Abstract
Melanoma can occur as a metastasis within subcutaneous tissue, lymph nodes, or viscera without a detectable primary tumor. Among patients with metastatic melanoma of unknown primary lesion, those with endobronchial metastasis are exceedingly rare. Herein we report a case of an endobronchial and pulmonary metastasis in a patient with melanoma originating from an unknown primary site. The patient without a previous history of melanoma presented with blood-tinged sputum. Fiberoptic bronchoscopy revealed a black polypoid tumor obstructing the posterior basal segmental bronchus of the right lower lobe. A final diagnosis of the malignant melanoma was made based on an immunohistochemical study of the bronchoscopic biopsy specimen. Skin, ophthalmic, oral, and nasal examinations failed to identify occult primary lesions. Subsequent evaluation including positron emission tomography/computed tomography scans did not uncover any abnormalities other than the metastatic pulmonary melanoma. We also describe the characteristic bronchoscopic features of melanoma.
Malignant melanoma of unknown primary site (MUP) is defined as histologically-confirmed subcutaneous, nodal, or visceral metastatic melanoma occurring without any known cutaneous, mucosal, or ocular primary lesion1. A recent comprehensive systemic review of the existing literature2 showed that the incidence of MUP is estimated to be 3.2% although this figure varies considerably between different studies3,4. Amongst patients who are diagnosed with MUP, those with visceral metastasis are relatively infrequent compared to ones with subcutaneous or lymphnode metastasis2-5. Even individuals with endobronchial metastasis from unknown primary melanoma are extremely sparse6. Herein we report a case of MUP with endobronchial metastasis showing characteristic bronchoscopic features.
A 74-year-old man presented with one-month history of coughing and blood-tinged sputum. He was a former smoker who smoked half a pack of cigarettes per day between the ages of 20 and 69 years. He had also worked as a coal miner for past 14 years and had been diagnosed with coal worker's pneumoconiosis 5 years ago. He had no history of previous skin excisions or resected ocular tumors.
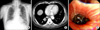
Physical examination revealed a fixed localized wheezing in the right lower lung zone. Routine laboratory studies and blood chemistries were normal. Chest x-rays showed numerous small nodules in the bilateral whole lungs (Figure 1A). These bilaterally-scattered nodules did not appear to have significantly changed compared to his past chest x-ray. However, a mass measuring 2.2×3.4 cm in the right lower lobe and several nodules of various size (range, 0.8~1.6 cm) in both lungs along with pneumoconiotic nodules were observed on computed tomography (CT) scans of the chest (Figure 1B). The patient then underwent a bronchoscopy. A black polypoid tumor obstructing the posterior basal segmental bronchus of the right lower lobe was found (Figure 1C).
Histologic examination of the bronchoscopic biopsy specimen showed that the lesion was composed of large round and spindle-shaped cells arranged in closely packed sheets (Figure 2). Large amounts of fine granular pigment were present within the tumor cells. Immunohistochemical staining showed that the tumor cells were positive for S-100 and HMB-45. Therefore, the patient was diagnosed with malignant melanoma.
F-18 fluorodeoxyglucose (FDG) positron emission tomography (PET)/CT scan was performed, which showed a metabolically active lesion in the right lower lobe (maximum standardized uptake value [SUVmax], 6.3; Figure 3). Additionally, several nodules seen in both lungs by CT were metabolically active (SUVmax, 7.0). However, cutaneous, mucosal, or ocular lesions suggesting primary melanoma were not detected.
Subsequent evaluation including brain magnetic resonance imaging, esophagogastroduodenoscopy, and colonoscopy did not uncover any additional abnormalities. Skin, ophthalmic, oral, and nasal examinations by specialists failed to identify any occult primary lesions. Interferon-α therapy was recommended, but the patient refused treatment. Follow-up CT scan of chest was performed 3 months after discharge when he presented with worsening dyspnea at emergency department. It showed increases in the size of previous endobronchial and several pulmonary lesions found metabolically active in PET/CT scan. Ultimately, he died of respiratory failure due to tumor progression 4 months after his initial diagnosis.
Most primary melanomas develop as cutaneous lesions, and a few develop in recognized mucosal or ocular sites. MUP is the term used to describe a relatively uncommon situation in which patients have metastatic melanoma, but no known primary cutaneous, mucosal or ocular lesions. This unusual condition was initially characterized by Dasgupta et al.1 who first described the criteria for MUP in 1963. Careful examination is essential when searching for primary tumors and includes the following: a complete exam of the skin and mucosal surfaces, ophthalmologic and otolaryngologic examinations, gastrointestinal endoscopic examination, and cerebral, neck, thoracic, and abdominal CT scan7. In the present study, PET/CT scans in addition to a thorough evaluation that included the procedures mentioned above were performed to identify a potential primary site. Although the use of PET/CT for evaluating the primary site of MUP is not well established8, this technique might be helpful for detecting a primary site in patients with MUP. This possibility is supported by the fact that the incidence of MUP has been reduced since the introduction of CT scan2.
