Abstract
Meningioma's account for around 15% of all primary brain tumors with some 10% of meningiomas arising in the posterior fossa. In rare cases, a meningioma can form around the endolymphatic sac. When formed in the posterior fossa, meningioma tumors can produce vague, non-specific vertiginous symptoms. Research has observed that a subset of these lesions could produce symptoms indistinguishable from those of Meniere's disease. Therefore, we described the clinical features of a case of posterior petrous meningioma with recurrent vertigo as well as the substantial resolution of symptoms after tumor removal via transmastoid approach.
Meningiomas are the most common benign tumors of the brain. The incidence rate of meningioma is around 15% of all primary brain tumors. Research suggests some 8% of tumors from the cerebellopontine angle (CPA) are meningioma's [1]. Approximately 10% of meningiomas arise in the posterior fossa [1]. As these tumors grow and involve the CPA, their clinical manifestations mimic those commonly seen in patients with ascoustic neuroma.
However, a few cases were reported of meningiomas inducing vertiginous sensations where the meningioma does not occupy the internal auditory meatus, but surrounds the region of the endolymphatic sac. Coelho et al. [2] presented 3 cases of posterior fossa meningiomas with Ménière's-like symptoms. In their report, the posterior fossa meningioma's were limited to the dura overlying the endolymphatic sac; not in the region of internal auditory meatus. This suggests that posterior fossa meningiomas around the endolymphatic sac could produce vertiginous sensations by inducing endolymphatic hydrops.
In this article, we describe one case of a posterior fossa meningioma with recurrent vertigo and headache.
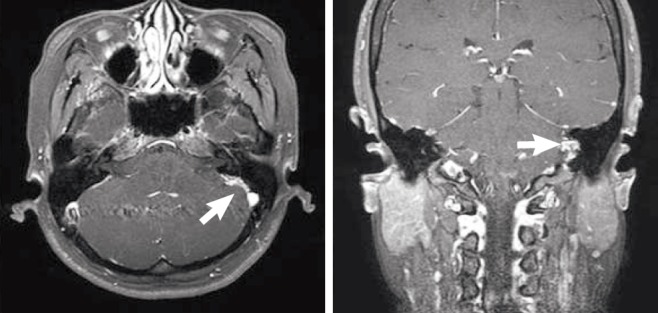
A 44-year-old woman presented with several-years history of episodic vertigo lasting from several minutes up to several hours and was accompanied by headache. She did not complain of hearing loss, tinnitus, otalgia, otorrhea, or facial palsy. She had no other significant medical history. A complete otolaryngologic examination including flexible nasopharyngoscopy and neurologic tests suggested the autonomic system was normal. Over the years, the severity has increased in the episodes. Just before seeking help at our hospital, the patient visited the emergency room twice for vertigo and headache. We performed a pure-tone audiogram, vestibular function tests, rotation test, electrocochleography (EcoG), vestibular evoked myogenic potential, computer tomography (CT), and magnetic resonance imaging (MRI). Her pure-tone audiogram proved to be normal, but the Caloric test indicated a left canal paralysis of 72% and right directional preponderance of 30%. The cochlear summating potential to auditory nerve action potential ratio (SP/AP ratio) of the electrocochleogram was 0.29-0.16. A temporal bone CT scan was performed that revealed a 1.5×1.0 cm round, bony defect at the left posterior petrous ridge (Fig. 1). A contrast-enhanced MRI scan confirmed that a broad-band 1.5×1.0 cm mass was attached to the left posterior petrous ridge. It did not enter the internal auditory canal (IAC). The mass exhibited intense homogenous enhancement after intravenous contrast administration (Fig. 2). Therefore, we surmised that the tumor was an endolymphatic sac tumor. The decision was taken to remove the mass via a transmastoid approach.
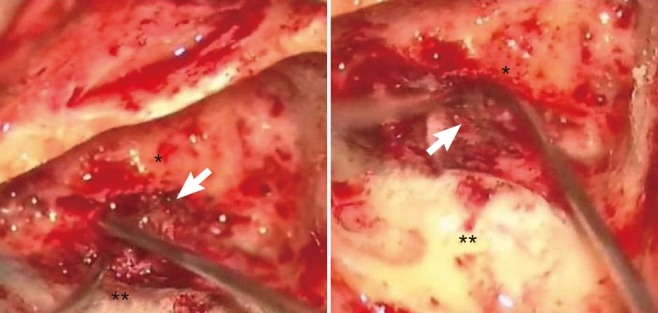
Intraoperatively, the tumor was found to be attached to the dura overlying the endolymphatic sac (Fig. 3). Since there was no evidence that the tumor and 8th nerve were in contact, the tumor and surrounding dura were excised. The endolymphatic duct was identified and was allowed to drain into the posterior fossa. The dural defect was patched with temporalis fascia, and the mastoid cavity was packed using abdominal fat grafts. The final pathology report was consistent with a meningioma. There were no significant postoperative symptoms or relapse and the patient no longer complains of dizziness following surgery. At 1 year, she remains asymptomatic.
Meningiomas constitute approximately 13-18% of all intracranial tumors [3]. Of these, approximately 8-12% are located in the posterior cranial fossa [4, 5]. The most common sites of origin, in descending order, are the parasagittal region, falx, convexit, olfactory groove, tuburculum sellae, sphenoid ridge, anterior petrous face, posterior petrous face, and so on [6]. Meningiomas of the posterior cranial fossa compose 5% to 8% of all intracranial meningiomas and around 10% to 15% of CPA tumors [6].
