Abstract
Purpose
This study aimed to evaluate the usefulness of a behavioral cue checklist (BCC) containing 17 items developed by Wilkes et al. (2010) for identifying potentially violent patients in emergency departments.
Methods
This was a prospective observational study to evaluate the usefulness of the Korean version of a BCC (K-BCC) as an assessment tool for predicting patient violence in emergency departments, and was conducted over 4 weeks in a regional emergency medical center located in B City. A total of 1,324 patients were finally analyzed.
Results
Logistic regression analysis was performed to investigate whether each item of the K-BCC predicts violence, and a parsimonious set of 8 statistically significant items was selected for the tool. Receiver operating characteristic analysis of the BCC showed that the area under the curve was .97 (95% confidence interval: .94~1.0). The sensitivity, specificity, positive predictive value, and negative predictive value at the cut-off score of 2 were 75.6%, 98.9%, 68.2%, and 99.2%, respectively.
Conclusion
The K-BCC was found to be useful in predicting patient violence toward emergency department staff. This tool is simple, and fast to use and can play a significantly role identifying potentially violent patients. Owing to this advance identification, this tool can be helpful in preventing the potential for violence from manifesting as violent behaviors.
References
1. Jackson D, Wilkes L, Luck L. Cues that predict violence in the hospital setting: Findings from an observational study. Collegian. 2014; 21(1):65–70. https://doi.org/10.1016/j.colegn.2013.02.006.

2. Kim MH, Park SB. Service design for the prevention of ER violence: Based on the ER cases of Korea University Medical Center. Journal of Basic Design & Art. 2016; 17(3):29–44.
3. Park EY, Lee EN. Predictors of violent behavior by patient or caregiver of patient in the emergency department. Korean Journal of Adult Nursing. 2014; 26(5):500–511. https://doi.org/10.7475/kjan.2014.26.5.500.

4. Simon RI. Patient violence against health care professionals [Internet]. Newburyport (MA): Psychiatric Times;c2011. [cited 2011 Mar 3]. Available from:. https://pro.psychcentral.com/patient-violence-against-health-care-professionals/00775.html.
5. Gates DM, Ross CS, McQueen L. Violence against emergency department workers. The Journal of Emergency Medicine. 2006; 31(3):331–337. https://doi.org/10.1016/j.jemermed.2005.12.028.

6. Copeland D, Henry M. Workplace violence and perceptions of safety among emergency department staff members: Experiences, expectations, tolerance, reporting, and recommendations. Journal of Trauma Nursing. 2017; 24(2):65–77. https://doi.org/10.1097/jtn.0000000000000269.

7. Korea Ministry of Government Legislation. Medical Law [Internet]. Sejong: Korea Ministry of Government Legislation;c2016. [cited 2016 May 29]. Available from:. http://www.law.go.kr/lsInfoP.do?lsiSeq=183646#0000.
8. Kim JC, Seol YM, Song HS. Survey of emergency department violence. Journal of the Korean Society of Emergency Medicine. 2003; 14(3):309–313.
9. Roy JA. Predictive behavioral cues of patient violence in the emergency department [master’s thesis]. Providence (RI): Rhode Island College;2013. p. 1–41.
10. Kim SC, Ideker K, Todicheeney-Mannes D. Usefulness of aggressive behaviour risk assessment tool for prospectively identifying violent patients in medical and surgical units. Journal of Advanced Nursing. 2012; 68(2):349–357. https://doi.org/10.1111/j.1365-2648.2011.05744.x.

11. Noh JH, Na YK. Effects of violence experience, emotional labor, and job stress on clinical nurses’ depression. Korean Journal of Occupational Health Nursing. 2015; 24(3):153–161. https://doi.org/10.5807/kjohn.2015.24.3.153.

12. Yang JH, Jung HY. Relationship between violence response, coping, and burnout among emergency department nurses. Journal of Korean Academy of Fundamentals of Nursing. 2009; 16(1):103–111.
13. Luck L, Jackson D, Usher K. STAMP: Components of observable behaviour that indicate potential for patient violence in emergency departments. Journal of Advanced Nursing. 2007; 59(1):11–19. https://doi.org/10.1111/j.1365-2648.2007.04308.x.

14. Chapman R. Styles I. An epidemic of abuse and violence: Nurse on the front line. International Emergency Nursing. 2006; 14(4):245–249. https://doi.org/10.1016/j.aaen.2006.08.004.
15. Novitsky MA, Julius RJ, Dubin WR. Non-pharmacologic management of violence in psychiatric emergencies. Primary Psychiatry. 2009; 16(9):49–53.
16. Deans C. The effectiveness of a training program for emergency department nurses in managing violent situations. Australian Journal of Advanced Nursing. 2004; 21(4):17–22.
17. Bjørkly S, Hartvig P, Heggen FA, Brauer H, Moger TA. Development of a brief screen for violence risk (V-RISK-10) in acute and general psychiatry: An introduction with emphasis on findings from a naturalistic test of interrater reliability. European Psychiatry. 2009; 24(6):388–394. https://doi.org/10.1016/j.eurpsy.2009.07.004.

