Abstract
Abnormally located liver tissue has been described in the vicinity of the liver proper, near anatomical structures such as the gallbladder, the umbilical fossa, the adrenal gland, the pancreas, and the spleen. Supradiaphragmatic ectopic liver is a rare finding, but has been reported to have been found in the intrathoracic cavity and in the pericardium. In the majority of supradiaphragmatic ectopic liver cases, there was an accompanying transdiaphragmatic pedicle of the main liver body into the abdominal cavity. In a minority of supradiaphramatic ectopic liver cases, the liver was completely separated from the abdominal cavity without a connection between the thorax and the abdomen, with accompanying diaphragmatic anomalies. We describe one case of intrathoracic ectopic liver in a patient with a previous history of lower chest wall trauma, and a brief review of the English-language medical literature on this topic.
Abnormally positioned liver tissue has been described commonly in the vicinity of liver proper such as the gallbladder, umbilical fossa, adrenal gland, pancreas and the spleen1,2. Supradiaphragmatic ectopic liver is a rare finding, which has been reported in the intrathoracic cavity and pericardium1-14. In a majority the supradiaphragmatic ectopic liver was accompanied by a transdiaphragmatic pedicle into the main body of liver in the abdominal cavity4-6,9-11. In other cases supradiaphramatic ectopic liver was completely separated from the abdominal cavity without a connection between the thorax and the abdomen, and diaphragmatic anomalies1,2,7. We describe one case of intrathoracic ectopic liver in a patient with previous history of trauma on the lower chest wall and a brief review of the English literature.
A 48-year-old woman was refered to our center due to a right supradiaphragmatic, pleural mass. Approximately 9 years ago, the patient had an injury on the right lower chest wall by car accident, and underwent closed thoracostomy. After the treatment in duration of about one week, the patient had no sequent problem. One month ago, the patient visited a local clinic due to cough and dyspnea. A computed tomography (CT) scan performed, which showed an oval well-enhancing mass in the mediastinal pleural side at the right lower lung zone, abutting the inferior portion of the right major fissure (Figure 1). On the clinical impression of benign fibrous tumor of the pleura or peripheral lung carcinoid tumor, the patient underwent a video-assisted thoracoscopic surgery. The operative field showed a 2 cm-sized oval mass based on the right hemidiaphragm close to the mediastinum, but the mass was not attached to the lung and liver (Figure 2A). Neither otherwise abnormal structure such as pedicle nor defect of the surrounding organs including the diaphragm and lung was identified. The mass was separated with easy by excision using electrocautery. The cut surface of the mass was homogenously solid and brown in color with well defined fibrous capsule (Figure 2B). Microscopically, the mass showed normal liver tissue consisting of polygonal hepatocytes without significant pathologic abnormality (Figure 2C).
Ectopic liver have been classified into four types by Collan et al.15. These consist of 1) an accessory lobe of the liver of considerable size and with a connecting stalk to the liver, 2) a small accessory lobe of the liver attached to the liver, 3) ectopic liver located without connection to the liver, and 4) microscopic ectopic liver tissue. Ectopic liver mostly occurs in the intraabdominal cavity as the first or second type, but rare cases of supradiaphragmatic ectopic were reported in the literature. The case we described herein belongs to the third of these categories.
A search of the medical literature worldwide disclosed 17 fully described cases of supradiaphragmatic heterotopic liver (Table 1). The first case was described in 1957 by Hansbrough and Lipin3. In all of the cases published so far, including our one, the age at initial diagnosis varied 26 weeks' gestational age to 63 years and male to female ratio was 1.43:1. The sizes of the lesion varied from 0.3 to 12 cm in the largest dimension. The adult patients usually showed no specific symptom. The most common symptoms in the pediatric patients were respiratory distress and chest pain. In one case, the patient presented with thoracic pain caused by an incomplete torsion of an intrathoracic ectopic liver lobe5.
Intrathoracic heterotopic liver usually is found incidentally in chest X-ray as a radiopaque mass14. Although, high-resolution CT is useful for evaluating intrathoracic masses, hetertopic liver cannot be diagnosed using imaging alone. In some cases, the patient was diagnosed as having tumor of pleura, diaphragm or mediastinum on preoperative CT5,6,12. Like these, accurate preoperative diagnosis of intrathoracic heterotopic liver is difficult due to its rarity. However, ultrasonography or CT-guided biopsy may be helpful to establish a correct diagnosis. In one case, supradiaphragmatic heterotopic liver was misdiagnosed as the pulmonary sequestration13. Color Doppler ultrasonography or angiography may show a feeding vessel and also contribute to differentiate pulmonary sequestrations from heterotopic liver10.
