Abstract
Purpose
This study was conducted to address a school-based program to properly manage atopic dermatitis in school children.
Methods
A modified Korean version of written questionnaires from the International Study of Asthma and Allergies in Childhood was completed by the parents of 125 first-grade children. Skin prick tests (SPTs) for nine common inhalants and food allergens were performed. Air cleaners, HEPA vacuum cleaners, wet blackboards, and wet towels were used to clean the floor in the classroom. Students and their parents participated in school-based educational programs about atopic dermatitis. A follow-up questionnaire and SPTs were performed at 6 months after improving the classroom conditions. Indoor air quality was measured at the 3 months interval in July and September of the same year after the school-based program.
Results
The prevalence of itchy eczema ever and a diagnosis of atopic dermatitis, within “” “the last 12 months was 26.4% and 12.0%, respectively. Eleven students (34.4%) showed positive” results among 32 students who were examined with SPTs. All children who showed positive results were sensitized with house dust mites. After the environmental change, the prevalence of itchy “eczema within the last 6 months and diagnosis of atopic dermatitis within the last 6 months was” “” 14.7% and 7.8%, respectively. Skin reactivity assessed by mean wheal diameter decreased. Measured indoor air quality values improved in all classrooms by September.
References
1. Hahn EL, Bacharier LB. The atopic march: the pattern of allergic disease development in childhood. Immunol Allergy Clin North Am. 2005; 25:231–46. v.

2. Spergel JM. Epidemiology of atopic dermatitis and atopic march in children. Immunol Allergy Clin North Am. 2010; 30:269–80.

3. Rhim JW, Moon KS, Kong DY, Pyun BY. An Investigation into the actual condition of outbreak and treatment in atopic dermatitis. Pediatr Allergy Respir Dis(Korea). 2005; 15:44–52.
4. Hong SJ, Ahn KM, Lee SY, Kim KE. The prevalences of asthma and allergic diseases in Korean children. Pediatr Allergy Respir Dis (Korea). 2008; 18:15–25.

5. Gupta MA, Gupta AK, Schork NJ, Ellis CN. Depression modulates pruritus perception: a study of pruritus in psoriasis, atopic dermatitis, and chronic idiopathic urticaria. Psychosom Med. 1994; 56:36–40.

6. Paller AS, McAlister RO, Doyle JJ, Jackson A. Perceptions of physicians and pediatric patients about atopic dermatitis, its impact, and its treatment. Clin Pediatr (Phila). 2002; 41:323–32.

7. Scheinmann P, Paty E, de Blic J. What environmental measures should be taken for the treatment of atopic dermatitis in children and the prevention of other atopic manifestations? Ann Dermatol Venereol. 2005; 132:Spec No 1:. 1S86–9.
8. Salo PM, Sever ML, Zeldin DC. Indoor allergens in school and day care environments. J Allergy Clin Immunol. 2009; 124:185–92. 192.e1–9.

9. Broberg A, Kalimo K, Lindblad B, Swanbeck G. Parental education in the treatment of childhood atopic eczema. Acta Derm Venereol. 1990; 70:495–9.
10. Melnyk BM, Alpert-Gillis L, Feinstein NF, Crean HF, Johnson J, Fairbanks E, et al. Creating opportunities for parent empowerment: program effects on the mental health/coping outcomes of critically ill young children and their mothers. Pediatrics. 2004; 113:e597–607.

11. Kunz B, Oranje AP, Labrèze L, Stalder JF, Ring J, Taïeb A. Clinical validation and guidelines for the SCORAD index: consensus report of the European Task Force on Atopic Dermatitis. Dermatology. 1997; 195:10–9.

12. Demoly P, Bousquet J, Romano A. In vivo methods for study of allergy. Adkinson NF, Holgate ST, Busse WW, Bochner BS, Lemanske Jr. RF, Adkinson Jr. NF, editors. editors.Middleton's Allergy: Principles and Practice. 7th Ed.Philadelphia: Mosby;2009. p. 1267–79.
13. Chamlin SL, Frieden IJ, Williams ML, Chren MM. Effects of atopic dermatitis on young American children and their families. Pediatrics. 2004; 114:607–11.

14. Lee SH, Yum HY. Complementary medicine of atopic dermatitis. Pediatr Allergy Respir Dis (Korea). 2008; 18:326–38.
15. Staab D, von Rueden U, Kehrt R, Erhart M, Wenninger K, Kamtsiuris P, et al. Evaluation of a parental training program for the management of childhood atopic dermatitis. Pediatr Allergy Immunol. 2002; 13:84–90.

16. Wenninger K, Kehrt R, von Rü den U, Lehmann C, Binder C, Wahn U, et al. Structured parent education in the management of childhood atopic dermatitis: the Berlin model. Patient Educ Couns. 2000; 40:253–61.