18. Wilkes L, Mohan S, Luck L, Jackson D. Development of a violence tool in the emergency hospital setting. Nurse Researcher. 2010; 17(4):70–82. https://doi.org/10.7748/nr2010.07.17.4.70.c7926.

19. Irwin A. The nurse’s role in the management of aggression. Journal of Psychiatric and Mental Health Nursing. 2006; 13(3):309–318. https://doi.org/10.1111/j.1365-2850.2006.00957.x.

20. Kim GR. Workplace mistreatment in Korea and Europe-comparison study of discrimination, sexual harassment and violence [master’s thesis]. Seoul: Seoul National University;2017. p. 1–58.
21. Faul F, Erdfelder E, Buchner A, Lang AG. Statistical power analyses using G*Power 3.1: Tests for correlation and regression analyses. Behavior Research Methods. 2009; 41(4):1149–1160. https://doi.org/10.3758/BRM.41.4.1149.

22. Polit DF, Beck CT. The content validity index: Are you sure you know what’s being reported? Critique and recommendations. Research in Nursing & Health. 2006; 29(5):489–497. https://doi.org/10.1002/nur.20147.

23. National Institute for Occupational Safety and Health. Violence: Occupational hazards in hospitals [Internet]. Atlanta: U.S. Department of Health & Human Services;c2002. [cited 2014 Jun 6]. Available from:. http://www.cdc.gov//niosh/docs/2002-101/pdfs/2002-101.pdf.
24. Daniel C, Gerdtz M, Elsom S, Knott J, Prematunga R, Virtue E. Feasibility and need for violence risk screening at triage: An exploration of clinical processes and public perceptions in one Australian emergency department. Emergency Medicine Journal. 2015; 32(6):457–462. https://doi.org/10.1136/emermed-2013-202979.

25. Weir JP. Quantifying test-retest reliability using the intraclass correlation coefficient and the SEM. Journal of Strength and Conditioning Research. 2005; 19(1):231–240. https://doi.org/10.1519/00124278-200502000-00038.

26. Song SW. Using the receiver operating characteristic (ROC) curve to measure sensitivity and specificity. Korean Journal of Family Medicine. 2009; 30(11):841–842. https://doi.org/10.4082/kjfm.2009.30.11.841.

27. Lalkhen AG, McCluskey A. Clinical tests: Sensitivity and specificity. Continuing Education in Anaesthesia Critical Care & Pain. 2008; 8(6):221–223. https://doi.org/10.1093/bjaceaccp/mkn041.

