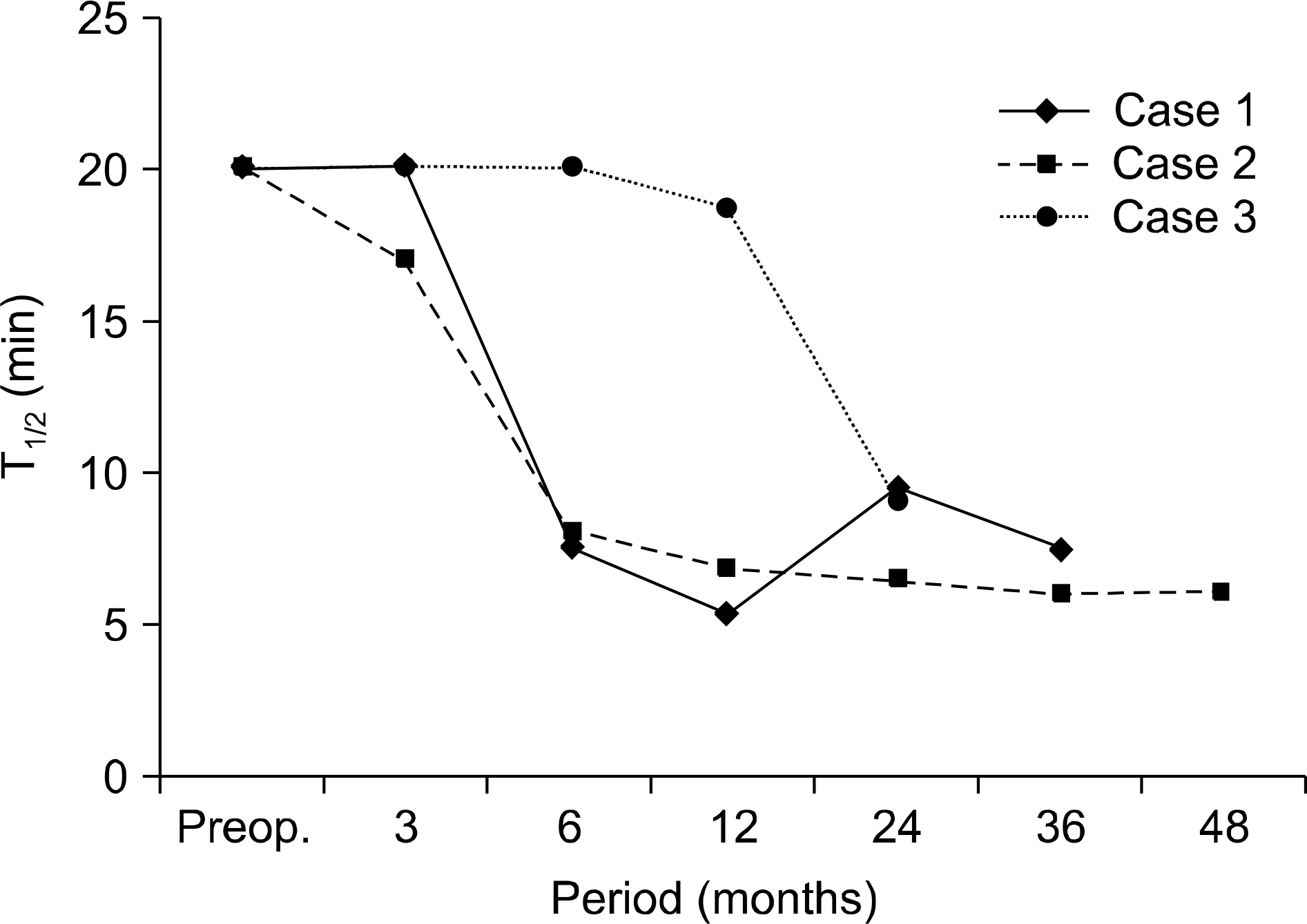 | Fig. 2.The change in T1/2 in 99mTC-MAG3 for three patients who had no symptoms preoperatively. In all three patients, T1/2 improved within 2 years after surgery. |
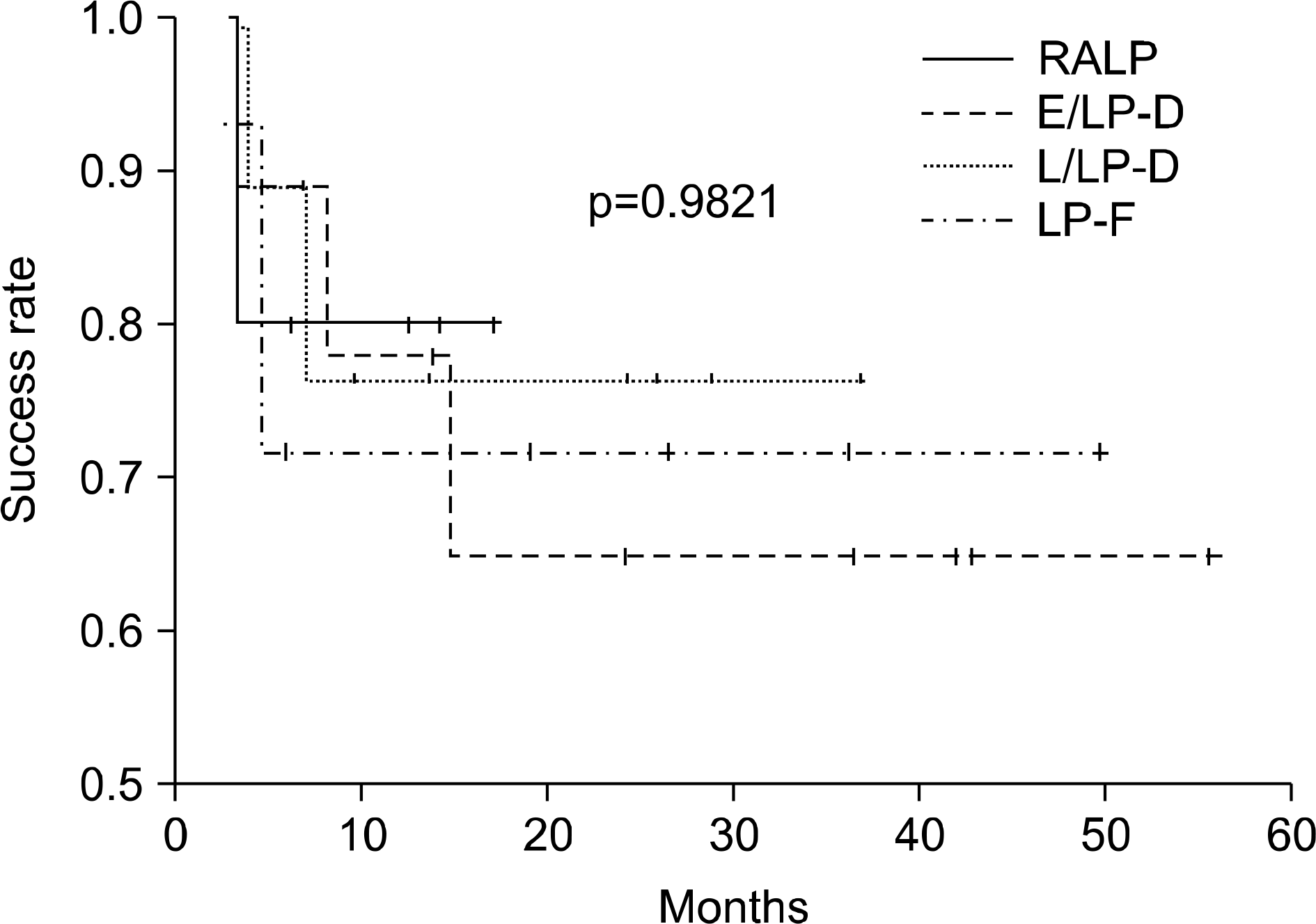 | Fig. 3.Recurrence-free survival. Of the 8 cases with failure, 7 cases failed before 10 months. Robot-assisted laparoscopic pyeloplasty showed the highest success rate with 80%, followed by late laparoscopic pyeloplasty-dismembered with 77.8%, laparoscopic pyeloplasty-Fenger with 71.4%, and early laparoscopic pyeloplasty-dismembered with 66.7%, but these rates were not significantly different (p>0.05). Because the follow-up of robot-assisted laparo-scopic pyeloplasty was short, it was hard to compare to laparo-scopic surgery. RALP: robot assisted laparoscopic pyeloplasty, E/LP-D: early laparoscopic pyeloplasty-dismembered type, L/LP-D: late laparoscopic pyeloplasty-dismembered type, LP-F: laparoscopic pyeloplasty-Fenger’s type |
Table 1.
Patient characteristics
Table 2.