The clinical manifestations of meningiomas of the CPA are similar to those of acoustic neuromas, and it is often difficult to differentiate these two entities by their clinical presentations. Progressive hearing loss, tinnitus, disequilibrium, and other cranial nerve function abnormalities are common to both lesions [1]. However, the onset of clinical manifestations of posterior petrous meningioma are often insidious, although it is dependent on the site of origin. Due to the fact that meningiomas grow insidiously, neurological findings are absent in the majority of cases until the tumor becomes relatively large [4]. In the case of meningiomas in the IAC or posterior petrous area, the initial symptoms are frequently otologic such as hearing loss or vertigo [7]. In 1996, Friedman et al. [7] described two similar patients with posterior petrous meningiomas presenting atypical Ménière's disease. Cmejrek and Megerian [8] described 3 patients with Ménière's-like symptomatology who were diagnosed as having a meningioma affecting the endolymphatic sac. Coelho et al. [2] presented 3 cases of posterior fossa meningiomas with Ménière's-like symptoms. Arachnoid cysts in the posterior fossa have also been reported to cause Ménière's-like symtoms. Hadley et al. [9] described a posterior fossa arachnoid cyst in a 40-year-old man with unilateral tinnitus, constant lightheadedness, disequilibrium, and occasional vertigo. Haberkamp et al. [10] described one of three study cases of posterior fossa arachnoid cyst in which the patient exhibited classic symptoms of Ménière's disease. In our case, the patient presented with only episodic vertigo and headache without fluctuating hearing loss, tinnitus, or dizziness because of a very small sized tumor.
The mechanism by which a posterior petrous meningioma results in Ménière's-like symptoms remains unknown. However, some authors described the intimate involvement of these tumors with the endolymphatic sac. The subsequent dysfunctions of the sac resulting from local invasion, compression by local hyperostosis, or changes in the microcirculation lead to aberrant endolymphatic homeostasis and subsequent hydrops [7]. Direct tumor invasion or hyperostotic compression of the endolymphatic system leading to hydrops has been well described in the guinea pig model [11]. However, the difficulty of detecting hydrops in human subjects has made it difficult to verify, with any certainty, a cause-and-effect relationship between endolymphatic obstruction and hydrops. Recently, several cases support the concept that obstruction of the endolymphatic sac and duct by a tumor can produce Ménière's-like symptoms; possibly via the production of endolymphatic hydrops, similar to observations in the guinea pig [11]. Friedman et al. [7] noted that a tumor in the region of the endolymphatic sac causes endolymphatic hydrops and that the resultant endolymphatic hydrops trigger Ménière's-like symptoms. Preserved hearing, in this case, was explained as non-invasion of the internal acoustic canal, or spread into the endolymphatic sac. This concept is supported by 2 cases of Ménière's-like symtoms reported by Cmejrek and Megerian [8] in which endolymphatic sac compression resulted in EcoG changes suggestive of hydrops. Kakigi et al. [12] described normalization of an elevated SP/AP ratio on EcoG tests after removal of a posterior fossa meningioma. Although our case has not presented fluctuating hearing loss or a change of SP/AP ratio, the case has provided further evidence to support the concept that endolymphatic hydrops represents the pathophysiologic mechanism in the production of Ménière's symptomatology.
Once these tumors are diagnosed, their surgery is fairly straightforward. Most tumors can be removed through a presigmoid or retrolabyrinthine approach. This approach, familiar to neuro-otologists, provides adequate exposure for smaller tumors, including petrous ridge meningioma [13]. If wider exposure is needed, hearing preservation action should be undertaken with the retrosigmoid approach. This technique includes a direct approach through the temporal bone and no cerebellar retraction. Hearing is preserved since no nerves are manipulated [13]. In our case, the patient's small-sized tumor was removed through a transmastoid approach and the remaining mastoid cavity was plugged with fat to prevent a postoperative cerebrospinal fluid leakage.
In summary, a meningioma presenting Ménière's symptoms is very rare, but it is worthy of diagnostic consideration even in those patients with typical or atypical Ménière's disease. Once diagnosed, clinicians should consider the surgical removal of tumors to facilitate the complete resolution of symptoms. In our case, the mechanisms of recurrent vertigo were the repeated injuries
of vestibular system by the invasion of endolymphatic sac or mechanical obstruction of endolymphatic sac from tumor.
References
1. Brackmann DE, Bartels LJ. Rare tumors of the cerebellopontine angle. Otolaryngol Head Neck Surg. 1980; Sep-Oct. 88(5):555–559. PMID: 6969383.

