Abstract
Isolated chylopericardium as a complication of cardiac surgery is very rare. Two cases of chylopericardium have been previously reported in Korea; both patients suffered from chylopericardium after a corrective cardiac surgery for a congenital heart disease such as atrial or ventricular septal defect. We report a case of chylopericardium in a 55-year-old mitral valve replacement patient. The reason for chylopericardium was unclear, but it might have been related with the damaged lymph nodes and blunt dissection of the thymus. While most chylopericardium cases require surgical intervention, we managed this chylopericardium case with a low-fat diet for 3 days.
Chylothorax is defined as leakage from the thoracic duct or one of the main lymphatic vessels that drain into thoracic cavity. The most common causes are lymphoma and trauma resulting from thoracic surgery.[1] If the patient is on a normal diet, the effusion can be identified by its white and milky appearance, as it contains high levels of triglycerides. This chyle composition of triglycerides is mostly in the form of chylomicron. Chylopericardium, however, especially after open heart surgery is very rare, and its causes are uncertain. We experienced a case of isolated chylopericardium after mitral valve replacement for adult patient, and reviewed previous worldwide reports.
A 55-year-old male presented with exacerbating dyspnea on exertion. An echocardiogram showed severe mitral valve regurgitation with flail anterior mitral valve leaflets and moderate tricuspid valve regurgitation with pulmonary hypertension. An electrocardiogram revealed atrial fibrillation with slow ventricular response. We performed a mitral valve replacement with mechanical valve, a tricuspid valve annuloplasty using Kay type, and a modified Cox-Maze procedure with radiofrequency ablation. The operation was uneventfully conducted with routine procedure such as median sternotomy, aortic cannulation on the distal ascending aorta, bicaval venous cannulation, infusion of antegrade cardioplegic solution into the aortic root, and so on. Cardiopulmonary bypass time was 150 minutes and cross-clamping time was 95 minutes.
The patient was weaned from mechanical ventilation 3 hours after the operation and achieved a sinus cardiac rhythm. There was no acute complication, and the patient was transferred to general ward at the next day. The amount of the pericardial tube drainage was unexpectedly increased relatively to the previous day (> 200 ml) 4 days after the operation. The drained pericardial effusion was yellow-gray colored and cloggy which findings were compatible with the chyle. Biochemical analysis and microscopic cell differentiation of the chylous fluid confirmed a chylopericardium; total cholesterol = 47 mg/dl, triglyceride = 699 mg/dl, lymphocyte = 95%.
We decided to prescribe low-fat diets because of the relatively small amount of the chyle. The color of the drained pericardial effusion was converted into serous color 2 days later. Then the pericardial tubes were removed after the drainage was under 120 ml/day. The patient was discharged 13 days after the operation, and followed-up for 3 months without any evidence of the chylopericardium. Fig. 1 shows clinical course by X-ray findings of the patient.
Isolated chylopericardium after open heart surgery is a rare entity and initially described by Thomas and McGoon[2] in 1971. Since then a few sporadic cases had been reported, and in 1986, the first case of chylopericardium following cardiac surgery was reported in Korea.[3] The patient was diagnosed as an atrial septal defect and underwent a patch closure with autologous pericardium. The other report in Korea described a case of chylopericardium after cardiac surgery for ventricular septal defect and patent ductus arteriosus.[4] While all the patients who have been reported previously were categorized in congenital heart disease, our case was adult heart disease.
The pathophysiology of isolated postoperative chylopericardium is still uncertain. Thomas and McGoon[2] suggested that thrombosis of the left subclavian vein resulting from an external jugular vein catheter could obstruct the thoracic duct flow leading to chylopericardium. Kim et al.[3] found severe stenosis of the innominate vein compressed by adhesive fibrous tissue. Additionally, other reports strengthen the suggestion for a causal relationship between the chylopericardium and the venous thrombosis.[5,6] Our patient had a left subclavian vein catheter, but had no signs of vein obstruction.
We assume that some mechanical injuries are related to the chylous leakage, such as traumatic dissection of the superior vena cava, too extensive T-shaped pericardiotomy to the right lower mediastinum, and rough division of the thymus. On the operative filed, we recognized there were a few enlarged lymph nodes on the patient’s thymus. A transparent fluid leaked out the lymph nodes when we divided the thymus lobe bilaterally. So we performed a mass ligation of the lymph nodes separately, and applied biologic glue on the ligated lymph nodes. We propose that the minimal delayed leakage might be aroused from the damaged lymph nodes. Similarly, Navaratnarajah et al.[7] reported a case of chylotamponade and chylothorax following radiofrequency Maze procedure using a bipolar device. They hypothesized that the Maze procedure could have resulted in iatrogenic injury to the thoracic duct having several anatomical variations.
Chylopericardium can be managed conservatively or surgically. Fluid and electorolyte replacement with intravenous parenteral nutrition or a low-fat with high medium-chain triglycerides diet can help to resolve the effusion.[4,8] Unfortunately, there have been more often cases failed by conservative measures for 2 to 4 weeks. The most reviewed patients needed surgical interventions such as redo sternotomy, ligation of the thoracic duct, formation of pericardial-peritoneal shunt, and creating a pericardial window. [3,5–7,9] In the case of Kim et al.[3], the patient was presented with dyspnea and facial edema one month after the patch closure for atrial septal defect. She was diagnosed with massive chylopericardium and underwent a pericardial resection and ligation of the soft tissues surrounding the innominate vein through a redo sternotomy after parenteral hyperalimentation for 3 weeks. She discharged with normal diet 10 days after the second operation.
Increasing amount of the pericardial effusion after cardiac operation would demonstrate a chylopericardium that is rare with uncertain pathophysiology. Conservative treatments including parenteral nutrition or a low-fat diets should proceed before surgical interventions. We report a case resolving the chylopericardium through low-fat diets for 3 days.
REFERENCES
1). Jeon JS, Ryu HG, Lee HN, Yoo DH. Chylopericardial tamponade in a patient with chylothorax after pulmonary lobectomy. Korean J Crit Care Med. 2013; 28:327–30.

