Abstract
Background
The treatment success rates in patients with tuberculosis are known to be lower in the private sector compared to the public sector. To improve treatment outcomes in the private sector we developed a public-private collaboration model for strengthening health education and case holding activities with public health nursing in the private sector.
Methods
We performed a prospective cohort study in new smear positive pulmonary tuberculosis patients treated at private hospitals, selected by non-randomization, with an intervention consisting of health education and case holding activities by specially trained public health nurses (intervention group) results were compared with cases treated without the intervention (conventional group). Physicians were asked to treat both groups routinely. The treatment outcomes of patients under treatment by the National Tuberculosis Programme were also analyzed for comparison.
Results
There were 172 cases each in the intervention and conventional groups. The mean age was 48.9±19.0 and 48.2±19.7 in the respective groups (p=0.66). The PHN interacted with the cases in the intervention group by initial face to face interview and telephone calls an average of 7.1±9.2 times during the initial six months. The intervention group showed a significantly higher treatment success rate, 91.6%, (Rate Ratio [RR]; 1.23, 95% Confidence Interval [CI]; 1.12~1.36), lower default, 3.6%, (RR; 0.31, 95% CI; 0.13~0.75) and transfer-out rate, 3.0%, (RR; 0.32, 95% CI; 0.12~0.86) than the conventional group where they were: 75.0%, 11.6%, 9.3%, respectively. The success rate was even higher than the rate (80.5%) of 1,027 cases treated in health centers (RR; 1.11, 95% CI; 1.05~1.17). Of the completed cases in the intervention group, 82.2% regarded the role of the public health nurse as very helpful.
Tuberculosis (TB) treatment has been offered independently by both the public and private sector in Korea. Public health nurses (PHN) working in health centers (HC) have been in charge of health education and case-holding activities for registered cases. Since 1990, the cure rate of new smear positive pulmonary Tuberculosis (PTB) cases at HCs has been maintained at about 82% despite no directly observed treatment (DOT) and a relatively high transfer-out rate1. However, the private sector has had variable regimens with a 54% rate of success and a 29% default rate for new bacillary PTB cases according to a 1987 report2. Even though the success rate increased to 74% and the default rate decreased to 20% in 19933, treatment outcomes in the private sector have been disappointing.
With socioeconomic development and a medical insurance system covering all employees and self employed citizens in Korea, the proportion of patients in the private sector has been steadily increasing. The national TB prevalence survey (1995) showed that radiologically active TB cases treated at non-HC sites accounted for 45% of cases4. Recent notification data showed an increasing proportion of total TB patients in the private sector, 53% in 20015 and 59% in 20026 despite the low notification rate among the private sector. Therefore, to improve treatment outcomes, in the private sector, a public private collaboration model, with thorough case-holding, was developed.
The respiratory departments of eight private teaching hospitals participated in the study: five from Seoul and three from local cities. They were not chosen randomly, but rather, the selection was based on the hospitals that reported a relatively high number of cases from January 2001 to April 2001 through the Korean TB Surveillance System (KTBS). New smear positive PTB patients were enrolled into the intervention or conventional treatment groups.
All eligible cases diagnosed from August 2001 to April 2002 were assigned to the intervention group and notified by the Korean Institute of Tuberculosis (KIT) or HCs having jurisdiction over the hospital. The physician who diagnosed an eligible case referred the case to a nurse in the out-patient department or other appropriate health staff. The nurse then called the PHN. We did not evaluate the surveillance system for detecting eligible cases. For efficient case management, cases were given an appointment to see doctors for care. After notification, a PHN case worker interviewed the patient, explained the purpose of the study and verbal or written consent was given at the hospital, workplace or other study site. No patient declined PHN management. The PHN then conducted health education and case-holding activities during treatment. Basic knowledge regarding tuberculosis and the importance of routinely taking medication were initially explained to patients. Strategies for improving compliance within the intervention group were not based on DOT. Rather, self-administered treatment was encouraged. Appointment reminders using telephone calls and prompt phone calls for missed appointments, as well as open consultations were also provided in order to actively resolve any problems with treatment. These activities have been routinely provided to patients registered in the public sector.
