References
1. Ho LM, Paulson EK, Thompson WM. Pneumatosis intestinalis in the adult: benign to life-threatening causes. AJR Am J Roentgenol. 2007; 188:1604–1613.

2. Galandiuk S, Fazio VW. Pneumatosis cystoides intestinalis. A review of the literature. Dis Colon Rectum. 1986; 29:358–363.
3. Kim JS, Kwon SB, Kim W, et al. A case of primary pneumatosis cystoides intestinalis in a patient with chronic abdominal pain. Intest Res. 2011; 9:40–45.

4. Heng Y, Schuffler MD, Haggitt RC, Rohrmann CA. Pneumatosis intestinalis: a review. Am J Gastroenterol. 1995; 90:1747–1758.
Fig. 1.
Index colonoscopic findings. (A, B) Multiple submucosal tumors are observed between 20 cm and 40 cm from the anal verge. Some lesions show hyperemia. (C, F) Endoscopic mucosal resection is being performed on the largest lesion with easy-touch bleeding.
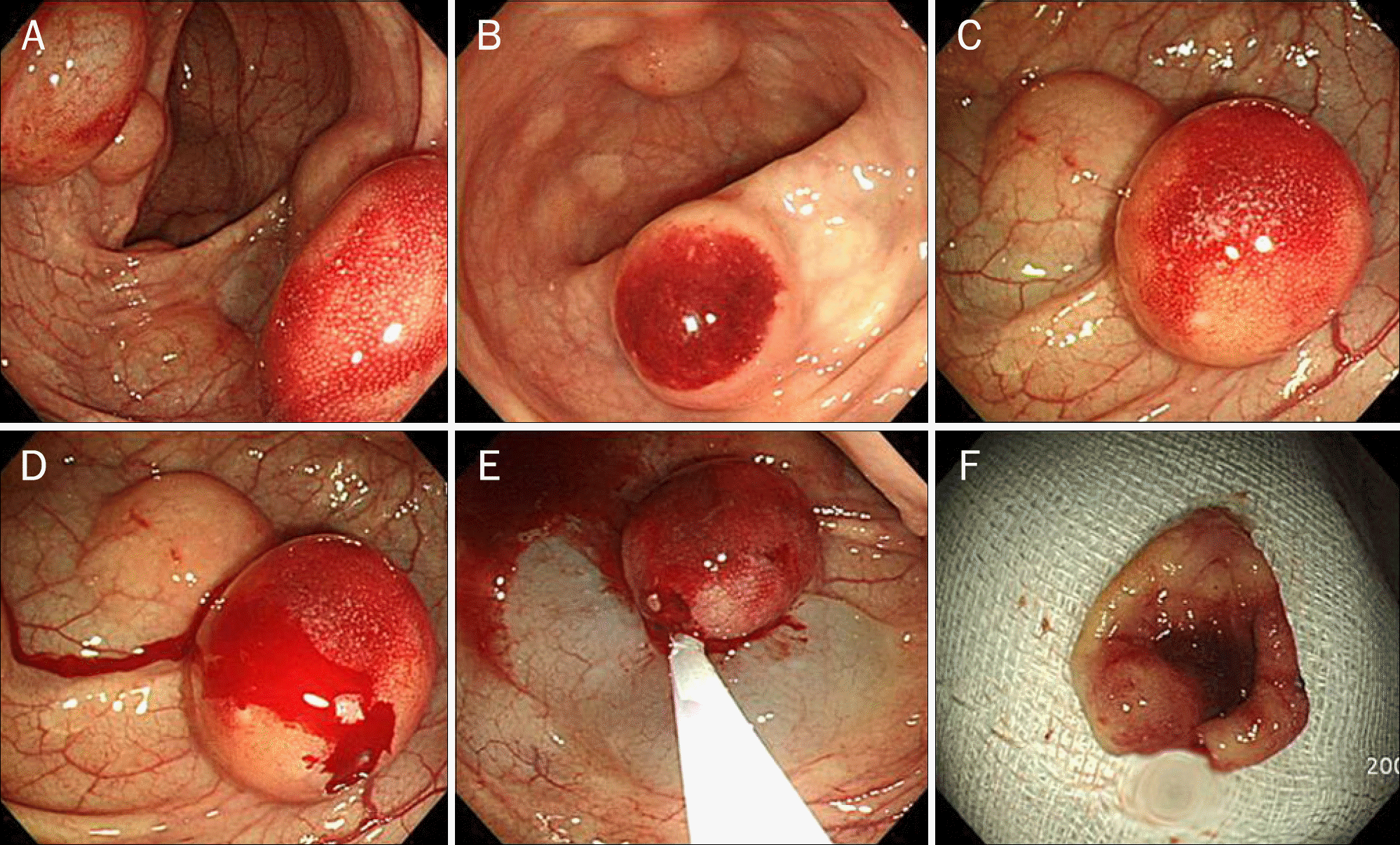
Fig. 2.
