Abstract
Purpose
To evaluate the usefulness of automated measurements of the localized retinal nerve fiber layer (RNFL) defects area in patients with glaucoma.
Methods
Fifty one patients with localized RNFL defects in RNFL red-free photographs and 53 healthy subjects were included. All participants were imaged with 3D spectral-domain optical coherence tomography (OCT). The area of defects was measured with the RNFL significance map (red = p < 1% and yellow = p < 5%) using Image J manually and Matlab software automatically. The area under the receiver operating characteristic curve (AUC) was calculated for the RNFL de-fect area of the RNFL photograph and RNFL maps, circumpapillary RNFL thickness, optic disc parameter, and macular in-ner retina thickness.
Results
High correlation was observed between manually and automatically measured defect areas in the significance map (red area r = 0.904, red and yellow area r = 0.890). The AUC for manually and automatically measured defects area (0.987, 0.966; p < 5%, p = 0.31, respectively) in the significance map was comparable. The latter demonstrated slightly higher but insignificant difference in AUC for inferior quadrant circumpapillary RNFL thickness (0.936; p = 0.22) and was significantly higher than the inferior ganglion cell layer plus inner plexiform layer thickness (0.894) and vertical cup to disc ratio (0.869) (p = 0.018, p = 0.008, respectively).
References
1. Schuman JS. Spectral domain optical coherence tomography for glaucoma (an AOS thesis). Trans Am Ophthalmol Soc. 2008; 106:426–58.
2. Kim NR, Lee ES, Seong GJ. . Spectral-domain optical coher-ence tomography for detection of localized retinal nerve fiber layer defects in patients with open-angle glaucoma. Arch Ophthalmol. 2010; 128:1121–8.

3. Leung CK, Lam S, Weinreb RN. . Retinal nerve fiber layer imaging with spectral-domain optical coherence tomography: analysis of the retinal nerve fiber layer map for glaucoma detection. Ophthalmology. 2010; 117:1684–91.
4. Leung CK, Choi N, Weinreb RN. . Retinal nerve fiber layer imaging with spectral-domain optical coherence tomography: pat-tern of RNFL defects in glaucoma. Ophthalmology. 2010; 117:2337–44.
5. Kang SY, Sung KR, Na JH. . Comparison between deviation map algorithm and peripapillary retinal nerve fiber layer measure-ments using Cirrus HD-OCT in the detection of localized glau-comatous visual field defects. J Glaucoma. 2012; 21:372–8.

6. Jeoung JW, Park KH, Kim TW. . Diagnostic ability of optical coherence tomography with a normative database to detect lo-calized retinal nerve fiber layer defects. Ophthalmology. 2005; 112:2157–63.

7. Yoo YC, Park KH. Comparison of optical coherence tomography and scanning laser polarimetry for detection of localized retinal nerve fiber layer defects. J Glaucoma. 2010; 19:229–36.

8. Yoo YC, Park KH. Influence of angular width and peripapillary position of localized retinal nerve fiber layer defects on their de-tection by time-domain optical coherence tomography. Jpn J Ophthalmol. 2011; 55:115–22.

9. Kang SM, Uhm KB. False negative findings of optical coherence tomography in eyes with localized nerve fiber layer defects. J Korean Ophthalmol Soc. 2011; 52:454–61.

10. Ye C, To E, Weinreb RN. . Comparison of retinal nerve fiber layer imaging by spectral domain optical coherence tomography and scanning laser ophthalmoscopy. Ophthalmology. 2011; 118:2196–202.

11. Mwanza JC, Oakley JD, Budenz DL, Anderson DR. Cirrus Optical Coherence Tomography Normative Database Study Group. Ability of cirrus HD-OCT optic nerve head parameters to discriminate nor-mal from glaucomatous eyes. Ophthalmology. 2011; 118:241–8. e1.
12. Schulze A, Lamparter J, Pfeiffer N. . Diagnostic ability of reti-nal ganglion cell complex, retinal nerve fiber layer, and optic nerve head measurements by Fourier-domain optical coherence tomography. Graefes Arch Clin Exp Ophthalmol. 2011; 249:1039–45.

