Dear Editor:
A 19-year-old male patient presented with one-month history of progressive whitening of his toenails. The nail change began with central white spots on the toenails that progressed over one month to almost total nail whitening. The growth of the nails was otherwise normal. He was healthy and without a previous medical history. He had not experienced any exposure to medications, chemicals, or mechanical trauma to the nails. There was no family history of leukonychia or other dermatologic diseases.
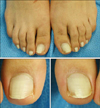
On physical examination, partial to total leukonychia of all toenails was observed. The right great toenail exhibited a totally chalky white discoloration. However, the distal portion of the other toenails had a pink transverse band about 2 or 3 mm wide at the free edge (Fig. 1). The surface of the nail did not demonstrable further change, such as pitting, ridging, or subungual hyperkeratosis. Otherwise, all fingernails were normal and the patient had no other organ abnormalities.
The results of the laboratory studies, including complete blood count, blood chemistry profile, and urinalysis, were all within normal limits. Repeated potassium hydroxide preparations and fungal cultures of the toenails were negative.
Punch biopsy was performed at the proximal nail fold of his left great toenail. Histopathologic examination of the nail plate revealed sparse parakeratosis with globular collection of keratohyaline granules (Fig. 2). A biopsy specimen from the nail bed and nail matrix were unremarkable. During the 6-month follow-up period, the discoloration of the toenails did not significantly change.
Leukonychia is the most common chromatic abnormality of the nail. True leukonychia is an abnormality of the nail plate that originates in the matrix1. The mechanism of leukonychia is not clear. The nail plate normally consists of cornified cells that contain keratin. However in leukonychia, as a result of abnormal matrix keratinization, persistent parakeratosis, keratohyaline granules, and dissociation of keratin bundles are present. Disorganization of the keratin fibrils leads to the diffraction of visible light in the parakeratotic cells, resulting in a white nail, which prevents visualization of the underlying pink vascular bed2,3,4,5.
True leukonychia may be inherited or acquired. Inherited leukonychia can be an isolated condition or one of several inherited leukonychia syndromes2. If true leukonychia is acquired, it may be associated with trauma, chemotherapeutic agents, hypocalcemia, zinc deficiency, heavy metal poisoning, local infection, and systemic diseases1,2,4,5.
Idiopathic acquired true leukonychia is a rare condition, with only six reported cases in the literature1,2,3,4,5. All of those cases as well as our case showed progression from leukonychia partialis to combined leukonychia totalis and partialis. All of previous reported cases involved the fingernails, and among these, four cases appeared at the fingernails and toenails. Our case is different from those reported cases; because of our case involved only the toenails without involvement of the fingernails.
In conclusion, true leukonychia can occur associated with trauma, drugs, infection, or systemic diseases. We thought that one of these must be the cause of development of true leukonychia, but we could not find any trauma history, systemic problem, or onychomycosis in our cases. Based on previous reports, we suggest that leukonychia might develop without underlying causes in some patients. This was a rare case with asymptomatic progressive idiopathic acquired true leukonychia totalis and partialis of the toenails without a hereditary cause.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download