Abstract
Although pathology reports of thyroid tissue in ovarian teratomas are abundant, benign teratomas of the thyroid are extremely rare in adolescents and adults. Therefore, their clinical characteristics are still not well characterized. We report a case of a 54-year-old woman with a growing mass in her neck. Left lobectomy of the thyroid revealed it to be a benign thyroid teratoma composed of tissues from all three germ layers. Preoperative evaluations included thyroid ultrasonography (US), ultrasound-guided fine needle aspiration cytology (FNAC), and computed tomography (CT) of the neck. A 4.7-cm, well defined, predominantly hypoechoic mass intermingled with hyperechoic internal lesions, was observed in the inferior portion of the left thyroid lobe with substernal extension on US. The posterior extent of the nodule was not visualized due to deep attenuation of the echo. US-guided FNAC failed to reveal any thyroid follicular cells, but suggested a benign cystic tumor. Neck CT hinted at the diagnosis of teratoma because the mass contained large amounts of fat, and the margin was well defined. Extrathyroidal extension and cervical lymphadenopathy were not seen. She underwent left thyroid lobectomy, and histologic examination confirmed benign thyroid teratoma. To the best of our knowledge, this is the first case report of benign thyroid teratoma in Korea.
Teratomas are germ cell tumors that are characterized by three germ layers: the ectoderm, mesoderm, and endoderm. Teratomas are usually diagnosed in unborn babies and infants, but rarely occur in adults [1-3]. This tumor normally arises inside the gonad, but it can also occur outside the gonad. About 40% of extragonadal teratomas originate from the sacrococcygeal region, followed by (not in order of incidence) the central nervous system, globe, pharynx, mediastinum, and retroperitoneum [4]. Head and neck teratomas account for 3% to 6% of all teratomas [5].
Thyroid tissue is occasionally found in extrathyroidal teratomas [6], but a thyroid teratoma is a very rare form of germ cell tumor. Only a single case of malignant teratoma of the thyroid that included primitive neuroectodermal tissue has been published in the local literature [7]. Teratomas that occur in unborn babies and infants are mostly benign, but can be malignant in adults [2,3,8]. Benign thyroid teratoma is very rare in adults, and its associated clinical characteristics are not well understood [9]. Here the authors diagnosed a benign teratoma of the thyroid through a lobectomy in a patient with a cervical mass. We present the clinical outcome and diagnostic imaging findings, along with a review of the literature. It is the first case, to our knowledge, of a benign thyroid teratoma in South Korea.
A thyroid mass was detected by ultrasound during a routine medical check-up 4 years ago. Since then her doctor took a wait and see approach. However, the mass became larger. She had a repeat thyroid ultrasound examination, which revealed that the mass had extended substernally, and she was subsequently transferred to our hospital.
She underwent a laparoscopic hysterectomy for the treatment of a uterine myoma 7 years ago. There was no medical history of diseases, particularly thyroid-associated diseases, in her family. She had no drinking and smoking history.
She had a blood pressure of 132/65 mm Hg, pulse of 59 beats per minute, respiration rate of 20 breaths per minute, and temperature of 36.0℃. She was conscious without acute distress. A solid and fixed mass was identified on the left side of the neck, but the cervical lymph nodes were not affected.
Complete blood count revealed a white blood cell count of 8,300/mm3, hemoglobin of 12.8 g/dL, hematocrit of 36.7%, and platelet count of 18,100/mm3. Biochemical examination of serum revealed blood urea nitrogen/creatinine of 13.2/0.4 mg/dL, total protein/albumin of 6.5/4.0 g/dL, aspartate aminotransferase/alanine aminotransferase of 22/16 IU/L, alkaline phophatase of 68 IU/L, and Ca of 8.2 mEq/L. Measurement of electrolytes showed Na/K of 143/3.6 mEq/L.
Thyroid hormone tests revealed thyroid stimulation hormone of 1.88 µIU/mL (normal range, 0.4 to 4.8), free thyroxine of 1.48 ng/dL (normal range, 0.8 to 1.71), and triiodothyronine (T3) of 1.44 ng/mL (normal range, 0.6 to 1.6), showing normal thyroid function. Results of antithyroid peroxidase antibody and antithyroglobulin antibody tests were negative.
Thyroid ultrasonography (US) revealed a hypoechoic and heterogeneous nodule measuring 4.7 cm in diameter, with substernal extension of the inferior portion of the left thyroid lobe. Hyperechoic internal lesions were also observed (Fig. 1). The posteriosr boundary of the nodule was not clearly visualized due to deep attenuation of ultrasound. Ultrasound-guided fine needle aspiration cytology (FNAC) was performed. Based on the cytological examination, thyroid follicular cells were not detected, but cystic liquid was mainly observed, leading to a suspicion of cystic tumor. Computed tomography (CT) scan, which was performed to evaluate the mass due to its substernal extension, exhibited a mass (6.1×5.0×3.6 cm in size) that extended from the left thyroid lobe to the anterior mediastinum, with irregular enhancement, and clear margins that contained fat (Fig. 2). The mass caused deviation of the airway to the right, but there was neither a change in shape nor adhesion. Abnormal enlargement of lymph nodes was not observed in the neck.
