Dear Editor,
Cognitive impairment and psychotic symptoms can develop after ischemic or hemorrhagic stroke. In some patients with vascular dementia (VaD), behavioral and psychotic symptoms can be complicated. Psychotic symptoms and VaD are more commonly associated with the right hemisphere.12
Herein, we report a patient with delusion and dementia after a cerebral infarction, who showed hypersexuality during the course of acetylcholinesterase inhibitor (AchEI) treatment.
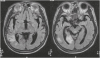
An age 80 male visited our clinic because of falling tendency, memory impairment, and delusional parasitosis complaining about lice in his clothes. He changed his clothes several times daily and sometimes sprayed insecticide on his clothes. His symptoms had begun one year ago, after an ischemic stroke in the territory of the right posterior cerebral artery (Fig. 1). He had been treated with hypertension and with no history of depression.
Neurological examination showed cognitive impairment (17/30 in Korea mini-mental status examination) without additional focal neurologic deficit. Further neuropsychological evaluation using the Seoul Neuropsychological Screening Battery-II showed global cognitive impairment without aphasia (Clinical Dementia Rating Scale=2). Although he was slightly apathic and had insomnia, all the symptoms were not sufficiently severe to meet the diagnostic criteria of major depressive disorders.
Under the impression of VaD, donepezil (5 mg/day) was initially administered for 1 month. As his symptoms remained unchanged, rivastigmine was introduced instead of donepezil. His cognitive function and delusional behavior improved with rivastigmine (3 mg/day). In the second month with rivastigmine (6 mg/day), he indulged in excessive sexual desire. He obtained a prescription for sildenafil citrate (Viagra®) from another physician and repeatedly demanded sexual intercourse throughout the day, with delusion of infidelity. He had slept with his wife less than once a month and had never used impotence drugs before the stroke. The couple had had no sex for 1 year after the stroke.
His hypersexuality did not improve just after the discontinuation of rivastigmine. Antipsychotics (haloperidol and risperidone) were administered without effect. Then escitalopram (10 mg/day) was administered, which could improve his hypersexual behavior and infidelity delusion, while his delusional parasitosis returned to the baseline status before rivastigmine medication.
Clinical features including temporal evolution, neuroimaging, and neuropsychiatric tests were compatible with VaD. Since psychiatric symptoms such as delusion and depressive mood were accompanied by dementia, they could be considered as behavioral and psychological symptoms of dementia (BPSD).
Post-stroke delusion of parasitosis was reported in some patients. Vascular lesions were in the frontal, temporo-parietal, and temporo-occipital lobe, respectively, which were in the right side345 and in these studies, cortical areas were mainly affected. However, recent neuroimaging studies underscored the involvement of striatum in delusional parasitosis not secondary to stroke.6 Although post-stroke symptoms provide better temporal correlation, prospective neuroimaging studies are needed to understand critical areas for delusional parasitosis.
These studies underscored the effect of the right-side lesion in post-stroke delusion. Multiple forms of delusion in this patient also support the delusion-prone status after a right hemispheric stroke.1 There are several hypotheses for the predominant role of the right hemisphere on delusion. Some argue that the underactivity of the right hemisphere may be overdriven by unopposed activity of the left hemisphere.1 Recent studies suggest the failure of pragmatic communication, perceptual integration, attentional surveillance, and belief updating as possible machineries.7
For the treatment of delusional parasitosis, antipsychotics or selective serotonin reuptake inhibitors could be used.5 In this case, AchEI was temporarily effective, albeit unexpected sexual problems limited the usefulness of AchEI. Further studies are needed to find optimal drug therapy for delusional parasitosis.
Sexual dysfunction is a common sequel to stroke, but hypersexuality in relation to stroke is infrequently reported. Various lesions such as temporal or thalamic stroke were common, albeit hemispheric laterality was indefinite.8910 In this patient, hypersexuality appeared during the treatment with AchEI.
Since his hypersexuality was not completely resolved after the discontinuation of AchEI, the causative role of AchEI on hypersexuality remains questionable. In case of BPSD, AchEI can be a useful option, but standard treatment for sexual behavior in dementic patients is not firmly established.11 Paradoxically, there were a few patients with hypersexuality related to donepezil.1213 Enhancing sexual arousal in the brain was suggested as a hypothetical mechanism.12 In this case, AchEI could have played a permissive role on the transformation of delusional parasitosis into a new form of delusion (infidelity delusion) and hypersexuality.
Our patient suffered from multiple psychotic problems and the medications were partly successful, only transforming clinical features into others. Further studies are needed to set up effective treatments for post-stroke psychotic problems.
Figures and Tables
References
1. Devinsky O. Delusional misidentifications and duplications: right brain lesions, left brain delusions. Neurology. 2009; 72:80–87.

2. Desmond DW, Moroney JT, Paik MC, Sano M, Mohr JP, Aboumatar S, et al. Frequency and clinical determinants of dementia after ischemic stroke. Neurology. 2000; 54:1124–1131.

3. Nagaratnam N, O'Neile L. Delusional parasitosis following occipito-temporal cerebral infarction. Gen Hosp Psychiatry. 2000; 22:129–132.

5. Blasco-Fontecilla H, Bragado Jiménez MD, García Santos LM, Barjau Romero JM. Delusional disorder with delusions of parasitosis and jealousy after stroke: treatment with quetiapine and sertraline. J Clin Psychopharmacol. 2005; 25:615–617.

6. Huber M, Karner M, Kirchler E, Lepping P, Freudenmann RW. Striatal lesions in delusional parasitosis revealed by magnetic resonance imaging. Prog Neuropsychopharmacol Biol Psychiatry. 2008; 32:1967–1971.

7. Gurin L, Blum S. Delusions and the right hemisphere: a review of the case for the right hemisphere as a mediator of reality-based belief. J Neuropsychiatry Clin Neurosci. 2017; 29:225–235.

8. Monga TN, Monga M, Raina MS, Hardjasudarma M. Hypersexuality in stroke. Arch Phys Med Rehabil. 1986; 67:415–417.
9. Spinella M. Hypersexuality and dysexecutive syndrome after a thalamic infarct. Int J Neurosci. 2004; 114:1581–1590.
10. Mutarelli EG, Omuro AM, Adoni T. Hypersexuality following bilateral thalamic infarction: case report. Arq Neuropsiquiatr. 2006; 64:146–148.

11. Cerejeira J, Lagarto L, Mukaetova-Ladinska EB. Behavioral and psychological symptoms of dementia. Front Neurol. 2012; 3:73.

12. Lo Coco D, Cannizzaro E. Inappropriate sexual behaviors associated with donepezil treatment: a case report. J Clin Psychopharmacol. 2010; 30:221–222.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download