Dear Editor,
Salmonella is one of the major pathogens causing bacterial gastroenteritis or foodborne disease worldwide. Infections with non-typhoidal
Salmonella have been reported in more than 2,000 patients in Korea every year from 2017 to 2019, and it is the fifth most common cause of gastrointestinal infections in Korea following norovirus,
C. perfringens,
Campylobacter, rotavirus group A [
1]. Non-typhoidal
Salmonella infection usually manifests as acute onset of fever, chills, vomiting, and diarrhea, and focal or blood-stream infections develop in some cases [
2].
Production of hydrogen sulfide (H
2S) is a unique property of
Salmonella, and it is commonly detected to differentiate
Salmonella species from other bacterial pathogens using biochemical test media such as triple sugar iron (TSI) agar. However, several non-H
2S-producing
Salmonella species have been isolated in various countries (mainly China) from poultry meat [
3] or clinical samples such as stool or sacral wound (
Table 1) [
45678910]. Enzymes encoded by the
phs,
cysJIH, and
asr operons are essential for H
2S production. Previous studies reported nonsense mutations at different sites on the
phs operon in H
2S-negative
Salmonella strains [
8]. Here, we report a non-H
2S-producing
Salmonella enterica serovar Infantis clinical isolate obtained from the blood sample of a Korean patient, the first such finding in Korea to our knowledge (
Table 1). This study was approved by the Institutional Review Board.
A 63-year-old woman was admitted to Severance Hospital, Seoul, Korea, from January to February 2019 for flank and pelvic pain, and poor general condition. Eight years ago, she was diagnosed as having pancreatic neuroendocrine carcinoma with multiple liver metastases and diabetes mellitus. The patient received chemotherapies from 2011 to 2018 along with radiation therapy in 2017 for bone metastases. On the second day of hospitalization, fever and chills began, accompanied by watery stool and abdominal pain. Her complete blood counts were as follows: leukocytes, 5.2×109/L (neutrophil 82.9%); hemoglobin, 88 g/L; platelets, 111×109/L. Results of biochemical analysis were as follows: BUN/Cr, 15.7/0.15 nmol/L; C-reactive protein, 1,625.7 nmol/L. Urinalysis with microscopy showed 2+ blood, 2+ ketone, and 3+ leukocyte esterase (scale of 0 to 4+ with urine strip), along with a white blood cell count >30/high-power field, indicating pyuria. Notably, two blood cultures and a urine culture obtained on the second and third days of hospitalization, respectively, showed no growth, whereas PCR analysis of stool sample was positive for Salmonella. Abdominopelvic computed tomography showed no bowel wall thickening. On the fourth day, a stool culture was obtained and no colony was detected.
Two sets of blood culture bottles (BacT/Alert FA Plus and BacT/Alert FN Plus; bioMérieux, Marcy-l'Étoile, France) were obtained on the fourth day and immediately incubated in a BacT/Alert 3D automated blood culture system (bioMérieux). After 24 hours, a specific colorimetric visual signal was detected in the BacT/Alert FN plus bottle. Subculture on MacConkey agar plate showed colorless, pale colonies of gram-negative rods (
Fig. 1A). Matrix-assisted laser desorption ionization–time-of-flight mass spectrometry (MALDI-TOF MS) using VITEK MS (bioMérieux) and Bruker Biotyper (Bruker Daltonics, Bremen, Germany) identified
Salmonella species (score ≥2.0) with 99% reliability. The isolate was identified as belonging to serogroup C with a polyvalent antisera kit (JoongKyeom, Ilsan, Korea). The TSI agar biochemical test results were as follows: alkaline, acid, gas-negative, H
2S-negative (
Fig. 1B). The isolate was sent to Research Institute of Public Health and the Environment, Seoul, Korea, to further identify the serotype, and
Salmonella enterica serovar Infantis was confirmed.
Anti-microbial susceptibility of the isolate was determined by the automated broth microdilution method using VITEK 2 (bioMérieux). The isolate was resistant to cefazolin (minimal inhibitory concentration [MIC], 4 µg/mL), cefoxitin (MIC, 4 µg/mL), amikacin (MIC, 2 µg/mL), and gentamicin (MIC, 1 µg/mL). The patient was empirically treated with piperacillin/tazobactam and levofloxacin due to suspected urinary tract or gastrointestinal infection. Metronidazole and ciprofloxacin were administered based on the positive Salmonella PCR result. The blood culture on the eighth day of hospitalization was negative. However, ceftriaxone was administered because fever spiking persisted until discharge (February 2019).
Direct sequencing of the
phs and
cysJIH operons of the isolate was performed, and the sequences aligned to those of strain
Salmonella enterica serovar Infantis FSIS1502916 (NZ_CP016408.1) using DNAman 6.0 (Lynnon, Quebec, Canada). The primers were as follows: cysJ1 forward 5′-CGGCATCGGACAGTTTACCT-3′ and reverse 5′-CTGGATGCTCAGGCGCTAAT-3′, cysJ2 forward 5′-GATTAGCGCCTGAGCATCCA-3′ and reverse 5′-CGTGTCGATGCTGACGTTGA-3′, cysJ3 forward 5′-TTCAACGTCAGCATCGACAC-3′ and reverse 5′-CTGCGTTTACTCACCCCAGT-3′, cysI1 forward 5′-CTCGCGGTATACCTTGCCTG-3′ and reverse 5′-CTGCTGGAGATCGCGAAGAT-3′, cysI2 forward 5′-GCACGCTGGCAATAATCAGG-3′ and reverse 5′-TGCATGCTGAAGCCTACGAA-3′, cysI3 forward 5′-CGATATCATTTTGCGGCGGG-3′ and reverse 5′-CGGTATGGACCTCGAATCGG-3′, cysH forward 5′-GCCGGATTTTTCATAGCAGCA-3′ and reverse 5′-CAGGCAAGGTATACCGCGAG-3′, and previously reported primers for
phs [
10]. Unlike previous cases [
10], no point mutation was found in the coding region of the
phs operon, whereas a nucleotide change (C to T) at the first base pair in the 3′-untranslated region of
phsC was observed. In addition, a 1247A>G variant, causing the V416A missense mutation, was found in
cysJ. This is the first report of a missense mutation in the cys gene in non-H
2S-producing
Salmonella. However, further research is needed to determine whether these mutations influence H
2S production or not.
Since the identification of Salmonella serotype is not possible in most clinical laboratories using conventional biochemical testing, non-H2S-producing Salmonella can be misdiagnosed as Salmonella Typhi or even other Enterobacteriaceae. Therefore, caution is needed with the diagnosis of Salmonella infection.
Figures and Tables
Fig. 1
Biochemical result of non-H2S-producing Salmonella (A) Pale and colorless colonies on a MacConkey agar plate. (B) Non-H2S-producing bacteria in triple sugar iron agar.

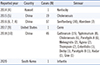
Table 1
Recent worldwide reports of non-H2S-producing Salmonella isolated from clinical samples




 PDF
PDF ePub
ePub Citation
Citation Print
Print





 XML Download
XML Download