13. Seong M, Sung KR, Choi EH. . Macular and peripapillary reti-nal nerve fiber layer measurements by spectral domain optical co-herence tomography in normal-tension glaucoma. Invest Ophthalmol Vis Sci. 2010; 51:1446–52.

14. Tan O, Li G, Lu AT. . Mapping of macular substructures with opti-cal coherence tomography for glaucoma diagnosis. Ophthalmology. 2008; 115:949–56.

15. Taliantzis S, Papaconstantinou D, Koutsandrea C. . Comparative studies of RNFL thickness measured by OCT with global index of visual fields in patients with ocular hypertension and early open angle glaucoma. Clin Ophthalmol. 2009; 3:373–9.

16. Cvenkel B, Kontestabile AS. Correlation between nerve fibre layer thickness measured with spectral domain OCT and visual field in patients with different stages of glaucoma. Graefes Arch Clin Exp Ophthalmol. 2011; 249:575–84.

17. Lopez-Peña MJ, Ferreras A, Larrosa JM. . Relationship be-tween standard automated perimetry and retinal nerve fiber layer parameters obtained with optical coherence tomography. J Glaucoma. 2011; 20:422–32.

18. Harwerth RS, Charles F. Prentice Award Lecture 2006: a neuron doctrine for glaucoma. Optom Vis Sci. 2008; 85:436–44.
19. Tan O, Chopra V, Lu AT. . Detection of macular ganglion cell loss in glaucoma by Fourier-domain optical coherence tomography. Ophthalmology. 2009; 116:2305–14. e1-2.

20. Mori S, Hangai M, Sakamoto A, Yoshimura N. Spectral-domain optical coherence tomography measurement of macular volume for diagnosing glaucoma. J Glaucoma. 2010; 19:528–34.

Figure 1.
(A) The cSLO RNFL photographs were overlaid with a color disc photograph (5 × 5 mm2) as a reference image that was obtained by Topcon 3D OCT-2000. (B) The retinal blood vessels (arrow) and RNFL defects (arrow head) were matched between the cSLO RNFL photograph and the reference image. cSLO = confocal scanning laser ophthalmoscope; RNFL = retinal nerve fi-ber layer; OCT = optical coherence tomography; T = temporal; N = nasal.

Figure 2.
(A) Original photograph in the retinal nerve fiber layer (RNFL) significance map, RNFL thickness map, optic disc photo-graph, and cSLO RNFL photograph. The RNFL significance map, RNFL thickness map, and optic disc photograph were obtained by Topcon 3D OCT-2000, and the RNFL photograph was captured by a Nidek F-10 cSLO. (B) Each boundary of the RNFL defects was manually delineated. The areas of the RNFL defects were measured on the 5 × 5 mm2 parapapillary area using Image J software (yellow lines) manually. Superpixels coded in red, red and yellow were automatically calculated by a Matlab computer program ac-cording to the red, green, and blue values in the 5 × 5 mm2 circumpapillary region. Measurement of the area of localized RNFL defect in the significance map (red area = 1.11 mm2, red and yellow area = 2.79 mm2), thickness map (1.40 mm2), cSLO RNFL photograph (1.77 mm2) manually, and automated measurement using significance map (red area = 0.84 mm2, red and yellow area = 3.59 mm2). cSLO = confocal scanning laser ophthalmoscope; RNFL = retinal nerve fiber layer; OCT = optical coherence tomography.

