Abstract
Objective
The aim of this study was to compare the surgical outcomes of single-port access (SPA) and conventional multi-port access total laparoscopic hysterectomies (TLH) among patients with very large uteri (500 g or more).
Methods
Fifty consecutive patients who received TLH for large uterine myomas and/or adenomyoses weighing 500 g or more between February 2009 and December 2012 were retrospectively reviewed. SPA and conventional TLH were each performed in 25 patients. Surgical outcomes, including operation time, estimated blood loss, postoperative hemoglobin change, postoperative hospital stay, postoperative pain, and perioperative complications, were compared between the two groups.
Results
There were no significant demographic differences between the two groups. All operations were completed laparoscopically with no conversion to laparotomy. Total operation time, uterus weight, estimated blood loss, and postoperative hemoglobin change did not significantly differ between the two groups. Postoperative hospital stay was significantly shorter for the SPA-TLH group compared to that of the conventional TLH group (median [range], 3 [2.0-6.0] vs. 4 [3-7] days; P=0.004]. There were no inter-group differences in postoperative pain at 6, 24, and 72 hours after surgery. There was only one complicated case in each group.
Total laparoscopic hysterectomy (TLH) is currently the standard procedure in patients requiring hysterectomy. Laparoscopy has several advantages over laparotomy, including improved cosmetic results, shorter hospital stays, faster recovery, lower costs, reduced incisional morbidity, and reduced pain [1,2]. To optimize the benefits of this minimally invasive technique, surgeons have attempted to decrease the port size and number of trocars used in the procedure [3,4,5]. The concept of single-port laparoscopic surgery was introduced to gynecology about 40 years ago. In 1969, Wheeless [6] and in 1971, Thompson and Wheeless [7] published a study of laparoscopic tubal ligation using single-trocar laparoscopy. In 1991, Pelosi and Pelosi [8] reported laparoscopic hysterectomy (LH) with bilateral salpingo-oophorectomy (BSO) using a single incision. Single-port access (SPA) laparoscopy results in reduced trauma to the abdominal wall and improved cosmetic effects compared to those achieved with multi-port access laparoscopy. However, gynecologic surgeons have not rapidly adopted SPA laparoscopy due to technical difficulties. However, advanced surgical skills and instruments now enable many surgeons to perform single-port laparoscopic surgery. SPA laparoscope-assisted vaginal hysterectomy (LAVH) has been shown to be a feasible approach [9,10]. However, it is difficult to remove a large uterus laparoscopically because of reduced pelvic space, an extensive vascular supply, and the distorted pelvic anatomy, which increase the risk of bleeding and complications [11]. Therefore, few studies of SPA-LAVH or SPA-TLH for large uteri exist [9,11,12]. Song et al. [9] and Song et al. [12] published a prospective study of single-port laparoscopy and showed that it was safe; however, this was a case series without a control group. In 2012, Lee et al. [11] published a retrospective report of SPA-LH in patients with large uteri; this study showed that SPA-LH required a longer operating time. In this study, we retrospectively evaluated the feasibility and safety of SPA-TLH compared to those of conventional TLH in patients with large uteri (≥500 g).
There were 50 patients who received a TLH with or without salpingo-oophorectomy for benign disease of the uterus weighing 500 g or more from February 2009 to December 2012 at Severance Hospital, Yonsei University College of Medicine in Seoul, Korea. We evaluated 50 consecutive patients with large uteri who received SPA-TLH (n=25) or conventional TLH (n=25) with or without salpingo-oophorectomy. Written informed consent was obtained from all patients prior to surgery. Patients with confirmed gynecologic malignancies or relatively small uteri weighing less than 500 g and patients who received concurrent surgery in additional anatomical areas were excluded.
