Abstract
Purpose
Materials and Methods
Results
Conclusions
Figures and Tables
Fig. 1
Cystometrograms with intravesical infusion of saline at 150 µL per minute in conscious rats. Voiding bladder contractions, micturition frequency and voided volumes are shown at 8- and 16-week bladder ischemia versus sham controls. Changes in intravesical pressure and micturition patterns consistent with bladder overactivity and changes resembling detrusor underactivity were evident in the 8- and 16-week ischemic bladders, respectively.

Fig. 2
Cystometrograms in anesthetized rats with constant intravesical volume of 0.8 mL without saline infusion. After 8-week ischemia, increased fluctuations in intravesical pressure similar to detrusor overactivity were present. After 16-week ischemia, the bladder tended to contract frequently but produced little changes in intravesical pressure, suggesting frequent contractile activities of reduced strength.

Fig. 3
Western blotting of muscarinic receptors in 8-week ischemic bladders versus sham. A significant increase in muscarinic M2 receptor expression was found after 8-week bladder ischemia compared with sham control. Both M1 and M3 expression showed a tendency to increase after 8 weeks ischemia but did not reach significance.
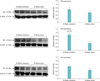
Fig. 4
Western blotting of muscarinic receptors in 16-week ischemic bladders versus sham. After 16-week bladder ischemia, in addition to M2 upregulation, a significant increase in M1 expression and significant decrease in M3 expression were found compared with corresponding sham controls.
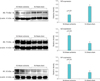
Fig. 5
Transmission electron microscopy of nerve bundles after 8- (C) and 16-week (D) bladder ischemia are shown versus corresponding sham controls (A and B, respectively). Disrupted axonal ultrastructures after 8-week bladder ischemia and swollen degenerating axons with considerable connective tissue proliferation around the nerve bundles are shown after 16-week bladder ischemia (×9,300).
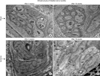
Fig. 6
Immunoreactive nerve fibers in the ischemic (C and D) and sham control (A and B) bladder tissues are shown at ×400 magnifications. Progressive decrease in neural density was evident with increasing duration of ischemia. The number of immunopositive nerves decreased after 8-week bladder ischemia but did not reach significance. After 16-week bladder ischemia, immunoreactive nerve fibers density significantly decreased versus sham control. Arrows point to immunopositive nerve fibers. SE, standard error.
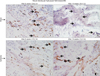
Table 1
Bladder blood flow, voiding patterns and conscious cystometric parameters after 8- and 16-week bladder ischemia

Values are presented as mean±standard error.
Hemodynamic measurements, metabolic cage data and conscious cystometric findings in 8- and 16-week bladder ischemia versus corresponding sham groups. At 8-week ischemia, bladder blood flow (BBF, mL/min/100-g tissue) was lower (p=0.003), micturition frequency (MF) per 24 hours was greater (p=0.043), and voided volume (VV) was smaller (p=0.035). BBF and MF decreased (p=0.002 and p=0.021, respectively) at 16-week ischemia. VV at 16-week ischemia was not significantly different versus 16-week sham (p=0.076). There was no significant difference in baseline bladder pressure (BP) and threshold pressure (TP) among the animals. Micturition pressure (MP) decreased after 16-week ischemia (p=0.025). Postvoid residual volume (RV) and bladder capacity (BC) increased at 16-week ischemia (p=0.008 and p=0.026, respectively).




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download