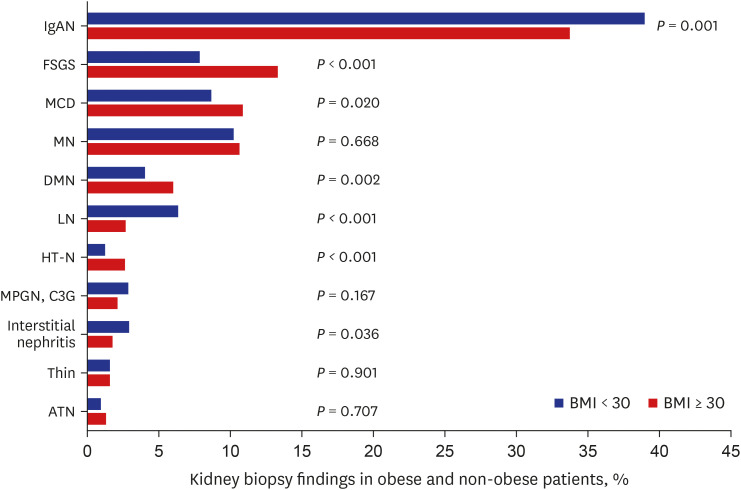
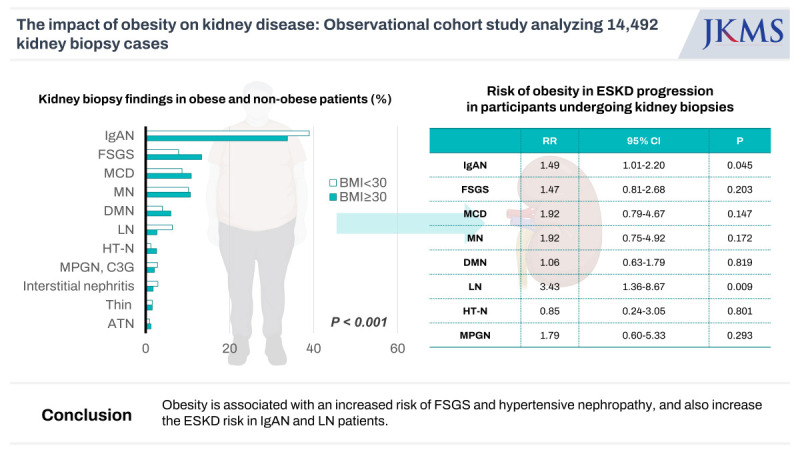
In this study, we have demonstrated the followings. First, the most common kidney biopsy finding in obese participants who underwent a kidney biopsy in Korea was IgAN (33.7%) although the prevalence of IgAN was significantly lower in obese participants than in non-obese participants. Second, although obesity independently increased the risk for FSGS and HT-N, it did not increase the risk of ESKD in these participants. However, obesity significantly increased the risk of ESKD in patients with IgAN and LN during the 93.1 months of follow-up. Third, 31 percent of the obese participants undergoing kidney biopsy had ORG. Among them, only 22.8% of the participants had ORG alone while 77.2% had combined other glomerular diseases. Higher serum albumin levels, lower IgA levels, and a history of DM were significantly related to ORG without other renal diseases. ORG participants without other renal diseases showed more favorable renal outcomes. The risks of ESKD and renal function decline were significantly increased in participants with ORG accompanied by another renal diseases.
The histology of ORG includes glomerulomegaly and FSGS.
6101417 A previous study identifying 128 ORG participants from 6,818 native kidney biopsies found that the mean glomerular diameter in participants with ORG was 1.3-fold larger than that of age and sex-matched normal controls.
14 The dominance of perihilar segmental sclerosis might manifest greater ultrafiltration pressure at the afferent vascular pole than at the efferent vascular pole.
6 ORG showed increases in the diameter of the afferent arteriole and decreases in podocyte density.
61417 These features are caused by increases in renal plasma flow, GFR, filtration fraction, and tubular sodium reabsorption.
3 Obesity is a major factor in metabolic syndrome and is associated with the incidence of HTN, DM, hyperuricemia, and dyslipidemia.
710 Among kidney biopsies, including 239 morbid obese participants (BMI ≥ 40 kg/m
2), 27.6% had DMN, and 19.2% had hypertensive nephrosclerosis.
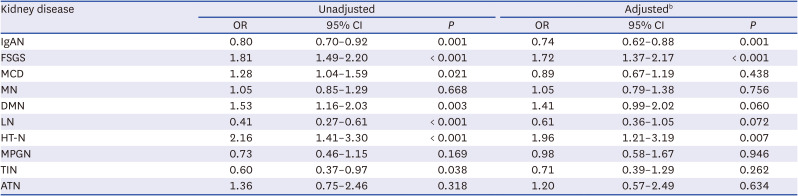
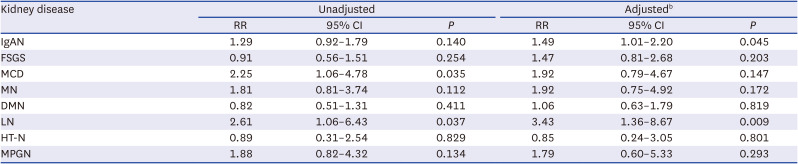
10 In our study, we found that obesity was independently associated with an increased prevalence of FSGS and HT-N. However, interestingly, it did not affect ESKD progression. In contrast, obesity was associated with significantly higher risk of ESKD in patients with IgAN and LN in our study indicating the differential effect of obesity according to different types of glomerular diseases. The mechanism of renal injury in immune-mediated GN in obese participants is not clear. Adipose tissue hypertrophy causes an increase in adipokines and inflammatory mediators, such as tumor necrosis factor-α (TNF-α), interleukin-6 (IL-6), leptin, adiponectin, and angiotensinogen, that could play crucial roles in kidney function and BP.
