INTRODUCTION
With more than 30 therapeutic antibodies approved worldwide, therapeutic antibodies have become a major category in the pharmaceutical market. In an effort to further expand the potential of therapeutic antibodies, several approaches are being employed, such as improving the effector functions of the antibodies, designing antibody-drug conjugates, and downsizing the antibody molecule. Among these approaches, enhancing antibody-dependent cellular cytotoxicity (ADCC), which is the major effector function of an antibody, is thought to be one of the most promising and practical approaches to make an antibody more efficacious. In this "Perspective", we have provided an overview of such ADCC-enhancing technologies, while focusing mainly on our Potelligent® Technology, which has been most extensively tested in clinical trials.
ADCC AS A MAJOR MODE OF ACTION OF ANTIBODY THERAPY
ADCC is a cytolytic effector mechanism by which an antigen-specific antibody stimulates immune effector cells, primarily NK (natural killer) cells, to kill antigen-expressing cells. This process is triggered by the binding of the Fc domain of an antibody to the FcγRs (FcγRIIIa in human) on NK cells, followed by the activation of NK cells, and then, the destruction of target cells. A number of preclinical studies have shown that ADCC is a major mechanism of action of antitumor antibodies such as rituximab, trastuzumab, and alemtuzumab. Furthermore, the importance of ADCC has also been shown by clinical trials, which have provided evidence of a significant correlation between FcγRIIIa functional polymorphisms and clinical outcomes, demonstrated by multiple therapeutic antibodies, including rituximab, trastuzumab, cetuximab, and infliximab. Thus, ADCC is now considered an important clinical mechanism, and enhancing ADCC has become a logical approach to improve the efficacy of therapeutic antibodies.
ADCC-ENHANCING TECHNOLOGIES
ADCC can be enhanced in several different ways, one of which is the modification of amino acids in the Fc domain. Shields et al. have shown that the Fc-domain variants with up to 3 mutations improved binding of the Fc domain with FcγRIIIa and enhanced the capacity for ADCC [1]. More recently, Lazar et al. have utilized computational 3D modeling methods to design an IgG1-Fc variant with 3 mutations that showed markedly enhanced FcγRIII binding, ADCC, and, importantly, B-cell depletion in monkeys by using an anti-CD20 system [2].
The other established approach for enhancing ADCC is the modification of the oligosaccharide structure in the Fc domain. The Fc region of an IgG molecule has 2 N-linked glycosylation sites located at N297 (asparagine 297) of the 2 heavy chains. The N297-linked oligosaccharide chains are of the complex biantennary type, which has structural heterogeneity in certain moieties, and this heterogeneity affects the antibody's effector functions. While it was know that the presence of the terminal sialic acid might affect FcγRIIIa binding and ADCC, Umaña et al. have shown that increased amount of bisecting GlcNAc (N-acetyl-D-glucosamine) adjacent to the core mannose resulted in a 10-fold ADCC enhancement [3]. Meanwhile, our group, as well as several others, has been focusing on the fucose residue for its possible effect on ADCC; these studies eventually led to the establishment of the Potelligent® Technology.
POTELLIGENT® TECHNOLOGY
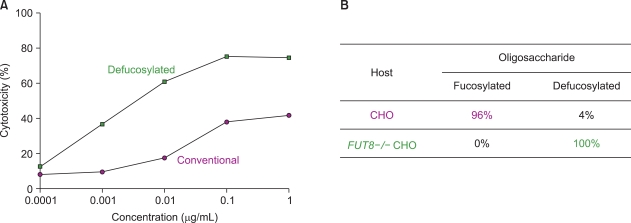
Potelligent® Technology, one of the most potent technologies for enhancing ADCC, originated from the initial discovery that reducing or eliminating fucose from the oligosaccharides on the Fc domain significantly increased FcγRIIIa binding and dramatically enhanced ADCC by -100 fold; the impact of this modification was, by far, greater than that of any other glycomodifications (Fig. 1A) [4]. Intensive studies have shown that a defucosylated antibody has a number of desirable features for clinical applications: it can induce potent ADCC at a lower dose and antigen density than a conventional antibody can [5], and it induces more potent in vivo anti-tumor activity than its conventional counterpart in animal models [5]. Additionally, in contrast to the antibodies obtained by introducing amino acid mutations, an antibody with no fucose is a natural component of human serum, and therefore, has a lower risk of immunogenicity.
For clinical application of this technology, it was critical to establish a robust production system, because all the commonly used host cells for biologics manufacturing produce highly fucosylated proteins. To this end, we generated a genetically engineered Chinese hamster ovary (CHO) host cell line that is incapable of adding fucose to an oligosaccharide chain; this was achieved by knocking out the FUT8 gene, which encodes the only enzyme that catalyzes the core fucosylation in mammals [6]. The established FUT8-/- CHO cells were confirmed to produce fully defucosylated antibodies (Fig. 1B), with their other basic characteristics being undistinguishable from a wild-type CHO cell, thereby making the knockout cell an ideal host for ADCC-enhanced antibodies.
CLINICAL APPLICATION OF THE POTELLIGENT® TECHNOLOGY
To date, as many as 10 Potelligent®-applied antibodies produced by using the FUT8-/- CHO cells have been investigated in human clinical trials, and a growing body of evidence has now confirmed the clinical benefits of this technology. Among those antibodies, the anti-CCR4 antibody, KW-0761 (mogamulizumab), is the most advanced. In a phase I/II study in patients with relapsed/refractory cutaneous T-cell lymphoma, KW-0761 produced an overall response rate of 39% with a manageable safety profile [7]. In a separate pivotal phase II study in patients with relapsed adult T-cell leukemia-lymphoma, a remarkable overall response rate of 50% was observed [8]; a new drug application for this antibody was filed with the Japanese regulatory agency in April 2011.
CONCLUSION
With therapeutic antibodies becoming a major pharmaceutical entity, an effort to create next-generation antibodies is in full swing. The Potelligent® defucosylation technology is among the approaches for creating such engineered antibodies, and it has proven clinically effective. More clinical data from multiple antibodies are needed to fully evaluate the clinical benefits of this technology.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download