The two groups were compared for age, parity, body mass index (BMI), previous abdominal surgeries, and uterine weight. The BMI was calculated according to the standard Word Health Organization criteria. Vaginal delivery and cesarean section delivery were included in parity. The uterus was weighed immediately after the hysterectomy in the operating room. Surgical outcomes, including operation time (minutes), estimated blood loss (mL), serum hemoglobin (Hb) drop (change between the preoperative Hb and Hb one day after surgery), postoperative hospital stay (days), and number of pain killers (times), were compared between the SPA-TLH and conventional TLH groups. Operation time was defined as the time from umbilical incision to completion of skin closure. The estimated blood loss was based on the total volume of suction. Patients were discharged if they had no fever, were able to tolerate a soft or normal diet, walked well, and were able to self-void after removal of the urinary catheter. The total number of injected pain killers before discharge was retrospectively determined from medical records. Postoperative pain intensity was evaluated using the visual analog scale with scores from 0 (no pain) to 10 (the worst pain). We asked patients to rate their pain intensity at 6, 24, and 72 hours after surgery.
All single-port laparoscopic procedures were performed according to a technique previously described by our group [13]. Briefly, a RUMI uterine manipulator was placed with a KOH colpotomizer system (Cooper Surgical, Shelton, CT, USA) in all patients. For a single-port system, after making a 1.5-cm vertical intra-umbilical skin incision, the Alexis wound retractor (Applied Medical, Laguna Hills, CA, USA) was inserted into the peritoneal cavity through the umbilicus. A 7½ surgical glove was fixed to the outer ring of the wound retractor. After making small incisions in the finger-tip portions of the glove, two 5-mm trocars and one 11-mm trocar were inserted. A 45-cm-long, rigid, 30-degree, 5-mm endoscope was used for the single-port system. For the conventional TLH, two 5-mm and two 10-mm trocars were inserted, and a 30-cm-long, rigid, 30-degree, 10-mm endoscope was used. Surgical instruments included bipolar forceps, monopolar L-hook, scissors, atraumatic graspers, toothed biopsy forceps with a slightly bent shaft, laparoscopic needle holders, a suction-irrigation system, and the LigaSure system (Covidien, Boulder, CO, USA).
The overall procedure of SPA-TLH was similar to that of conventional TLH with three or four ports. Traction of the distal portion of the fallopian tube was introduced with a biopsy forceps that had a slightly bent steel shaft. The tube pedicles and utero-ovarian ligaments were then secured and divided by the LigaSure system. The round ligaments were retracted with a bent biopsy forceps and secured and divided by the LigaSure system. To expose the pelvic side wall, the uterine body was pushed medially with a bent biopsy forceps; the broad ligaments were then dissected with a monopolar L-hook (Fig. 1). The vesico-uterine peritoneal fold was opened, and the bladder was mobilized with a blunt and sharp dissection using an L-hook until the anterior vagina was identified. At the same time, the huge uterus was retro-flexed and pushed toward the abdominal cavity with a bent biopsy forceps. Anterior colpotomy was performed with an L-hook over the colpotomizer cup. The uterine vessels were skeletonized, sealed, and divided using an L-hook and the LigaSure system. After securing the bilateral uterine vessels once more, the lateral vaginal wall was cut with a monopolar L-hook. The posterior vaginal wall was cut at the cervicovaginal junction just above the uterosacral ligament, leaving the vaginal supports intact. The huge uterus was removed through the vagina. To close the vaginal cuff, a 40-mm, round-bodied needle was introduced through the 11-mm port, and an intracorporeal continuous suture and tie were introduced.
Demographic findings of patients are shown in Table 1. Among women who received SPA-TLH, 13 had previous abdominal surgeries. In addition, 13 women had myomas, one with adenomyosis and 11 with both adenomyosis and myoma. Among 25 participants who had conventional TLH, six had previous abdominal surgeries, and 15 had myomas, two with adenomyosis and eight with both adenomyosis and myoma. In the SPA-TLH group, 16 patients received only TLH. Seven patients had TLH with unilateral salpingo-oophorectomy (USO)/BSO; one patient had TLH with cystectomy, and one patient had TLH with appendectomy. In the conventional group, 19 patients received TLH only. Four patients had TLH with USO/BSO; one had TLH with ovarian/parovarian cystectomy, and one had TLH with transobturator tape. There were no significant differences in age, BMI, parity, or uterine weight (Table 1).