Figure 3.
(A) Scatter plots showing the relationship of manually measured red area (p < 1%) of significance map against automati-cally measured red area (p < 1%) of significance map (r = 0.904, p < 0.001). (B) Relationship of manually measured red and yel-low area (p < 5%) of significance map against automatically measured red and yellow area (p < 5%) of significance map (r = 0.890, p < 0.001).
Figure 4.
Bland-Altman plots of agreement between manually and automatically measured (A) red area (p < 1%) and (B) red and yellow area (p < 5%) in the significance map. Differences between automatically and manually measured areas were plotted against the means. Dash lines represent the 95% confidence intervals.
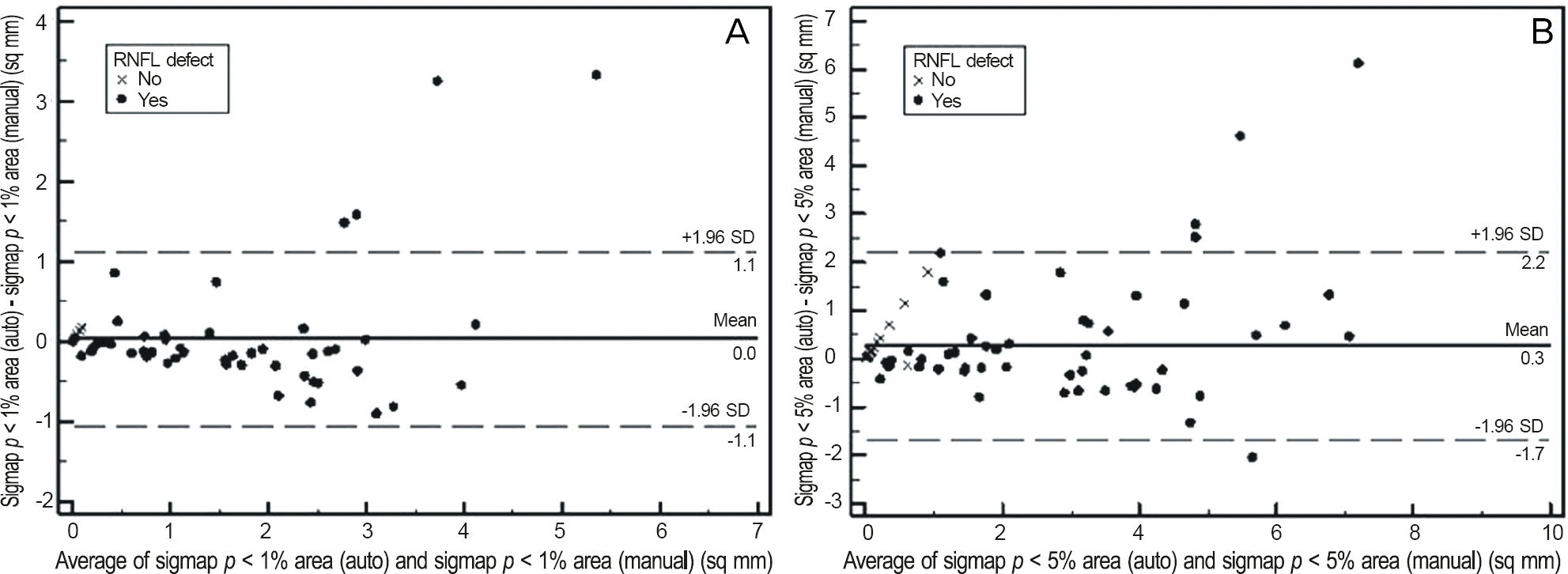
Figure 5.
The cut-off point (>0.546 mm2), sensitivity (90.2%), and specificity (94.3%) of automated measurements of sig-nificance map red and yellow area (p < 5%).
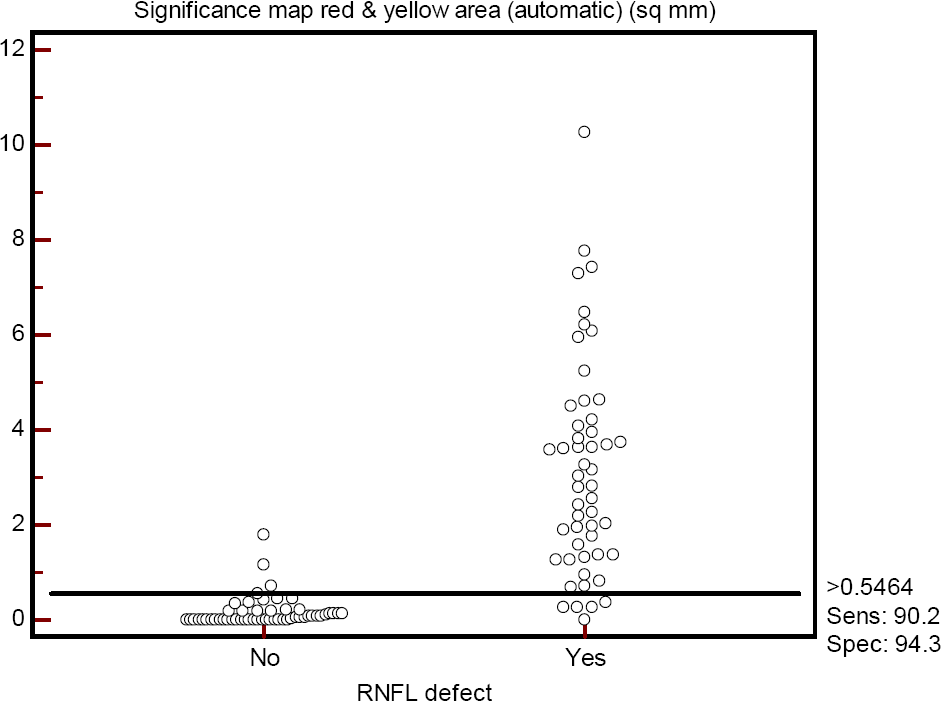
Figure 6.
Receiver operating characteristics curves of the man-ually measured significance map red and yellow area (p < 5%), automatically measured significance map red and yellow area (p < 5%), circumpapillary inferior quadrant retinal nerve fi-ber layer (RNFL) thickness, inferior ganglion cell layer + in-ner plexiform layer thickness (GCL + IPL thickness), and vertical cup to disc ratio (CDR).