A PHN was in charge of the management of cases enrolled in Seoul. In other cities, case management was conducted by a PHN working at a HC. Before the study, PHNs were trained in case management methods. The PHN encouraged cases not to move to the HCs. At the time of treatment completion a questionnaire survey was conducted to evaluate the role of PHN.
Due to the limited study period and eligible cases, we selected cases from the conventional (control) group and matched them with the same number of cases in the intervention group, from each hospital retrospectively from July 2001 on the basis of date of diagnosis. Age and gender were not matched. The PHN did not come in contact with the cases in the conventional group. Therefore, case management was not provided to the conventional group by the PHN. The data and treatment outcomes for the conventional group were collected by review of the medical records only.
Physicians were asked to treat both groups as usual. Dosage of anti-TB drugs was routinely provided to patients on a weekly or monthly basis by self-administration, except for the hospitalized patients. Sputum AFB smear examinations and culture for tubercle bacilli were carried out in the laboratory at each hospital.
Follow-up was conducted for both groups up until September 30, 2002. Treatment outcomes of the cases treated with the regimen containing Isoniazid (INH, H), Rifampicin (RFP, R), Pyrazinamide (PZA, Z) and others or not treated were classified on the basis of six months of treatment as following7: 1) cured as defined by a negative smear or culture after six months of treatment and on at least one previous occasion 2) completed was defined as completion of treatment for six months or more, without confirmation of cure or failure 3) failed was defined as persistent smear positive or positive again at five months or later during treatment 4) died was recorded for cases that died for any reason during the course of their treatment: 5) default was defined as any case that interrupted their treatment for more than two consecutive months duringthe initial six months 6) a transfer out was defined as a case who had continued treatment at another medical facility and its treatment result was unknown 7) success was defined as cases who were cured or completed the treatment. Treatment outcomes of cases were based on treatment regimens with INH, RFP and others, or not, was determined on the basis of nine months of treatment with similar criteria (except for PZA).
In order to compare treatment outcomes in the two groups and compare this with the public sector, a cohort analysis was conducted on new smear positive PTB cases registered in 2000. These cases were collected during the period from August 2001 to July 2002 from 30 randomly selected HCs during central supervisory visits by the KIT. Treatment regimens for the public sector have been standardized to a six-month short course regimen, self-administered on a monthly dosage basis without DOT. Subjects received health education, motivation and case holding activities by the TB health workers.
Statistical analyses were performed using the SAS System Software (Version 8.0, Cary, NC, USA). Rate ratio (RR) was calculated to compare treatment outcomes between the intervention and conventional groups, and cases registered in HCs. Differences were considered statistically significant on the basis of a p-value of 0.05 or less.
Both the intervention and conven-tional groups were composed of 172 cases. In the intervention group, there were 93 male and 79 female cases (ratio 1.2:1) with a mean age of 48.8±19.0 years (95% Confidence Interval [CI]; 46.0~51.9), ranging from 14 to 90 years (Table 1). The conventional group consisted of 106 male and 66 female cases (ratio 1.6:1) with a mean age of 48.2±19.7 years (95% CI; 45.3~51.1), ranging from 17 to 85 years. There was no significant difference in the sex ratio (p=0.1436) or age distribution (p=0.6614) between the two groups. There were 118 (68.6%) cases in each group that were selected from Seoul, and the others were selected from other cities. Due to insufficient medical recording in the conventional group, substantial information regarding the subjects' social history such as smoking habits, alcohol use, and educational status were not properly obtained. Five cases from the intervention group were excluded in the cohort analysis because those subjects had been treated for less than six-months by the end of the study.
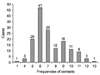
Cases in the intervention group participated in a face-to-face interview (s) with a PHN at the beginning of treatment and thereafter, if necessary; 145 cases had only one interview with a PHN; 24, two interviews; one, five interviews; and finally, one case had seven interviews with a PHN during treatment. Of all 172 cases, only one case failed to participate in a face-to-face interview. Among the 153 cases labeled as a 'success' in the intervention group, 49% had contact with a PHN six to seven times via a face-to-face interview or telephone discussions during the initial six-month treatment period (Figure 1). The mean frequency of total contact with a PHN during the initial six-month treatment period was 7.1±9.2.
