Abstract
Purpose
To introduce a modified technique of bicanalicular silicone tube intubation, which can reduce slitting of the canaliculus and protrusion of the tube.
Methods
This study included 46 patients who underwent modified surgery for Congenital Nasolacrimal Duct (CNLD) obstruction. To be included in this study, patients were older than 13 months and had a history of failed probing. Using our modified technique, tube lengths can be appropriately adjusted by either pulling or releasing the tube at the medial canthus until a tube loop is in place without any tension to the upper and lower canaliculi. Two threads of silicone tube were tied together using 5–0 nylon over a silicone sponge (5×5 mm) and left within the nasal cavity for several months without fixation to the nasal mucosa. A successful surgery was clinically defined as no epiphora and no dye retention in the conjunctival sac.
Results
The mean age of patients at the time of surgery was 32.8 (±18.9) months. There were 22 males and 24 females. Prior to intubation, patients had been probed an average of 1.5 (±1.3) times, and the mean follow-up period was 12.6 (±14.2) months. The tube was removed at 5.4 (±1.3) months postoperatively on average. The success rates were 88%. Tube protrusions occurred in three eyes, and canalicular splittings were recorded in two eyes. No other serious complications were encountered.
References
1. Cassady JV. Dacryocystitis in infancy. Am J Ophthalmol. 1948; 31:773–80.
2. Guerry D III, Kendig EL Jr. Congenital impotency in the nasolacrimal duct. Arch Ophthalmol. 1948; 39:193–204.
3. Chaabouni M, Zayani A, Chebini S, et al. Congenital obstruction of lacrimal ducts in 578 children. Arch Er Pediatr. 1993; 50:107–9.
4. Paul TO, Shepherd R. Congenital nasolacrimal duct obstruction: natural history and the timing of optimal intervention. J Pediatr Ophthalmol Strabismus. 1994; 31:362–7.

5. Lee SY, Chung HS, Kim HB, et al. The incidence of congenital nasolacrimal duct obstruction on Korean neonates. J Korean Ophthalmol Soc. 1989; 30:5–8.
7. Baker JD. Treatment of congenital nasolacrimal system obstruction. J Pediatr Ophthalmol Strabismus. 1985; 22:34–6.

8. Kassoff J, Meyer DR. Early office-based vs late hospital-based nasolacrimal duct probing: a clinical decision analysis. Arch Ophthalmol. 1995; 113:1168–71.
9. El-Mansoury J, Calhoun JH, Nelson LB, Harley RD. Results of late probing for congenital nasolacrimal duct obstruction. Ophthalmology. 1986; 93:1052–4.

10. Honavar SG, Prakash VE, Rao GN. Outcome of probing for congenital nasolacrimal duct obstruction in order children. Am J Ophthalmol. 2000; 130:42–8.
11. Katowitz JA, Welsh MG. Timing of initial probing and irrigation in congenital nasolacrimal duct obstruction. Ophthalmology. 1987; 94:698–705.

12. Sturrock SM, MacEwan CJ, Young JD. Long term results after probing for congenital nasolacrimal duct obstruction. Br J Ophthalmol. 1994; 78:892–4.
13. Ahn DH, Helen Lew, Kim HY, Lee SY. The effect of probing for congenital nasolacrimal duct obstruction. J Korean Ophthalmol Soc. 1998; 39:836–40.
14. Moon JS, Choi WC. Office probing of congenital nasolacrimal duct obstruction. J Korean Ophthalmol Soc. 1999; 40:2357–61.
15. Dortzbach RK, France TD, Kushner BJ, Gonnering RS. Silicone intubation for obstruction of the nasolacrimal duct in children. Am J Ophthalmol. 1982; 94:585–90.

16. Leone CR, Van Gemert JV. The success rate of silicone intubation in congenital nasolacrimal duct obstruction. Ophthalmic Surg. 1990; 21:90–2.
17. Kraft SP, Crawford JS. Silicone tube intubation in disorders of the lacrimal system in children. Am J Ophthalmol. 1982; 94:290–9.

18. Beigi B, O'Keefe M. Results of Crawford tube intubation in children. Acta Ophthalmol. 1993; 71:405–7.

19. Veloudios A, Harvey JT, Philippon M. Long-term placement of silastic nasolacrimal tubes. Ophthalmic Surg. 1991; 22:225–7.

20. Kim KS, Park TK, Choi WC. Intranasal endoscopic diagnosis and treatment in congenital nasolacrimal duct obstruction. J Korean Ophthalmol Soc. 2001; 42:7–12.
21. Anderson RL, Edwards JJ. Indications, complications, and results with silicone stents. Ophthalmology. 1979; 86:1474–87.