Microscopic finding. Cystic structure with surrounding fibrosis in the submucosal layer is seen. Marked hemorrhage in the mucosa layer is also observed (H&E, ×100).
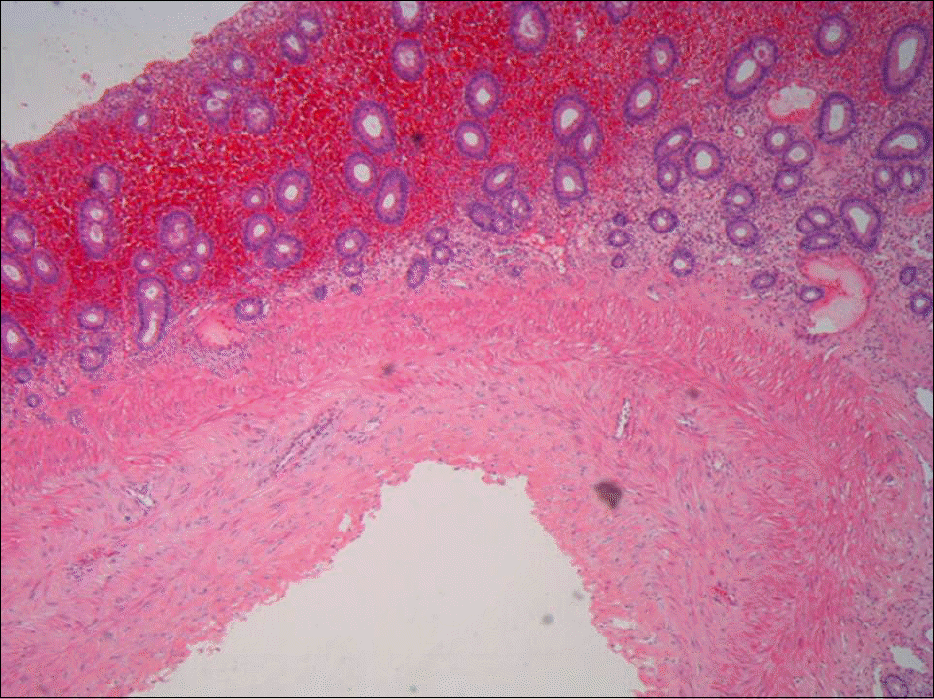
Fig. 3.
Computed tomography scan. Transverse (A) and coronal (B) views show multiple isolated intramural air-filled cystic lesions (arrows) in the left-sided colon on lung window settings (width of 1,500 HU and level of −400 HU).