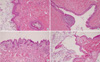
Results of FNAC and CT scan of the neck revealed a low possibility for a malignant tumor. However, the large size of the mass was concerning, and a lobectomy was performed to remove the left lobe. In histological examination, the removed mass was soft, but extended to the anterior mediastinum from the left thyroid lobe. The cut surface was dark yellow. There were multiple cystic masses, which were encapsulated in a wall of fibrotic capsule (Fig. 3). A microscopic examination revealed cystoma multiplex in which pilosebaceous structures, ciliated respiratory epithelium, intestinal columnar epithelium with goblet cells, and muscular structures were mixed (Fig. 4). Since there was no infiltration into surrounding tissues, benign thyroid teratoma was diagnosed. The patient is currently taking 50 µg of levothyroxine daily and attending outpatient clinic.
Cervical teratomas are divided into thyroid teratomas and extrathyroid teratomas depending on where they originated [10]. Although diagnostic criteria for thyroid teratomas still stir controversy among researchers, thyroid teratomas must meet at least one of the following criteria: 1) the tumor occupies part of the thyroid, 2) the tumor is located in direct continuity with the thyroid, or 3) the thyroid is not completely developed, but teratoma exists in the neck [3,11]. In this report, the mass met two criteria by occupying part of the thyroid and being located in direct continuity with the thyroid. Besides, the mass was comprised of all three germ layers identified with histological evidence [3,11]. As there was no infiltration into surrounding tissues, or metastasis to lymph nodes, the possibility of a malignant teratoma was ruled out. Benign thyroid teratoma in adults is a very rare tumor that is composed of solid and cystic portions. This tumor can grow fast in adolescents and young adults [5,12,13].
Many case reports have discussed thyroid cancer, thyroiditis, and other thyroid disorders, which originate from struma ovarii that contains thyroid tissue [6]. This is the first case of benign thyroid teratoma in South Korea. Kim et al. [7] reported a case of malignant thyroid teratoma that included primitive neuroectodermal tissue. In that case, the infiltration into extrathyroid soft tissue and metastasis of lymph nodes was evident even during diagnosis. Radical neck dissection on both sides was combined with strong chemotherapy for treatment [7].
In US, hypoechogenicity, spiculated margin, microcalcification, and taller than wide shape are considered specific features that increase the risk for thyroid cancer. Particularly, a hypoechoic mass is an important ultrasound finding with a sensitivity of 41%, and specificity of 92% [14]. In this case, the boundary between the thyroid tissue and the mass was clear and the nodule appeared hypoechoic, but hyperechoic internal lesions were observed within the nodule making it difficult to differentiate malignant tumor from benign tumor in US. The posterior boundary of the nodule was not clearly visualized due to excessive attenuation of ultrasound in the nodule. It was said that an ovarian teratoma with fatty tissue and hair results in hyperechoic and excessive ultrasound attenuation [15]. It appears that the same ultrasonic features were induced by fatty tissue in this case. Schmitz et al. [16] reported mixed hyperechoic, hypoechoic, and nonechoic lesions as characteristics of teratoma in ultrasonic evaluation. However, they also added that teratoma-specific ultrasonic features are not clear.
CT scan is known to be more effective than ultrasound in diagnosing teratoma that occurs in the mediastinum or retroperitoneum [17,18]. In this case, a CT scan of the neck exhibited a benign tumor containing inhomogenously enhancing cystic portions, with a clear margin that extended to the anterior mediastinum from the left thyroid lobe without invasion into lymph nodes or surrounding tissue, and with fatty components suggesting the diagnosis of a teratoma. Mediatinal teratoma can be diagnosed with the presence of a cystoma in a thick wall with fatty tissue and calcification [19].
When thyroid teratoma is suspected, the differential diagnosis should include lymphoid hyperplasia, lymphoma, cystic hygroma, and thyroglossal duct cyst. If fatty components or calcifications are not found in imaging tests, further aggressive testing should be performed to differentiate malignant disease [3]. In this case, although CT scan and FNAC indicated a benign tumor, the possibility of malignant tumor was not completely ruled out. A lobectomy was performed for further analysis and treatment, and a benign teratoma was diagnosed based on histological evidence.
Thyroid teratoma is a rare form of benign tumor that can cause airway compression and adverse symptoms, depending on site and size of the lesion. The tumor may arise in conjunction with malformation of the neck. The likelihood of a malignant thyroid teratoma is high in adults. Diagnostic imaging tests are not enough to differentiate malignant tumors from benign tumors, so a surgical resection is required for diagnosis and treatment [5,7].