2. Coelho DH, Roland JT Jr, Golfinos JG. Posterior fossa meningiomas presenting with Ménière's-like symptoms: case report. Neurosurgery. 2008; 11. 63(5):E1001. PMID: 19005363.
3. Maniglia AJ. Intra and extracranial meningiomas involving the temporal bone. Laryngoscope. 1978; 9. 88(9 Pt 2):Suppl 12. 1–58. PMID: 355750.

4. Scott M. The surgical management of meningiomas of the cerebellar fossa. Surg Gynecol Obstet. 1972; 10. 135(4):545–550. PMID: 5077720.
5. Castellano F, Ruggiero G. Meningiomas of the posterior fossa. Acta Radiol Suppl. 1953; 104:1–177. PMID: 13147998.
6. Laird FJ, Harner SG, Laws ER Jr, Reese DF. Meningiomas of the cerebellopontine angle. Otolaryngol Head Neck Surg. 1985; 4. 93(2):163–167. PMID: 3921906.

7. Friedman RA, Nelson RA, Harris JP. Posterior fossa meningiomas intimately involved with the endolymphatic sac. Am J Otol. 1996; 7. 17(4):612–616. PMID: 8841708.
8. Cmejrek RC, Megerian CA. Obstructing lesions of the endolymphatic sac and duct mimicking Ménière's disease. Ear Nose Throat J. 2004; 11. 83(11):753–756. PMID: 15628631.

9. Hadley MN, Grahm TW, Daspit CP, Spetzler RF. Otolaryngologic manifestations of posterior fossa arachnoid cysts. Laryngoscope. 1985; 6. 95(6):678–681. PMID: 3999903.

10. Haberkamp TJ, Monsell EM, House WF, Levine SC, Piazza L. Diagnosis and treatment of arachnoid cysts of the posterior fossa. Otolaryngol Head Neck Surg. 1990; 10. 103(4):610–614. PMID: 2123320.

11. Kimura RS, Schuknecht HF. Membranous hydrops in the inner ear of the guinea pig after obliteration of the endolymphatic sac. Pract Otorhinolaryngol (Basel). 1965; 27(6):343–354.

12. Kakigi A, Sawada S, Takeda T, Takeuchi S, Higashiyama K, Azuma H. Elevated summating potential in a case of posterior fossa meningioma was normalized by tumor removal. Auris Nasus Larynx. 2002; 7. 29(3):287–290. PMID: 12167453.

13. Russell SM, Roland JT Jr, Golfinos JG. Retrolabyrinthine craniectomy: the unsung hero of skull base surgery. Skull Base. 2004; 2. 14(1):63–71. PMID: 16145586.





 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download