A total of 135 cases completed the questionnaire survey at the end of the treatment, which evaluated of the role of PHN; 111 (82.2%) cases found the PHN 'very helpful'; 20 (14.8%) 'somewhat helpful'; three (2.2%) 'somewhat troublesome'; and one (0.7%) 'very troublesome'. Subjects who found the PHN to be troublesome were primarily concerned that frequent contacts with a PHN would reveal their diseases to acquaintances.
The regimen consisted of INH, RFP, Ethambutol (E, EMB) and PZA prescribed for 163 (94.8%) cases in the intervention group and 153 (89.0%) cases in the conventional group (Table 2). Four and seven in the respective groups were treated with individually tailored regimens because of adverse drug reactions or accompanying diseases. In the intervention group, the mean duration of treatment for cases that completed the protocol or were being treated with the EHRZ regimen was 7.7 (±2.0) months; 59 (36.2%) cases completed treatment during the six-month period. On the other hand, the mean duration of treatment for cases in the conventional group who completed treatment with the EHRZ regimen was 9.7 (±3.3) months; this was significantly different from the intervention group (p<0.0001); 27 (17.6%) cases completed treatment during the six-month period. The mean duration of treatment for each hospital was significantly different (p=0.0001), ranging from a period of 6.8 to 10.7 months.
Among the cases whose treatment was completed, sputum smear examinations were performed fewer than three times during the first six months of treatment in 92 (59.7%) cases in the intervention group and 83 (63.3%) cases in the conventional group. The mean frequency of monitoring sputum smear examinations, during the first six months of treatment, was 2.3 (±1.7) and 2.1 (±1.6) in the respective groups.
Among the 167 cases in the intervention group, whose treatment outcomes were analyzed, 58.7% were considered cured and 32.9% were defined as completed (Table 3). As for the conventional group, only 33.1% were considered cured, while 41.9% were defined as completed. The cure rates of the two groups showed a significant difference (Rate Ratio [RR]: 1.77, 95% Confidence Interval [CI]: 1.38~2.27). Furthermore, there was a significant difference in the success rates of the two groups (RR: 1.23, 95% CI: 1.12~1.36). For comparison with the public sector, treatment outcomes of 1,027 cases in 30 HCs were also analyzed. Although the cure rate in the intervention group was lower than that of HCs, the success rate of the former (91.6%) was significantly higher than the latter (80.5%); this was due to a higher proportion of completed cases (RR: 1.11, 95% CI: 1.05 0~1.17). The transfer-out rate in the former was also significantly lower than that of the latter.
Univariate analysis of the study cases revealed that three variables had a significant influence on treatment success: gender, study group and hospital location. A favorable response was significantly associated with female cases (RR: 1.17, 95% CI: 1.08~1.28), cases in the intervention group and treatment location in a hospital in Seoul (RR: 1.22, 95% CI: 1.07~1.38) (Table 4). However, for the multivariate analysis, the study group and hospital location were significantly associated with a favorable response.
Study cases were selected from eight teaching hospitals, to maximize the number of cases, increase efficiency of case holding activity with more patients per PHN during a limited study period. It is well known that compliance of patients, appropriate treatment regimen, initial drug resistance and adverse drug reactions are important factors influencing the success of TB treatment 8,9. This study focused on improving treatment efficiency in the private sector by strengthening case holding activities to improve compliance by using a PHN intervention.
Hong et al6 reported that 65.3% of the new cases treated at private clinics were prescribed an EHRZ regimen in 1993. In this study, 316 (91.9%) cases were treated with the EHRZ regimen, suggesting a more extensive use of this regimen than previously. However, the inclusion of private clinics alters the nature of the statistics because in our study the participating facilities that were teaching hospitals, with internship or residency programs, are more likely to use the most current available chemotherapy. In the intervention group, the mean duration of treatment with the EHRZ regimen was two months shorter than the conventional group. The limited study period, however, may have skewed these results. Case registration for the intervention group began in August 2001, but for the conventional group, cases prior to August 2001 were selected retrospectively. Consequently, while 47 cases in the intervention group were still undergoing treatment, only two cases in the conventional group had not completed treatment by the end of the study. Therefore, the mean treatment duration of 9.4 months for the conventional group is more likely to represent the current treatment period implemented at general hospitals. Leff et al. reported that in 1996, the treatment duration for patients treated with EHRZ regimen was approximately eight months10. Prolonged treatment of TB patients in the private sector frequently occurs in other countries also11-17.