22. Hong SW, Chang HK. The complications of silicone tube ntubation after lacrimal surgery. J Korean Ophthalmol Soc. 1998; 39:2469–76.
23. Yoon TJ, Na KS, Yoon WJ. The effect of silicone tube intubation in pediatric nasolacrimal duct obstruction. J Korean Ophthalmol Soc. 2002; 43:155–9.
24. Cho KW, Lee SY, Kim SJ. Treatment of congenital nasolacrimal duct obstruction using silicone intubation set. J Korean Ophthalmol Soc. 1995; 36:553–8.
25. Mun HJ, Jung WS. Surgical efficacy of probing with silicone intubation for lacrimal apparatus obstruction in children. J Korean Ophthalmol Soc. 2002; 43:2375–81.
26. Ratliff CD, Meyer DR. Silicone intubation without intranasal fixation for treatment of congenital nasolacrimal duct obstruction. Am J Ophthalmol. 1994; 118:781–5.

27. Lim CS, Martin F, Beckenham T, Cumming RG. Nasolacrimal duct obstruction in children: outcome of intubation. J AAPOS. 2004; 8:466–72.

28. Welsh MG, Katowitz JA. Timing of silastic tubing removal after intubation for congenital nasolacrimal duct obstruction. Ophthal Plast Reconstr Surg. 1989; 5:43–8.

29. Jordan DR, Anderson RL. Prevention of prolapsed silicone stents in dacryocystorhinostomy surgery. Arch Ophthalmol. 1987; 105:455.

