References
2. Touraine A, Solente G, GoléL . Un syndrome osteodermopathique: la pachydermie plicaturee avec pachyperostose des extremites. Presse Med. 1935; 43:1820–4.
3. Castori M, Sinibaldi L, Mingarelli R, Lachman RS, Rimoin DL, Dallapiccola B. Pachydermoperiostosis: an update. Clin Genet. 2005; 68:477–86.

4. Rush PJ, Gladman DD, Shore A, Anhorn KA. Absence of an association between HLA typing in cystic fibrosis arthritis and hypertrophic osteoarthropathy. Ann Rheum Dis. 1991; 50:763–4.

5. Sinha GP, Curtis P, Haigh D, Lealman GT, Dodds W, Bennett CP. Pachydermoperiostosis in childhood. Br J Rheumatol. 1997; 36:1224–7.

6. Jajic Z, Jajic I, Nemcic T. Primary hypertrophic osteoarthropathy: clinical, radiologic, and scintigraphic characteristics. Arch Med Res. 2001; 32:136–42.
7. Pineda CJ, Martinez-Lavin M, Goobar JE, Sartoris DJ, Clopton P, Resnick D. Periostitis in hypertrophic osteoarthropathy: relationship to disease duration. AJR Am J Roentgenol. 1987; 148:773–8.

8. Tohtz SW, Putzier M. Secondary hypertrophic osteoarthropathy in colitis ulcerosa-a case demonstration. Z Orthop Ihre Grenzgeb. 2004; 142:486–8.
9. Matucci-Cerinic M, Sacerdoti L, Perrone C, Carossino A, Cagnoni ML, Jajic I, et al. Pachydermoperiostosis (primary hypertrophic osteoarthropathy): in vitro evidence for abnormal fibroblast proliferation. Clin Exp Rheumatol. 1992; 10(Suppl 7):57–60.
10. Silveira LH, Martinez-Lavin M, Pineda C, Fonseca MC, Navarro C, Nava A. Vascular endothelial growth factor and hypertrophic osteoarthropathy. Clin Exp Rheumatol. 2000; 18:57–62.
11. Bianchi L, Lubrano C, Carrozzo AM, Iraci S, Tomassoli M, Spera G, et al. Pachydermoperiostosis: study of epidermal growth factor and steroid receptors. Br J Dermatol. 1995; 132:128–33.

12. Maeda H, Kumagai K, Konishi F, Katayama Y, Hiyama K, Ishioka S, et al. Successful treatment of arthralgia with tamoxifen citrate in a patient with pachydermoperiostosis. Rheumatology (Oxford). 2000; 39:1158–9.

13. Jojima H, Kinoshita K, Naito M. A case of pachydermoperiostosis treated by oral administration of a bisphosphonate and arthroscopic synovectomy. Mod Rheumatol. 2007; 17:330–2.

14. Guyot-Drouot MH, Solau-Gervais E, Cortet B, Deprez X, Chastanet P, Cotten A, et al. Rheumatologic manifestations of pachydermoperiostosis and preliminary experience with bisphosphonates. J Rheumatol. 2000; 27:2418–23.
15. Matsuo A, Shuto T, Hirata G, Satoh H, Matsumoto Y, Zhao H, et al. Antiinflammatory and chondrop-rotective effects of the aminobisphosphonate incadro-nate (YM175) in adjuvant induced arthritis. J Rheumatol. 2003; 30:1280–90.
Fig. 1.
(A, B) Clubbing of fingers and toes. (C) Plain radiograph shows soft tissue swelling of the fingers. (D) Soft tissue edema and effusion of knees (right > left), and enlarged ankles. (E) Deep furrowing of forehead.