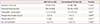
There were no conversions to laparotomy in either group. In the SPA-TLH and conventional TLH groups, the total operation time (median [range], 137 [63-313] vs. 122 [80-298] min; P=0.233), estimated blood loss (median [range], 100 [10-800] vs. 100 [25-1,000] mL; P=0.717), postoperative hemoglobin change (median [range], 1.2 [-1.0-2.9] vs. 1.0 [-2.5-5.3] g/dL; P=0.641), and number of pain control medications (median [range], 6 [2-17] vs. 8 [0-12]; P=0.283) were not significantly different between the two groups. Transfusion was performed in four SPA-TLH and two conventional TLH patients before surgery due to severe anemia. Blood transfusion after surgery was performed in one SPA-TLH and three conventional TLH patients. The SPA-TLH group had a significantly shorter hospital stay than that of the conventional TLH group (median [range], 3 [2-6] vs. 4 [3-7] days; P=0.003) (Table 2).
As shown in Table 3, there was no significant difference in pain score between SPA-TLH and conventional TLH at 6 hours (median [range], 4 [2-7] vs. 4 [3-10]; P=0.368), 24 hours (median [range], 3 [2-6] vs. 3 [2-6]; P=0.621), and 72 hours (median [range], 2 [0-3] vs. 2 [0-4]; P=0.512) after surgery. There was one complication in each group. In the SPA-TLH group, a woman, who had a previous appendectomy, had a huge uterus weighing 1,235 g and severe pelvic adhesions, including intestinal-peritoneal, omento-peritoneal, and utero-tubo-ovarian adhesions. After adhesiolysis, left ureteral thermal injury was suspected; therefore, a left ureteral stent indwelling was added after surgery. The ureteral stent was removed after 24 days, and there were no further complications. In the conventional TLH group, a woman who previously had an appendectomy had a slight tearing of the small bowel serosa during extraction of the huge uterus through the vagina. She was administered additional IV antibiotics during her hospital stay.
In gynecology, laparoscopic surgery has replaced laparotomy for most cases requiring hysterectomy [14]. Laparoscopy is accepted as a safe and efficient method because of reduced complications and faster recovery. Recently single-port laparoscopic surgery has become an alternative method for laparoscopy that further minimizes trauma. The single-port system has several advantages. It is easy to convert to the multi-port system if necessary, and the wound retractor prevents subcutaneous emphysema. In addition, small incisions produce better cosmetic effects [15].
There are some disadvantages to single-port laparoscopy, such as crowding of instruments in the umbilicus, limited numbers of available instruments for traction, and difficulty adding sutures. In addition, single-port procedures may take more time and effort for the surgeon to learn. Although SPA-TLH was feasible and had comparable perioperative outcomes to those of conventional TLH or LAVH, according to previous studies [10,13,16,17], SPA-TLH was the most common method for normal-sized or slightly enlarged uteri. Because there is limited access to the uterine vessels in large uteri because of the bulky uterine volume, there may be a higher risk of surgical complications, such as bleeding and ureteral and vascular injuries. Despite difficulty in performing single-port laparoscopy for a large uterus, studies of SPA laparoscopy have been reported for huge uteri. SPA-LAVH in uteri weighing more than 500 g was reported to be feasible and safe [9,18]. In 2013, Song et al. [12] published a prospective study of 11 cases of SPA-TLH in large uteri, and reported that SPA-TLH was feasible for large uteri. SPA-TLH has advantages over conventional TLH for large uteri. Large uteri can be safely moved to the medial side to create pelvic space, allowing ligation of uterine arteries; this can be done with a shaft of strong biopsy forceps instead of pooling or pushing with the tips of the forceps. In single-port laparoscopic surgery, the instrument for traction is used on the medial side of the uterus and not on the lateral side; thus, there is reduced risk of bleeding due to pulling or pushing the large uterus with a small instrument.
In our experience, the time to resect the uterus was not significantly different for a very large uterus compared to that required for a relatively small uterus in patients lacking pelvic adhesions. In LH, the larger the uterus, the longer it takes to retract the uterus from the pelvic cavity. In this study, there were some correlations between uterine weight and operation time in the SPA-TLH group, although this was not statistically significant (partial correlation coefficient adjusted by adhesion=0.277, P=0.191). There was also a tendency for pelvic adhesion to be correlated with operation time, although this was not statistically significant (partial correlation coefficient=0.309, P=0.141).