Operative and postoperative outcomes
| E/LP-D (n=9) | L/LP-D (n=9) | LP-F (n=7) | RALP (n=5) | p-value | |
|---|---|---|---|---|---|
| Success | 6/9 (66.7%) | 7/9 (77.8%) | 5/7 (71.4%) | 4/5 (80%) | 0.936a |
| Operation time (min) | 334±96 (213-460) | 248±39 (196-307) | 199±43 (154-273) | 276±41 (238-340) | 0.002b |
| Length of hospital stay | 6.1±2.1 day (3-10) | 4.0±0.9 day (3-6) | 3.6±0.5 day (3-4) | 4.2±0.8 day (3-5) | 0.003b |
| Postop./Preop. renal function | 1.08±0.25 (0.58-1.38) | 1.04±0.15 (0.79-1.27) | 1.11±0.60 (0.04-1.90) | 0.92±0.14 (0.80-1.14) | ) 0.808b |
Operation time and the length of hospital stay were shorter in the L/LP-D as compared to the E/LP-D. And operation time (288±76 min vs. 199±43 min, p=0.007) and the length of hospital stay (4.9±1.7 days vs. 3.6±0.5 days, p=0.004) were in the same manner in the Fenger’s method as compared to the dismembered. E/LP-D: early laparoscopic pyeloplasty-dismembered type, L/LP-D: late laparoscopic




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download