Abstract
Depression is a highly prevalent mental health disease that, fortunately, can easily be treated. However, depression is often inadequately managed because only some depressive patients seek professional help, and even when they do, they often discontinue their treatments. Research has shown that there is a high association between suicide and depression. Proper depression management plans help depressive patients adhere to treatment medication and support them in continuing treatment. These efforts for treating depression may reduce suicidal ideation and behavior. Simply giving screening results to clinicians was not enough to have treatment outcomes. Besides informing clinicians of patients' screening results, staff-assisted care, including educating patients, following-up on assessments and treatment schedules, helping patients adhere to prescribed antidepressant medications, and referring to mental health care professionals would be critical to achieving successful treatment outcomes. A higher level of staff-assisted care has been reported to have higher treatment outcomes. Future studies in Korea are needed to establish a depression screening system, including post-screening management programs in primary care or community care settings, and to assess the effectiveness of this system. Attaining a higher depression diagnosis rate through screening and running post-screening management programs with sufficient staffing for treatment adherence will reduce depression relapse and suicidal attempts.
Figures and Tables
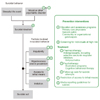
Figure 1
Targets of suicide prevention interventions (From Mann JJ et al. JAMA 2005;294:2064-2074, with permission from American Medical Association) [57].
References
1. Lang RS. Lang RS, Hensrud DD, editors. Depression and suicide: recognition and early intervention. Clinical preventive medicine. 2004. Chicago: American Medical Association.
2. Mathers CD, Bernard C, Iberg KM, Inoue M, Fat DM, Shibuya K, Stein C, Tomijima N, Xu H. Global burden of disease in 2002: data sources, methods and results. 2003. Geneva: World Health Organization.
3. Unutzer J, Patrick DL, Diehr P, Simon G, Grembowski D, Katon W. Quality adjusted life years in older adults with depressive symptoms and chronic medical disorders. Int Psychogeriatr. 2000. 12:15–33.

4. Cho MJ. A prevalence and correlates of major mental disorders among Korean adults: 2006 national epidemiologic survey. 2008. Seoul: Ministry of Health & Welfare.
5. Canadian Task Force on the Periodic Health Examination. The Canadian guide to clinical preventive health care. 1994. Ottawa: Health Canada.
6. Kessler RC, Chiu WT, Demler O, Merikangas KR, Walters EE. Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005. 62:617–627.

7. Hasin DS, Goodwin RD, Stinson FS, Grant BF. Epidemiology of major depressive disorder: results from the National Epidemiologic Survey on Alcoholism and Related Conditions. Arch Gen Psychiatry. 2005. 62:1097–1106.
8. Narrow WE, Rae DS, Robins LN, Regier DA. Revised prevalence estimates of mental disorders in the United States: using a clinical significance criterion to reconcile 2 surveys' estimates. Arch Gen Psychiatry. 2002. 59:115–123.

9. Beekman AT, Copeland JR, Prince MJ. Review of community prevalence of depression in later life. Br J Psychiatry. 1999. 174:307–311.

11. Johnstone A, Goldberg D. Psychiatric screening in general practice. A controlled trial. Lancet. 1976. 1:605–608.
12. Moore JT, Silimperi DR, Bobula JA. Recognition of depression by family medicine residents: the impact of screening. J Fam Pract. 1978. 7:509–513.
13. Linn LS, Yager J. The effect of screening, sensitization, and feedback on notation of depression. J Med Educ. 1980. 55:942–949.

14. Zung WW, Magill M, Moore JT, George DT. Recognition and treatment of depression in a family medicine practice. J Clin Psychiatry. 1983. 44:3–6.
15. Zung WW, King RE. Identification and treatment of masked depression in a general medical practice. J Clin Psychiatry. 1983. 44:365–368.
16. Hoeper EW, Nycz GR, Kessler LG, Burke JD Jr, Pierce WE. The usefulness of screening for mental illness. Lancet. 1984. 1:33–35.

17. Rucker L, Frye EB, Cygan RW. Feasibility and usefulness of depression screening in medical outpatients. Arch Intern Med. 1986. 146:729–731.

18. Shapiro S, German PS, Skinner EA, VonKorff M, Turner RW, Klein LE, Teitelbaum ML, Kramer M, Burke JD Jr, Burns BJ. An experiment to change detection and management of mental morbidity in primary care. Med Care. 1987. 25:327–339.

19. Rand EH, Badger LW, Coggins DR. Toward a resolution of contradictions. Utility of feedback from the GHQ. Gen Hosp Psychiatry. 1988. 10:189–196.