2). Thomas CS Jr, McGoon DC. Isolated massive chylopericardium following cardiopulmonary bypass. J Thorac Cardiovasc Surg. 1971; 61:945–8.

3). Kim SH, Park KY, Park PW, Lee YK, Moon HS. One case of surgical treatment for chylopericardium following cardiac surgery. Korean J Thorac Cardiovasc Surg. 1986; 19:695–8.
4). Chung KY, Lee DY, Kim DK, Yoo KJ, Cho BK, Hong SN. Management of chylothorax and chylopericardium. Korean J Thorac Cardiovasc Surg. 1989; 22:731–8.
5). Rose DM, Colvin SB, Danilowicz D, Isom OW. Cardiac tamponade secondary to chylopericardium following cardiac surgery: case report and review of the literature. Ann Thorac Surg. 1982; 34:333–6.

6). Bakay C, Wijers TS. Treatment of cardiac tamponade due to isolated chylopericardium following open heart surgery. J Cardiovasc Surg. 1984; 25:249–51.
7). Navaratnarajah M, Raja SG. Chylothorax and chylopericardium following mitral and tricuspid valve repairs and radiofrequency maze procedure. J Card Surg. 2011; 26:279–81.

8). Bar-El Y, Smolinsky A, Yellin A. Chylopericardium as a complication of mitral valve replacement. Thorax. 1989; 44:74–5.

9). Mundra V, Savage EB, Novaro GM, Asher CR. Delayed chylous pericardial effusion after aortic valve replacement. Tex Heart Inst J. 2011; 38:431–2.
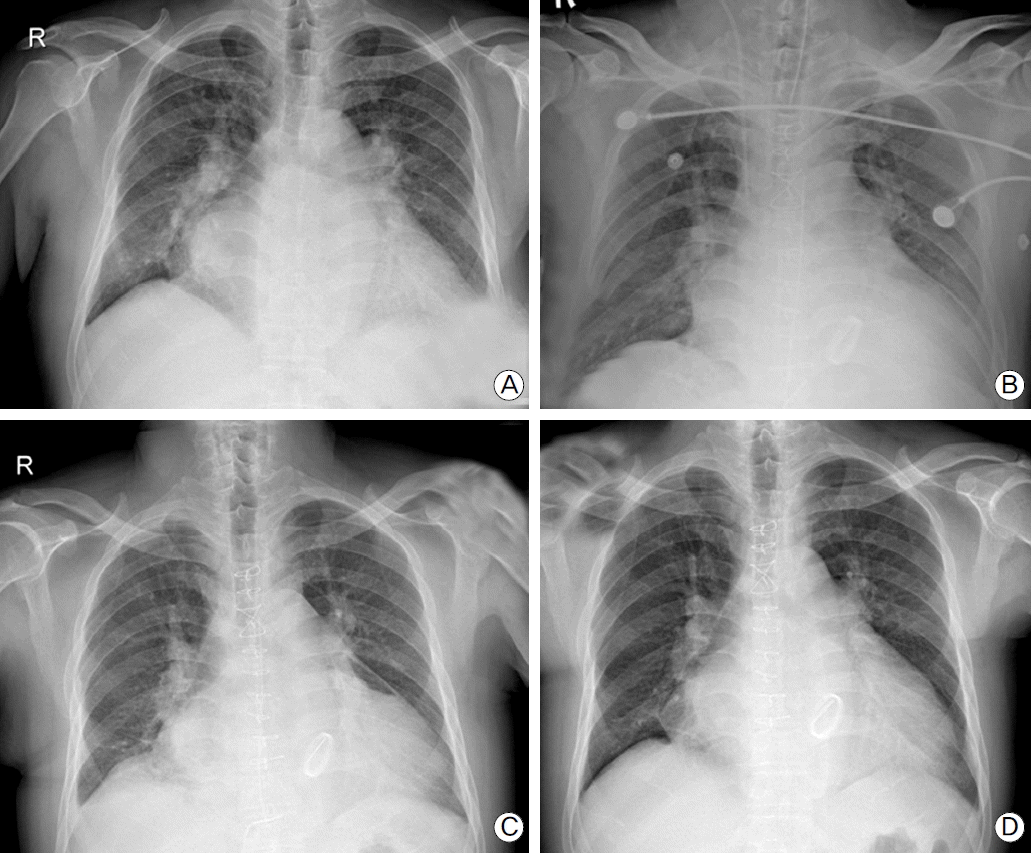
Fig. 1.
X-ray findings of the patient. The patient had a severe cardiomegaly with the enlarged left atrium preoperatively (A). The patient underwent uneventful mitral valve replacement and had a usual x-ray findings immediate postoperatively (B). We recognized chylopericardium and pneumopericarium resulting from drainage of the pericardial effusion 4 days after the operation (C). The patient has been free from the pericardial effusion for 3 months after discharge (D).




 PDF
PDF Citation
Citation Print
Print


 XML Download
XML Download