Abstract
Purpose
Methods
Results
Figures and Tables
Fig. 1
Pathology of Takayasu arteritis. (A) Adventitia of artery showed markedly fibrotic and inflammatory cell infiltration at medioadventrial junction (H&E, ×10). (B) A few granulomas with giant cells are identified in medioadventitial junction (H&E, ×100).

Fig. 2
Aorto-uni-carotid bypass. Connecting aorta to left carotid artery using expanded polytetrafluoroethylene ringed graft.
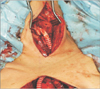
Fig. 3
Aorto-bi-carotid bypass. Connecting aorta to bilateral carotid artery using expanded polytetrafluoroethylene bifurcated graft.
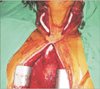
Fig. 4
CT angiography: preoperative (A, right; B, left) and postoperative (C) images of aorto-bi-carotid bypass. Female/24 years old, Bilateral common carotid artery occlusion case.
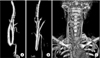
Fig. 5
Distribution of interval from diagnosis to operation. Dividing patients to 4 subgroups according to interval within 1 year, 2 years, 3 years, and over 3 years. Bold midline indicates median value, square indicates interquartile range.

Fig. 6
Cerebrovascular complications after surgery. Five intracranial haemorrhage cases including 2 expired cases, and 4 intracranial infarction cases including 1 expired case. Two cases suffered both intracranial haemorrhage and intracranial infarction.
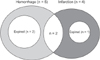
Fig. 7
Postoperative course according to postoperative blood pressure (BP). ICH, intracranial hemorrhage.

Table 4
The type of graft and critical complications

e-PTFE, expanded polytetrafluoroethylene; GSV, great saphenous vein.
a)One patient received aorto-bi-carotid bypass, b)One patient received aorto-bi-carotid bypass and suffered left graft occlusion turned to intracranial infarction, c)Same patient received aorto-uni-carotid bypass, d)Same patient received aorto-uni-carotid bypass, e)Same patient received aorto-uni-carotid bypass.
Table 5
Major complications after surgery

a)Same patient received aorto-bi-carotid bypass with e-PTFE. b)Same patient received aorto-uni-carotid bypass with e-PTFE. c)Same patient received aorto-bi-carotid bypass with e-PTFE suffered left graft occlusion turned to intracranial infarction. d)Same patient received aorto-uni-carotid bypass with e-PTFE. e)Same patient received aorto-uni-carotid bypass with GSV. f)Same patient received aorto-uni-carotid bypass with e-PTFE suffered left graft occlusion. g)Same patient received aorto-bi-carotid bypass with e-PTFE suffered right graft occlusion. e-PTFE, expanded polytetrafluoroethylene; GSV, great saphenous vein; CPR, cardiopulmonary resuscitation; ROSC, return of spontaneous circulation; ECG, electrocardiogram; F/U, follow-up; PCC, pericardiocentesis; SFA, superior femoral artery.




 PDF
PDF ePub
ePub Citation
Citation Print
Print





 XML Download
XML Download