17. Holm EA, Esmann S, Jemec GB. Patient education and morbidity in atopic eczema. Dermatol Nurs. 2005; 17:35–46.
18. McKenna SP, Doward LC. Quality of life of children with atopic dermatitis and their families. Curr Opin Allergy Clin Immunol. 2008; 8:228–31.

19. Lewis-Jones MS, Finlay AY, Dykes PJ. The Infants' Dermatitis Quality of Life Index. Br J Dermatol. 2001; 144:104–10.

21. Sublett JL. The environment and risk factors for atopy. Curr Allergy Asthma Rep. 2005; 5:445–50.

22. Schmitt J, Apfelbacher C, Chen CM, Romanos M, Sausenthaler S, Koletzko S, et al. Infant-onset eczema in relation to mental health problems at age 10 years: results from a prospective birth cohort study (German Infant Nutrition Intervention plus). J Allergy Clin Immunol. 2010; 125:404–10.

23. Peters AS, Kellberger J, Vogelberg C, Dressel H, Windstetter D, Weinmayr G, et al. Prediction of the incidence, recurrence, and persistence of atopic dermatitis in adolescence: a prospective cohort study. J Allergy Clin Immunol. 2010; 126:590–5.e1–3.

24. Devereux G, Seaton A. Diet as a risk factor for atopy and asthma. J Allergy Clin Immunol. 2005; 115:1109–17.

25. Jung T, Stingl G. Atopic dermatitis: therapeutic concepts evolving from new pathophysiologic insights. J Allergy Clin Immunol. 2008; 122:1074–81.

26. McNally NJ, Williams HC, Phillips DR. Atopic eczema and the home environment. Br J Dermatol. 2001; 145:730–6.

27. Song S, Lee K, Lee YM, Lee JH, Lee SI, Yu SD, et al. Acute health effects of urban fine and ultrafine particles on children with atopic dermatitis. Environ Res. 2011; 111:394–9.

