Abstract
Purpose
This study was designed to determine the effects of pre-warming on core body temperature (CBT) and hemodynamics from the induction of spinal anesthesia until 30 min postoperatively in surgical patients who undergo total hip replacement under spinal anesthesia. Our goal was to assess postoperative shivering and inflammatory response.
Methods
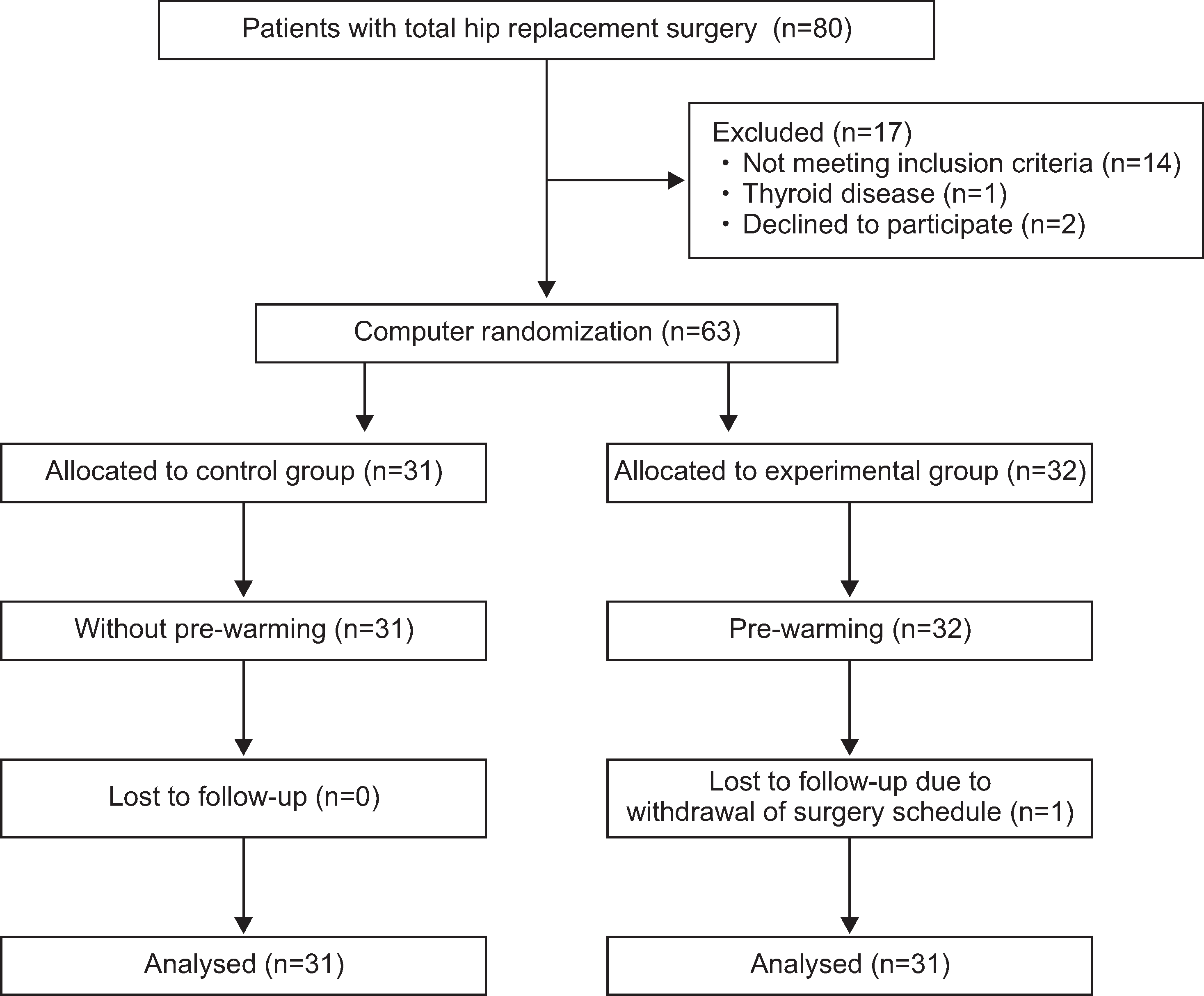
Sixty-two surgical patients were recruited by informed notice. Data for this study were collected at a 1,300-bed university hospital in Incheon, South Korea from January 15 through November 15, 2013. Data on CBT, systemic blood pressure (SBP), and heart rate were measured from arrival in the pre-anesthesia room to 3 hours after the induction of spinal anesthesia. Shivering was measured for 30 minutes post-operatively. C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) were measured pre-operatively, and 1 and 2 days postoperatively. The 62 patients were randomly allocated to an experimental group (EG), which underwent pre-warming for 30 minutes, or a control group (CG), which did not undergo pre-warming.
Results
Analysis of CBT from induction of spinal anesthesia to 3 hours after induction revealed significant interaction between group and time (F=3.85, p=.008). In addition, the incidence of shivering in the EG was lower than that in the CG (χ2=6.15, p=.013). However, analyses of SBP, heart rate, CRP, and ESR did not reveal significant interaction between time and group.
References
1. Sessler DI, Moayeri A, Støen R, Glosten B, Hynson J, Mc-Guire J. Thermoregulatory vasoconstriction decreases cutaneous heat loss. Anesthesiology. 1990; 73(4):656–660.