30. Yazici B, Akarsu C, Salkaya M. Silicone intubation with the Ritleng method in children with congenital nasolacrimal duct obstruction. J AAPOS. 2006; 10:328–32.
Figure 1.
Bicanalicular silicone tube is in place and silicone sponge is placed 2∼3 mm below the inferior meatus.
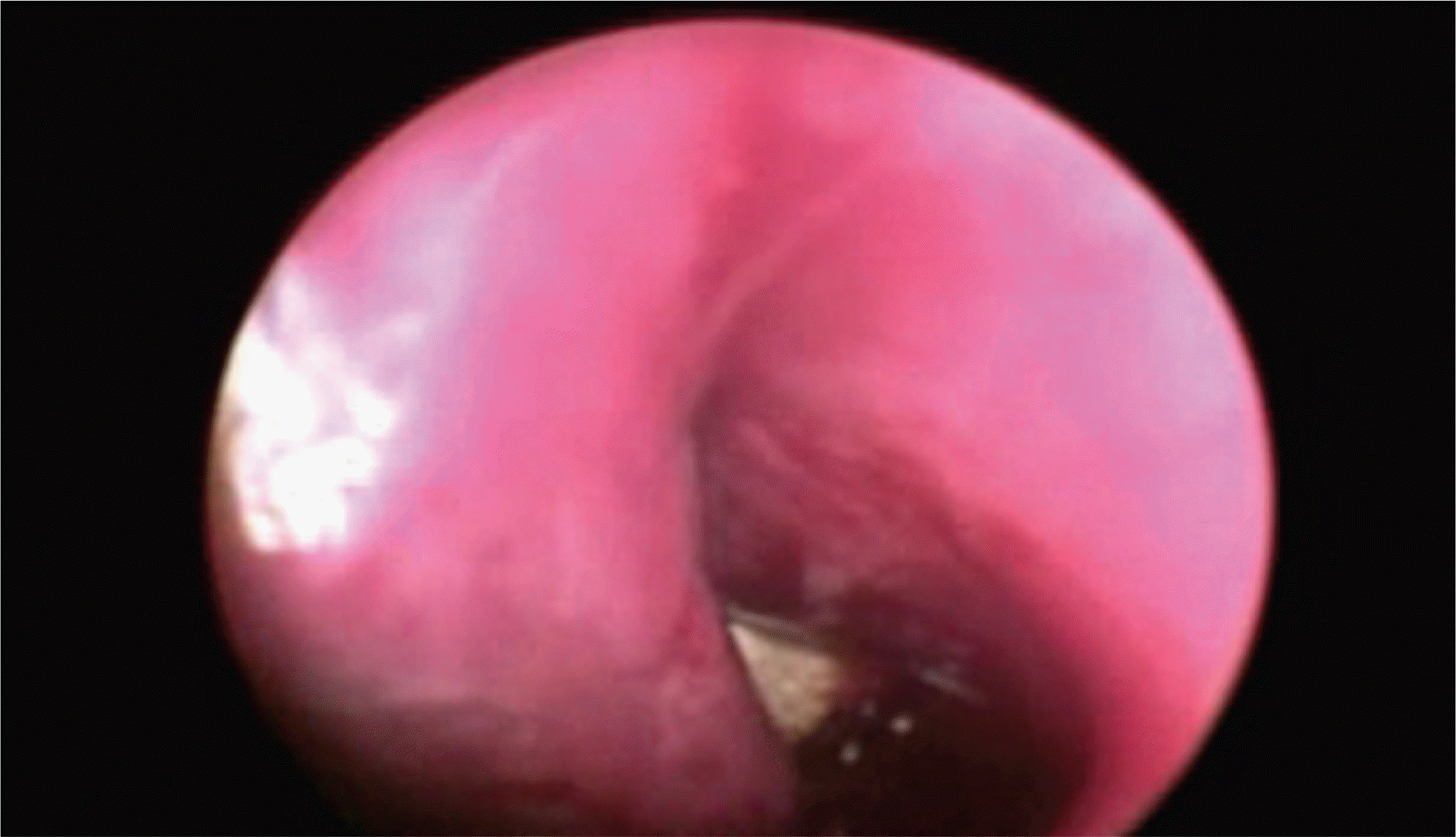
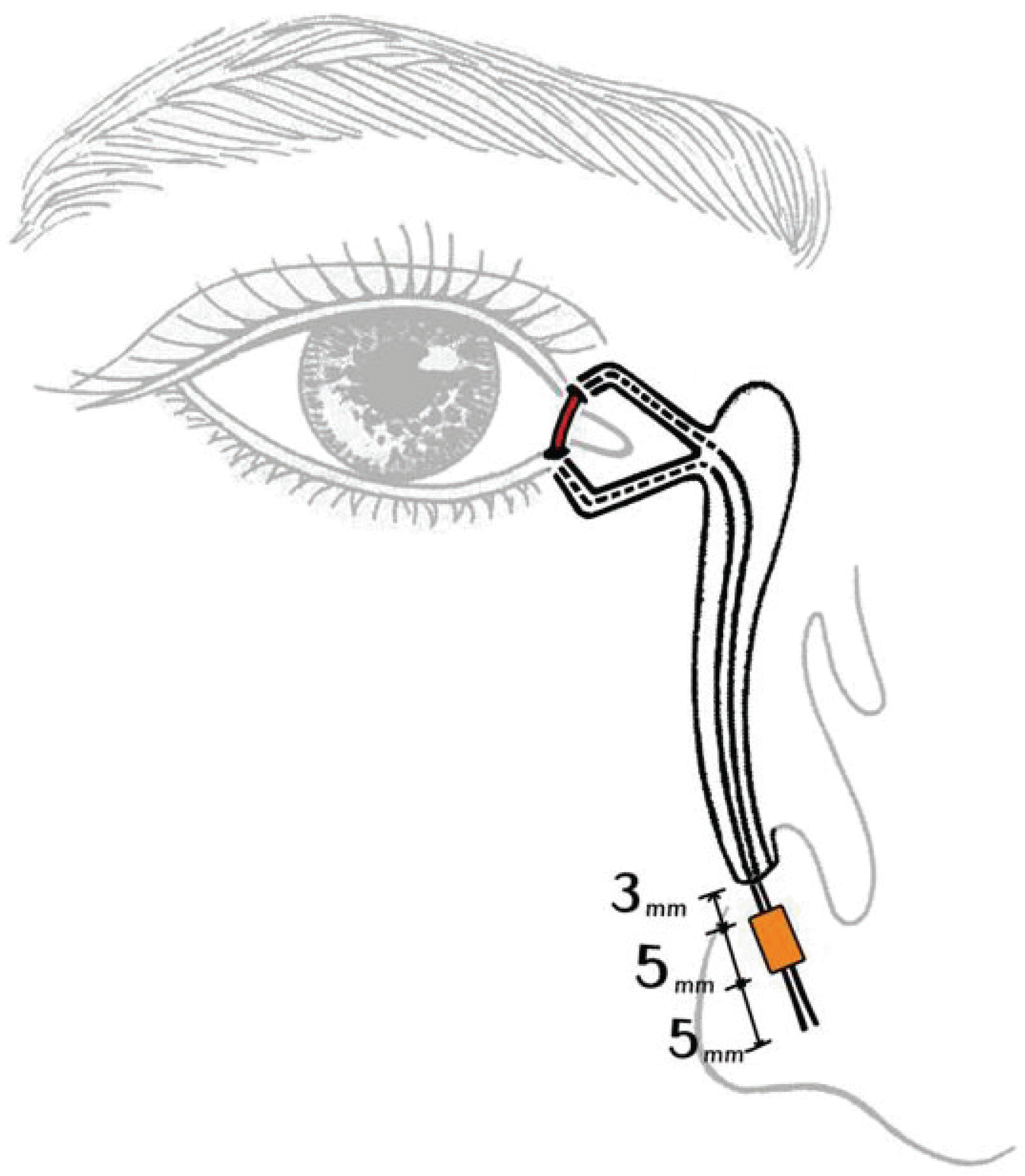
Figure 2.
Schematic diagram shows that the ideal position of the silicone tube intubated in modified surgery is in place without tension and the silicone sponge is placed 2∼3 mm below the inferior meatus.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download