Abstract
Background and Objectives
This study was designed to compare the nasalance between chronic rhinosinusitis (CRS) patients and normal controls and to determine the correlation of nasalance with nasal volume, nasal resistance, CT score, and polyp score in CRS patients.
Materials and Methods
This study enrolled 150 CRS patients and 154 normal adults. All subjects underwent acoustic rhinometry and rhinomanometry. Nasalance scores were measured with the nasometer. All CRS patients were graded according to the Lund-Mackay CT staging system and the degree of nasal polyp.
Results
Nasal volume was decreased and nasal resistance was increased in CRS patients compared with normal controls. However, the nasalance scores for oro-nasal and nasal passages were significantly higher in CRS patients compared with normal controls. In CRS patients, the nasalance score for the nasal passage showed positive correlation with nasal volume and negative correlation with nasal resistance and Lund-Mackay CT score. However, no significant correlation was found between nasalance score and endoscopic polyp score.
References
1). 김익태, 민양기, 양경헌. 비강 및 부비동의 생리. 민양기. 임상비과학. 1st ed.Seoul: 일조각;1997. p. 41–62.
2). Hosemann W, Göde U, Dunker JE, Eysholdt U. Influence of endoscopic sinus surgery on voice quality. Eur Arch Otorhinolaryngol. 1998; 255:499–503.

3). Gerek M, Durmaz A, Aydin U, Birkent H, Hidir Y, Tosun F. Relationship between nasal valve changes and nasalance of the voice. Otolaryngol Head Neck Surg. 2012; 147:98–101.

4). Williams RG, Eccles R, Hutchings H. The relationship between nasalance and nasal resistance to airflow. Acta Otolaryngol. 1990; 110:443–9.

5). Mora R, Jankowska B, Dellepiane M, Mora F, Crippa B, Salami A. Acoustic features of voice after septoplasty. Med Sci Monit. 2009; 15:CR269–73.
6). Havel M, Ertl L, Bauer D, Schuster M, Stelter K, Sundberg J. Res-onator properties of paranasal sinuses: preliminary results of an anatomical study. Rhinology. 2014; 52:178–82.

7). Soneghet R, Santos RP, Behlau M, Habermann W, Friedrich G, Stammberger H. Nasalance changes after functional endoscopic sinus surgery. J Voice. 2002; 16:392–7.

8). Dhong HJ, Kim SI, Kwon JK, Yun YS, Kang SM, Chu KC. Effects of endoscopic sinus surgery on nasality. Korean J Otolaryngol. 1999; 42:871–5.
9). Hong KH, Kwon SH, Jung SS. The assessment of nasality with a nasometer and sound spectrography in patients with nasal polyposis. Otolaryngol Head Neck Surg. 1997; 117:343–8.

10). Chen MY, Metson R. Effects of sinus surgery on speech. Arch Otolaryngol Head Neck Surg. 1997; 1213:845–52.

11). Jiang RS, Huang HT. Changes in nasal resonance after functional endoscopic sinus surgery. Am J Rhinol. 2006; 20:432–7.

12). Kim SD, Park HJ, Kim GH, Wang SG, Roh HJ, Cho KS. Changes and recovery of voice quality after sinonasal surgery. Eur Arch Otorhinolaryngol. 2015; 272:2853–9.

13). Kim YH, Lee SH, Park CW, Cho JH. Nasalance change after sinonasal surgery: analysis of voice after septoturbinoplasty and endoscopic sinus surgery. Am J Rhinol Allergy. 2013; 27:67–70.

15). Park MK, Lee EK, Yu SC, Koh KS, Kim BJ, Baek RM. Nasalance scores in normal Koreans. 65th American Cleft Palate-Craniofacial Association Annual Meetings. 2008 April 14. -18; Philadelphia, PA, USA.
16). Park M, Baek WS, Lee EK, Koh KS, Kim BK, Baek RM. Nasalance scores for normal Korean-speaking adults and children. J Plast Reconstr Aesthet Surg. 2014; 67:173–7.