2. Matsukawa T, Sessler DI, Christensen R, Ozaki M, Schroeder M. Heat flow and distribution during epidural anesthesia. Anesthesiology. 1995; 83(5):961–967.

3. Kurz A, Sessler DI, Christensen R, Dechert M. Heat balance and distribution during the core-temperature plateau in anesthetized humans. Anesthesiology. 1995; 83(3):491–499.

4. Matsukawa T, Sessler DI, Sessler AM, Schroeder M, Ozaki M, Kurz A, et al. Heat flow and distribution during induction of general anesthesia. Anesthesiology. 1995; 82(3):662–673.

5. National Institute for Health and Clinical Excellence. Clinical Practice Guidelines: The management of inadvertent perioperative hypothermia in adults. London: Royal College of Nursing;2008. p. 1–567.
6. Kim EJ, Yoon H. Preoperative factors affecting the intraoperative core body temperature in abdominal surgery under general anesthesia: an observational cohort. Clinical Nurse Specialist. 2014; 28(5):268–276. http://dx.doi.org/10.1097/NUR.0000000000000069.
7. Lee SH, Yoon HS. Factors affecting intraoperative body temperature in surgical patients with laparotomy under general anesthesia. Journal of Korean Biological Nursing Science. 2015; 17(3):236–244. http://dx.doi.org/10.7586/jkbns.2015.17.3.236.

8. Kasai T, Hirose M, Matsukawa T, Takamata A, Yaegashi K, Tanaka Y. Preoperative blood pressure and catecholamines related to hypothermia during general anesthesia. Acta Anaes-thesiologica Scandinavica. 2003; 47(2):208–212. http://dx.doi.org/10.1034/j.1399-6576.2003.00048.x.

9. Matsui T, Ishikawa T, Takeuchi H, Okabayashi K, Maekawa T. Mild hypothermia promotes pro-inflammatory cytokine pro- duction in monocytes. Journal of Neurosurgical Anesthesiology. 2006; 18(3):189–193. http://dx.doi.org/10.1097/01.ana.0000188639.39844.f6.
10. Cereda M, Maccioli GA. Intraoperative temperature monitoring. International Anesthesiology Clinics. 2004; 42(2):41–54.

11. Eberhart LH, D derlein F, Eisenhardt G, Kranke P, Sessler DI, Torossian A, et al. Independent risk factors for postoperative shivering. Anesthesia and Analgesia. 2005; 101(6):1849–1857.

12. Shakya S, Chaturvedi A, Sah BP. Prophylactic low dose ketamine and odansetron for prevention of shivering during spinal anaesthesia. Journal of Anaesthesiology, Clinical Pharmacology. 2010; 26(4):465–469.
13. Frank SM, Fleisher LA, Olson KF, Gorman RB, Higgins MS, Breslow MJ, et al. Multivariate determinants of early postoperative oxygen consumption in elderly patients. Effects of shivering, body temperature, and gender. Anesthesiology. 1995; 83(2):241–249.
14. Kong MJ. Risk factors of intraoperative hypothermia in laparo-scopic abdominal surgery [Master’s thesis]. Incheon: Gachon University;2013. p. 1–42.
15. Kasai T, Hirose M, Yaegashi K, Matsukawa T, Takamata A, Tanaka Y. Preoperative risk factors of intraoperative hypothermia in major surgery under general anesthesia. Anesthesia and Analgesia. 2002; 95(5):1381–1383.