28. Cartieaux E, Rzepka MA, Cuny D. Indoor air quality in schools. Arch Pediatr. 2011; 18:789–96.
Fig. 1.
Modified International Study of Asthma and Allergies in Childhood written Questionnaires were conducted before (A) and 6 months after (B) school-based better management programs.
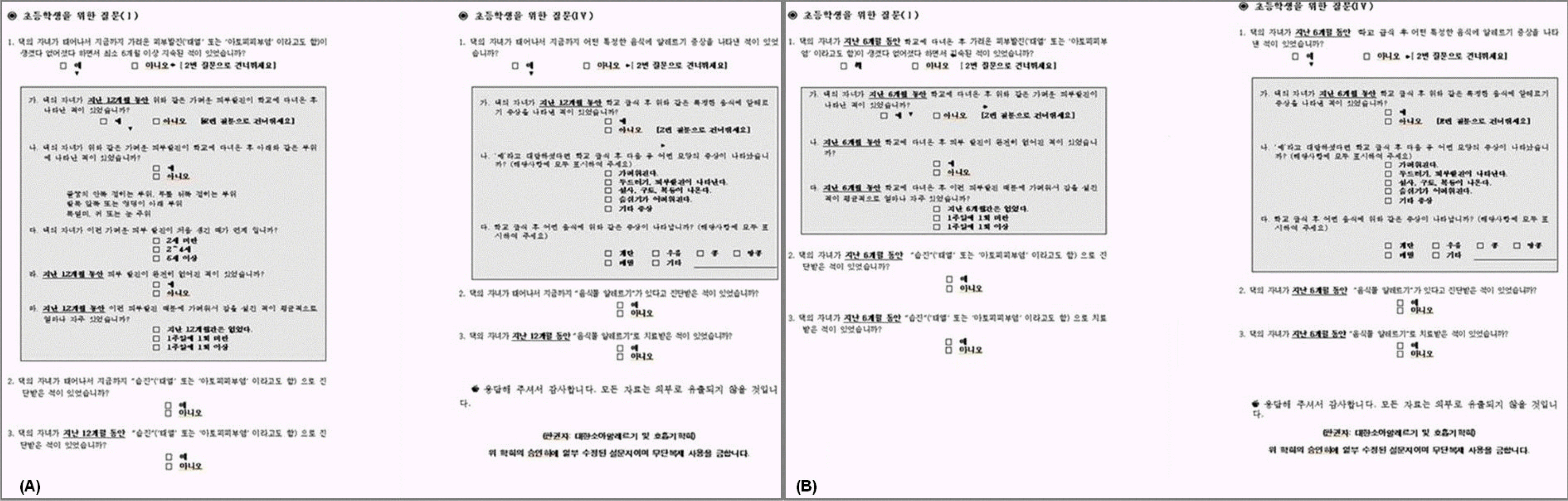
Fig. 2.
The results of skin prick tests. Number of sensitized allergens (A) and mean wheal diameter (B) in before and after the environmental change (P <0.05).
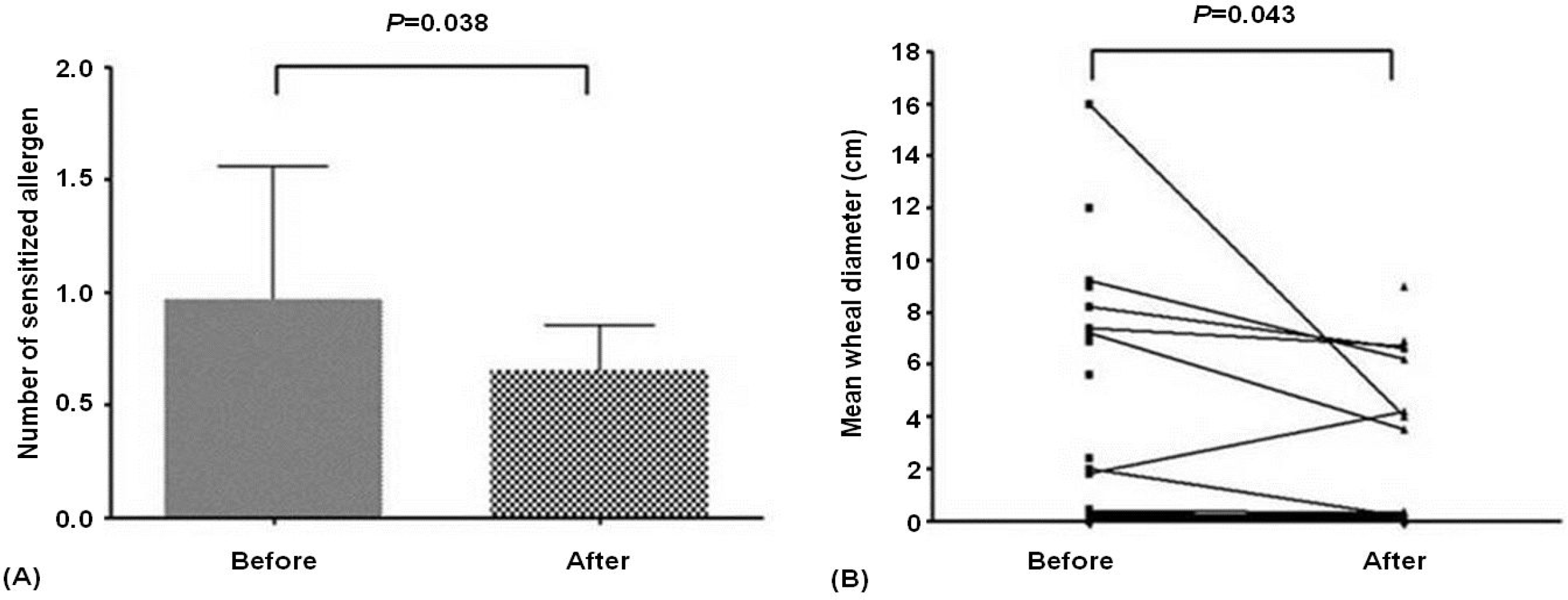
Table 1.
The Prevalence of Atopic Dermatitis in School Children Studied
Table 2.
Indoor Air Quality Measured after School-Based Program at July and September 2009 in School Classroom
| No | Classroom | Fine particulate 3) (g/m µ | CO (ppm) | CO2 (ppm) | HCHO (ppm) | Result | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| 150 ≤ ∗ | 25 ≤ ∗ | 1,000 ≤ ∗ | 0.096 ≤ ∗ | ||||||||
| 1st† | 2nd‡ | 1st† | 2nd‡ | 1st† | 2nd‡ | 1st† | 2nd‡ | 1st† | 2nd‡ | ||
| 1 | 1–1 | 112.7 | 25.0 | 0.1 | 0 | 574 | 500 | 0 | 0 | Normal | Normal |
| 2 | 2–1 | 398.0 | 35.0 | 0.6 | 0.8 | 2154 | 499 | 0.01 | 0 | Abnormal | Normal |
| 3 | 6–1 | 114.2 | 44.2 | 0.1 | 0.3 | 842 | 430 | 0.29 | 0.02 | Abnormal | Normal |
| 4 | 6–2 | 84.0 | 62.0 | 0 | 0 | 1,122 | 402 | 0 | 0 | Abnormal | Normal |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download