Table 1.
Demographics and characteristics of subjects with localized RNFL defects and normal controls
| Normal eyes (n = 53) | Eyes with RNFL defects (n = 51) | p-value | |
|---|---|---|---|
| Age (years) | 56.3 ± 10.7 | 57.7 ± 13.7 | 0.54* |
| Gender (male:female) | 28:25 | 29:22 | 0.68† |
| Eye (right:left) | 24:29 | 21:30 | 0.67† |
| Spherical equivalent (diopters) | -0.15 ± 1.29 | -0.65 ± 2.05 | 0.15* |
| Central corneal thickness (μ m) | 543.78 ± 32.17 | 539.33 ± 31.98 | 0.50* |
| Mean deviation (dB) | -1.45 ± 0.91 | -6.15 ± 4.33 | <0.001* |
| Pattern standard deviation (dB) | 1.58 ± 0.69 | 6.08 ± 4.20 | <0.001* |
| Type of glaucoma | NA | ||
| Preperimetric | 7 | ||
| Perimetric | 44 | ||
| Localized RNFL defects | NA | 64 | |
| Superior | 11 | ||
| Inferior | 27 | ||
| Superior and inferior | 13 |
Table 2.
Area under the receiver operating characteristic curves (AUCs) of the red-free photograph, thickness map, and significance map between normal controls and eyes with RNFL defects
| Normal (n = 53) | Eyes with RNFL defects (n = 51) | p-value* | AUCs (95% CI) | Sn/Sp (Sp ≥ 80%) | Sn/Sp (Sp ≥ 90%) | |
|---|---|---|---|---|---|---|
| Defect area (mm2) | ||||||
| Photographic (manual) | 0 | 2.41 ± 1.46 | <0.001 | 1.000 (1.000-1.000) | NA | 100/100 |
| Thickness map (manual) | 0 | 2.04 ± 1.35 | <0.001 | 1.000 (1.000-1.000) | NA | 100/100 |
| Significance map red (manual) | 0 | 1.65 ± 1.17 | <0.001 | 0.961 (0.924-0.998) | NA | 92/100 |
| Significance map red & yellow (manual) | 0.01 ± 0.10 | 2.77 ± 1.83 | <0.001 | 0.987 (0.967-1.000) | NA | 98/98 |
| Significance map red (automatic) | 0.01 ± 0.04 | 1.70 ± 1.43 | <0.001 | 0.963 (0.925-1.000) | 94/85 | 94/92 |
| Significance map red & yellow (automatic) | 0.16 ± 0.32 | 3.15 ± 2.25 | <0.001 | 0.966 (0.932-1.000) | 98/83 | 90/94 |
Table 3.
Area under the receiver operating characteristic curves (AUCs) of circumpapillary RNFL thickness between normal con-trols and eyes with RNFL defects
| Normal (n = 53) | Eyes with RNFL defects (n = 51) | p-value* | AUCs (95% CI) | Sn/Sp (Sp ≥ 80%) | Sn/Sp (Sp ≥ 90%) | |
|---|---|---|---|---|---|---|
| Circumpapillary RNF | FL thickness (μ m) | |||||
| Average | 104.2 ± 8.1 | 83.3 ± 12.8 | <0.001 | 0.917 (0.864-0.970) | 78/81 | 76/92 |
| Quadrant | ||||||
| Temporal | 79.2 ± 10.6 | 69.3 ± 12.2 | <0.001 | 0.726 (0.628-0.823) | 55/81 | 35/91 |
| Superior | 122.7 ± 12.6 | 101.7 ± 18.3 | <0.001 | 0.863 (0.791-0.935) | 80/85 | 67/91 |
| Nasal | 84.7 ± 14.4 | 74.5 ± 15.8 | 0.001 | 0.710 (0.608-0.811) | 51/81 | 39/91 |
| Inferior | 129.2 ± 10.8 | 90.3 ± 22.2 | <0.001 | 0.936 (0.890-0.981) | 88/81 | 82/91 |
| Clock-hour | ||||||
| 9 (temporal) | 68.0 ± 10.9 | 64.3 ± 12.6 | 0.12 | 0.602 (0.492-0.713) | 35/81 | 24/91 |
| 10 | 91.2 ± 12.8 | 77.1 ± 19.4 | <0.001 | 0.719 (0.618-0.820) | 57/81 | 47/91 |
| 11 | 127.2 ± 17.5 | 99.6 ± 29.2 | <0.001 | 0.786 (0.695-0.877) | 65/81 | 61/91 |
| 12 (superior) | 122.6 ± 18.2 | 103.3 ± 22.9 | <0.001 | 0.771 (0.680-0.862) | 51/81 | 39/92 |
| 1 | 122.0 ± 15.2 | 102.3 ± 19.3 | <0.001 | 0.795 (0.709-0.881) | 65/81 | 49/91 |
| 2 | 99.1 ± 16.2 | 85.3 ± 20.5 | <0.001 | 0.718 (0.617-0.819) | 61/81 | 33/92 |