16. Kitamura A, Hoshino T, Kon T, Ogawa R. Patients with diabetic neuropathy are at risk of a greater intraoperative reduction in core temperature. Anesthesiology. 2000; 92(5):1311–1318.

17. Kongsayreepong S, Chaibundit C, Chadpaibool J, Komoltri C, Suraseranivongse S, Suwannanonda P, et al. Predictor of core hypothermia and the surgical intensive care unit. Anesthesia and Analgesia. 2003; 96(3):826–833. http://dx.doi.org/10.1213/01.ANE.0000048822.27698.28.

18. A statistical year book for 2015 major surgical case [Internet]. Seoul: National Health Insurance Service;2016. [cited 2017 May 31]. Available from:. http://www.nhis.or.kr/bbs7/boards/B0039/22280.
19. Hynson JM, Sessler DI, Moayeri A, McGuire J, Schroeder M. The effects of preinduction warming on temperature and blood pressure during propofol/nitrous oxide anesthesia. Anesthesiology. 1993; 79(2):219–228. discussion 21A-22A.

20. Horn EP, Bein B, B hm R, Steinfath M, Sahili N, H cker J. The effect of short time periods of pre-operative warming in the prevention of peri-operative hypothermia. Anaesthesia. 2012; 67(6):612–617. http://dx.doi.org/10.1111/j.1365-2044.2012.07073.x.

21. Andrzejowski J, Hoyle J, Eapen G, Turnbull D. Effect of prewarming on post-induction core temperature and the incidence of inadvertent perioperative hypothermia in patients undergoing general anaesthesia. British Journal of Anaesthesia. 2008; 101(5):627–631. http://dx.doi.org/10.1093/bja/aen272.

22. Akhtar Z, Hesler BD, Fiffick AN, Mascha EJ, Sessler DI, Kurz A, et al. A randomized trial of prewarming on patient satisfaction and thermal comfort in outpatient surgery. Journal of Clinical Anesthesia. 2016; 33:376–385. http://dx.doi.org/10.1016/j.jclinane.2016.04.041.

23. Fettes S, Mulvaine M, Van Doren E. Effect of preoperative forced-air warming on postoperative temperature and postanesthesia care unit length of stay. AORN Journal. 2013; 97(3):323–328. http://dx.doi.org/10.1016/j.aorn.2012.12.011.

24. Wong PF, Kumar S, Bohra A, Whetter D, Leaper DJ. Randomized clinical trial of perioperative systemic warming in major elective abdominal surgery. British Journal of Surgery. 2007; 94(4):421–426. http://dx.doi.org/10.1002/bjs.5631.

25. Fossum S, Hays J, Henson MM. A comparison study on the effects of prewarming patients in the outpatient surgery setting. Journal of Perianesthesia Nursing. 2001; 16(3):187–194. http://dx.doi.org/10.1053/jpan.2001.24039.

26. Sessler DI, Schroeder M, Merrifield B, Matsukawa T, Cheng C. Optimal duration and temperature of prewarming. Anesthesiology. 1995; 82(3):674–681.

27. Crossley AW, Mahajan RP. The intensity of postoperative shivering is unrelated to axillary temperature. Anaesthesia. 1994; 49(3):205–207. http://dx.doi.org/10.1111/j.1365-2044.1994.tb03422.x.

28. Kim HY, Lee KC, Lee MJ, Kim MN, Kim JS, Lee WS, et al. Comparison of the efficacy of a forced-air warming system and circulating-water mattress on core temperature and postanesthesia shivering in elderly patients undergoing total knee arthroplasty under spinal anesthesia. Korean Journal of Anesthesiology. 2014; 66(5):352–357. http://dx.doi.org/10.4097/kjae.2014.66.5.352.

29. Mekjavi IB, Bligh J. Core threshold temperatures for sweating. Canadian Journal of Physiology and Pharmacology. 1989; 67(9):1038–1044.
30. C-reactive protein: Clinical applications [Internet]. Delhi: Em-bee Diagnostics;c2002. [cited 2017 July 07]. Available from: www.embeediagnostics.com.
Table 1.
Measurement of Outcome by Time Sequence
Table 2.
Baseline Demographic and Clinical Characteristics of Subjects (N=62)
Table 3.
Comparison of Body Temperature, Systolic Blood Pressure, Heart Rate and Shivering between Control and Experimental Groups (N=62)
Table 4.
Comparison of CRP and ESR between Control and Pre-warming Groups (N=62)




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download