In summary, this case had a rather large mass with a clear boundary showing a combination of hypoechoic and hyperechoic lesions. The posterior boundary of the nodule was not clearly visualized due to excessive ultrasound attenuation. CT scan of the neck exhibited fatty tissue, and thyroid teratoma was suspected before surgery. After lobectomy, a benign teratoma was diagnosed. Since the possibility of a malignant thyroid teratoma is high in adults, a final diagnosis needs to be made with surgical resection in doubtful cases.
Figures and Tables
Fig. 1
(A) Transverse and (B) longitudinal ultrasonographic scans show the well defined, heterogeneously hypoechoic nodule, intermingled with hyperechoic foci in the lower portion of left thyroid lobe (arrowheads).
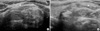
Fig. 2
Computed tomography scans of the neck show (A) a heterogeneous enhancing mass (arrowhead) in the left lobe of the thyroid, and (B) a large cystic fat-containing mass extending into the mediastinum (arrowhead).

References
1. Oka K, Okane M, Okuno S, Kawasaki T, Yonekawa N, Okano M, Nakayama M. Congenital cervical immature teratoma arising in the left lobe of the thyroid gland. APMIS. 2007. 115:75–79.
2. Djalilian HR, Linzie B, Maisel RH. Malignant teratoma of the thyroid: review of literature and report of a case. Am J Otolaryngol. 2000. 21:112–115.
3. Thompson LD, Rosai J, Heffess CS. Primary thyroid teratomas: a clinicopathologic study of 30 cases. Cancer. 2000. 88:1149–1158.
4. Lack EE. Extragonadal germ cell tumors of the head and neck region: review of 16 cases. Hum Pathol. 1985. 16:56–64.
5. Nishihara E, Miyauchi A, Hirokawa M, Kudo T, Ohye H, Ito M, Kubota S, Fukata S, Amino N, Kuma K. Benign thyroid teratomas manifest painful cystic and solid composite nodules: three case reports and a review of the literature. Endocrine. 2006. 30:231–236.
6. Kim SM, Choi BK, Kang JH, Kim MR, Jeon YK, Kim SS, Kim BH, Kim IJ. A case of bilateral struma ovarii combined with subclinical hyperthyroidism. Endocrinol Metab. 2012. 27:72–76.
7. Kim E, Bae TS, Kwon Y, Kim TH, Chung KW, Kim SW, Ro J, Lee ES. Primary malignant teratoma with a primitive neuroectodermal tumor component in thyroid gland: a case report. J Korean Med Sci. 2007. 22:568–571.
8. Riedlinger WF, Lack EE, Robson CD, Rahbar R, Nose V. Primary thyroid teratomas in children: a report of 11 cases with a proposal of criteria for their diagnosis. Am J Surg Pathol. 2005. 29:700–706.
9. Chen JS, Lai GM, Hsueh S. Malignant thyroid teratoma of an adult: a long-term survival after chemotherapy. Am J Clin Oncol. 1998. 21:212–214.
10. Rothschild MA, Catalano P, Urken M, Brandwein M, Som P, Norton K, Biller HF. Evaluation and management of congenital cervical teratoma. Case report and review. Arch Otolaryngol Head Neck Surg. 1994. 120:444–448.
11. Kimler SC, Muth WF. Primary malignant teratoma of the thyroid: case report and literature review of cervical teratomas in adults. Cancer. 1978. 42:311–317.
12. Partlow WF, Taybi H. Teratomas in infants and children. Am J Roentgenol Radium Ther Nucl Med. 1971. 112:155–166.
13. Meuwly JY, Lepori D, Theumann N, Schnyder P, Etechami G, Hohlfeld J, Gudinchet F. Multimodality imaging evaluation of the pediatric neck: techniques and spectrum of findings. Radiographics. 2005. 25:931–948.
14. Henrichsen TL, Reading CC. Thyroid ultrasonography. Part 2: nodules. Radiol Clin North Am. 2011. 49:417–424.
15. Sheth S, Fishman EK, Buck JL, Hamper UM, Sanders RC. The variable sonographic appearances of ovarian teratomas: correlation with CT. AJR Am J Roentgenol. 1988. 151:331–334.
16. Schmitz H, Spelsberg F, Hefele-Roedel B, Meister P. Ultrasound diagnosis of benign teratoma of the thyroid gland. Bildgebung. 1990. 57:93–95.
17. Davidson AJ, Hartman DS, Goldman SM. Mature teratoma of the retroperitoneum: radiologic, pathologic, and clinical correlation. Radiology. 1989. 172:421–425.
18. Moeller KH, Rosado-de-Christenson ML, Templeton PA. Mediastinal mature teratoma: imaging features. AJR Am J Roentgenol. 1997. 169:985–990.
19. Fulcher AS, Proto AV, Jolles H. Cystic teratoma of the mediastinum: demonstration of fat/fluid level. AJR Am J Roentgenol. 1990. 154:259–260.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download