20. Magruder-Habib K, Zung WW, Feussner JR. Improving physicians' recognition and treatment of depression in general medical care. Results from a randomized clinical trial. Med Care. 1990. 28:239–250.

21. Brody DS, Lerman CE, Wolfson HG, Caputo GC. Improvement in physicians' counseling of patients with mental health problems. Arch Intern Med. 1990. 150:993–998.

22. Bergus GR, Hartz AJ, Noyes R Jr, Ward MM, James PA, Vaughn T, Kelley PL, Sinift SD, Bentler S, Tilman E. The limited effect of screening for depressive symptoms with the PHQ-9 in rural family practices. J Rural Health. 2005. 21:303–309.

23. Wells KB, Sherbourne C, Schoenbaum M, Duan N, Meredith L, Unutzer J, Miranda J, Carney MF, Rubenstein LV. Impact of disseminating quality improvement programs for depression in managed primary care: a randomized controlled trial. JAMA. 2000. 283:212–220.

24. Jarjoura D, Polen A, Baum E, Kropp D, Hetrick S, Rutecki G. Effectiveness of screening and treatment for depression in ambulatory indigent patients. J Gen Intern Med. 2004. 19:78–84.

25. Rost K, Nutting P, Smith J, Werner J, Duan N. Improving depression outcomes in community primary care practice: a randomized trial of the quEST intervention. Quality Enhancement by Strategic Teaming. J Gen Intern Med. 2001. 16:143–149.

26. U.S. Department of Health and Human Services. Mental health and mental health disorder. 2000. 2nd ed. Washington, D.C.: U.S. Government Printing Office.
27. Robinson WD, Geske JA, Prest LA, Barnacle R. Depression treatment in primary care. J Am Board Fam Pract. 2005. 18:79–86.

28. Callahan CM, Hendrie HC, Dittus RS, Brater DC, Hui SL, Tierney WM. Improving treatment of late life depression in primary care: a randomized clinical trial. J Am Geriatr Soc. 1994. 42:839–846.

29. Bosmans J, de Bruijne M, van Hout H, van Marwijk H, Beekman A, Bouter L, Stalman W, van Tulder M. Cost-effectiveness of a disease management program for major depression in elderly primary care patients. J Gen Intern Med. 2006. 21:1020–1026.

30. Whooley MA, Avins AL, Miranda J, Browner WS. Case-finding instruments for depression. Two questions are as good as many. J Gen Intern Med. 1997. 12:439–445.
31. Rubenstein LZ, Alessi CA, Josephson KR, Trinidad Hoyl M, Harker JO, Pietruszka FM. A randomized trial of a screening, case finding, and referral system for older veterans in primary care. J Am Geriatr Soc. 2007. 55:166–174.

32. Spitzer RL, Kroenke K, Williams JB. Validation and utility of a self-report version of PRIME-MD: the PHQ primary care study. Primary Care Evaluation of Mental Disorders. Patient Health Questionnaire. JAMA. 1999. 282:1737–1744.

33. Kroenke K, Spitzer RL, Williams JB. The Patient Health Questionnaire-2: validity of a two-item depression screener. Med Care. 2003. 41:1284–1292.
34. Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961. 4:561–571.

35. Sartorius N, Ban T, editors. Assessment of depression. 1986. New York: Springer-Verlag.
36. Radloff LS. The CES-D scale: a self-report depression scale for research in the general population. Appl Psychol Meas. 1977. 1:385–401.
37. Yesavage JA, Brink TL, Rose TL, Lum O, Huang V, Adey M, Leirer VO. Development and validation of a geriatric depression screening scale: a preliminary report. J Psychiatr Res. 1982. 17:37–49.