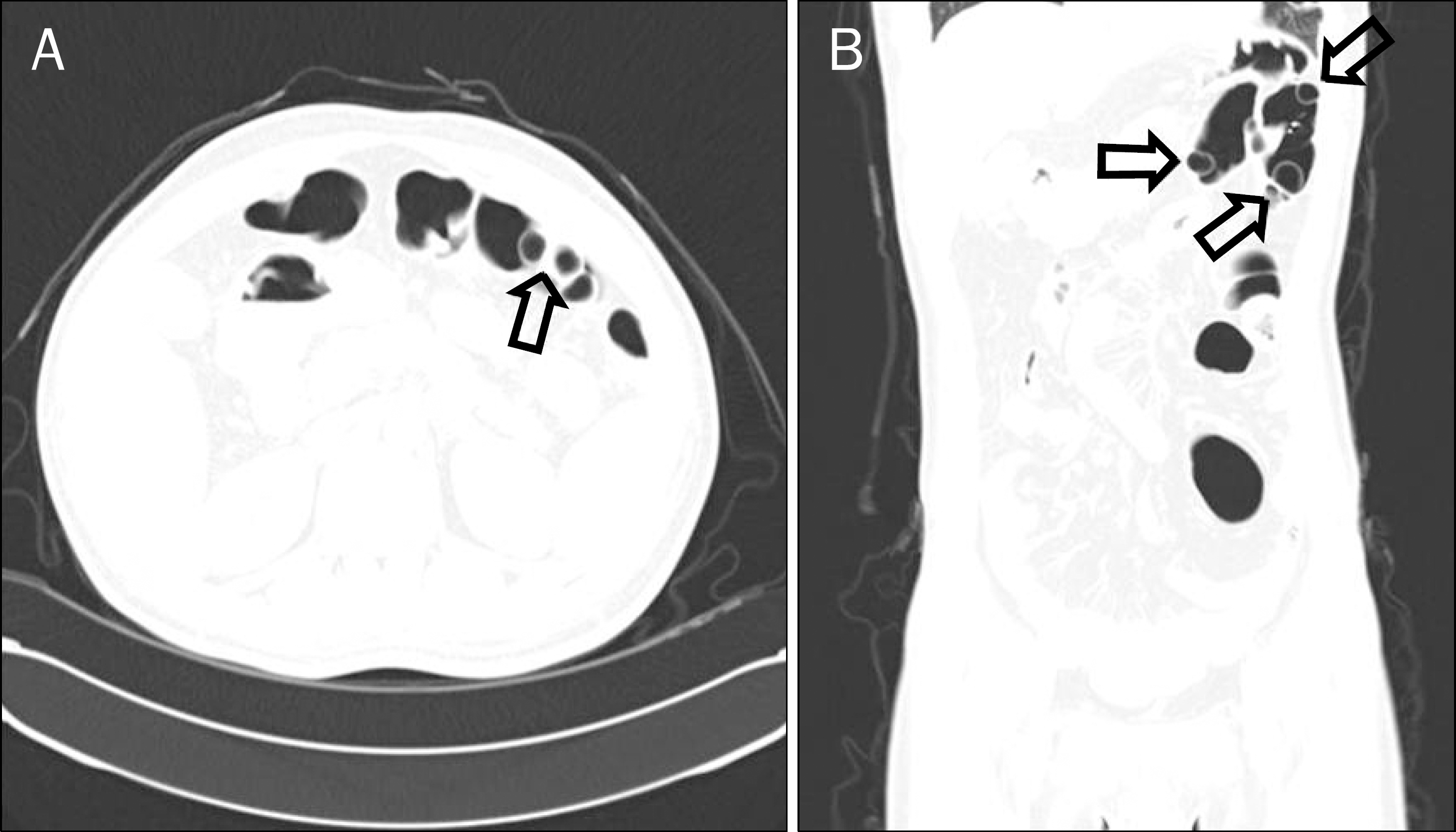
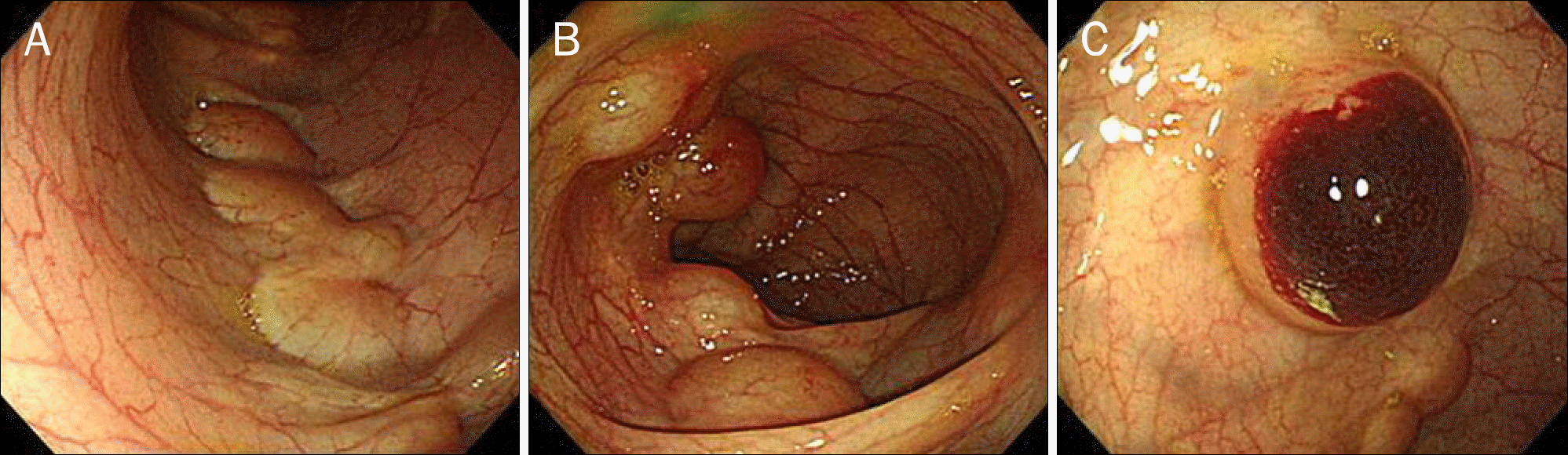
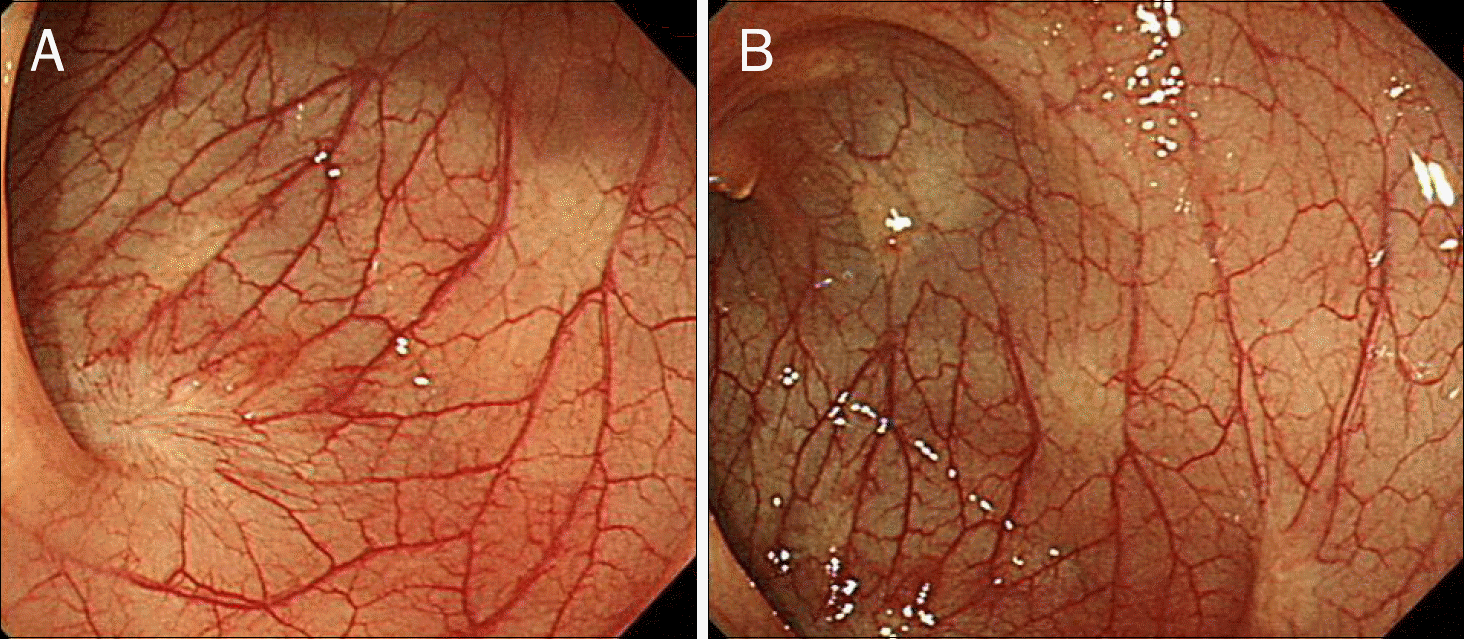
Fig. 4.
Findings of the second colonoscopic examination performed 6 months after the index colonoscopy. (A, B) Although multiple submucosal tumors are still noted, the degree of distension and congestion of individual lesions seem to have decreased. Endoscopic mucosal resection is being performed on the most hyperemic lesion (C).




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download