17). Birkent H, Erol U, Ciyiltepe M, Eadie TL, Durmaz A, Tosun F. Relationship between nasal cavity volume changes and nasalance. J Laryngol Otol. 2009; 123:407–11.

18). Pegoraro-Krook MI, Dutka-Souza JCR, Williams WN, Teles Magal-haes LC, Rossetto PC, Riski JE. Effect of nasal decongestion on nasalance measures. Cleft Palate Craniofac J. 2006; 43:289–94.

19). Lund VJ, MacKay IS. Staging in rhinosinusitis. Rhinology. 1993; 31:183–4.
20). Johansen LV, Illum P, Kristensen S, Winther L, Petersen SV, Synner-stad B. The effect of budesonide (Rhinocort) in the treatment of small and medium-sized nasal polyps. Clin Otolaryngol. 1993; 18:524–7.

21). Abou-Elsaad T, Quriba A, Baz H, Elkassaby R. Standardization of nasometry for normal Egyptian Arabic speakers. Folia Phoniatr Logop. 2012; 64:271–7.

22). Awan SN, Bressmann T, Poburka B, Roy N, Sharp H, Watts C. Di-alectical effects on nasalance: a multicenter, cross-continental study. J Speech Lang Hear Res. 2015; 58:69–77.

23). Kim CS, Kong SK, Lee HS, Cho KS, Wang SG, Roh HJ. Analysis of changes in nasal formant, spectra and resonant volume in rhino-sinus after endoscopic sinus surgery. Korean J Otolaryngol. 2000; 43:1208–15.
Fig. 1.
Correlation between the total nasal cavity volume and the nasalance score for three passages in patients with chronic rhinosinusitis. A: Oral passage. B: Oro-nasal passage. C: Nasal passage.
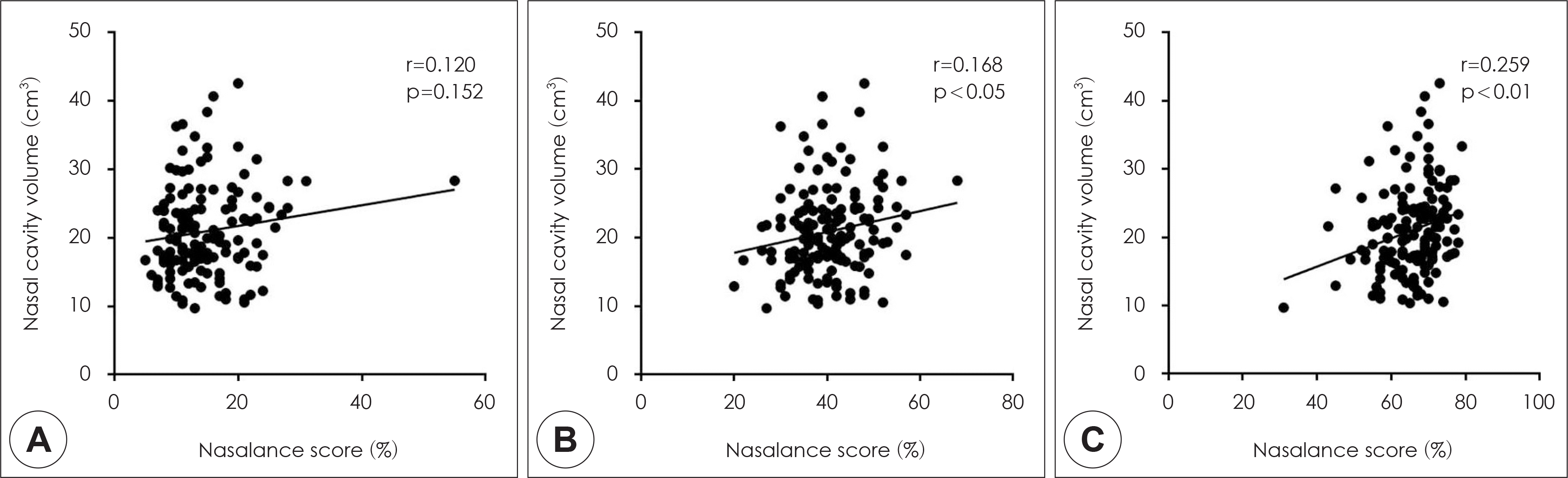
Fig. 2.