38. U.S. Preventive Services Task Force. Screening for depression: recommendations and rationale. Ann Intern Med. 2002. 136:760–764.
39. National Institute for Health and Clinical Excellence. National Collaborating Centre for Mental Health. Depression: manage-ment of depression in primary and secondary care. 2009. London: National Institute for Health and Clinical Excellence.
40. Hahn HM, Yum TH, Shin YW, Kim KH, Yoon DJ, Chung KJ. A standardization study of beck depression inventory in Korea. J Korean Neuropsychiatr Assoc. 1986. 25:487–502.
41. Cho MJ, Bae JB, Suh GH, Hahn BJ, Kim HK, Lee DW, Kang MH. Validation of geriatric depression scale, Korean version (GDS) in the assessment of DSM-III-R major depression. J Korean Neuropsychiatr Assoc. 1999. 38:48–63.
42. Cho MJ, Kim KH. Diagnostic validity of the CES-D (Korean version) in the assessment of DSM-III-R major depression. J Korean Neuropsychiatr Assoc. 1993. 32:381–399.
43. Lim KH, Park YN, Kim DH, Shin IH, Lee WS, Kim JB. A preliminary study of the standardization of the Korean version of the patient health questionnaire-9. Korean J Health Promot Dis Prev. 2009. 9:275–280.
44. Shin HC, Kim CH, Park YW, Cho BL, Song SW, Yun YH, Ou SW. Validation of zung's self-rating depression scale: detection of depression in primary care. J Korean Acad Fam Med. 2000. 21:1317–1329.
45. Choi HS, Choi JH, Park KH, Joo KJ, Ga H, Ko HJ, Kim SR. Standardization of Korean version of patient health questionnaire-9 as a screening instrument for major depressive disorder. J Korean Acad Fam Med. 2007. 28:114–119.
46. Myung SK, Jeong B, Lee WJ, Koh HJ, Suh SY, Yoo T, Sik HH. Standardization of the two-question case finding instrument as a screening instrument for the adolescent's depression. J Korean Acad Fam Med. 2000. 21:100–106.
47. U.S. Preventive Services Task Force. Screening for depression in adults: U.S. preventive services task force recommendation statement. Ann Intern Med. 2009. 151:784–792.
48. Barraclough B, Bunch J, Nelson B, Sainsbury P. A hundred cases of suicide: clinical aspects. Br J Psychiatry. 1974. 125:355–373.

49. Dorpat TL, Ripley HS. A study of suicide in the Seattle area. Compr Psychiatry. 1960. 1:349–359.

50. Rich CL, Fowler RC, Fogarty LA, Young D. San Diego Suicide Study. III. Relationships between diagnoses and stressors. Arch Gen Psychiatry. 1988. 45:589–592.
51. Robins E, Murphy GE, Wilkinson RH Jr, Gassner S, Kayes J. Some clinical considerations in the prevention of suicide based on a study of 134 successful suicides. Am J Public Health Nations Health. 1959. 49:888–899.

52. Shaffer D, Gould MS, Fisher P, Trautman P, Moreau D, Kleinman M, Flory M. Psychiatric diagnosis in child and adolescent suicide. Arch Gen Psychiatry. 1996. 53:339–348.

53. Drake RE, Bartels SJ, Torrey WC. Williams R, Dalby JT, editors. Suicide in schizophrenia: clinical approaches. Depression in schizophrenics. 1989. New York: Plenum Press;171–186.

54. Brent DA, Johnson BA, Perper J, Connolly J, Bridge J, Bartle S, Rather C. Personality disorder, personality traits, impulsive violence, and completed suicide in adolescents. J Am Acad Child Adolesc Psychiatry. 1994. 33:1080–1086.

55. Luoma JB, Martin CE, Pearson JL. Contact with mental health and primary care providers before suicide: a review of the evidence. Am J Psychiatry. 2002. 159:909–916.

56. Andersen UA, Andersen M, Rosholm JU, Gram LF. Contacts to the health care system prior to suicide: a comprehensive analysis using registers for general and psychiatric hospital admissions, contacts to general practitioners and practising specialists and drug prescriptions. Acta Psychiatr Scand. 2000. 102:126–134.

57. Mann JJ, Apter A, Bertolote J, Beautrais A, Currier D, Haas A, Hegerl U, Lonnqvist J, Malone K, Marusic A, Mehlum L, Patton G, Phillips M, Rutz W, Rihmer Z, Schmidtke A, Shaffer D, Silverman M, Takahashi Y, Varnik A, Wasserman D, Yip P, Hendin H. Suicide prevention strategies: a systematic review. JAMA. 2005. 294:2064–2074.
58. Robins E. The final months: a study of the lives of 134 persons who committed suicide. 1981. New York: Oxford University Press.
59. Bottlender R, Jager M, Strauss A, Moller HJ. Suicidality in bipolar compared to unipolar depressed inpatients. Eur Arch Psychiatry Clin Neurosci. 2000. 250:257–261.

60. Schou M, Weeke A. Did manic-depressive patients who committed suicide receive prophylactic or continuation treatment at the time. Br J Psychiatry. 1988. 153:324–327.

61. Martin RL, Cloninger CR, Guze SB, Clayton PJ. Mortality in a follow-up of 500 psychiatric outpatients. II. Cause-specific mortality. Arch Gen Psychiatry. 1985. 42:58–66.

62. Lee CH, Chon KK, Hahn DW, Kim KH. The Korean adaptation if the State-Trait Depression Inventory: STDI-K. Korean J Health Psychol. 1999. 4:1–14.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download