Most patients generally favor large hospitals over small clinics or HCs, even with a national health insurance program that covers the burden of most fees treatment efficiency in the private sector is generally lower than in the public sector. This disparity results from a difference in case-holding activities. TB control workers in HCs ensure that cases receive thorough health education and case-holding activities which are supplemented by follow up programs, usually via telephone calls. Unlike the public sector, private physicians commonly omit or have difficulty in performing case- holding activities, including default tracing. In this study, by improving case-holding activities, default and transfer-out cases were reduced, resulting in more desirable treatment outcomes. Moreover, the success rate of the intervention group was increased much higher than that of the HCs. However, the cure rate of the intervention group was somewhat lower than that of the HCs this may have been due to the lack of sputum examination monitoring by private physicians. Hong et al. reported that only 24.4% of general practitioners perform periodic chest X-rays and sputum examinations during patient treatment18. Vyas et al. reported that 56.8% of private physicians believe that sputum examinations were essential for monitoring TB treatment19. Due to insufficient treatment monitoring via sputum examinations, 32.9% and 41.9% of the intervention and conventional group, respectively, were classified as completed rather than cured. As a result of the limitations of a non randomized study, performance of follow up sputum examination was higher in the study group than in the conventional group. This bias might have contributed to a higher completion rate in the conventional group. The cure rate may have also been higher if the study cases had been monitored regularly with sputum examinations. Therefore, it is clear that private physicians should follow more rigorously the current guidelines of treatment and monitoring of TB patients including sputum examinations.
The location of the healthcare seemed to be an important factor influencing treatment success in the study cases. The hospitals in Seoul had more favorable responses than those at community sites; this was likely due to the accessibility of the hospitals in Seoul. Hospitals in local communities treat patients residing in rural areas also. Differences in Socio- economic position, between individuals in Seoul and other cities may also have influenced the results.
In regard to the questionnaire survey conducted in 134 cases whose treatment was completed, 97% replied that the case-holding activities of the PHN was helpful for treatment completion and responding to medical problems during treatment. It can therefore be concluded that most TB patients in the private sector would like increased assistance during treatment. In order to avoid unnecessary conflicts between the public and private sector regarding patient treatment, PHN may become members of non-govenmental organizations. However, the greatest utility for the PHN may be the local communities where medical facilities for TB patients are more limited. They could provide case-holding activities such responsibilities would seem more appropriate for health workers providing services in the public sector.
Case selection using double blind methodology was not used in this study; this was due to the limited study period for selection of sufficient cases and determination of treatment outcomes. Therefore, we are unable to exclude the possibility that physicians participating in this study may have been more biased to one group. If so, the conventional group may have received more attention to increase their success rate by enhancing the quality of treatment, as opposed to the intervention group, by avoiding criticism of poor case management.
Favorable treatment outcomes and patient satisfaction with the role of the PHN support consideration of the implementation of a public-private collaboration model for enhancing treatment outcomes in the private sector. However, there are several barriers to public- private collaboration for TB care such as: interest in profit, treatment patterns not in accordance with standard regimens and low priority of public health functions in the private sector. To have a successful relationship between the public and private sectors, it is essential to show transparency, mutual respect and understanding, cooperative participation, and active involvement of the private sector at all levels20. In order to accomplish the above, it is necessary to strengthen the role of the government in regulatory affairs, sharing information, and the financing of public health interventions, all in partnership with the private sector21.
Figures and Tables
Figure 1
Frequency of contact with public health nurse in the intervention group: cases with successful outcome.
Acknowledgements
The authors are greatly thankful to Jin-Bum Lee and Soo-Yeon Oh at the section of the programme cooperation, Korean Institute of Tuberculosis for their invaluable contribution to the study.
Notes
References
1. Hong YP, Kim SJ, Lew WJ, Lee SH, Lee EK. Cohort analyses of the treatment of smear-positive pulmonary tuberculosis patients under programme conditions in Korea, 1983-1994. Int J Tuberc Lung Dis. 1998. 2:365–371.