1819 TNF-α and IL-6 were also shown to play a major role in the pathogenesis of systemic lupus erythematosus (SLE).
2021 In addition to heightened inflammation, high blood pressure (BP) in obese participants might also contribute to renal injury, which can activate innate and adaptive immunity and immune cell infiltration in the kidneys.
19 Elevated BP is an independent risk factor for disease progression in patients with IgAN and LN.
222324 The previous observation showing that higher prevalence not only HTN and proteinuria, but also CKD, dialysis or death events in the overweight or obese IgAN compared to no obese participants also support the negative effect of obesity in IgAN.
24 In a study of 393 lupus patients, obesity was independently associated with the incidence of newly developed LN and cumulative organ damage.
25 Obesity was related to significant negative effects on function in patients with SLE.
26 Given this possible impact of obesity on progression of IgAN and LN, randomized studies testing the effect of weight reduction on outcome are warranted. The prevalence of ORG, defined as FSGS with glomerulomegaly or glomerulomegaly alone, has been reported as 29.4% in morbidly obese participants,
10 and this is comparable to the rate in our study (31.5%). However, the spectrum of kidney diseases accompanying ORG was completely different; most kidney diseases were HT-N (56.8%), DMN (25.0%), and acute tubular necrosis (18.2%) in the that study including predominantly white and black races in the United States.
10 In contrast, the most common kidney disease accompanying ORG was IgAN (40.9%), followed by DMN (15.2%) and MN (13.5%) in our study. These findings might reflect the regional/racial differences in glomerular disease frequencies.
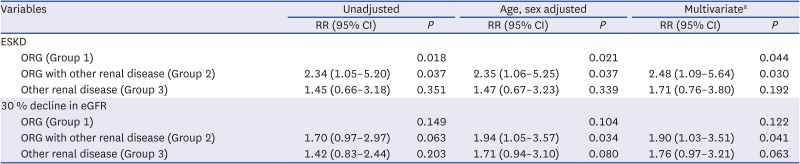
27 We also found that the renal outcomes in participants with ORG accompanied by other renal diseases were significantly worse than those of participants with ORG or other renal diseases alone. This finding suggest that the kidney biopsy is important in predicting outcomes in obese participants. We also found that baseline eGFRs in DMN, IgAN, and LN patients were significantly lower in Group 2 than in Group 3, suggesting that superimposed ORG in these diseases is an important factor in kidney disease progression. Favorable outcomes were seen in participants with ORG alone. Higher serum albumin levels, lower IgA levels, and a history of DM might be considered predictive factors for ORG alone to guide treatment and prognosis in clinical practice.
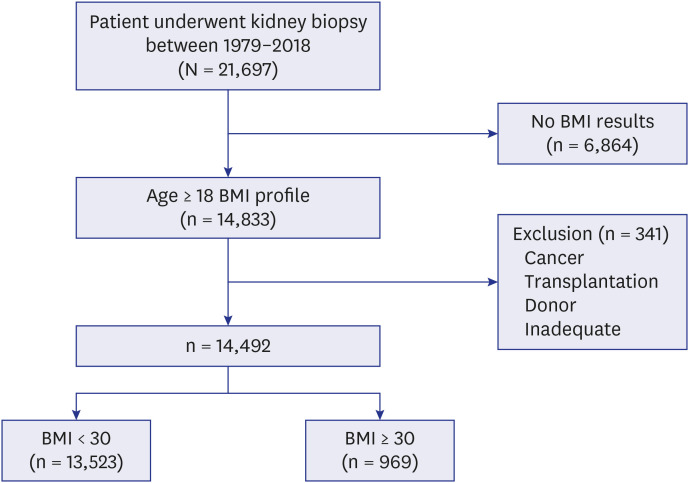
Despite several novel findings including long-term outcomes, our study had some limitations. First, this study had a retrospective nature, and treatment data were limited. Second, there were no patient BMI results for 31.6% of the total kidney biopsies, so bias could exist in patient selection. Third, among the pathologic data, glomerulomegaly was assessed in routine clinical practice by trained renal pathologists in the tertiary hospital. However, the strength of our study was the large-scale study based on pathologic data. We gathered total 21,697 kidney biopsies from 18 tertiary hospitals in Korea and compared characteristics and long-term outcomes of obese (n = 969) and nonobese (n = 13,522) participants. We analyzed the effect of obesity on risk and prognosis of various glomerular diseases. We also found that many different types of glomerular diseases can be combined with ORG in these participants and these participants might have worse renal outcome. In addition, types of glomerular diseases frequently combined with ORG in obese participants are different according to a different regions and ethnicity. Given that there have been only few reports on pathologic data in severely obese participants in Asia, our study shows the heterogeneity of kidney pathology and outcomes in obese participants and indicates the importance of a kidney biopsy in both deciding the management and predicting outcomes.




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download