28. Jo YH. A study on violence experience among nurse in university hospitals [master’s thesis]. Busan: Dong-A University;2017. p. 1–93.
Figure 1.
Behavioral Cue Checklist (BCC) Receiver Operating Characteristics (ROC) curve. Diagonal broken line represents the line of no discrimination with Area Under the Curve (AUC) of .5. Solid curve represents the BCC with AUC of .97 (95% CI=0.94~1.0; p<.001).
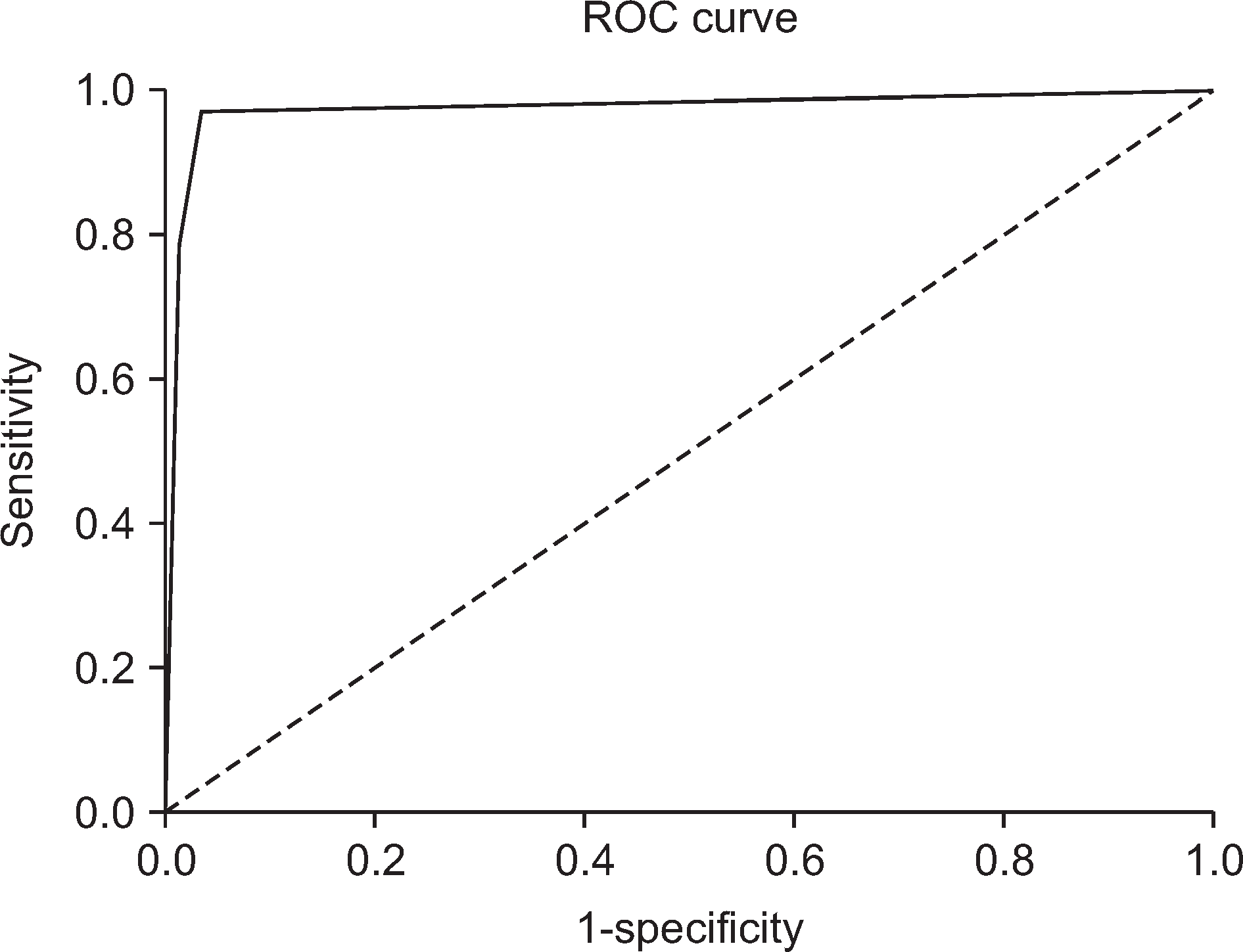
Table 1.
General Characteristics and Violence-Related Characteristics (N=1,324)
Table 2.
Comparison of Cue Occurrence Between Violent and Non-Violent Group (N=1,324)
| Cues | Violent Group (N=37) n (%) | Non-violent Group (N=1,287) n (%) | χ2* | p | |
|---|---|---|---|---|---|
| 1 | Threat of harm | 12 (32.4) | 5 (0.4) | 291.36 | <.001 |
| 2 | Clenched fists/Tense posture | 9 (24.3) | 21 (1.6) | 83.63 | <.001 |
| 3 | Name-calling | 11 (29.7) | 5 (0.4) | 259.35 | <.001 |
| 4 | Irritability | 10 (27.0) | 22 (1.7) | 97.74 | <.001 |
| 5 | Sharp or caustic retorts | 13 (35.1) | 5 (0.4) | 323.80 | <.001 |
| 6 | Demanding attention | 12 (32.4) | 11 (0.9) | 210.09 | <.001 |
| 7 | Aggressive statements | 11 (29.7) | 3 (0.2) | 299.09 | <.001 |
| 8 | Resisting healthcare | 13 (35.1) | 8 (0.6) | 274.46 | <.001 |
| 9 | Swearing | 5 (13.5) | 2 (0.2) | 122.03 | <.001 |
| 10 | Walking back and forth to nurses' station | 8 (21.6) | 5 (0.4) | 166.78 | <.001 |
| 11 | Demeaning inflection | 7 (18.9) | 0 (0.0) | 244.78 | <.001 |
| 12 | Humiliating remarks | 1 (2.7) | 0 (0.0) | 34.81 | .028 |
| 13 | Intimidation | 3 (8.1) | 0 (0.0) | 104.58 | <.001 |
| 14 | Prolonged staring at nurse | 9 (24.3) | 3 (0.2) | 232.41 | <.001 |
| 15 | Increased volume of speech | 15 (40.5) | 4 (0.3) | 411.52 | <.001 |
| 16 | Pacing | 4 (10.8) | 5 (0.4) | 57.86 | <.001 |
| 17 | Belligerence | 10 (27.0) | 5 (0.4) | 227.85 | <.001 |
| Number of patients displaying cues | 100 (7.6) | ||||
| Number of patients not displaying cues | 1,224 (92.4) | ||||
Table 3.
Prediction of Violence with Cues




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download