According to the literature, several possible mechanisms for development of heterotopic liver were proposed. In pediatric and young adult patients presenting supradiaphramatic liver with a connection such as a transdiaphragmatic pedicle into the liver proper and/or diaphragmatic hernia, the cause could be explained by anomaly in the development of diaphragm and liver bud4,6. Embryologically, the hepatic bud originating from the forgut grows into the mesenchyme of the septum transversum around the fourth week of gestation and then proliferates actively. At the approximately same time, the diaphragm develops centrally from the septum transversum and peripherally from the right and left pleuroperitoneal membranes. Normally the pleuroperitoneal cavity closes between the sixth and seventh week of gestation. A small portion of proliferating hepatic tissue may grow into the thoracic cavity before complete closure of the diaphragmatic membrane and the defect in fusion of the diaphragmatic membranes may allow the sequestration of hepatic tissue. As a result, supradiaphramatic liver could develop with atrophy or regression of the original connection to the abdominal liver2. Other possibility could be the development of an entirely separate liver bud independent of the main hepatic diverticulum without any prior connection2. This mechanism might explain the pathogenesis of the supradiaphragmatic liver without a pedicle into the liver proper.
Another explainable mechanism for minority of cases in the literature was related with previous trauma history. In two previously reported cases, heterotopic liver in the right thoracic cavity were detected following a trauma on the lower chest in patients who were 51 and 63 years old1,12. The heterotopic liver presented as a newly detected supradiaphramatic mass in both cases and were considered as acquired rather than congenital by the authors. According to one of these reports, the most plausible explanation was that during the previous trauma a fragment of liver parenchyma was introduced into the thoracic cavity, followed by through subsequent regeneration and development of a nodular mass1. This mechanism seems to be more possible in cases of middle-aged or old patients who had not represented any abnormality in the diaphragm and the liver in their childhood and young adulthood and underwent later traumatic injury on the lower chest or/and upper abdomen. The pathogenesis in our case can be also explained by the last proposed mechanism, and that a tiny fragment of liver parenchyme might be sequestered in to the right thoracic cavity during the injury by car accident in nine years ago.
In reviewing all reported cases of supradiaphragmatic heterotopic liver to date, the surgery has been straightforward with excellent prognosis. Heterotopic tissue, although extremely rare, should be taken in consideration into differential diagnosis of a supradiaphragmatic mass.
To the best of our knowledge, this is not only a rare case of supradiaphragmatic heterotopic liver, but also a third case of patient having this entity with a previous trauma history in English literature. We believe that awareness and understanding pathogenesis of this entity is helpful in preoperative evaluation and a correct intraoperative diagnosis of a supradiaphragmatic mass.
Figures and Tables
Figure 1
CT shows an oval well-enhancing mass in mediastinal pleural side at the right lower lung zone (arrows).
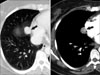
Figure 2
(A) The operative field shows a 2 cm-sized oval mass based on the right hemidiaphragm close to the mediastinum, but the mass is not attached to the lung and liver. (B) The mass have a well defined fibrous capsule (H&E stain, ×1). (C) Microscopically, the mass shows normal liver tissue consisting of polygonal hepatocytes without significant pathologic abnormality (H&E stain, ×40).

References
1. Lasser A, Wilson GL. Ectopic liver tissue mass in the thoracic cavity. Cancer. 1975. 36:1823–1826.
2. Mendoza A, Voland J, Wolf P, Benirschke K. Supradiaphragmatic liver in the lung. Arch Pathol Lab Med. 1986. 110:1085–1086.
3. Hansbrough ET, Lipin RJ. Intrathoracic accessory lobe of the liver. Ann Surg. 1957. 145:564–567.
4. Le Roux BT. Heterotopic mediastinal thyroid. Thorax. 1961. 16:192–196.
5. Sehdeva JS, Logan WD Jr. Heterotopic (supradiaphragmatic) liver. Ann Thorac Surg. 1971. 11:468–471.
6. Rendina EA, Venuta F, Pescarmona EO, Martelli M, Ricci C. Intrathoracic lobe of the liver: case report and review of the literature. Eur J Cardiothorac Surg. 1989. 3:75–78.
7. Shapiro JL, Metlay LA. Heterotopic supradiaphragmatic liver formation in association with congenital cardiac anomalies. Arch Pathol Lab Med. 1991. 115:238–240.
8. Kinnunen P, Kulmala P, Kaarteenaho-Wiik R, Vuopala K. Ectopic liver in the human pericardium. Histopathology. 1997. 30:277–279.
9. Iber T, Rintala R. Intrapulmonary ectopic liver. J Pediatr Surg. 1999. 34:1425–1426.
10. Babu R, Van der Avoirt A. Ectopic intrathoracic liver. Pediatr Surg Int. 2001. 17:461–462.
11. Luoma R, Raboei E. Supradiaphragmatic accessory liver: a rare cause of respiratory distress in a neonate. J Pediatr Surg. 2003. 38:1413–1414.
12. Huang CS, Hsu WH, Hsia CY. Supradiaphragmatic ectopic liver: delayed traumatic hepatic hernia mimics pulmonary tumor. Thorac Cardiovasc Surg. 2007. 55:277–278.
13. Choi SU, Kim HK, Kim J. Heterotopic supradiaphragmatic liver combined with intralobar pulmonary sequestration. Ann Thorac Surg. 2008. 85:1809–1810.
14. Hudson TR, Brown HN. Ectopic (supradiaphragmatic) liver. J Thorac Cardiovasc Surg. 1962. 43:552–555.
15. Collan Y, Hakkiluoto A, Hästbacka J. Ectopic liver. Ann Chir Gynaecol. 1978. 67:27–29.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download