2. Jin BW, Jang DJ. An analysis of tuberculosis patient management in private sector (in Korean). Tuberc Respir Dis. 1990. 37:399–406.
3. Hong YP, Kim SJ, Lee EG, Lew WJ, Bai JY. Treatment of bacillary pulmonary tuberculosis at the chest clinics in the private sector in Korea, 1993. Int J Tuberc Lung Dis. 1999. 3:695–702.
4. Ministry of Health and Welfare. Korean National Tuberculosis Association. Report on the 7th tuberculosis prevalence survey in Korea. 1996. Seoul: Korean National Tuberculosis Association.
5. Korean National Institute of Health. Korean Institute of Tuberculosis. Annual report on the notified tuberculosis patients in Korea: based on Korean Tuberculosis Surveillance System. 2002. Seoul: Korean Institute of Tuberculosis.
6. Korean National Institute of Health. Korean Institute of Tuberculosis. Annual report on the notified tuberculosis patients in Korea: based on Korean Tuberculosis Surveillance System. 2003. Seoul: Korean Institute of Tuberculosis.
7. World Health Organization. Treatment of tuberculosis: guidelines for national tuberculosis, WHO/CDS/TB 2003.313. 2003. Geneva: WHO.
8. Fox W. General considerations in the choice and management of regimens of chemotherapy for pulmonary tuberculosis. Bull Int Union Tuberc. 1972. 47:49–67.
9. Horne NW, Ross JD. Modern drug treatment of tuberculosis. 1990. 7th ed. London: The Chest, Heart and Stroke Association;43–45.
10. Leff DR, Leff AR. Tuberculosis control policies in major metropolitan health departments in the United States: VI. standard practice in 1996. Am J Respir Crit Care Med. 1997. 156:1487–1494.
11. Ormerod LP, Bentley C. The management of pulmonary tuberculosis notified in England and Wales in 1993. J R Coll Physicians Lond. 1997. 31:662–665.
12. Simpson AJ, Watt B, Heald SH, Sudlow MF, Leitch AG. The management of pulmonary tuberculosis in adults notified in Scotland in 1993. Respir Med. 1998. 92:1289–1294.
13. Rothe TB, Karrer W. Short-course therapy of pulmonary tuberculosis: doctor's compliance. Tuber Lung Dis. 1996. 77:93–97.
14. Sumartojo EM, Geiter LJ, Miller B, Hale BE. Can physicians treat tuberculosis?: report on a national survey of physician practices. Am J Public Health. 1997. 87:2008–2011.
15. Ollé-Goig JE, Cullity JE, Vargas R. A survey of prescribing patterns for tuberculosis treatment amongst doctors in a Bolivian city. Int J Tuberc Lung Dis. 1999. 3:74–78.
16. Singla N, Sharma PP, Singla R, Jain RC. Survey of knowledge, attitudes and practices for tuberculosis among general practitioners in Delhi, India. Int J Tuberc Lung Dis. 1998. 2:384–389.
17. Bloch AB, Cauthen GM, Simone PM, Kelly GD, Dansbury KG, Castro KG. Completion of tuberculosis therapy for patients reported in the United States in 1993. Int J Tuberc Lung Dis. 1999. 3:273–280.
18. Hong YP, Kwon DW, Kim SJ, Chang SC, Kang MK, Lee EP, et al. Survey of knowledge, attitudes and practices for tuberculosis among general practitioners. Tuber Lung Dis. 1995. 76:431–435.
19. Vyas RM, Small PM, DeRiemer K. The private-public divide: impact of conflicting perceptions between the private and public health care sectors in India. Int J Tuberc Lung Dis. 2003. 7:543–549.
20. Uplekar M, Pathania V, Raviglione M. Private practitioners and public health: weak links in tuberculosis control. Lancet. 2001. 358:912–916.
21. Weil DE. Advancing tuberculosis control within reforming health systems. Int J Tuberc Lung Dis. 2000. 4:597–605.




 PDF
PDF ePub
ePub Citation
Citation Print
Print






 XML Download
XML Download