Fig. 2.
(A) Plain radiograph of lower extremity demonstrates irregular shaggy diaphyseal cortical thickening (arrows). (B) Bone scan shows increased periosteal uptake in the bilateral tibias, radii, and ulnas. Focal active bone lesion in the right patella consistent with previous fracture. (C) Knee radiograph shows periosteal and cortical thickening of tibia and fibula. (D) MRI of the right knee reveals a large effusion and irregular thickening of synovium.
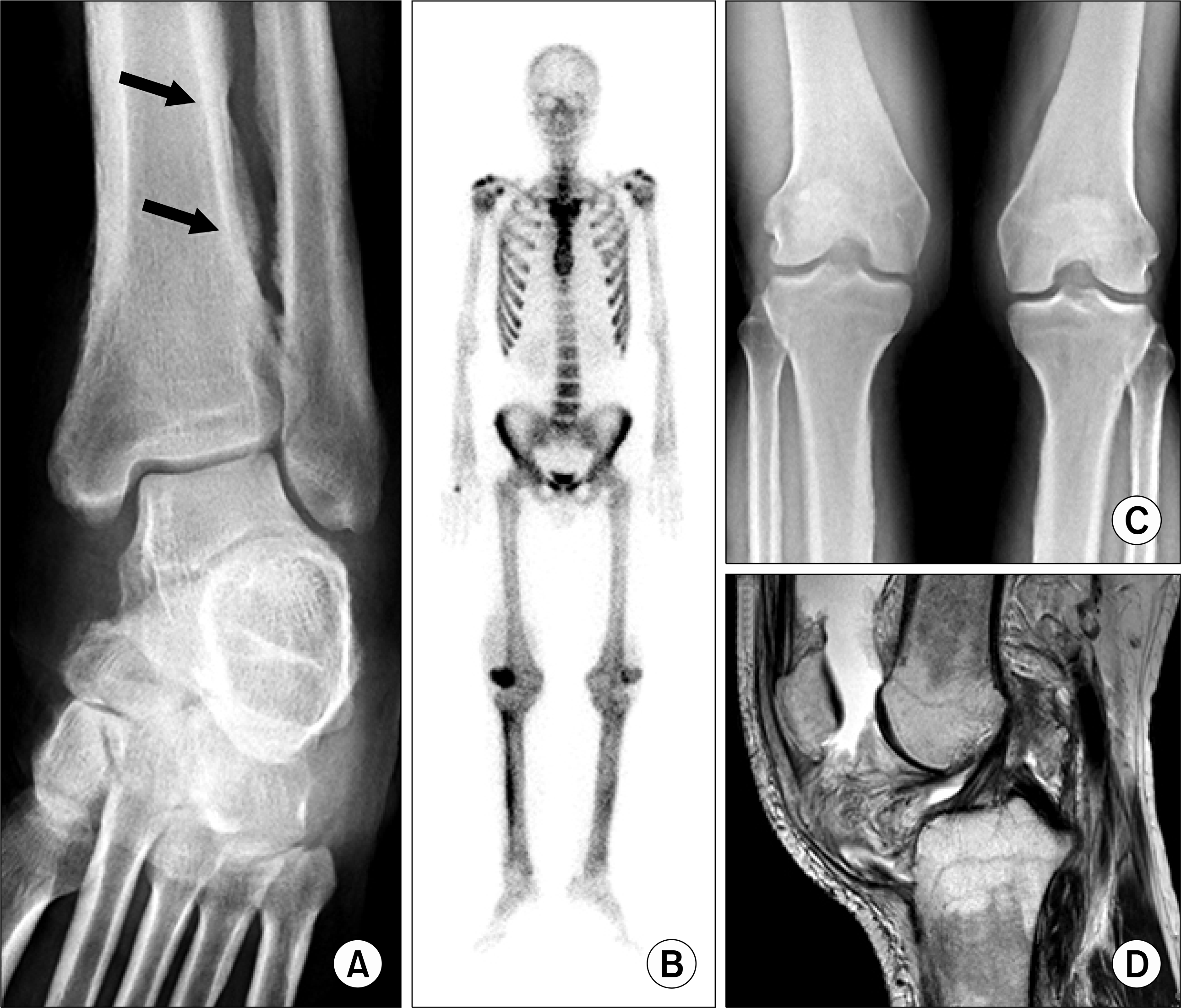
Fig. 3.
(A) Knee arthroscopy shows proliferative villonodular synovitis. (B) Chronic perivascular inflammatory infiltrates is observed in the synovial tissue (×100, H&E stain).
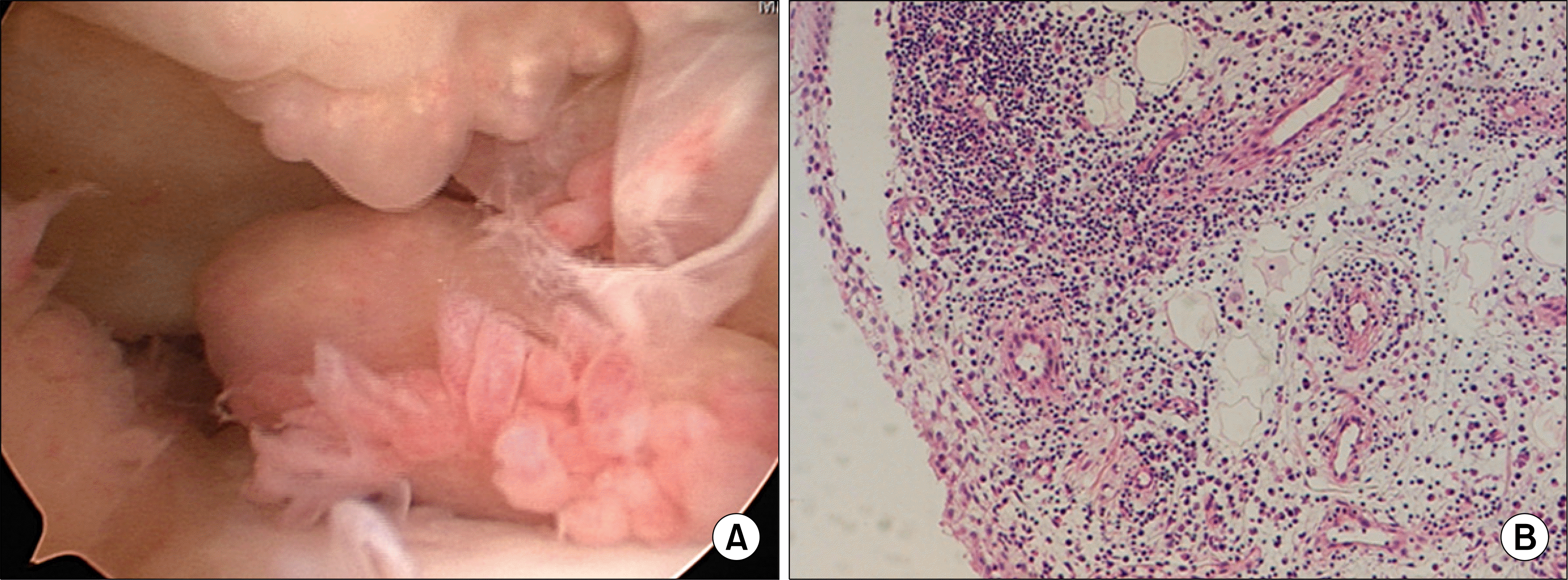
Table 1.
Major underlying diseases of secondary hypertrophic osteoarthropathy




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download