Correlation between the expiratory total nasal resistance and the nasalance score for three passages in patients with chronic rhinosinusitis. A: oral passage. B: Oro-nasal passage. C: Nasal passage.
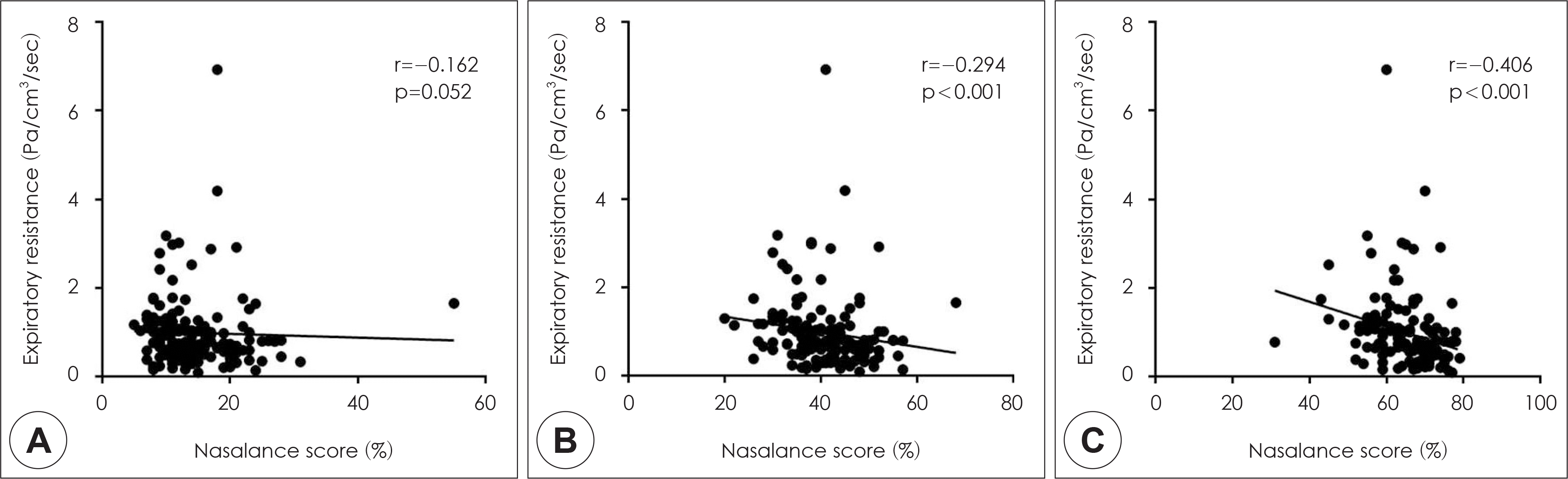
Fig. 3.
Correlation between the CT score and the nasalance score for three passages in patients with chronic rhinosinusitis. A: Oral passage. B: Oro-nasal passage. C: Nasal passage.
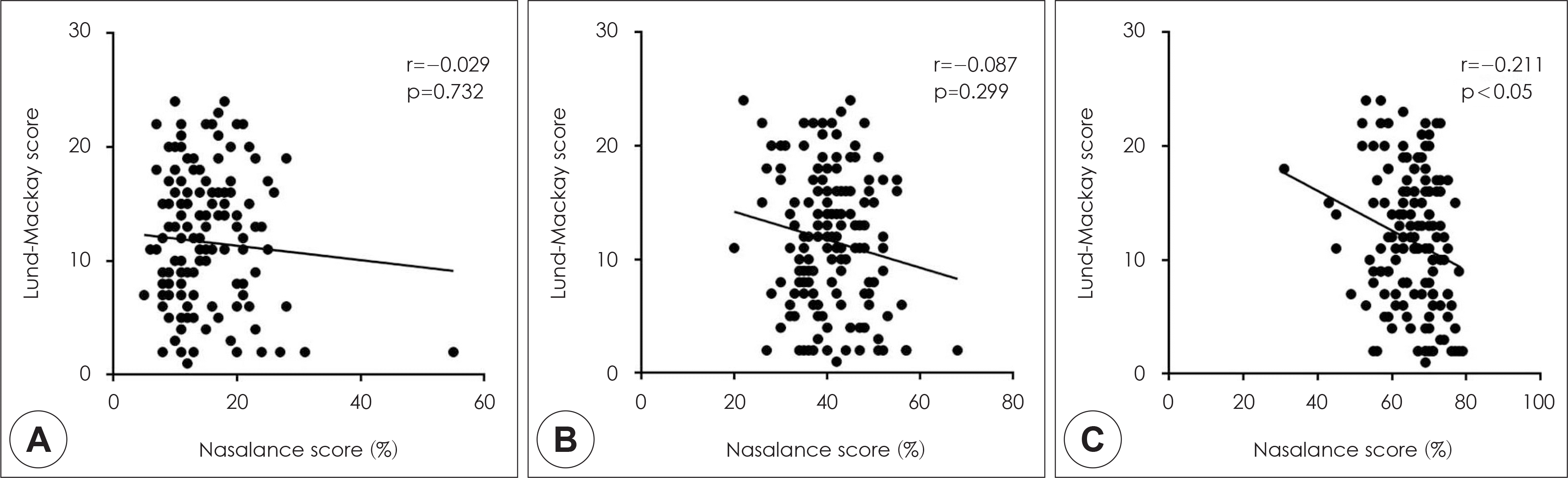
Fig. 4.
Correlation between the endoscopic polyp score and the nasalance score in patients with chronic rhinosinusitis. A: Oral passage. B: Oro-nasal passage. C: Nasal passage.
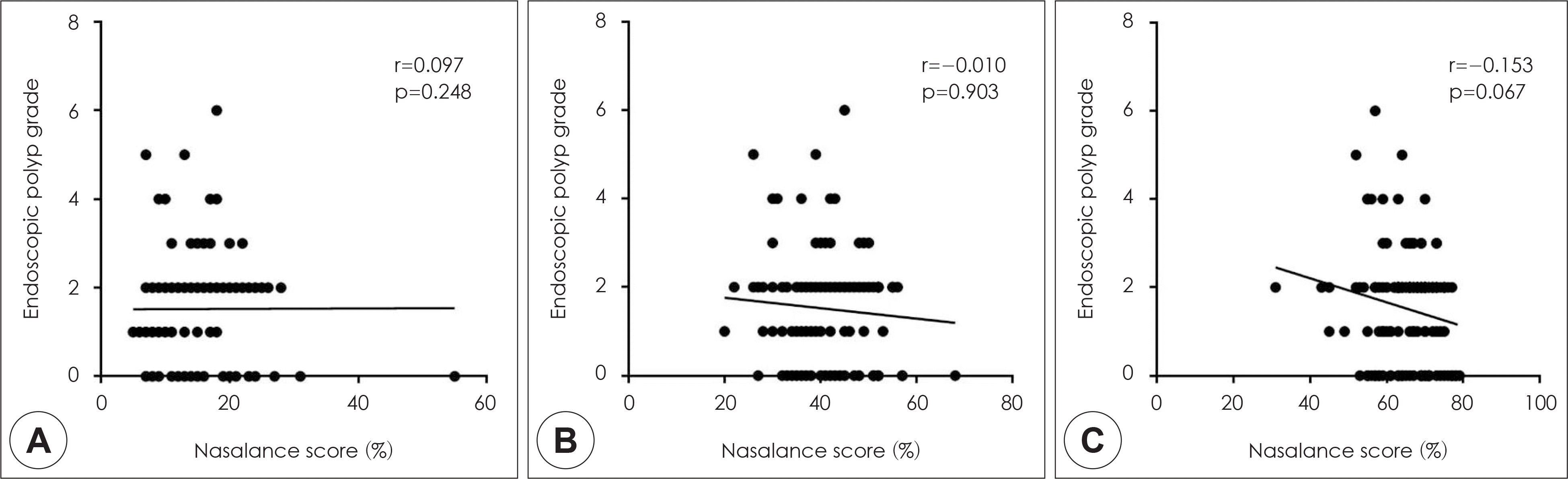
Fig. 5.
Comparison of the nasalance score between normal controls and patient groups classified according to the Lund-Mackay CT