To date, the etiology of MUP remains unclear although various hypotheses have been developed1,3. The first proposal is that MUP results from complete spontaneous regression of the primary melanoma3. Partial or complete spontaneous resolution of melanoma cells from the primary site is fairly common and it was actually described in various study2. A second assumption is that the melanoma originates from melanocytes in lymph nodes or viscera1,4. In fact, malignant melanoma detected in the lung may represent a primary lesion that has arisen in the lung. However, diagnosing primary pulmonary melanoma requires strict criteria which produce evidence that suggests a primary occurrence in the lung9-11. One of the criteria is that the pulmonary lesion should be solitary. Our patient with an endobronchial tumor and multiple pulmonary nodules did not fulfill it. Moreover, his pathologic features did not show junctional change with invasion of intact bronchial mucosa by malignant melanoma cells suggested as histopathological criteria for primary pulmonary melanoma9. Therefore, he was finally diagnosed with MUP when considering these currently proposed criteria for primary pulmonary melanoma. However, pathologic examination was performed in not a surgically removed specimen but the bronchoscopically obtained smaller one. It would limit accurate pathologic assessment for differentiating between primary and metastatic pulmonary melanoma. Therefore, the possibility that our patient might have a primary pulmonary melanoma with lung to lung metastasis cannot be completely excluded.
Endobronchial metastases of malignant melanoma detected bronchoscopically are also uncommon12,13. The tumor in the present case had a black polypoid appearance. This differed from previous cases that had yellowish or brown nodular lesions6,14,15. If a bronchoscopist encounters an endobronchial mass with the characteristics similar to the ones described in our study, malignant melanoma should be considered as an initial exclusive diagnosis.
Interestingly, the patient in the present case had worked as a coal miner. Consequently, he was diagnosed with coal worker's pneumoconiosis 5 years prior to this study. We could not find any existing literature on the relationship between malignant melanoma and coal worker's pneumoconiosis.
In general, the management of MUP patients is the same as that of stage-matched melanoma cases with a known primary site2. The role of adjuvant systemic chemotherapy remains unclear. As presented by the short survival time of our case, the prognosis for patients with visceral cases of MUP is generally poor2.
Figures and Tables
Figure 1
(A) Chest radiograph. Numerous small nodules were evenly scattered throughout both lungs with increased opacities toward the bilateral lower lobes. (B) Chest CT. Enhanced chest CT scan displayed a mass measuring 2×3 cm in the right lower lobe (white arrow) and another small nodule in the left lower lobe (gray arrow). (C) Bronchoscopic finding. A black polypoid tumor was found to be obstructing the posterior basal segmental bronchus of the right lower lobe. CT: computed tomography.
References
1. Dasgupta T, Bowden L, Berg JW. Malignant melanoma of unkonwn primary origin. Surg Gynecol Obstet. 1963. 117:341–345.
2. Kamposioras K, Pentheroudakis G, Pectasides D, Pavlidis N. Malignant melanoma of unknown primary site. To make the long story short. A systematic review of the literature. Crit Rev Oncol Hematol. 2011. 78:112–126.
3. Anbari KK, Schuchter LM, Bucky LP, Mick R, Synnestvedt M, Guerry D 4th, et al. University of Pennsylvania Pigmented Lesion Study Group. Melanoma of unknown primary site: presentation, treatment, and prognosis--a single institution study. Cancer. 1997. 79:1816–1821.
4. Savoia P, Fava P, Osella-Abate S, Nardò T, Comessatti A, Quaglino P, et al. Melanoma of unknown primary site: a 33-year experience at the Turin Melanoma Centre. Melanoma Res. 2010. 20:227–232.
5. Kelly J, Redmond HP. Melanoma of unknown origin: a case series. Ir J Med Sci. 2010. 179:629–632.
6. Min YH, Kim SW, Chin HJ, Lee TY, Song HH, Lee KS, et al. Case of unknown primary malignant melanoma with pulmonary and endobronchial metastasis. Tuberc Respir Dis. 2002. 53:196–201.
7. O'Neill JK, Khundar R, Knowles L, Scott-Young N, Orlando A. Melanoma with an unknown primary--a case series. J Plast Reconstr Aesthet Surg. 2010. 63:2071–2080.
8. Gutzeit A, Antoch G, Kühl H, Egelhof T, Fischer M, Hauth E, et al. Unknown primary tumors: detection with dual-modality PET/CT--initial experience. Radiology. 2005. 234:227–234.
9. Allen MS Jr, Drash EC. Primary melanoma of the lung. Cancer. 1968. 21:154–159.
10. de Wilt JH, Farmer SE, Scolyer RA, McCaughan BC, Thompson JF. Isolated melanoma in the lung where there is no known primary site: metastatic disease or primary lung tumour? Melanoma Res. 2005. 15:531–537.
11. Carstens PH, Kuhns JG, Ghazi C. Primary malignant melanomas of the lung and adrenal. Hum Pathol. 1984. 15:910–914.
12. Shepherd MP. Endobronchial metastatic disease. Thorax. 1982. 37:362–365.
13. Salud A, Porcel JM, Rovirosa A, Bellmunt J. Endobronchial metastatic disease: analysis of 32 cases. J Surg Oncol. 1996. 62:249–252.
14. Koyi H, Brandén E. Intratracheal metastasis from malignant melanoma. J Eur Acad Dermatol Venereol. 2000. 14:407–408.
15. Seam N, Khosla R. Metastatic endobronchial melanoma. Respiration. 2009. 77:214.




 PDF
PDF ePub
ePub Citation
Citation Print
Print




 XML Download
XML Download