| 3 (nasal) | 74.4 ± 15.5 | 66.4 ± 15.3 | 0.009 | 0.667 (0.562-0.773) | 41/81 | 20/92 |
| 4 | 80.3 ± 18.2 | 71.6 ± 19.6 | 0.02 | 0.644 (0.537-0.751) | 41/81 | 20/91 |
| 5 | 114.1 ± 16.5 | 95.3 ± 20.5 | <0.001 | 0.767 (0.674-0.861) | 67/83 | 41/91 |
| 6 (inferior) | 134.4 ± 17.5 | 93.4 ± 25.7 | <0.001 | 0.896 (0.836-0.957) | 80/83 | 75/91 |
| 7 | 138.7 ± 17.5 | 82.0 ± 34.6 | <0.001 | 0.907 (0.845-0.970) | 84/85 | 82/94 |
| 8 | 78.3 ± 12.9 | 66.6 ± 16.2 | <0.001 | 0.736 (0.637-0.835) | 63/81 | 49/92 |
Table 4.
Area under the receiver operating characteristic curves (AUCs) of macular inner retina thickness and optic disc parameter between normal controls and eyes with RNFL defects
| Normal (n = 53) | Eyes with RNFL defects (n = 51) | p-value* | AUCs (95% CI) | Sn/Sp (Sp ≥ 80%) | Sn/Sp (Sp ≥ 90%) | |
|---|---|---|---|---|---|---|
| Macular inner retina thick | kness (μ m) | |||||
| NFL | ||||||
| Superior | 34.1 ± 4.9 | 29.6 ± 7.5 | <0.001 | 0.719 (0.616-0.822) | 59/81 | 39/92 |
| Inferior | 37.6 ± 4.2 | 24.3 ± 10.5 | <0.001 | 0.859 (0.778-0.941) | 75/83 | 73/92 |
| Total | 35.8 ± 4.0 | 26.9 ± 7.6 | <0.001 | 0.846 (0.762-0.930) | 78/83 | 73/94 |
| GCL + IPL | ||||||
| Superior | 72.1 ± 5.7 | 65.9 ± 5.5 | <0.001 | 0.789 (0.702-0.876) | 51/85 | 39/94 |
| Inferior | 70.5 ± 5.9 | 60.4 ± 6.2 | <0.001 | 0.894 (0.832-0.956) | 75/85 | 71/91 |
| Total | 71.3 ± 4.8 | 63.2 ± 5.0 | <0.001 | 0.879 (0.815-0.943) | 65/83 | 59/94 |
| GCC | ||||||
| Superior | 106.2 ± 7.8 | 95.5 ± 12.0 | <0.001 | 0.770 (0.678-0.863) | 61/83 | 39/91 |
| Inferior | 108.0 ± 8.3 | 84.6 ± 15.6 | <0.001 | 0.893 (0.829-0.958) | 82/81 | 73/91 |
| Total | 107.2 ± 7.8 | 90.1 ± 11.9 | <0.001 | 0.875 (0.806-0.943) | 82/81 | 67/92 |
| Optic nerve head | ||||||
| Cup area (mm2) | 1.06 ± 0.50 | 1.61 ± 0.68 | <0.001 | 0.732 (0.636-0.828) | 47/83 | 43/91 |
| Rim area (mm2) | 2.01 ± 0.47 | 1.24 ± 0.52 | <0.001 | 0.869 (0.796-0.941) | 84/85 | 65/91 |
| C/D area ratio | 0.34 ± 0.14 | 0.56 ± 0.17 | <0.001 | 0.827 (0.747-0.907) | 69/81 | 63/91 |
| Linear CDR | 0.57 ± 0.14 | 0.74 ± 0.13 | <0.001 | 0.824 (0.744-0.905) | 69/81 | 61/91 |
| Vertical CDR | 0.58 ± 0.13 | 0.79 ± 0.14 | <0.001 | 0.869 (0.798-0.940) | NA | 73/91 |
| Cup volume (mm3) | 0.24 ± 0.18 | 0.35 ± 0.25 | 0.01 | 0.628 (0.520-0.736) | 43/81 | 18/91 |
| Rim volume (mm3) | 0.17 ± 0.19 | 0.15 ± 0.17 | 0.56 | 0.562 (0.448-0.675) | 37/83 | 22/91 |
Table 5.
Comparison of significance map area analyzed by manual and automatic method
| Manual | Automatic | Difference | p-value* | r | p-value† | |
|---|---|---|---|---|---|---|
| Significance map red area (mm2) | 0.81 ± 1.16 | 0.84 ± 1.31 | -0.03 ± 0.56 | 0.54 | 0.904 | <0.001 |
| Significance map red and yellow area (mm2) | 1.38 ± 1.89 | 1.64 ± 2.19 | -0.26 ± 1.00 | 0.009 | 0.890 | <0.001 |
Table 6.
Relationships (correlation coefficients) between retinal nerve fiber layer defect areas and structural-functional p parameters
Table 7.
Probability values for the differences (upper triangle of numbers) between area under the receiver operating characteristic curves




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download