score. A: Oral passage. B: Oro-nasal passage. C: nasal passage. The lower and upper limits of the boxes represent the 25th and 75th percentiles, respectively. Horizontal bars represent the median values; whiskers represent the range. *: p<0.05, **: p<0.01, ***: p<0.001.
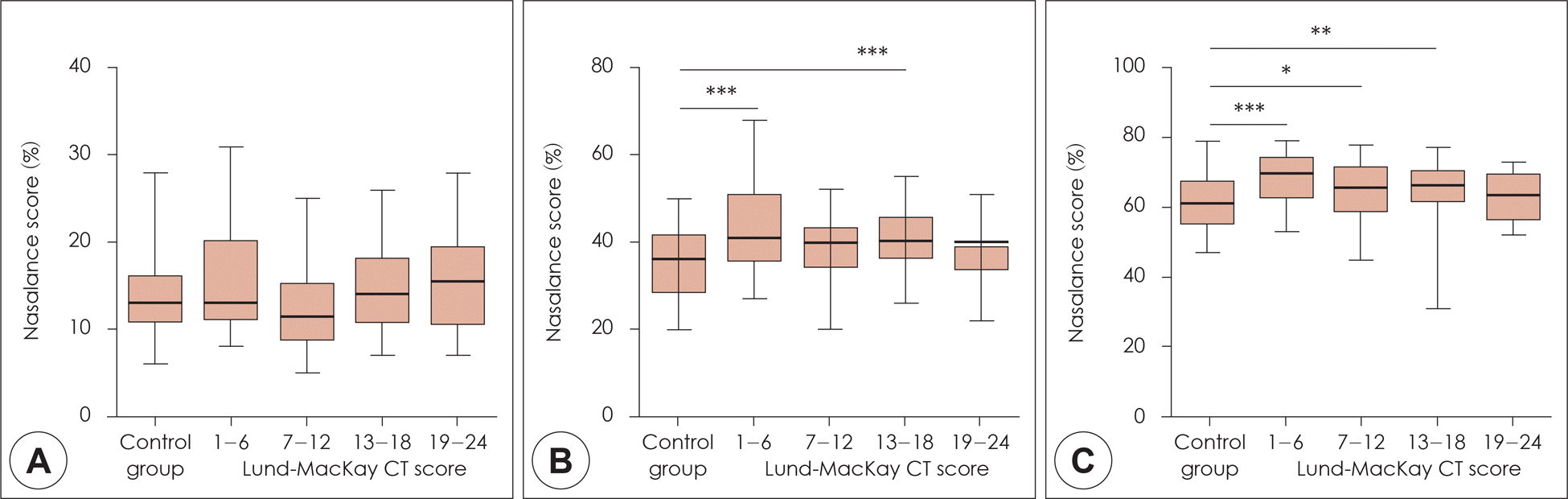
Fig. 6.
Comparison of the nasalance score between normal controls and patient groups classified according to the endoscopic polyp score. A: oral passage. B: oro-nasal passage. C: nasal passage. The lower and upper limits of the boxes represent the 25th and 75th percentiles, respectively. Horizontal bars represent the median values; whiskers represent the range. *: p<0.05, ***: p <0.001.
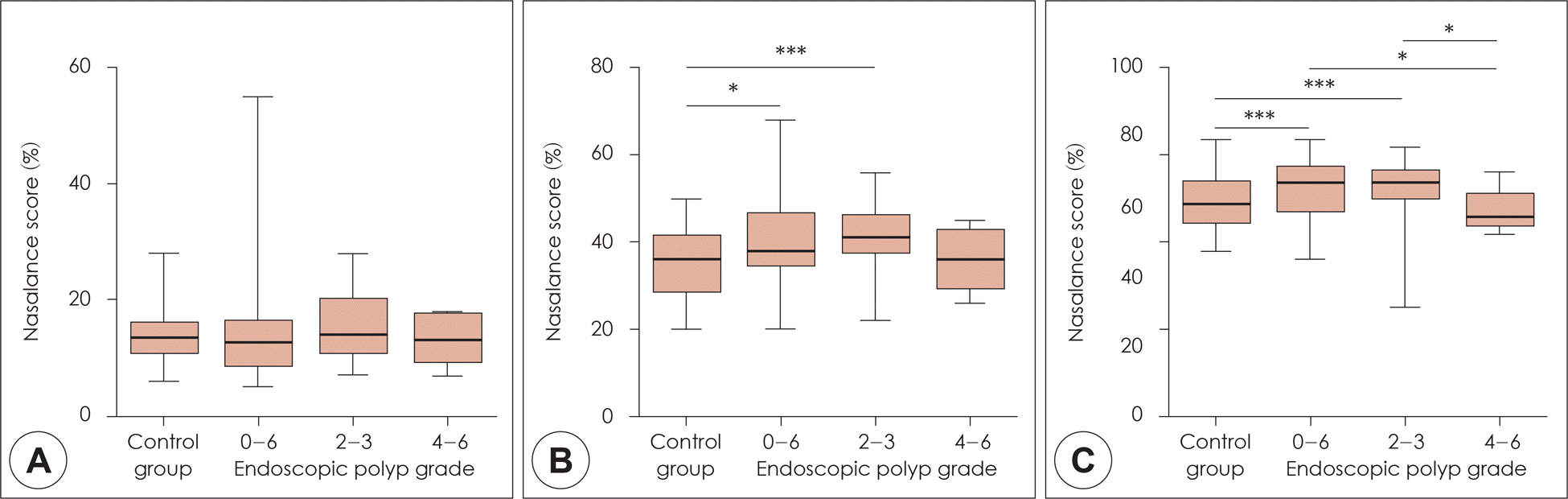
Table 1.
Korean passages used in nasometric test
Table 2.
Comparison of the mean values of nasal cavity volume, total nasal resistance and nasalance score between CRS patients group and normal controls
| Control group (n=154) | CRS group (n=150) | |
|---|---|---|
| Age | 45.02 (21–70) | 47.06 (20–79) |
| Sex (male/female) | 101/53 | 101/49 |
| Total nasal cavity volume (cm3) | 26.80±6.71 | 20.92±6.51* |
| Total nasal resistance (Pa/cm3/sec) | ||
| Inspiratory | 00.29±0.20 | 00.81±0.72* |
| Expiratory | 00.30±0.20 | 00.99±0.84* |
| Nasalance score (%) | ||
| Oral passage | 13.68±4.28 | 14.70±6.36* |
| Oro-nasal passage | 36.07±7.08 | 40.54±7.69* |
| Nasal passage | 60.98±7.11 | 65.25±7.73* |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download