Lee et al. [11] reported a longer total operating time and greater decrease in postoperative hemoglobin and hematocrit in SPA-LH compared to conventional LH. In their study, the vaginal cuff was closed through the vagina. In contrast, we closed the vaginal vault through the laparoscope and found that the total operating time, estimated blood loss, and postoperative hemoglobin were not different between the two groups. In this study, there was one possible ureteral thermal injury in the SPA-TLH group in a patient with a huge uterus who had severe pelvic adhesions from a previous surgery. In this patient, the right ureter may have had a thermal injury during dissection; cystoscopy and RGP were performed, but no urinary leakage was found. We decided to insert a ureteral stent due to the possibility of ureteral thermal damage. After 24 days, the ureteral stent was removed, and the patient had no further complications. This complicated case (4%) in the SPA-TLH group was unusual. Thus, SPA-TLH appears feasible in selected patients who lack severe adhesions, even those with huge uteri.
Some studies report that SPA surgery produces less postoperative pain and faster recovery than those of the conventional method [19,20]. However, there was a study that reported no difference in postoperative pain [11,16]. In this study, there was no difference in post-operative pain score and the amount of pain killers. The postoperative pain can be determined by several factors such as abdominal incision size and numbers, type of pelvic surgery, and anesthesia. We believe that the skin incision numbers in multi-port access or single port access LH for huge uterus are not the main factor that determines postoperative pain. The pelvic operation itself may be the main cause of the postoperative pain rather than the skin incision. The SPA-TLH group showed shorter hospital stays than those of the conventional group; however, it was difficult to find sufficient detailed information regarding the patient's condition due to the retrospective nature of the study. One possible reason may be due to the surgeon's preferences regarding discharge.
This study had some limitations. Multiple surgeons were initially included in this study. Conventional TLH was performed by seven surgeons who had extensive experience in multi-port access laparoscopy hysterectomy, and SPA-TLH was performed by three surgeons who were well-trained in single-port surgery. The fact that all of the operations were not performed by a single surgeon is a potential limitation, although it does demonstrate the potential generalizability of our findings. In addition, the patients were retrospectively studied, which may introduce selection bias. Overall, this study showed that skillful surgeons can achieve comparable surgical outcomes with SPA-TLH and multi-port laparoscopy.
In conclusion, in a case of huge uterus weighing 500 g or more, SPA-TLH is a feasible method for hysterectomy when compared to conventional TLH in selected patients. Additional large-scale, randomized, controlled studies are important for further understanding the advantages of single-port laparoscopy in patients with huge uteri.
Figures and Tables
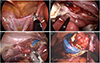
Fig. 1
Intraoperative findings in single-port access total laparoscopic hysterectomy. (A) Left utero-ovarian ligaments were ligated with the LigaSure system, as the uterus was pushed medially with a biopsy forceps containing a slightly bent steel shaft (arrow). (B) The uterus was medially pushed away with a biopsy forceps (arrow) to create a right pelvic space to dissect the right uterine artery (arrowhead). (C) The left uterine artery (arrowhead) was ligated with the LigaSure system. (D) The posterior vaginal wall was cut with a monopolar L-hook (M), as the uterus was lifted up with a biopsy forceps. M, monopolar; Ut, uterus.
References
1. Kongwattanakul K, Khampitak K. Comparison of laparoscopically assisted vaginal hysterectomy and abdominal hysterectomy: a randomized controlled trial. J Minim Invasive Gynecol. 2012; 19:89–94.
2. Bijen CB, Vermeulen KM, Mourits MJ, Arts HJ, Ter Brugge HG, van der Sijde R, et al. Cost effectiveness of laparoscopy versus laparotomy in early stage endometrial cancer: a randomized trial. Gynecol Oncol. 2011; 121:76–82.
3. Canes D, Desai MM, Aron M, Haber GP, Goel RK, Stein RJ, et al. Transumbilical single-port surgery: evolution and current status. Eur Urol. 2008; 54:1020–1029.
