Lesions in the cervicothoracic junction are not rare, but surgical exposure of this region remains challenging. The anterior sternotomy approach to the cervicothoracic junction requires exact knowledge of the surgical anatomy, skill and careful planning according to the pathology in this region. This is especially true for commonly needed anterior approach lesions in the vertebral body. However, the kyphosis of the upper thoracic spine make the vertebral bodies hard to locate due to its depth, and the presence of neurovascular and osseous obstacles limit the surgical approach.
6101115) To decrease the surgical risk, a thoracic surgeon may aid exposure. In our institute we performed this approach together with a thoracic surgeon for safety and to reduce operation time. Injury to the brachiocephalic veins, thoracic duct, and recurrent laryngeal nerves, may lead to significant complications.
13) The best method is to reach the spine through neurovascular space, and to bypass them. Surgical access is not always limited by osseous obstacles. If simple access to T1 and upper levels is required, the traditional anterior low cervical approach can be enough. However, traditional anterior low cervical approach limits additional work field for procedures such as anterior plating, corpectomy because of the anterior bony structure. Previous authors have mentioned such problems.
6) The sternal manubrium and clavicles often interrupt access to the upper thoracic level (T1–T3). Surgical techniques such as the transsternal, the transclavicular-transmanubrial and transmanubrial approaches have been recommended to gain access. Each approach has its advantages, but limitations exist in all of them. Fielding and Stillwell
5) first reported the anterior low cervical approach to cervicothoracic junction in 1976, but an exposure caudal to T2 is usually limited by sternal manubrium and clavicles. Cauchoix and Binet
2) first described a full median sternum-splitting approach, for T1–T3 in 1957. Hodgson et al.
7) reported that they had performed median sternotomy in upper thoracic tuberculosis spondylitis in 1960. Sundaresan et al.
16) suggested a transclavicular-transmanubrial approach for improving exposure and providing a strut graft in 1984. A modified transmanubrial approach was used by Darling et al.
3) and by Xiao et al.
18) T4, and occasionally T5 can be accessed by this technique. However, a relatively narrow access to the spine is provided (a width of no more than 4 cm).
6) For more working room of this area, Luk et al.
15) used bilateral manubriotomy. This technique could provide a width of approximately 8 cm, but transverse osteotomy of the sternum and ligations of the bilateral internal thoracic arteries is needed.
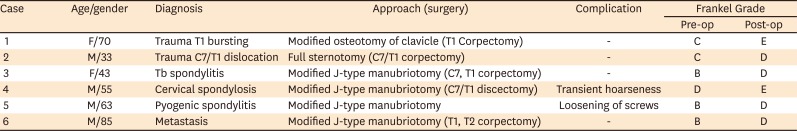
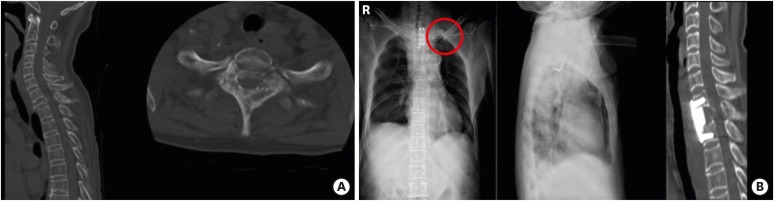
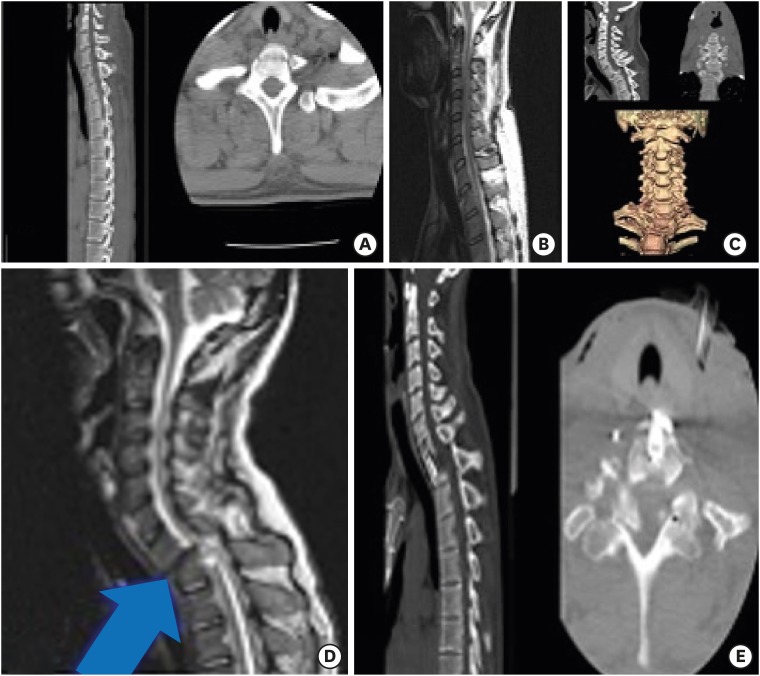
In our case, we used 2 modified anterior cervicothoracic approach methods. We performed a modified transmanubriosternal approach combined with a standard cervical incision (Smith-Robinson approach) in one case and a modified transsternal transclavicular approach with standard cervical incision in another case. Both approach provided the same surgical field. To decide the surgical approach pre-operative radiologic evaluation must be done to determine the extent of surgery and to anticipate the surgical field. We used three guidelines for pre-operative radiologic evaluation. The Teng guideline determined the extent of operation based on the lesion location using the Cervicothoracic angle as the standard.
17) The Karikari guideline also determined the extent of operation using the intervertebral disc line as a standard.
9) The Falavigna guideline was used to determine the extent of surgery and also anticipate the surgical field using the Surgeons' view line.
4)
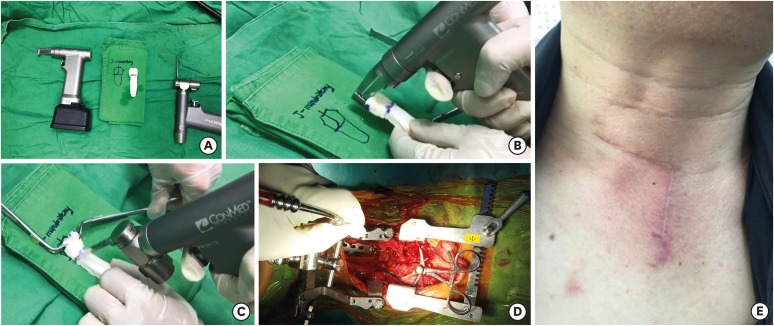
With our experience, we recommend the modified transmanubriosternal approach combined with a standard cervical incision. This procedure is somewhat simple to perform, requires little additional operative time for opening or closure. It provides excellent operative field view. The regional anatomy is also familiar to neurosurgeons. There is no associated severe complication and comorbidity related to this approach.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download