This article has been
cited by other articles in ScienceCentral.
A 46-year-old man was admitted with neck injury due to self-inflicted airgun shot 2 months prior. An internal carotid artery stent insertion was performed and the patient was alert and oriented but had evidence of dysphagia and hoarseness. The laryngoscopy revealed left vocal cord paralysis and the videofluoroscopic swallowing study (VFSS) revealed pyriform sinus residue, aspiration, laryngeal elevation, and failure of upper esophageal sphincter (UES) relaxation. After being diagnosed with left vocal cord paralysis due to left vagus nerve injury and cricopharyngeal dysfunction, endoscopic CO
2 laser cricopharyngeal myotomy using CO
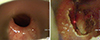
2 laser 3.0 watt, super-pulse continuous mode and injection laryngoplasty of left vocal cord using Restylene™ (Q-Med, Uppsala, Sweden) were performed under general anesthesia (
Fig. 1A and B). During the laryngoscopy performed 30 days after the operation, there was no glottic gap when vocal cord movement was observed. Esophagography did not reveal the beak-like narrowing. Seven months after the operation, dysphagia and hoarseness symptoms improved and progress was observed.
A 25-year-old woman without a specific history was admitted due to persistent dysphagia, throat pain, and cough after drinking a presumed alkaline fluid for a suicide attempt. After the event, subtotal esophagectomy and cervical colon interposition were immediately performed in thoracic surgery. Laryngoscopy revealed the right vocal cord paralysis, and stricture of the UES in esophagography was observed. Upper gastrointestinal endoscopy was performed due to persistent dysphagia and vomiting, and revealed stenosis of the pharyngo-esophageal junction. Endoscopic CO
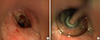
2 laser surgery and balloon dilatation with both controlled radial expansion (CRE™) balloon dilator 12 mm (Boston Scientific, Marlborough, MA, USA) and number 11 hepatobiliary dilator were performed under general anesthesia (
Fig. 2A and B). Postoperative esophagography revealed no esophageal stenosis. Six months after the surgery, at the outpatient clinic follow-up, the patient displayed the symptom of swallowing discomfort, but esophagography showed no obstruction or stricture. Currently she has been doing well in follow-ups.
We are reporting 2 cases of attempted suicides presenting with dysphagia due to UES dysfunction. The UES consists of the inferior pharyngeal constrictor muscle, cricopharyngeus muscle and part of the upper esophagus (
12). Incomplete relaxation of cricopharyngeus muscle, stiffness due to tissue fibrosis, and stricture can cause dysphagia in which a food bolus fails to enter the esophagus and remains or refluxes into airways. Endoscopic CO
2 laser cricopharyngeal myotomy has been recently reported to reduce the complications of esophageal fistulae and vocal cord paralysis (
23). Another method is endoscopic balloon dilatation. The endoscopic balloon dilatation has limitations of long-lasting effects compared to cricopharyngeal myotomy, but is useful for elderly patients with high risk of anesthesia or surgery-related complications, and can be considered in patients with cricopharyngeal fibrosis (
4). These 2 cases occurred secondary after suicide attempt and are disorders of the UES relaxation due to different mechanisms. The first case was UES relaxation failure due to injury of vagus nerve, which is failure of neural inhibition of tonic cricopharyngeal contraction. The second case was pharyngo-esophageal junction stenosis due to the fibrotic change of UES after esophageal surgery. In addition, the second patient refused an invasive surgery after previous thoracic surgery. Therefore, we performed conservative treatment with endoscopic balloon dilatation. Although these patients were already treated with appropriate life-saving treatment, we treated the complication of dysphagia caused by disorders of the UES.










 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download