4. Kaouk JH, Haber GP, Goel RK, Desai MM, Aron M, Rackley RR, et al. Single-port laparoscopic surgery in urology: initial experience. Urology. 2008; 71:3–6.
5. Choi YS, Park JN, Oh YS, Sin KS, Choi J, Eun DS. Single-port vs. conventional multi-port access laparoscopy-assisted vaginal hysterectomy: comparison of surgical outcomes and complications. Eur J Obstet Gynecol Reprod Biol. 2013; 169:366–369.
6. Wheeless CR Jr. A rapid inexpensive, and effective method of surgical sterilization by laparoscopy. J Reprod Med. 1969; 3:65–69.
7. Thompson B, Wheeless RC. Outpatient sterilization by laparoscopy: a report of 666 patients. Obstet Gynecol. 1971; 38:912–915.
8. Pelosi MA, Pelosi MA 3rd. Laparoscopic hysterectomy with bilateral salpingo-oophorectomy using a single umbilical puncture. N J Med. 1991; 88:721–726.
9. Song T, Kim TJ, Kim MK, Park H, Kim JS, Lee YY, et al. Single port access laparoscopic-assisted vaginal hysterectomy for large uterus weighing exceeding 500 grams: technique and initial report. J Minim Invasive Gynecol. 2010; 17:456–460.
10. Park SN, Hong GY, Kim HY, Kim BR, Lee C. A comparison of single-port laparoscopically assisted vaginal hysterectomy using transumbilical SILS port access and three-port laparoscopically assisted vaginal hysterectomy. Korean J Obstet Gynecol. 2012; 55:22–28.
11. Lee GW, Kim JK, Shin CS, Choi WK, Kang BH, Yang JB, et al. Single port access laparoscopic hysterectomy for large uterus of more than 500 g. Korean J Obstet Gynecol. 2012; 55:392–397.
12. Song T, Lee Y, Kim ML, Yoon BS, Joo WD, Seong SJ, et al. Single-port access total laparoscopic hysterectomy for large uterus. Gynecol Obstet Invest. 2013; 75:16–20.
13. Yim GW, Jung YW, Paek J, Lee SH, Kwon HY, Nam EJ, et al. Transumbilical single-port access versus conventional total laparoscopic hysterectomy: surgical outcomes. Am J Obstet Gynecol. 2010; 203:26.e1–26.e6.
14. Ribeiro SC, Ribeiro RM, Santos NC, Pinotti JA. A randomized study of total abdominal, vaginal and laparoscopic hysterectomy. Int J Gynaecol Obstet. 2003; 83:37–43.
15. Tai HC, Lin CD, Wu CC, Tsai YC, Yang SS. Homemade transumbilical port: an alternative access for laparoendoscopic single-site surgery (LESS). Surg Endosc. 2010; 24:705–708.
16. Jung YW, Lee M, Yim GW, Lee SH, Paek JH, Kwon HY, et al. A randomized prospective study of single-port and four-port approaches for hysterectomy in terms of postoperative pain. Surg Endosc. 2011; 25:2462–2469.
17. Lee JH, Choi JS, Jeon SW, Son CE, Hong JH, Bae JW. A prospective comparison of single-port laparoscopically assisted vaginal hysterectomy using transumbilical GelPort access and multiport laparoscopically assisted vaginal hysterectomy. Eur J Obstet Gynecol Reprod Biol. 2011; 158:294–297.
18. Choi YS, Shin KS, Choi J, Park JN, Oh YS, Rhee TE. Single-port access laparoscopy-assisted vaginal hysterectomy: our initial experiences with 100 cases. Minim Invasive Surg. 2012; 2012:543627.
19. Chen YJ, Wang PH, Ocampo EJ, Twu NF, Yen MS, Chao KC. Single-port compared with conventional laparoscopic-assisted vaginal hysterectomy: a randomized controlled trial. Obstet Gynecol. 2011; 117:906–912.
20. Yoon A, Kim TJ, Lee WS, Kim BG, Bae DS. Single-port access laparoscopic staging operation for a borderline ovarian tumor. J Gynecol Oncol. 2011; 22:127–130.




 PDF
PDF ePub
ePub Citation
Citation Print
Print





 XML Download
XML Download